Archived Whitepapers
The following whitepapers have been made available to readers of Becker's Hospital Review. Click on a category below to see the whitepapers available on that topic.
- Archived Whitepapers - click here to download all.
- ASC/Spine - click here to download all.
- Clinical Excellence - click here to download all.
- Health Information Technology - click here to download all.
- Hospital Finance - click here to download all.
- Payer - click here to download all.
- Process Improvement - click here to download all.
- Quality and Infection Control - click here to download all.
- Dental - click here to download all.

Reducing these administrative burdens to improve surgical care efficiency is a key opportunity for independent operators to stay competitive in their markets.
This white paper outlines five tips to decrease administrative burden and maximize surgical efficiency in orthopedic practices based on expert insights from a panel at the Becker’s Annual Spine & Ortho Conference.

However, shipping is an overlooked opportunity for significant savings. This brief report covers how Mountain View Hospital lowered shipping costs while supporting quality care through a collaboration with OptiFreight® Logistics.
Readers will learn about key insights that led to success, including:
- Tailored, innovative shipping solutions with no change to current processes
- Dedicated support from a team of committed logistics experts to continuously identify savings opportunities
- Data analytics and dashboards to track performance and share with departments and executive management

In this whitepaper, you'll learn current challenges, creative approaches and best practices pharmacy leaders are using at hospitals and health systems across the country to help manage pharmacy costs.
Key learning points:
- The role of pharmacy departments in controlling costs
- Key metrics leaders are assessing in an evolving billing landscape
- Partnerships that can promote financial well-being

In less than a year, Atlas Healthcare Partners — one of the nation’s fastest growing ASC management companies — has been able to significantly free up capacity for existing revenue cycle staff. This has led to measurable financial and productivity gains, and improved satisfaction for patients and staff.
This case study delves into how the company leveraged workforce automation and analytics solutions to solve long standing inefficiencies facing many revenue cycle teams.
Key learning points:
- Using technology to create additional capacity for existing staff
- Optimizing tasks across the RCM cycle, from pre-registration to back-office building
- 4 major areas of improvement when revenue cycle automation is done right

It's time to work smarter, not harder. That means revenue cycle leaders need to find new ways to do more with less.
This white paper explores how to streamline processes with intelligent automation, simplify cross-training and onboarding, and cut down on outdated manual processes.
Learnings include:
- Specific benefits of automation in rev cycle
- How to create an intelligent automation strategy
- How to decide which tasks to automate first

By streamlining documentation processes and adopting tailored solutions, ASCs can give physicians more time back in their day, fostering a more sustainable and fulfilling work environment. This white paper shares how ASC leaders can use AI-powered mobile solutions to capture patient-provider conversations for easier and faster documentation.
Key benefits include:
- Up to two hours saved on documentation daily
- 90% accurate notes generated seconds after a patient visit
- Increased access to patient records

This white paper examines how the TOPS System provides an entirely new modality to treat patients with spinal stenosis and spondylolisthesis. TOPS is the first and only FDA-approved facet replacement device with a superiority-to-fusion claim.
A disruptive breakthrough in spinal care, TOPS uniquely addresses the needs of patients, surgeons, facilities and payers to create a broad win for all stakeholders.
Key takeaways about TOPS:
- Motion alternative to lumbar spinal fusion
- FDA labeled as superior to spinal fusion
- New Technology Add-on Payment of up to $11,375 for Medicare eligible procedures

Obviously, this is difficult for patients — but it's also debilitating for healthcare organizations.
When patient collections are down, providers face bad debt, poor patient retention, and decreased satisfaction for patients and staff.
It's time to create a better patient collections experience. Providers who take action now can change a potentially bleak future simply by rethinking patient collections. Download the whitepaper to learn how to leverage data to create consumer-friendly experiences, improving both patient engagement and profit margin.
Key points include:
- The current state of patient collections, from deductibles to denials
- Why transparency is key to patient satisfaction + compliance
- Using automation + data to improve patient collections
- How to empower patients to pay with the 3 Cs

These growth opportunities present risks for physicians who fiercely value and guard their independence and control over their practices. For investors and advisers, recognizing and addressing these concerns when discussing possible deals is critical to successful transactions.
This white paper outlines current specialty consolidation trends and the top challenges of balancing needed growth with desired autonomy.
Key learnings:
- Macro trends in specialty consolidation
- Types of consolidation business models
- Pros and cons of consolidation

At least 1.6 million U.S. adults seek treatment for spinal deformities every year.
The Rationale for Personalized Interbody Devices is a literature review of published research about the potential benefits of patient specific interbody devices. Over 30 studies describe the benefits related to personalized geometry and endplate fit, which may help surgeons achieve sagittal and coronal alignment goals more reliably.
1. Personalized geometry and fit may help surgeons more reliably achieve optimal alignment, which is the most significant predictor of improved clinical outcomes in surgery to correct spinal malalignment.
2. Compared to non-personalized cage designs, personalized interbody cages reduced endplate stress, increased contact area for bone graft loading, lowered stress on posterior rods and caused a lower stress increase on adjacent levels.
3. Endplate conforming cages provided comparable clinical results and fusion rates in comparison to the traditional cage but with decreased postoperative subsidence and a lower severity of subsidence-related neck pain in follow-up.

Discover how you can transform your own supply chain strategy with these non-acute best practices and key learnings, including the use of data and increased visibility. Read this case study to learn more.

The opportunity for greater surgical volumes is ripe for minimally invasive procedures performed in ASCs.
Although robotic surgeries are a costly investment, the migration of procedures to the outpatient setting can ensure a return on investment.
This white paper from Intuitive Surgical, manufacturer of the da Vinci robotic surgery platform, will offer best practices in adding a robotic surgery line to your ASC.

While the OR is “ground zero” for recent financial problems, it also represents the best opportunity to rebuild hospital margins. In fact, better-performing hospitals are now leveraging surgical services to launch a sustainable financial recovery.
Disruptions in the OR workforce, changes in the surgery market and other factors have complicated the path to recovery. To rebuild surgical services revenue, hospital executives need to plan and execute a complete OR reset.
This report details for hospital executives how to lead a post-pandemic financial recovery by reinvigorating OR performance and reworking OR strategy.

This whitepaper offers quick insights into how one surgery center with 12,000 cases annually achieved $100,000 in savings through simple changes to their pack program.
Download to learn more.

In 2020, providers made 238 million claim status inquiries by phone, fax or email. Most payers still limit the number of inquiries allowed per call, which means more calls, more work for staff and more time wasted. And that’s before adding in the time it takes to update claim statuses in practice management or hospital information systems.
New financial performance demands are forcing revenue cycle, financial services and billing professionals to reevaluate their approach to claim monitoring. To unlock the cost savings and smarter workflows they need, it’s critical to deploy tech and tools that can easily automates the process. And not just any tech—you’ll need solutions efficient and flexible enough to meet the unique needs of your organization.
This whitepaper breaks down the most effective strategy for achieving smarter claim monitoring and shows you how to navigate the challenges you’ll face along the way.
Download this guide to learn:
- How providers handle claim status inquiries today
- Why current processes are inefficient
- How to solve claims status challenges

The leadership team at the Beaverton-based Oregon Surgical Institute and their JV partner, Regent Surgical Health, anticipated the future back in 2016 and embraced what at the time might have been considered a risky and uncertain strategy. Ever since, OSI has been making good on its bet.
This whitepaper provides a look into OSI's total joint journey. Learnings include:
- Best practices for practice design
- Insights on building clinical teams
- How to make continuous improvements to TJR programs

This study reveals how advancements in nano-surface technology on spinal interbody devices influenced a reduction in the postoperative opioid usage when comparing the same implant design with and without Nanotechnology.
Download this whitepaper to learn:
- Which factors were predictive of opioid use after surgery
- How interbody surface type was associated with postoperative opioid use

Key Points:
- Sagittal alignment is the most dominant radiographic predictor of outcomes in deformity patients
- UNiD™ Adaptive Spine Intelligence predictive models can successfully predict postoperative spinopelvic parameters in the instrumented and uninstrumented spine
- Degenerative patients have been found to be at 10 times greater risk for adjacent segment disease if their PI-LL mismatch is greater than 10 degrees

This interview with Ron Strachan, Healthcare CIO Advisor at Zoom shares what healthcare organizations — whether a provider, payer or life science company — need to build a modern, robust contact center.
Learning points:
- Why contact centers have gained renewed attention as a top priority
- How a cloud based, video enabled, contact center solution can expand patient engagement and satisfaction
- Ways the modern contact center can increase flexibility for physicians and potentially reduce burnout

Download this whitepaper where William Rifkin, MD, Associate Vice President and Managing Editor at MCG Health, breaks down the general framework around observation care, which aims to help users employ such care correctly to ensure patient safety and reduce friction with payers.
Key learning points:
- Discussion of the intended duration of observation care
- Comparing utilization patterns for selected diagnoses
- Analyzing the stability of observation vs. inpatient rates (including a combined analysis of ED decision making for all potentially ambulatory diagnoses)

Seeking a more efficient and effective tool than their wholesaler analytics platform, Sentara opted to implement a new drug spend optimization platform. The decision helped detect overcharges, simplify the credit and rebill process and identify lower-cost alternatives. Within five months, Sentara eliminated more than $1 million in annual drug spend.
This brief report delves into how the system achieved such significant savings.
Key learnings:
- The advantages of utilizing a spend optimization platform
- Best practices behind the success of Sentara's software implementation
- Benefits of leveraging both a supply chain expert and software to optimize purchasing workflows and drive savings

The system's marketing team has collaborated with its Office of Health Informatics and Analytics for several years, using data and technology to personalize patients' lifelong health journeys. This white paper delves deeper into UCLA Health's marketing strategy and successful initiatives, including:
- What marketing channels the system uses to connect with consumers
- How the system navigates stringent compliance requirements
- Deployments of new marketing technology from Oracle

This Forrester trends report leverages analysts' insights to forecast how digital experiences — ranging from chats to the metaverse — will affect the healthcare industry across three key dimensions: revenue, cost savings and patient experiences.
Download the report to learn:
- Which digital interface will affect healthcare the most
- How invisible experiences will have a larger financial impact
- Ways proactive engagement prevents illness before treatment is needed

See the huge impact the system made on protocol adherence and incidence of pressure injuries.
- 1 randomized controlled trial
- 7 conference abstracts
- Study results included both clinical and health economic data
The LEAF System combines wearable patient sensors with a user interface, offering:
- Personalized care for each patient
- Digital turn reminders (in room and at the nurses’ station)
- Confirmation that patient turns have sufficiently offloaded pressure
- Automatically generated reports that can be used for root cause analysis

Learn how, with TRIMEDX and a comprehensive clinical asset management strategy, Ascension identified and acted upon proactive opportunities that leveraged its medical equipment and amplified the positive impact the organization has on patients, staff, and communities.

Faced with these challenges, healthcare organizations must take a proactive approach leveraging historical data to develop predictive analytics to manage nurse onboarding and retention. This whitepaper shares how nurse leaders can apply a quality improvement methodology to streamline the onboarding process while addressing work-life balance concerns to successfully retain new nurses beyond their first few years of practice.
Key takeaways:
- 7 questions to consider when assessing your onboarding strategy
- 4 strategies to streamline new nurse onboarding
- The benefits of a centralized onboarding model

With safety and efficiency in mind, two Mayo Clinic physicians have reimagined the surgical gown to reduce instrument drops and improve instrument accessibility. One of the physicians recently caught up with Becker's to share how a simple change can help minimize contamination risks, procedural delays and enhance overall convenience and efficiency.
Download this brief summary to learn about:
- How a gown redesign can address key complexities in the delicate choreography of surgery
- Simplifying communication among OR staff
- The science behind "an extra hand" in resource-constrained environments

Under Mr. Desai's leadership, the Louisville, Ky.-based system is centralizing, automating and optimizing pharmacy operational, clinical and regulatory processes across nine hospitals and 450+ ambulatory care sites. This whitepaper details Baptist Health's success story so far, offering insights into tackling top challenges pharmacies are facing today — rising costs, drug and labor shortages, pricing/reimbursement complexities, and increasingly stringent regulations.
Download the whitepaper to learn how to:
- Gain real-time visibility into and control over drug products to optimize inventory, reduce costs, and minimize waste and expiry
- Free pharmacists from manual inventory management tasks and allow more time for patient care
- Centralize oversight of regulatory requirements to maintain safety and compliance

Specialty drugs account for more than half of drug spending. As employee benefit costs continue to cut into hospital margins, transitioning your outpatient pharmacy strategy to filling employees' specialty prescriptions in-house can generate significant savings — with the added benefit of improving patient satisfaction and care quality through expanded resources.
This whitepaper examines how a critical access hospital drove $300,000 in additional value from its employee benefit plan in one year and extended community care.
You'll learn:
- How to drive additional value in employee benefit plans
- New ways to capture specialty prescription volume in your outpatient pharmacy
- Real-world examples of challenges and successes
This white paper shares five key lessons from Michigan Medicine in Ann Arbor and Allina Health in Minneapolis, two systems that have built thriving hospital-at-home programs.
Key learning points:
- Important actions health systems have taken to plan for and stand up a hospital at home program
- Identify and overcome barriers related to launching a program
- Best practices and to grow and maintain a strong program

The Hackensack Meridian Neuroscience Institute at Hackensack University Medical Center became the first hospital in New Jersey to offer focused ultrasound treatment for tremor-dominant Parkinson's disease and essential tremor in June 2021. The team knew that to build a successful program, they would need to develop a marketing campaign that targeted patients as well as physicians.
Download the white paper to learn how they built brand awareness, surpassed their goal for cases in the first year and maximized the campaign's reach to potential patients.

However, organizations commonly struggle to find the right balance in these two areas. Organizations must maintain high operational maturity and a strong patient experience to strengthen patient loyalty and improve efficiency, build a positive reputation, and gain an edge over their competitors.
Download this e-book and see where your organization falls on the patient access maturity matrix.
Learning points:
- Common barriers to patient access and top areas of focus
- Ways for organizations to balance the patient experience and operations
- Steps to develop and execute a plan to improve patient access
Only 4% of U.S. residents feel consumer experiences have improved over the past year, according to a study by Customer Contact Week Digital. A staggering 57% feel they've gotten worse.
As competition in healthcare intensifies, hospitals and health systems can gain a competitive advantage by crafting an exceptional consumer experience. The trends detailed in this e-book reveal what consumers crave from digital experiences.
Learnings include:
- How to align the digital experience strategy with consumer needs.
- How to harness cutting-edge tools and other advanced consumer experience solutions.
- A breakdown of how AI is revolutionizing the consumer experience across industries.

Patients are frustrated by poor communication, hard-to-solve billing disputes and — when they are able to get an appointment — feeling rushed. As a result, more providers are innovating and exploring possibilities in elevated care models, including personalized primary care via concierge medicine or membership-based healthcare.
In these five must-reads, you'll learn about:
- New wellness models being embraced by health systems
- Innovation in primary care
- Why patient experience scores are on the decline

This interview with Ron Strachan, Healthcare CIO Advisor at Zoom shares what healthcare organizations — whether a provider, payer or life science company — need to build a modern, robust contact center.
Learning points:
- Why contact centers have gained renewed attention as a top priority
- How a cloud based, video enabled, contact center solution can expand patient engagement and satisfaction
- Ways the modern contact center can increase flexibility for physicians and potentially reduce burnout

Hospitals and health systems are increasingly embracing communication technology to enhance the patient experience, address labor shortages and foster better collaboration among clinicians. However, the implementation of such technology requires careful consideration to avoid compromising patient experience.
This white paper outlines strategic approaches for healthcare organizations to thoughtfully implement communication technology to help — not hurt — the patient experience.
Key learnings:
- The rise of hospital 'smart' rooms
- Virtual communication 'don'ts' that can hinder patient experience
- The benefits of an integrated virtual communication technology strategy

Learn more in our latest whitepaper where we will:
Review the ongoing challenges health systems face providing mental health care in the ED today.
Examine why post-discharge care is so vital for higher severity patients and how technology-enabled telehealth solutions can help ease the burden.
Explore how health systems can partner with technology-enabled telepsychiatry solutions to improve access, outcomes, and ED throughput
Discuss the latest clinical outcomes from Brightside Health’s technology-enabled telehealth solution.

This whitepaper details how LEAF reminders sent wirelessly from the wearable sensor to a display at the nurses’ station, have been shown to exceed turn protocols from the national average of 48% to a turn adherence rate of 98%. If each HAPI represents an average financial burden of $21,767, reducing the incidence of avoidable cases could save the average hospital hundreds of thousands or even millions of dollars each year.

In this paper, you'll access insights from a discussion with pharmacy leadership at IU Health and learn how they implemented a centralized service center (CSC) to improve hospital operations, clinical workflows, and patient and employee satisfaction.
You'll learn:
- How CSCs help with medication management and non-pharmacy supply chains
- IU Health's advice + best practices for other organizations planning to stand up a CSC
- Strategies for meeting established milestones and measuring success

In this whitepaper, Look Beyond the Operating Room, you’ll learn:
- How you can implement sustainable technology in your hospitals and healthcare facilities
- Cost-effective options for cleaning methods
- Ways to continuously clean surfaces and air in different rooms within healthcare settings

In this insightful guide, Valerie Bandy, PharmD, MBA, BS, RPh, discusses CPSCs and dispels common misconceptions. Dr. Bandy highlights the broader benefits beyond cost reduction, including inventory optimization, staff redeployment and enhanced patient care.
Key takeaways:
- Identify the five CPSC myths that are top of mind for pharmacy supply chain leaders today.
- Recognize the importance of integrated pharmacy supply chain and warehouse management systems within CPSCs.
- Understand the strategic role of CPSCs in efficiently managing a wide range of services.
- Learn how CPSCs enable a sharper focus on critical operational and patient care requirements.

To better support staff and reduce unnecessary spending, healthcare organizations must streamline clinicians' onboarding process, which sets the stage for retention and frees up time to focus on what really matters: patient care.
This white paper details how a streamlined, automated onboarding process can be a strategic differentiator. Download to learn more about:
- Current hurdles and inefficiencies in most onboarding processes
- The role of technology in simplified clinician onboarding
- How better onboarding supports regulatory, licensing and compliance needs

If hospitals and health systems want to retain and attract nurses, they must reduce caregiver burden, enhance safety protocols, improve nurse well-being and remain patient-focused.
In this white paper, three nursing experts discuss the role new technology can play in addressing nursing-related challenges.
The experts include:
- Annette Brown, BSN, RN, chief nursing informatics officer, Eisenhower Health (Rancho Mirage, Calif.)
- Marianne Hatfield, RN, DNP, chief nursing officer, Wellstar Kennestone Regional Medical Center (Marietta, Ga.)
- Michael Williams, MD, chief medical information officer, UVA Health (Charlottesville, Va.)
- Why documentation is a significant burden for healthcare staff — especially nurses
- The importance of grounding efforts to unburden nurses in workplace safety
- How new technologies are driving safer, more connected care and reducing caregiver burden

In this guide for healthcare marketers, readers will learn how to bridge the gap between patient privacy and digital marketing quickly and cost-effectively.
Key learnings include:
- How to navigate HHS guidance around tracking tools and technologies
- How to make your most important analytics and marketing tools HIPAA compliant
- How to do digital advertising without sharing protected health information

This latest whitepaper from NeuroFlow explores how organizations can take a data-driven approach to suicide prevention and population risk management. It covers how real-time data provides greater visibility into previously overlooked populations, and how these insights arm care teams with the tools and confidence they need to prevent crises.
This white paper will answer key questions such as:
- What is the cost of suicide on the healthcare industry and society?
- What is the liability of suicide prevention programs?
- What are innovators doing to identify at-risk individuals at scale?

But roadblocks remain. Health equity is a major concern, both because limited data could exacerbate health disparities and because many patients cannot afford care. Additionally, a large pool of patients is needed to ensure comprehensive data, and some payers still need to be convinced of precision oncology's value.
During a Becker's advisory call, leaders from hospitals and health systems across the country discussed these challenges and how the field will continue to evolve, offering insights on how organizations of any size can find success utilizing precision oncology for treatment.
Download the white paper to learn:
- The biggest roadblocks to precision oncology today + strategies to overcome them
- How leaders are addressing health equity, reimbursement + more
- How to prepare for the future of precision oncology

In this article, you'll find a recap of an exclusive discussion with health system clinical and technology leaders, who candidly share their stance on generative AI, how they're currently using it and what's "keeping them up at night."
Download to learn more about:
- Where health systems currently stand in generative AI adoption
- Key patient considerations (age, data ownership, etc.)
- How leaders are navigating challenges and concerns in accuracy, safety and unintended consequences

In this white paper, you'll learn how health system leaders are building their precision medicine programs, fueled by genomics, and tips for navigating common challenges along the way.
Download to find more on:
- Approaches to strategic partnerships
- Data and tech capabilities that drive successful programs
- The need for aligning incentives/payment models
- How to ensure equitable access in precision medicine

In this white paper, you'll learn how a decentralized PCR testing infrastructure supports all aspects of the Quadruple Aim, and how health systems are using technology to scale quick, accurate and accessible tests for better outcomes.
Download to learn more about:
- Benefits of decentralized testing, including reduced length of stay and readmissions
- How decentralized PCR testing data supports disease tracking + antibiotic stewardship
- How standardized molecular diagnostics helps health systems achieve the Quadruple Aim

In this report, you’ll have access to survey findings and perspectives of 13,000 medical residents in their final year of training. The report sheds light on the level of demand for graduating medical residents, as well as their practice preferences and plans. As a thought leadership resource, this analysis also is intended to help healthcare organizations recruit medical residents and assess the priorities of newly trained physicians entering the field.
Download for more insights on:
- The relative importance of various job features as residents evaluate practice opportunities
- The population size of communities where residents would most like to practice
- The types of practice settings residents prefer

- Equip clinicians with evidence-based medicine, clinical research, and site-specific preferences at the point of care
- Streamline clinical and pharmacy workflows with clinical decision support embedded directly into the electronic health record (EHR)
- Standardize the delivery of high quality care across cancer center sites and patient populations
- Drive financial success by capturing and reporting payer-required data elements

Hospitals across the U.S. are dipping their toes into the world of virtual nursing, but many are unsure where to start and not making much progress. Yet Aurora, Colo.-based UCHealth has been in the virtual care game for years and can be viewed as a roadmap for other facilities looking to cope with capacity challenges, staffing shortages and extended emergency department wait times.
Download the whitepaper to learn:
- Concrete strategies and starting points for implementing virtual care
- How virtual nursing can improve employee retention and patient outcomes
- Real-world results from a successful virtual nursing program

While permanent allied healthcare staff remain hard to find in local markets, travelers have proven a reliable supplement with geographical flexibility. However, the job market has become more competitive as demand for a flexible allied healthcare workforce grows nationwide.
This white paper outlines numerous strategies healthcare organizations can use to successfully staff allied healthcare travelers.
Key learnings:
- The benefits of employing allied travel professionals
- Five ways to make allied travel assignments more appealing
- Workers' biggest pain points in the job search process

Publication summary covers:
- Improvement in turn protocol adherence
- Reduction in incidence of pressure injuries
- Specifics on ventilator-dependent patients
The LEAF System combines wearable patient sensors with a user interface, offering:
- Personalized care for each patient
- Digital turn reminders (in room and at the nurses’ station)
- Confirmation that patient turns have sufficiently offloaded pressure
- Automatically generated reports that can be used for root cause analysis

In this e-book, you'll find a collection of seven must-read articles that highlight innovation, challenges and viewpoints of leading hospitals and health systems like CommonSpirit Health (Chiago), UPMC (Pittsburgh) and more as they work toward building a unified digital environment.
You'll find:
- What leaders predict healthcare will look like in 100 years
- How digital chiefs are preparing for the near future
- Best practices for achieving a unified tech environment that's safe + compliant

To learn more about the state of POCT today, Becker's Hospital Review spoke with Rhonda Ashcraft, laboratory manager for clinical operations with Memorial Hermann Medical Group in Houston, and two leaders from Cue Health, an innovator in molecular point-of-care diagnostics.
This white paper contains insights on:
- The evolution and limitations of antigen testing
- Traditional barriers to molecular POCT and how to overcome them
- Why molecular POCT is becoming the "gold standard" of POCT solutions

Becker's Hospital Review recently spoke with digital experts — including Maria Fernandez, director of patient experience at Emory Johns Creek (Ga.) Hospital — to discuss how to deliver the consumer-centric experience patients are demanding and achieve each of the above goals.
This brief report covers:
- Key factors driving patient frustration
- The type of technology hospitals can use to streamline digital interactions
- How Emory Johns Creek Hospital is improving staff and patient experience

This new report answers these questions and examines more trends affecting the patient experience. It covers:
- Why healthcare providers need a strong, proven patient-experience strategy
- Which patient-experience projects should be top priority for providers
- How artificial intelligence is impacting the quality of digital patient experience
- 6 practical recommendations for achieving success

care teams, enabling them to dedicate their energy to patient care rather than grappling with disjointed tools.
Connexall solutions power the connected hospital with an integrated end-to-end communication platform to promote care quality, enhance patient experience, elevate staff satisfaction, and improve health outcomes.
This interactive guide illustrates examples of how Connexall is helping transform patient care and realize their vision of a becoming truly connected hospitals.
Learning Objectives:
Through this guide, users will:
- Recognize the positive impact that smart integration technology can have on streamlining workflows, improving care delivery, and enhancing patient and staff satisfaction.
- Understand the value of employing a flexible, vendor neutral, and fully customizable use case-based methodology to realize the vision of a smart connected hospital.
- Experience how leading health systems across North America are employing Connexall solutions to more effectively meet the unique needs of their patients, providers, and communities.

To unpack this issue, Becker's Hospital Review hosted an advisory call with technology and patient engagement leaders from prominent hospitals and health systems. Organizations represented on the call include:
- Intermountain Health (Salt Lake City)
- MUSC Health (Charleston, S.C.)
- UPMC (Pittsburgh)
- The barriers to a positive tech experience for patients
- Health systems' inclusive, proactive patient-facing digital strategies
- Why change management is the biggest hurdle in any technology journey

This report covers how to speed up resolution after patient-harm events, lower costs, and mitigate clinician stress and care team disruptions. Cases close three times faster than the national average in instances where intervention happens quickly and indemnity is paid, according to early findings.
Learning objectives:
- Why reporting harm events early is important
- How early reporting influences both expenses and the lifecycle of a case positively
- The elements of early intervention and their benefits

An onboarding process can take up to six months and cost up to $300,000 per clinician, and the cost of losing one nurse is estimated to be $52,350. It's imperative for healthcare
organizations to streamline clinicians' onboarding and hold on to them once they're up to speed.
This white paper details how an automated and seamless onboarding process can be a strategic differentiator and free up clinicians to focus on what really matters: patient care.
You'll learn:
- What parts of the onboarding process are frustrating for providers
- Why efficient onboarding is vital for employee retention, patient care and finances
- How to create a unified, seamless onboarding process through intelligent automation

The bottom line: Pharmacies can't afford to lag behind on digital innovation. Pharmacy workers are already struggling to keep up with the growing demand, and patients expect the convenience, accessibility and reduced costs that a digital experience can offer. This whitepaper lays out the evidence that the pharmacy industry is poised for a movement and offers concrete ways to prepare.
You'll learn:
- The three telltale signs of an incoming movement for pharmacy
- Why it's vital for pharmacies to transform the way they operate
- Strategies for innovation and tech advancement, patient satisfaction and retention, and tackling economic headwinds

The annual AMN Healthcare/Merritt Hawkins Review of Physician and Advanced Practitioner Recruiting Incentives is a benchmarking resource used by hospitals, medical groups and other facilities to inform recruitment efforts.
Download the report to learn:
- How demand for physicians and advanced practitioners is changing and which are most challenging to recruit
- The types of financial and other incentives used to recruit physicians and advanced practitioners
- The types of practice settings into which physicians and advanced practitioners are being recruited and the types of communities that are recruiting them based on population size

Efficient and effective care for intermediate-risk patients requires a series of correct clinical determinations and decisions. This white paper explores an evidence-based approach to give ED clinicians confidence when caring for patients presenting with immediate-risk chest pain.
It covers:
- Appropriate risk assessment
- Next steps for intermediate-risk patients
- Revascularization versus medical therapy

The new findings also reveal more about hospital nurses' overall outlook on care quality, as well as what they want out of technologies to improve the work environment and patient safety.
Healthcare leaders will learn:
What nurses say they want technology to help them do
Where CDSS are being used outside of the ICU and the value nurses find in them
Key barriers to implementing CDSS outside of the ICU and how hospitals can overcome them
Read the full report.

This white paper narrates a patient's healthcare journey supported by cloud communications, demonstrating how this technology applied to each step — from scheduling to post-op, follow-up and billing — can empower and delight patients and support processes between all key players in the care continuum.

This playbook walks you through key components of a tech-enabled patient room, and how organizations like Novant Health (Winston-Salem, N.C.) and Tampa (Fla.) General Hospital are improving experiences for patients and their families, as well as streamlining clinical workflows for front-line teams.
You'll also find:
- Case studies linked throughout
- Concrete ways smart room technology supports and satisfies nurses
- Advances in tech that promote personalization and patient education

This whitepaper outlines how tailoring mobile experiences for various users creates a more personalized and engaging healthcare experience, ultimately boosting staff and patient experience — and your bottom line.
Key learnings:
- The benefits of patient and employee mobile apps
- How to adopt personalized mobile strategies

Publication summary covers:
- Improvement in turn protocol adherence
- Reduction in incidence of pressure injuries
- Specifics on ventilator-dependent patients
The LEAF System combines wearable patient sensors with a user interface, offering:
- Personalized care for each patient
- Digital turn reminders (in room and at the nurses’ station)
- Confirmation that patient turns have sufficiently offloaded pressure
- Automatically generated reports that can be used for root cause analysis

In this insight brief, we delve into value sets and their importance in various healthcare initiatives such as population health management, quality reporting, clinical trials, and more. We also highlight the challenges organizations face when managing value sets, including:
- Issues with processes such as time-consuming manual data manipulation due to code set updates and inconsistent methods for building value sets; and
- Issues with value set definitions and data ambiguity including competing methods for defining value sets and the frequent absence of a centralized repository in which to store them
Fortunately, like most challenges, there is a solution – in this case, one that leverages comprehensive clinical terminology and code mappings along with innovative tooling to streamline the creation and editing of value sets.

This white paper breaks down three possible scenarios for nationwide value-based care. In each scenario, industry experts describe what the future could look like, how it might unfold, and what that means for major stakeholders in healthcare — and what to do if this future doesn't look rosy for your organization.
Key takeaways:
- See how three different scenarios catalyze value-based care
- Discover who gains the advantage and how each projected path forward affects major stakeholders
- Learn how to secure a place in a value-based care future

The improved atrial fibrillation (AF) detection rates of MCOT followed by ILR reduce the likelihood of a secondary stroke due to new anticoagulant use, resulting in a significantly lower total cost of care.
This study demonstrates:
- MCOT as a first-line evaluation detected 4.6 times more patients with AF compared to ILR alone.
- MCOT followed by IRL resulted in almost 8 times lower costs compared to ILR alone, due to improved AF detection rates and reduction of secondary stroke risk.
- Total cost difference of MCOT followed by ILR vs ILR alone

For forward-thinking healthcare leaders, genomic screening is on the brink of becoming the standard of care.
In this whitepaper, you'll read three experts' thoughts on the evolving clinical and research landscape for genomics, as well as the business case for population genomics at an academic medical center.
Key learnings:
- Explore MUSC's innovative genomics initiative
- The growth of enterprise genomics programs
- How population genomics is transforming clinical care and driving strategic growth

Proper use of surgical gloves is a critical aspect of infection control efforts, but surgical gloves come with their own issues, such as being prone to perforation and causing skin problems for wearers after prolonged use. To minimize risks, healthcare providers should develop detailed and consistent guidelines for surgical glove use.
Download this white paper to learn:
- Factors to consider to choose the right surgical gloves
- Best practices for safe surgical glove usage
- How to stay up to date on hand hygiene best practices

See the huge impact the system made on protocol adherence and incidence of pressure injuries.
- 1 randomized controlled trial
- 7 conference abstracts
- Study results included both clinical and health economic data
- Personalized care for each patient
- Digital turn reminders (in room and at the nurses’ station)
- Confirmation that patient turns have sufficiently offloaded pressure
- Automatically generated reports that can be used for root cause analysis

In this whitepaper, organizations will learn how to implement a proactive approach to comprehensive clinical engineering for optimal patient care and greater return by:
- Using technology to support a preventative maintenance strategy
- Strengthening supply chains with a dedicated process
- Staying ahead of regulatory developments
- Establishing data-driven cybersecurity protocols for medical equipment

And because of that, personalized experiences are what consumers expect.
But as of 2023, receiving a personalized experience from a healthcare provider is an anomaly.
Because of this, patients are increasingly disappointed with the experience their providers deliver (and are starting to look at alternatives).
This whitepaper explores the personalization journey of two leading health systems and provides steps you can take to implement at your organization.
Discover how:
- Leading health systems combat patient leakage and maintain a competitive edge
- Personalization can help you save anywhere from $6–40 for every call avoided
- Leading health systems achieve 95%+ patient satisfaction

This case study reviews the research performed and the impact researchers found on patient survival rates and contribution margins.
Read more for key insights on:
- The value of reducing care variation
- The cancer center's clinical and financial successes, including enhanced patient survival rates and a 74 percent contribution margin increase
- Anticipated effects on provider efficiency and physician burnout

Common pain points, including failing to enroll the right people and missing the mark on holistic, socioeconomically sensitive services, leaving patients in the shuffle.
This whitepaper outlines how care management stakeholders can acknowledge shortfalls and bridge the gaps in financial, technical, and clinical strategies to support better the health and wellness of people with chronic conditions.
Key learnings:
- Insights from clinical executives at a leading national health plan and diabetes management organization
- 5 common pain points in the care management continuum
- Strategies to reinvent the care management status quo

This whitepaper shows how hospitals are harnessing the power of technology and artificial intelligence to increase productivity, improve clinician satisfaction, and work anytime, anywhere.
Find out how your hospital can experience:
- AI-driven GI documentation workflows
- Increased cybersecurity
- Robust enterprise reporting; and
- Advanced, always current medical content

Still, many leading healthcare organizations have identified and implemented evidence-based models that meet the needs of their populations with consistently positive outcomes. NeuroFlow has distilled that experience and advice into a helpful guide providing the tools your organization needs to develop an effective roadmap for integration.
In this whitepaper you'll learn:
- How to advance integrated behavioral health programs based on your organization's unique needs
- Opportunities to scale integrated behavioral health programs and key considerations to achieve financial sustainability
- How leading systems have successfully launched and expanded integrated behavioral health program

In this interview, hear from Cardinal Health’s specialty drug inventory expert about inventory technology that enables providers to better manage specialty drug inventory and ensure these expensive products aren't going to waste.
Learning points:
- Prepare for unpredictable demand without incurring carrying costs for limited distribution drugs
- Optimize your specialty inventory spend by only buying products you use
- Eliminate waste due to expired specialty medications

This guide offers a collection of updated, evidence-based guidelines for hand hygiene and surface disinfection to support your team as you navigate forward. You'll find actionable tips and insights on:
- Post-COVID revisions to infection prevention regulations
- Criteria for evaluating hand hygiene and surface disinfection products
- Resources that propel improved safety culture and infrastructure

This interview with Ron Strachan, Healthcare CIO Advisor at Zoom shares what healthcare organizations — whether a provider, payer or life science company — need to build a modern, robust contact center.
Learning points:
- Why contact centers have gained renewed attention as a top priority
- How a cloud based, video enabled, contact center solution can expand patient engagement and satisfaction
- Ways the modern contact center can increase flexibility for physicians and potentially reduce burnout

Despite the growth in outpatient procedures, challenges remain. Barriers to the continued expansion of outpatient procedures include differential payments for various sites of care, inadequate compensation for preoperative patient optimization, competing hospital priorities, and inequities in patient access.
This whitepaper provides a comprehensive overview on current trends in outpatient procedures and what healthcare organizations must do to remain successful in the future.
Key learnings:
- Current and future regulatory and financial trends
- Key considerations for shifting procedures to lower sites of care
- How benchmarking tools can provide guidance

In this white paper, you'll see insights gleaned from an executive roundtable at Becker's Hospital Review's 2023 Annual Meeting in Chicago, where leaders discussed the role of automated intelligence and platform-based tech in these areas. Read more to learn about:
- Core tech features of the redesigned, modernized patient room
- How clinical care coordination centers address efficiency and patient needs
- Why leaders should think twice before fully outsourcing to an AI system

In an advisory call, leaders from NYC Health + Hospitals in New York City, Allegheny Health Network in Pittsburgh and Baptist Memorial Health in Memphis, Tenn., discussed the patient payment landscape, and shared strategies to improve payment processes and the patient experience.
In this e-book, you'll learn what these healthcare organizations and others are doing to create a culture that fosters positive financial conversations with patients.
Key learnings:
- Tips for increasing point-of-service collections
- Best practices for educating patients on financial responsibility and health insurance
- How to personalize payments for a better patient experience

Becker's Healthcare recently spoke with four physicians about how pain management protocols in ASCs have evolved as more patients and procedures have shifted to outpatient settings and as the opioid crisis persists. Experts also shared the core components of a successful multimodal pain management program. The ASC surgical and pain management experts tapped for their insights included:
- Michael Briseño, MD, North Texas Orthopedics and Spine Center (Grapevine, Texas), Texas Health Orthopedic Surgery Center Heritage (Fort Worth, Texas)
- Jonathan Hyde, MD, Miami Spine Specialists
- Richard Teames, MD, BSN, Dallas-based Valiant Anesthesia Associates
- Shane Zamani, MD, Surgery Center at Doral (Fla.)

In this guide, you'll learn the key steps to properly select, store and use exam gloves to ensure the optimal health and well-being of your patients and clinicians.
You'll have access to resources including:
- An exam glove clinical application matrix to help you choose the right exam glove in every clinical setting
- An exam glove storage guide
- Step-by-step instructions for putting on and removing exam gloves for the best possible protection

In healthcare, transformational leadership yields numerous benefits, including employee engagement and retention, patient safety and organizational achievement.
The key question is: how to develop truly transformational leaders?
This new white paper lays out exactly what transformational leadership is, what the benefits are and most importantly – how to become a transformational leader.
Download this white paper now to learn:
- The definition of transformational leadership
- Characteristics of transformational leaders
- The many ways that transformational leadership benefits an organization
- Four steps to become a transformational leader

Our concise and hard-hitting trends guide shares concrete feedback that providers can use to become more patient-centric and successful.
You’ll learn:
- How patient feedback drives business results.
- How Google influences the patient journey.
- Why in-network retention is at risk.

Understanding who is most likely to no-show for an appointment — and why — is important to determining how to best tackle the issue.
In this whitepaper, you'll learn:
- 3 strategies that don't move the needle on no show rates
- 5 common misconceptions about patient behavior and motivations
- 7 things that actually work to radically reduce the number of no-shows

Online reviews, the expectation of price transparency and the popularity of wearable health-tracking devices are all influencing the way patients seek medical care. This e-book explores five trends in care delivery transforming the modern patient experience.
Key learnings include:
- How patients are choosing healthcare providers today
- Why price transparency is a must
- What patients are looking for in the care experience

In this paper, see:
- Highlights of the guidelines in an easy-to-read format.
- A comparison between auditory cueing and wireless patient monitoring technology.
- A case study showing how wireless patient monitoring improved efficiency for nursing staff and significantly reduced HAPI incidence in a 145-bed general hospital.
- Personalized care for each patient
- Digital turn reminders (in room and at the nurses’ station)
- Confirmation that patient turns have sufficiently offloaded pressure
- Automatically generated reports

But whether it’s navigating patients' post-pandemic perceptions or concerns about diversity, equity and inclusion, health system and pharma marketers can help female patients prioritize wellness and make confident healthcare decisions.
Download the special report to learn:
- Why women are missing out on care
- What obstacles prevent women from addressing health concerns
- The 3 biggest things women look for in a healthcare provider
- How marketers can enhance patient experiences and outcomes + 4 ways they can better serve women

In this white paper, you'll learn about the perioperative AIMS software that led an anesthesia group in a Florida health system to success with EHR integration, mobile flexibility, and an intuitive user interface.
Discover the benefits through their eyes — from improved staff satisfaction, documentation, and patient safety to cost savings and streamlined OR processes.
Read more to find out how your facility could enable:
- Automatic charting of patient vitals with wireless data streaming from anesthesia monitor machines
- On-the-go documentation with a mobile tablet that allows for real-time patient check-ins
- Improved patient safety and compliant documentation from pre-op to post-op and billing
- Increased staff satisfaction within an understaffed workforce

Point-of-care blood management systems can help reduce transfusion errors while improving efficiency and lowering costs. Discover how the implementation of this system helped one hospital save $436,000 annually.
In this whitepaper, you'll learn:
- The problems hospital blood supply chains face today
- Why the role of point-of-care blood management systems is more critical than ever
- How point-of-care blood management systems help support transfusion safety, compliance and efficiency while reducing costs

This white paper outlines how one health system successfully reduced readmissions for chronically ill patients by utilizing remote patient monitoring.
In this whitepaper, you'll learn:
- Best-practices for implementing a sustainable and effective remote patient management program.
- How Grand Forks, N.D.-based Altru Health System achieved significant reductions in readmissions for specific clinical case uses and expanded its remote patient monitoring program.
- How remote patient monitoring programs can increase patient-provider communication, improve patient engagement and encourage patient self-management.

In this whitepaper, you'll learn how community health center leaders and their organizations are adapting to the rise in demand for contraceptive care and how they're addressing barriers to providing services for patients.
Read more for insights on:
- The emerging role of primary care providers as key figures in contraceptive counseling, service delivery and access, and how leaders can support them in this role
- Navigating barriers to contraceptive care, such as insurance challenges
- Empowering staff to make time for contraceptive counseling and education and patient-centered care

CAD and PAD patients have always faced roadblocks along their post-intervention care journey, from costly treatments to finding the motivation and time for managing their conditions. Additionally, there's a disconnect between physicians' and patients' views on the value of digital tools in adhering to care plans.
This white paper from Year 3 of Abbott's Beyond Intervention research into the global state of vascular care contains key insights from over 2,000 patients, healthcare providers and healthcare leaders on how we might improve patient adherence and outcomes outside healthcare facilities.
Key learnings include:
- The importance of a comprehensive care experience within the healthcare system
- The biggest challenges for patients in adhering to post-discharge care plans
- How healthcare leaders and providers can provide multiple touchpoints and leverage digital tools to make adhering to a care plan at home easier for patients

For nearly 20 years, the Interferon Gamma Release Assay — a simple blood test — has offered a more efficient, more accurate alternative, yet 3 out of 4 healthcare providers default to the century old method. In this white paper, Quest Diagnostics will explore the facts and debunk the myths and misconceptions that have surrounded IGRAs since their inception.
Key learning points:
- How IGRA blood tests use the latest field-proven medical technologies to yield a conclusive result 97 percent of the time
- How the IGRA saves patients and physicians time and stress
- Why the IGRA is ultimately the most cost-effective choice

In this white paper, Duarte, Calif.-based City of Hope shares five key lessons learned from building their precision oncology program, as well as the success they're seeing in patient engagement and earlier detection.
You'll also learn:
- How precision oncology has changed over time, and how the more recent "panoramic" approach is better positioning clinicians to choose the right treatments for patients
- Why standardization of care in precision oncology is critical for equitable care
- The benefits that a precision oncology program can bring to patients and communities + the infrastructure and processes organizations should consider in building a successful program

In this white paper, you'll learn how clinical decision support tools can augment physicians' reasoning and enable them to visualize patient data, access specialist knowledge and identify trends to improve efficiency, accuracy and quality of care. You'll also find insights on:
- The dangers of unconscious bias in diagnostics
- The impact of inappropriate referrals
- Improving patient satisfaction and health equity

Healthcare leaders shouldn’t underestimate the importance of supplying staff with the right operating room products to ensure they feel confidently protected to care for patients.
This eBook explores how supply reliability affects clinical teams and the solutions that can help mitigate surgical drape and gown challenges in the OR.
Please fill out the form to download the eBook.
Learning objectives:
- Appropriate protection and comfort for any procedure
- The value of choosing the right drape and gown for each procedure
- How a healthy supply chain with state-side manufacturing can help keep shelves reliably stocked.

To tackle these challenges, Conway (Ark.) Regional Medical Center focused on patient monitoring to improve compliance rates and make doing the right thing easier for clinicians.
Read this case study to learn how Conway Regional:
- Identifies patients with sepsis earlier with continuous alerts and reminders that guide care
- Improved SEP-1 bundle compliance by more than 20 percent over four months
- Achieved cumulative savings of $384,000 in four months

Key Learning Objectives:
- Learn how modern utilization management solves multiple challenges for healthcare organizations
- Understand the keys to empowering patients and reducing unnecessary costs by ensuring appropriate care
- Find out how modern independent clinical review works seamlessly with your organization to expand your capabilities

The so-called "superclinic" houses hundreds of physicians in nearly three dozen specialties and represents one of the busiest outpatient centers in the U.S.
During this webinar, leaders will share how the Kirklin Clinic implemented an intelligent room scheduling system to address these challenges and grow patient volume without expanding physical space. Learn how the hospital achieved:
- A 7.4 percent increase in patient visits and 4.7 percent increase in clinic session volume
- Shortened patient wait times
- Reduced administrative burden and higher physician satisfaction

CHIME's 2022 Digital Health Most Wired survey assessed healthcare organization's digital health capabilities and usage across eight key categories, including patient engagement. This report offers a summary of the survey's patient engagement key findings, including a look at how organizations have improved patient engagement and what the intersection of patient empowerment and digital health will look like in the future.
In this report, you'll learn:
- Which tools the majority of systems now have and consider table stakes
- Which tools are most underutilized by systems
- How to maximize staff and patient engagement

This case study features the journeys of four such Stratum Med provider groups that implemented Deviceless RPM as the catalyst to overcome staffing shortages while extending care to rising-risk patients and preventing avoidable utilization to generate shared savings.
- Discover how Deviceless RPM strategies can increase staffing efficiency by up to 15x
- Learn from leaders at organizations in different stages of transitioning to value-based care
- Discover how Deviceless RPM can lead to improved chronic conditions outcomes and financial savings

This new e-book provides brief snapshots — one page each — summarizing the latest data and insights on important COVID-19 topics.
Topics include:
- Research shows Paxlovid cuts long COVID-19 risk
- Pediatric cases of COVID-19 jump
- How telehealth can increase access to Paxlovid
- Updates from Pfizer on boosters and a combo vaccine
- How pharmacists delivering vaccines lower healthcare costs
- The growth of new variants
- The impact of COVID-19 on gut bacteria and infections
- Data on COVID-19 and flu coinfections
- Updates on future COVID-19 vaccines and treatment

In this whitepaper, Quest Diagnostics outlines the benefits of TB blood tests, including cost-savings, patient experience and more.
Key learning points:
- How TB blood tests reduce patient visits
- The objective, accurate results provided by blood tests
- How blood tests yield cost savings for both patients and providers

This whitepaper summarizes five clinical studies that reveal how the KangarooTM feed/flush pumps with automatic flushing technology from Cardinal HealthTM are benefiting patients and hospitals.
Key learning points:
- Potential cost-savings from automated flushing
- The benefits of automated flushing vs. manual syringe flushing
- Solving for dehydration with automated flushing

Now, Gundersen is using an AI solution to automatically transcribe data in its renewal requests. This solution cuts down on manual clicks and keystrokes that can lead to medication errors and contribute to clinician burnout.
Download to learn how Gundersen has used this AI solution to:
- Improve "clean sigs" by 202 percent
- Automatically import 84 percent of prescription renewal data
- Save 100 hours of clinician data entry time
- Improve safety and decrease risk of errors

To get to a place where patients feel the level of convenience in their healthcare experience is on par with what they're used to from other industries, organizations need to craft a strategy that offers digital front doors, digital practices and personalized experiences.
This whitepaper features insights from Springfield, Mass.-based Baystate Health and Oracle Cerner on:
- Overcoming barriers in implementing digital solutions
- The features of a strong digital front door
- The difference between digital front doors and digital practices
- Building organizational culture into digital transformation

To learn more about how health systems are working to support veteran nurses and upskill new nurses, Becker's Hospital Review recently hosted an advisory call with several chief nursing officers and other clinical leaders. This report is based on that conversation. The topics covered included:
- Bridging information gaps to strengthen clinical judgement beyond onboarding
- Competency-based education focused on specific clinical environments
- Pre-skilling and immersion programs to transition nurses faster into leadership roles
- Emeritus roles for experienced nurses
Learn how leading organizations are improving nurse retention and preparing the next generation of high-performing nurses.

Is your hospital and health system’s TB screening strategy up-to-date?
Learn how leading health systems are using TB blood tests for pre-employment screens in the hiring process and to prevent post-exposure contagion.
In this new white paper, discover how new testing provide hospitals and health systems with shorter test times and lower false-positivity rates.
Key takeaways:
- Latest CDC guidance on workplace TB testing
- Benefits of IGRAs vs. traditional TSTs
- Best practices for pre-employment TB screening & post-exposure testing

This white paper discusses seven ways that mobile technology improves the intake experience for patients, providers and staff, and demonstrates why healthcare organizations that employ a mobile-first intake strategy are well-positioned to succeed in a rapidly changing healthcare system.
Read the white paper to learn:
- How embracing mobile communication helps healthcare organizations improve patient satisfaction
- Why embracing a mobile-first patient intake strategy helps providers save time and boost staff efficiency
- Tips about how to use mobile technologies to deliver the convenience and flexibility patients expect

Unfortunately, outdated interfaces turn customers away, which means more work for providers and administrators.
Health systems must look beyond basic EHR forms and cookie-cutter processes to get patients on board. The user experience is what matters. Winning organizations are using consumer-grade tech solutions that patients can navigate easily. As a result, they’re seeing fewer no-shows and higher patient satisfaction.
How do health systems with limited resources create user-friendly experiences?
In a new whitepaper, we look at how three health systems leverage intelligent automation to save time and increase revenue. Discover ways to reduce workloads by building intelligent automation into your existing EHR system.
We share how intelligent automation is helping health systems achieve:
- 8 percent reduction in no-shows
- 74 percent digital conversion rate
- 51 percent increase in co-payment
- 96 percent patient satisfaction rating

Conway (Ark.) Regional Medical Center gained more visibility into patients' status and timely, accurate alerts by partnering with Wolters Kluwer. This led to big improvements in the hospital's SEP-1 compliance rates and cost savings.
Read this Sentri7® Sepsis Monitor case study to learn how Conway Regional is:
- Identifying patients with sepsis earlier with real-time alerts and reminders that guide care
- Improving SEP-1 bundle compliance by more than 20 percent over four months
- Achieved cumulative savings of $384,000 in the four months since adopting Sentri7® Sepsis Monitor

However, despite a collective commitment to do better, organizations have lacked the technological infrastructure to enable detecting and addressing these inequities.
To shine a light on the technological infrastructure that is needed, Becker's Hospital Review spoke with David Feinberg, MD, chairman of Oracle Health, and two Indiana University Health leaders — Brownsyne Tucker Edmonds, MD, vice president and chief equity officer, and Nichole Wilson, vice president for community health operations — about the technology solutions required to addressing health inequities.
This white paper examines the:
- Foundational technological infrastructure needed to make progress on inequities – including data platforms and frameworks
- Datasets and analytics capabilities organizations need
- Talent and human capabilities required to turn data into insights and action
Achieving health equity will take more than good intentions – it requires data and a technological underpinning. Discover the technology infrastructure needed to move the needle on health inequities.

What did this survey find? A newly published ebook summarizes insights and analysis on the First Annual Health Equity Benchmarking Survey. This ebook focuses on:
- Actionable steps that healthcare organizations are taking to address health equity
- The main elements of health equity programs, budget commitments and status of the implementations
- Tools and technologies required to support organizations in achieving health equity
- Achieving health equity will take significant time, effort and investment. Discover what steps industry leaders are taking– and what your organization can do right now – to address this issue

Ascom's Challenges on The Job for U.S. Nurses survey includes responses from more than 500 nurses to give hospitals a closer look at the needs of today's nursing workforce and the main actions hospitals can take to attract and retain nursing talent.
Here's what you’ll learn:
- What are the top three workplace stressors
- How technology choices matter in deciding where to work
- Nurses' #1 rated technology tool and why it’s critical in day-to-day job satisfaction

- Amanda Loney, BScN, RN, wound, ostomy and continence consultant, Bayshore Home Care Solutions, in Mississauga, Ontario, Canada
- Abbé Benoit, BSN, RN, clinical resource specialist, Smith+Nephew
- How pain has a direct effect on the healing process
- How to determine when negative pressure wound therapy is appropriate
- How negative pressure wound therapy solutions can help to improve the patient experience
- How best practices can include use of both traditional and single use negative pressure wound therapy

A single pressure injury can cost hospitals more than $21,000 and often prolong patients' length of stay, among other unwanted outcomes. This report outlines how Mayo Clinic Florida in Jacksonville achieved a 67 percent reduction in hospital-acquired pressure injuries and a $500,000 return on investment after piloting a new system to remind employees of turning times.
Key learnings:
- The burden of hospital-acquired pressure injuries
- Key challenges in preventing the complication
- Best practices for implementing a sustainable pressure injury prevention program from Mayo Clinic Florida

This paper describes AdventHealth's approach to genomics and personalized health from both a strategic and programmatic standpoint. It includes underlying principles, lessons learned and a perspective on the future of therapeutic development.
Learning points:
- Identifying focus areas in genomics related to clinical utility
- Leveraging strategic partnerships to accelerate clinical deployment and care improvement
- Connecting genomic data with clinical data to create value from a research, discovery and data science perspective

Learn how Catholic Health System in Buffalo, N.Y., eliminated waste and cut these risks by leveraging an MME management program. This case study outlines how the health system used data to track equipment and accurately forecast utilization needs to ensure the right equipment was clean and ready for use when and where it was needed.
Key learning points:
- The improvements Catholic Health System saw in equipment utilization, cleanliness, and safety
- How the health system leveraged the program to increase staff satisfaction and face time with patients
- Lessons learned for successful adoption of an MME management system

In this white paper, learn how innovative collaborations extend the system's service lines by serving high-acuity patients at home to achieve:
- A Hedge Against Workforce Challenges and Margin Compression
- A More Cost-Effective Pathway, Solving for Repetitive Readmissions
- Appeal with Post-Covid Consumer Expectations

In this whitepaper, learn more about:
- Causes of diagnostic errors and delays
- Impacts of misdiagnosis
- How to help your staff be well equipped to accurately diagnose patients

Central to insight-driven efforts is a consumer science known as psychographics that pertains to people’s attitudes, beliefs, values and personalities. It gets to the heart of consumers' motivations, priorities and communication preferences.
Experienced healthcare leaders know that being consumer-centric is more than shifting costs and granting patients more choice and options in their care. Consumerism means delighting patients and surpassing their expectations with personalized experiences so they want to come back when the time comes in which a hospital is needed.
Psychographics have been used for decades by consumer products manufacturers and retailers, which has conditioned consumers to have higher expectations regarding products and services. Healthcare leaders must learn to take a page or two from the "consumer playbook" and develop strategies that are informed by deep consumer insights.
This report covers:
- The first Moment of Truth, when the healthcare consumer is "shopping" for a hospital and is making a decision on where to receive care services.
- The second Moment of Truth, when the healthcare consumer experiences the hospital’s services.
- Touchpoints that strengthen or detract from that brand experience.

These eight must-read Becker's articles offer the latest updates on masking in the era of COVID-19, from both an infection control and supply chain perspective. Readings include:
The value of wearing a mask when others don’t
Why did flu, COVID-19 ‘twindemic’ never happen? 1 explanation
How 4 systems keep supply issues from affecting care

To unlock the power of personalized medicine, stakeholders such as health systems, industry leaders, payers, and policymakers must work together to streamline system workflow processes and empower patients and providers. Discover how health systems can collaborate with industry to continue improving cancer diagnostics and seamlessly integrate these advancements into patient care protocols.

- See the huge impact the system made on protocol adherence and incidence of pressure injuries.
- 1 randomized controlled trial
- 7 conference abstracts
- Study results included both clinical and health economic data
The LEAF System combines wearable patient sensors with a user interface, offering:
- Personalized care for each patient
- Digital turn reminders (in room and at the nurses’ station)
- Confirmation that patient turns have sufficiently offloaded pressure
- Automatically generated reports that can be used for root cause analysis

This whitepaper uncovers insights and actions leaders can implement to surround individuals with a holistic care ecosystem — one designed to address seen and unseen drivers of health.
Explore how to:
Seize the moment for a holistic approach
Embrace a people-first plan
Connect community and key partners
Connect care in meaningful ways
Align information, resources and incentives

This guide, from Mobile Heartbeat, will take you step-by-step through the finer points of the implementation process so your clinical and operational teams are fully prepared and equipped with the necessary information for a successful deployment.
Guide topics include:
Understand the phases of implementation
How to align goals and objectives for successful implementation
Finding the right clinical communication and collaboration solution to meet your organizations needs

In the last three years, the FDA has released several updated safety recommendations regarding the potential for cross-contamination in endoscopy — first addressing duodenoscopes but now including other endoscopes.
A new, highly anticipated update to standards for reprocessing reusable endoscopic medical devices classifies flexible endoscopes as "high-risk," necessitating sterilization rather than high-level disinfection to rid the scopes of contaminants.
As increased attention is paid to infection control in hospitals, investments in single-use technology have surged. In this new report from Ambu, you will learn how sterile, single-use flexible endoscopes offer hospital systems the opportunity to provide every patient with the safest solution possible for routine, therapeutic, and emergency care.

From the ED’s unique vantage point, it is clear there is an unaddressed Care Gap costing the U.S. health care system, and all its stakeholders, dearly. Many return ED visits are preventable and involve patients who may struggle to fill new prescriptions or follow a new care plan. A recent analysis of more than 1 million patient encounters at 300 EDs nationwide found that 50 percent of hospitalizations occurred within 7.5 days of an ED discharge.
In this white paper, Randy Pilgrim, MD, FACEP, FAAFP, enterprise chief medical officer of SCP Health, identifies solutions and enumerates the benefits of narrowing and filling the Care Gap, including:
Improved patient outcomes
Decreased cost and risk
Increased capacity and optimized resources
Better performance in value-based models

With surgical site infections (SSIs) accounting for about 20% of HAIs1, it is vital to prophylactically use products that can help prevent SSIs. In this article, we’ll explore:
The prevalence of hospital-acquired infections (HAIs)
Why infections occur
Current trends in infection prevention
Iodophor vs. chlorohexidine gluconate (CHG) use cases

In healthcare, the stakes are high. Workforce shortages can translate into poor outcomes patients and intense psychological duress for nurses. Unless health system leaders find better ways to support clinicians, employee dissatisfaction, patient length of stay and the risk of missed care will increase. Leaders must pull all available strategic levers to help address these challenges. Technology can help.
This whitepaper examines strategies and tools to help mitigate the harm of critical staffing shortages. Key learnings include:
- 4 ways to decrease length of stay and address the staffing crisis
- How a seven-hospital health system reduced emergency department visits for high-utilizers by 20 percent
- How to reduce the workloads of bedside providers

Without a whole-person approach, population health will never reach its full potential of better targeting health interventions and preventing care episodes in the first place. A panel of senior healthcare executives recently convened to discuss how their organizations are considering the whole-person and opportunities to advance population health and equity goals.
This brief whitepaper presents three key takeaways from their discussion.
Key learning points:
How organizations are going beyond claims data to enhance preventive care
Improving risk stratification to address social determinants of health
Role for genomics in population health beyond cancer centers
Please fill out the form to download the whitepaper.

There are many myths surrounding personal protective equipment (PPE) today. Work with trusted experts who have the industry knowledge to help keep your staff protected at every step of the way.
Download the infographic to discover the answers to important questions including:
- When is PPE required in my facility?
- Is one piece of PPE all that is needed?
- Where can I get the PPE I need?

In this paper, see:
Highlights of the guidelines in an easy-to-read format.
A comparison between auditory cueing and wireless patient monitoring technology.
A case study showing how wireless patient monitoring improved efficiency for nursing staff and significantly reduced HAPI incidence in a 145-bed general hospital.
The first patient monitoring system designed to aid pressure injury prevention protocols is the LEAF◊ Patient Monitoring System, which combines wearable patient sensors with a user interface, offering:
Personalized care for each patient
Digital turn reminders (in room and at the nurses’ station)
Confirmation that patient turns have sufficiently offloaded pressure
Automatically generated reports

Using AccuReg EngageCare Provider for automated quality assurance, real-time eligibility and benefits verification, and price estimation and payments, KSB did the following:
- Reduced denials from 21 percent to 7 percent
- Prevented an average of $800,000 per month in denied charges—a savings of $20 million in revenue
- Improved first-pass initial accuracy rates from 63 percent to 95 percent and final accuracy from 80 percent to 99 percent
- Reduced staff turnover from 42 percent to 25 percent

Virtual nursing poses a variety of benefits for both clinicians and patients. This paper provides analysis and first-hand insight from prominent hospital systems that have successfully implemented this model. While these programs currently take place in an inpatient setting, opportunity exists to expand to outpatient and eventually home care as well, as research indicates sites of care will continue to shift toward these settings into the future.
This clinical whitepaper covers:
Survey results identify current and future trends in reimagining care delivery
The rise of the virtual nurse and how two hospitals implemented it differently
Shifts in site of care with growth in outpatient and hospital at home
Leveraging technology to reimagine who delivers care and how they deliver it
Please fill out the form to download the whitepaper.

Download this report to learn more about the impacts of delayed care and how healthcare navigation can help.
Key learning points:
- Timing matters — preventative care is critical to employees to maintain wellbeing and catch any underlying conditions early on
- The effects care delays have on both patients and clinicians
- Real-world examples of how healthcare navigation mitigates the effects of delayed care for patients.

MedHxSM, an AI-powered solution, allows pharmacists and other clinicians to spend more time providing care and less time manually gathering, entering and confirming medications.
Read the case study to see how Greensboro, N.C.-based Cone Health is using MedHxSM to:
- Gather data from 120 local and independent pharmacies
- Achieve a medication reconciliation "hit rate" of more than 93 percent
- Reduce the need for phone calls and manual entry

This report examines ~3.4 million provider ordering transactions to offer healthcare leaders a unique glimpse into laboratory utilization trends and opportunities to decrease clinically inappropriate laboratory ordering and unnecessary spend:
- Review ordering trends that are the driving sources of inappropriate laboratory utilization
- Understand the effect of inappropriate ordering on the laboratory's financial health
- Learn how to identify large financial and clinical wins across the spectrum of testing from genetics to daily labs.

These challenges threaten hospital finances, the patient experience, and quality of care. However, an often overlooked factor that plays a crucial role in ensuring success in each of these areas is the effective management of medical devices. This white paper outlines five approaches to medical device management that can positively impact patient safety and clinician satisfaction.
You will learn:
- How the effective management of medical devices can improve nurse satisfaction
- Innovative technologies that are easing administrative burdens and improving efficiency
- The consequences of non-clinical staff shortages, and recruiting and retention strategies to combat them

Click here to find out how NorthStar Anesthesia transformed the health system's preoperative processes and improved patient experience, from the leading physician anesthesiologist’s perspective.
You will learn:
- Why implementing modern preoperative processes can save time and money
- How to tailor the preadmission testing process to the procedures performed
- How an efficient preadmission testing process can improve collaboration and communication

Quick and effective antibiotic therapy in patients with sepsis can reduce the risk of death 8 percent per hour. Achieving both timely and optimal therapy hinges on a single variable — the speed at which organism identification and antibiotic susceptibility testing is produced by the clinical microbiology laboratory.
This whitepaper outlines how five health systems improved antibiotic stewardship metrics for patients with bloodstream infections and decreased length of stay by one day using rapid antibiotic susceptibility testing.

In this whitepaper, you'll learn about six key trends in patient experience, as well as how data that is already housed within your organization can be used to enhance patients' experiences, improve quality scores and increase revenue.
Download the whitepaper to learn more about the following trends:
- Growing consumerism
- Rising competition
- Reimbursement becoming tied to patient experience
- Declining reimbursement and increasing denials
- Hospitals carrying significant bad debt
- Centralized communication

Download this white paper and learn how to sustain successful hospital medicine programs. Discover:
- Improving quality of care through enhanced team culture and collaboration.
- Boosting key metrics including pre-discharge follow-up and sepsis compliance, while reducing barriers to care such as high length of stay.
- Creating facility-wide improvements through purposeful partnerships with hospital leadership and other specialty clinical departments.

National findings from the American Medical Association's recent survey of more than 1,000 residents illustrates the key stressors of today's residents and fellows. Download the summary report to learn more about these insights and discover organizational well-being resources available through the AMA Health System Program.
Key learnings:
- Do care teams feel valued by their organization?
- How is workload, work pace and EHR stress affecting residents?
- How is burnout affected by other residency experiences, like sleep and peer support?
- What organizational resources are available for improved resident well-being?

Tactically deploying newer cleaning technology that supplements established methods, can assist in the task of keeping an ultra clean healthcare facility.
Download the whitepaper to learn how Disinfection Done Right (DDR) helps implement a clever adjunctive method that is safe, requires little-to-no down time, minimal human involvement, and relatively minimal investment for air and surface pathogen reduction in hospitals, surgery centers, nursing homes, and medical offices.

Metrics tracking healthcare-associated infections and other forms of patient harm indicate multiple patient safety measures have significantly deteriorated amid the pandemic.
Key learning points:
- How persistent issues, such as staffing shortages and clinical staff behavioral health, can affect patient safety
- How bias and racism can undermine perceptions, behaviors, and outcomes related to safety
- How pandemic-related challenges affect care, including issues such as supply chain disruptions, products subject to emergency use authorization, and operationalizing telehealth
- Recommendations for systems-based approaches to eliminate risks and achieve total systems safety

This whitepaper explains how the ED improved the processes and tools used to gather a patient’s medication history to address these major sources of organizational pain.
Download the whitepaper to learn about:
- Avoiding medication errors
- Preventing adverse drug events
- Reducing hospital readmissions
- Staff satisfaction with technology

During a session at the Becker's Hospital Review 9th Annual CEO + CFO Roundtable in November, Pat Basu, MD, president and CEO of Boca Raton, Fla.-based Cancer Treatment Centers of America, and Alberto Casellas, executive vice president and CEO of CareCredit, shared observations about current financial challenges in healthcare and the importance of making the patient payment experience more modern, frictionless and user friendly.
Key learnings:
- What patients want from the healthcare payment experience
- Key payment challenges for health systems
- How Cancer Treatment Centers of America offers flexible and convenient financing options for patients

Download this white paper and learn:
- The urgency to offer highly engaging digital experiences
- Where patient engagement falls short
- The key to successful mobile strategy

This white paper outlines patients' and physicians' biggest pain points in primary care — based on a recent survey from MDVIP — and how health systems can address them through innovative primary care models.
Key learnings:
- What patients value most in a primary care experience
- Primary care physicians' top obstacles
- How health systems can better address their community's needs with patient-centered primary care solutions

Increased patient loads combined with clinician burnout and severe supply chain disruption can erode your culture of safety for routine procedures, such as injections.
The Cardinal Health Monoject Sharps Safety product division, in collaboration with Becker’s, have created an eBook depository of articles to raise awareness and provide actionable insights to enhance the culture of safety within your facility during the pandemic, despite ongoing labor shortages and vaccination administration.
Cardinal Health strives to be an industry leader and trusted partner committed to proactively delivering education and awareness as it relates to promoting a culture of safety.

Download this whitepaper to discover:
- The four challenges facing payers in delivering diabetes care
- How Integrating mental and physical health can save 16-28 percent of all costs
- How patient-centered care increases member engagement and satisfaction

North American Partners in Anesthesia worked with Raleigh, N.C.-based WakeMed Health to develop the nation's first ERAS cardiac program. In one year, the groundbreaking protocol has increased patient and surgeon satisfaction and saved the hospital nearly $2 million. Superior clinical outcomes achieved with the program also earned WakeMed Heart & Vascular the number one ranking in CMS' national outcomes listing for heart bypass surgery, and designation as the first U.S. ERAS Cardiac Center of Excellence.
This case study describes how NAPA's anesthesia leadership at WakeMed drove the clinical research, interdisciplinary collaboration, and education that inspired 100 percent participation by the medical staff and more.
Key learning points:
- How WakeMed’s cardiac ERAS program reduced patients’ ICU and hospital length of stay, opioid use, GI complications, reintubation rates, and ICU readmission rates
- How outstanding clinical outcomes increased patient and surgeon satisfaction, and produced operational efficiencies that contributed to better financial performance, including fewer patient-bed days, increased case volume, and an approximately $5 million reduction in cardiothoracic ICU insurance payments
- How NAPA’s anesthesia-driven, value-based approach promotes safer patient care and a stronger hospital balance sheet.

This report offers insights on the clinical and financial benefits of early reporting, based on an analysis of more than 31,000 national malpractice claims.
Dive into the data to learn:
- Why reporting harm early is so important
- How early reporting influences both expenses and the life cycle of a case
- The elements of a successful communication and resolution program
- How to foster a workplace culture that promotes reporting

Read how AI-driven CAPD solutions helped healthcare organizations, including Ardent Health Services and Halifax Health:
- Analyze relevant notes to identify undocumented diagnoses and comorbidities, and document them to withstand audit scrutiny
- Reduce severity of illness score by 41 percent and risk of mortality score by 49 percent
- Reduce retrospective severity queries to physicians by 63 percent

Arcadia worked with the COVID-19 Patient Recovery Alliance to analyze a massive real-world data set to identify potential drivers of the wide range of symptoms that make up long COVID-19.
Download this whitepaper to learn:
- How vaccination affects the likelihood and severity of long COVID-19
- How to use data sets to understand complex interactions and drive hypothesis creation that supports clinical research
- Recommendations for further investigation and policy work

Find out how ServiceNow® can help provide the connectivity and flexibility providers need to improve patient experiences from end-to-end, work efficiently, and securely leverage data to create value.

Although it might seem counterintuitive to solve technology struggles with more technology, sometimes it’s exactly the right fix. For example, tools that can help organize the problem list or make it easier to find pertinent patient information can enhance the EHR and decrease the amount of time spent clicking around in search of the right data.
So, what are some solutions that can help? Download IMO's latest eBook, "An unlikely remedy: How technology can alleviate the clinician HIT burden" to learn more.
Key learnings:
- How to effectively leverage the right IT solutions to lessen clinical burden
- The internal and external stressors contributing to clinical burden, and how to minimize them in meaningful ways
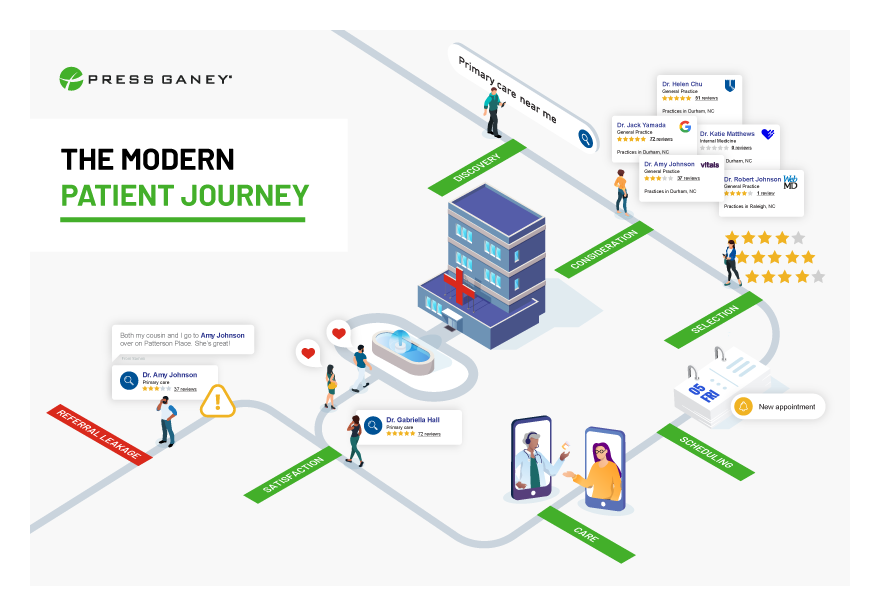
In September 2021, Press Ganey surveyed 1,000+ consumers to unlock insights into how they approach their journey to care. The findings provide a roadmap for accelerating digital transformation in 2022 and converting more care seekers into happy, loyal patients.

See how organizations across the United States and United Kingdom have used this approach to achieve measurable results and fuel a commitment to improvement that never stops. Highlights include:
- Defeating burnout with a culture of respect.
- Reducing wait times and optimizing technology by analyzing what truly adds value for patients.
- Improving equity by consistently weighing the social dimensions of policies, programs and services.

In this white paper, you’ll learn how to:
- Improve speed to care by reducing time needed to manage communication
- Instantly receive critical results, code alerts or patient communications
- Embed into the EMR, integrate with nurse call or alarm middleware
Develop a strategy for getting shared devices to nurses and equip them with the tools needed for today’s healthcare organizations.

With insight from more than 85 surgery leaders, this report takes a fresh look at perioperative leadership challenges, opportunities and priorities, including how to support a return to sustainable surgery volumes.
Key learning points:
- How to benchmark surgical productivity
- Identify the most impactful areas for improvement
- Why digital preoperative readiness is essential

Many factors contribute to readmissions, but a common thread among them is the increasing complexity of healthcare. Providers are taking on additional patients. At the same time, documentation requirements are growing, as is the need to interact with more systems and tools. The average health system has multiple different EHR systems in place across their network.
The result is cumbersome data integration and access, which creates care coordination challenges.
Many readmissions occur when patients move between care settings. Given the fragmented healthcare landscape, information can fall through the cracks, leading to suboptimal care transitions that put patients at risk.
But readmissions can be reduced by using the right care coordination tools that enable real-time data sharing and care collaboration.
The solution lies in the adoption of technology and processes that help providers at the point of care make safe and appropriate treatment decisions while providing meaningful insights to care managers monitoring patients across the continuum.

During the 2021 Precision Health Virtual Summit, a diverse group of thought leaders from health systems, providers, payers, employers, universities and start-ups reflected on the core lessons they've learned on their journey to precision health. Organizations represented at the summit included Cleveland Clinic, Danville, Pa.-based Geisinger and Danbury, Conn.-based Nuvance Health.
Download this eBook to learn:
- How to move past barriers to precision diagnostics adoption
- Approaches to leverage pharmacogenomics expertise
- How Precision Health Insight Networks are helping healthcare organizations bring precision health to scale.

Halting HAPIs in American hospitals demands attention. Recent reports from the Agency for Healthcare Research and Quality indicate that the incidence of many hospital-acquired conditions is falling. However, pressure injuries rates continue to rise despite being a top priority for health systems.
A recent survey conducted by Frost and Sullivan was designed to better understand the persistent rise of pressure injuries and examine potential solutions to the problem.
This report is based on those survey findings and in-depth interviews with 20 healthcare professionals.

Unwarranted variation can lead to inefficiencies, adverse events, increased lengths of stay, and higher mortality rates. Basically, all quality indicators are affected.
How you approach unwarranted variability can either help or hinder your efforts to improve patient care, rein in costs and thrive in this highly demanding healthcare environment. We examine decision points along the care continuum where unwarranted variability is most likely to happen and recommend actions you can take to drive sustainable and effective care.

Collective Medical believes shared success comes from those collaboration tools used in combination with data and technology sharing.
This whitepaper will cover:
- The importance of a partnership perspective
- Using care insights to drive success
- Collaboration and care insights in the real world
- How clinical collaboration groups improve stakeholder engagement across the care continuum

This move is making it clear that severe hypoglycemia related to insulin should be a never event that hospitals must actively work towards that goal by prioritizing the optimal treatment and management of severe hyperglycemia.
These measures will create the incentive for hospitals to prioritize glycemic management, which can be difficult without the proper support and technology. There are challenges to achieving optimal glycemic management, but it’s a must-have given that it benefits patients' safety and helps reduce costs for individuals, hospitals and the public.
In this whitepaper, you will:
- Learn the typical driving factors of poor glycemic management in the hospital.
- Understand the correlation between uncontrolled blood glucose and increased length of stay, cost of care and readmission rates.
- See real results from real hospitals that are using an eGlycemic Management System to reliably and consistently reduce the incidence of hypoglycemic and hyperglycemia in your healthcare system.

This new C-suite toolkit includes role specific, actionable guides with steps to help CEO’s, CFO’s, and CMO’s better understand the strategic, financial, and clinical implications of implementing health equity initiatives including:
- Defining your workforce equity goals
- Building equity into your leadership plan
- Ensuring equitable care across a diverse set of patients
- Making equity a part of your purpose and mission
- Building the business case to support resource allocations
- Addressing root causes of inequity in the broader community
- Enabling a diverse, inclusive workforce
- Activating your community relationships

In this guide, discover how to empower your clinical staff to:
- Diagnose and treat patients efficiently and effectively
- Enhance patient outcomes
- Develop advanced critical thinking skills

Learn how Carle Health and Change Healthcare:
- built a lab stewardship program that relies on CareSelect® Lab to address lab overutilization and low-value testing
- gained access to an aggregated view of its data to decide which undesirable ordering behaviors to target—and where and how to target them
- leveraged evidence-based guidelines authored by Mayo Clinic and provider communication to significantly reduce inappropriate ordering

While multimodal pain programs attempt to reduce opioids, their “one size fits all” approach is inefficient for physicians and may cause sentinel events or adverse side effects that prolong a patient’s recovery.
This case study describes how a new inpatient pain management protocol using pre-defined patient risk categories yields meaningful clinical, operational, and financial
results.
Key learning points:
- Why traditional multimodal pain programs that attempt to reduce opioids are inefficient
- The benefits of an updated inpatient pain management approach that relies on pre-defined patient risk categories
- How leveraging anesthesia expertise in this new approach to perioperative pain management saves time for busy hospitalists while improving patient safety and satisfaction

Now, it's essential for organizations to take protective steps to diversify their PPE supply chain and mitigate the risk of potential disruptions in the future.
In this white paper, you will learn:
- How the pandemic exposed PPE supply chain issues
- The importance of diversifying suppliers to increase resiliency
- Key considerations in selecting a PPE supplier

Download this e-book to see how you can:
- Connect care teams and proactively reach patients at home
- Empower every employee to address patient needs efficiently
- Personalize patient engagement using data insights

Clinical confidence may be the antidote to clinical burnout. The team at Philips aims to design technologies that increase clinical confidence by providing correct and complete information, as well as support caregiver collaboration.
Download our clinical confidence guide to:
- Bolster clinical confidence by focusing on purposeful innovation.
- Address the five leading factors that contribute to clinical burnout.
- Improve patient care, using lessons from other health systems that have leveraged technology.

Data was collected prospectively before the use of NAVIFY® Tumor Board (phase 1) through stable integration with the platform (phase 4). Data was collected across the breast, GI, hematopathology and ENT tumor boards looking at the following user groups across the institution: nurse navigators, pathology residents, radiologists and geneticists.
In this whitepaper you’ll learn:
- Positive impacts that NAVIFY® Tumor Board had on case preparation, case discussion time and case postponement rates at the test site
- Potential operational benefits seen at test site, including additional cases discussed and working days saved

However, mechanical prophylaxis, including intermittent pneumatic compression (IPC), can mitigate the risk for patients recovering at home.
Key learning points:
- Implications of the shift from inpatient to outpatient procedures and more patients heading home sooner
- Opportunities to implement at-home compression therapy for VTE risk reduction

To better understand what this shift means for healthcare supply chains, Becker's and Cardinal Health surveyed 100 C-suite and supply chain leaders from health systems nationwide in the first quarter of 2021. This research report outlines five key takeaways that emerged from leaders' responses.

Read this whitepaper to learn:
- Who is most (and least) likely to get a COVID-19 vaccination.
- Why healthcare consumers might avoid a COVID-19 vaccination.
- How psychographic segmentation can facilitate uptake of the COVID-19 vaccine.


By augmenting patient care with technology services, healthcare providers can focus on treating their patients and rely on outside experts to provide reliable communication assistance and cultural brokerage.
Here are key takeaways from this report:
- When it comes to treating LEP, Deaf and HoH patients, providers need a fast, easy-to-use solution to effectively communicate.
- Just as providers are committed to effectively treating patients, medical interpreters are committed to facilitating meaningful understanding between healthcare providers and patients from various cultural and linguistic backgrounds.
- The use of professional language services has been proven to improve the LEP patient experience and reduce the likelihood of readmissions.

But many questions remain. In this report, Optum surveyed more than 161 health care leaders from health plans, providers and life sciences and asked:
- Where are we making progress?
- What challenges still exist?
- Which areas do you prioritize for investment?


In this whitepaper, you’ll learn:
- Key AI technologies used by clinical digital assistants and what is technically possible today
- Five stages clinical assistants must go through to evolve
- Technical milestones needed to ultimately achieve a truly ambient clinical digital assistant

Find out how ServiceNow can orchestrate vaccine management, connecting workflows from distribution to monitoring, and help meet one of the most significant challenges of our lifetime.

As our country’s healthcare labor shortage looms, the need to ensure the safety of residents of all states has never been more acute.
Download this white paper to learn more about:
- The impacts of the current nursing shortage
- How a national license could improve healthcare
- Implementing a national model

Learn more about the current state of care-at-home programs and what the future may hold as two leaders from York-Pa.-based WellSpan Health shared their perspectives.
Key learnings:
- Why programs are considering switching vendors
- The future of care at home
- As the care at home model matures, health systems need enterprise solution vendors that can serve the entire care continuum

These were among the overarching themes of the recent Transform Hospital Operations Virtual Summit held during Becker's 14th Annual Meeting. Real-world case studies were presented with results that included saving OR staff 25 hours per week and achieving a $45M ROI.
In this whitepaper, you'll find key takeaways and insights from the event. Organizations represented at Transform included:
- CommonSpirit Health (Chicago)
- Oregon Health & Science University (Portland)
- NewYork-Presbyterian (New York City)

This research-based guide demonstrates how embracing hybrid care and asynchronous telehealth can help to solve healthcare's greatest challenges — like provider burnout, delayed/avoided care, health equity and more — and outlines important use cases.
Download to access:
- The basics on asynchronous virtual care and how it reduces clinician burnout and administrative burden
- Opportunities for improving patient experience and acquisition, downstream revenue and greater access for rural and non-English-speaking populations
- The largest case study on this care modality from the COVID-19 pandemic

In this whitepaper, learn how healthcare organizations across the country are deploying AI-powered technology and opportunities to improve clinical, operational and financial performance.
Key learning points:
- Three criteria for effective AI integration
- Overcoming implementation barriers
- Maximizing ROI with smart AI selection

Today, we’ve moved well beyond hype to the hope that advanced AI will be able to reshape the healthcare industry.
At Notable, we’ve spent the past eight months deploying conversational AI at patient care organizations throughout the United States, and we’ve learned valuable lessons along the way.
In this whitepaper, you’ll learn:
- Why an AI-readiness audit and strategy are essential first steps
- How conversational AI can deliver better experiences for patients and staff
- How leading healthcare organizations are putting the technology to work
- How AI is enabling organizations to rapidly iterate and optimize their workflows
- Successful approaches to programming conversational AI to meet specific outcomes

This article examines how care-at-home solutions alleviate strain by facilitating early discharges, transitional care, chronic disease management and resource optimization. Provider insights and outcomes along with market data demonstrate these programs improve capacity while enhancing patient care delivery.
Key learning points:
- Uncover the underlying challenges that are leading to constrained inpatient bed capacity
- How innovative care-at-home solutions can help unlock hospital capacity
- Insights from leading health systems about successful care-at-home programs

Becker's Hospital Review recently convened hospital and health system leaders from across the country to discuss current sentiments on AI adoption. They discussed factors driving adoption, barriers and challenges, and expectations for sustainably advancing the technology. This whitepaper offers a summary of the discussion.
Key insights:
- Health systems are taking a 'measured approach' to AI
- Advancing AI requires intentionality and metrics
- A shift is underway toward 'sustainable AI'
- Leaders expressed cautious optimism about the road ahead

However, new technology can empower clinicians to make the most of every moment by delivering real-time, data-driven insights to the bedside. Having a digital view into each patient's clinical story as it's happening can support swift, effective decision making in the moments that matter most.
Read this white paper to learn more about the potential of these technologies to reshape critical care.

Increasingly, ORs are outfitted with robotic surgical systems. When managed effectively, these systems can support efficient care delivery and quality surgical outcomes. However, they are significant investments — a single robot can cost as much as $2.5 million to purchase, while maintenance, supply, and leasing fees can mount up over time. To maximize the return on investment for surgical robots, hospital leaders must use a data-driven and strategic approach to optimize their efficiency. This playbook details the "magic equation" — of AI-powered automation, integrated workflows, and change management — needed to achieve that goal.
Learnings include:
- How to leverage data, AI-powered automation, integrated workflows, and change management to drive improved robot utilization and ROI
- A checklist of exactly what health systems need from an effective robot utilization solution
- Case study: How Baptist Medical Center Jacksonville (Fla.) delayed spending on additional robots

Healthcare government organizations face numerous challenges in meeting their healthcare mission, including the need for secure and compliant sharing of personal health information across multiple devices, users, and locations. In this eBook, learn how partnering with Lumen can provide your healthcare agency with the talent, expertise and infrastructure needed to unlock the full potential of your data and rapidly adopt game-changing technologies. Take advantage of the full range of capabilities needed for success in a digital-first business landscape, delivered in a simple platform approach that makes it easy to manage IT operations while also potentially reducing costs.
Key learnings:
- Unlock the keys to a winning digital transformation strategy across multiple business locations
- How to optimize omnichannel and deliver exceptional digital and physical healthcare experiences
- Explore ways to mitigate supply chain and cybersecurity risks

Effective clinical decision-making and treatment plans often hinge on data from diagnostic laboratories. But for many healthcare organizations, the patient data clinicians need is fragmented and siloed, making it difficult to integrate or match to the right patient — which can have severe consequences.
This whitepaper highlights Sonora Quest Laboratories' digital transformation journey to drive interoperability through identity data management. Sonora Quest Laboratories is a large, integrated diagnostic lab and joint venture between Phoenix-based Banner Health and Quest Diagnostics.
Download to learn:
- Challenges Sonora Quest faced in data identity management, per their CIO
- Four key takeaways from Sonora Quest's digital transformation + real results they achieved
- Best practices for improving patient matching technology

The mindset toward health IT is changing for many healthcare leaders. Organizations benefit by steering away from the “necessary expense” perspective to consider IT as a strategic asset. When this mindset is embraced, health IT is a powerful enabler for truly scaling and achieving operational efficiency across the enterprise.
This brief report discusses how leveraging health IT through comprehensive managed services can achieve sustainable growth.
Key learning points:
- Leveraging IT as a true asset to transform how care is delivered and overall operations
- How providers should strategize through partnerships to secure the greatest possible total value for their systems over time, instead of prioritizing the greatest short-term savings
- Examples on how a comprehensive managed services strategy provides opportunities for scale that aren't typically possible when IT delivery is solely handled in-house

Despite AI's meteoric rise in popularity across industries, healthcare has lagged behind on adoption, with 60% of leaders reporting their company is not moving quickly enough. At the same time, 86% of leaders believe the ability to effectively leverage tech, data and AI will define success over the next five years, meaning organizations need to bridge the gap quickly.
With healthcare's privacy, regulatory and security concerns adding a layer of complexity to AI implementation, the right third-party AI partner can offer a path forward — but healthcare organizations need to know what to look for. This whitepaper uses findings from a survey of healthcare leaders to examine AI adoption, barriers and factors for a successful AI partnership.
You'll learn:
- Where other organizations are in their AI journey
- How to lay the groundwork for successful AI adoption
- How to choose long-term partners to support AI growth and ROI

By now, healthcare leaders are familiar with AI's potential to alleviate documentation burden, lighten clinicians' cognitive load and streamline operations overall, but only 6% of organizations currently have a generative AI strategy in place.
Many leaders have been overwhelmed by how quickly the technology has burst into the public consciousness and the hype surrounding it. Hospital leaders need clarity on generative AI’s risks and use cases if they’re to create a successful strategy, and apply the technology safely and effectively.
In this guide, we look beyond the hype to explore five key areas every healthcare organization should consider when developing an AI strategy and assessing potential vendors’ solutions.
Key learning points:
- Criteria to look for in a vendor to ensure their solutions fit daily practices in healthcare
- Crafting a responsible approach to AI
- How to prioritize solutions that can be deployed effectively in real-world environments

Transforming the Cerner patient intake and registration process is not just an option, it’s a necessity.
63% of patients say their provider’s digital tools have not met their expectations and 41% of patients have switched providers due to a poor digital experience.
This guide provides a detailed look at the strategies other organizations use to deliver exceptional digital experiences with Cerner.
Why this guide?
- Innovate with confidence: Learn from a comprehensive analysis of successful Cerner-based digital transformations in patient engagement, distilled into actionable insights.
- Drive efficiency and enhance satisfaction: Uncover secrets to reducing administrative burdens while significantly improving patient and staff satisfaction.
- Stay ahead of the competition: From using AI and automation to integrating patient feedback loops, discover the approaches leading Cerner-based healthcare organizations are taking and the results they’re driving.

But there are significant challenges to tackle in order to get there, especially surrounding data ingestion, model training and validation. This white paper shares how healthcare organizations are deriving useful insights from complex imaging data.
Key learning points:
- Potential use cases for medical imaging AI
- How to build reliable, scalable solutions for managing complex data
- How analysis-ready data repositories promote rapid AI development

With over 100,000 procedure codes from three different coding systems currently in use, having consistent and complete mappings is critically important. This white paper details the best way to get the most out of your coding data.
You will learn:
- What service line groupers are available in the market today
- The types of coding systems
- How better grouping can help your system harness growth opportunities, target consumers and conduct market planning

This guide provides six actionable strategies that enhance patient access, communication and readiness based on insights from more than 700 million data points collected across 650 healthcare organizations like Fairview Health Services (Minneapolis) and UW Medicine (Seattle). It also covers improvement opportunities for critical areas such as self-scheduling, rescheduling, response rates, care follow-up and referral outreach.
Download to learn how to:
- Implement user-friendly, self-scheduling options that significantly improve patient access to care and reduce administrative workload
- Simplify the rescheduling process and use direct communication methods like SMS to greatly increase patient engagement and reduce no-shows
- Gather and act on real-time patient feedback to be able to improve patient satisfaction and enhance the overall healthcare experience

Becker's spoke with leaders from Salt Lake City-based Intermountain Health and Ottawa (Ontario) Hospital about how they're using a one-stop-shop data infrastructure to quickly get answers and action items for critical operational, research and innovation-related questions. This whitepaper offers a summary of the discussion.
Key learnings:
- The advantages of a comprehensive, real-time synthetic data platform
- Real-world case studies from Intermountain and Ottawa Hospital

But how prepared is your organization to harness its full potential?
Discover the roadmap to not just surviving but thriving in the age of AI.
- Combining insights gleaned from leaders at dozens of health systems with the experience of deploying AI to thousands of care sites, this guide covers:
- Why AI’s moment in healthcare is now
- 10 essential elements for building and deploying an enterprise-wide AI strategy
- How to ensure your AI efforts remain aligned with your business strategy

This whitepaper uses responses from recent a survey of healthcare CEOs, CFOs, CIOs, virtual care leaders and other decision-makers to detail three valuable insights on the current state of telehealth and how organizations can maximize results from their offerings.
You will learn:
How other health systems are using telehealth to overcome today's challenges
Where telehealth is headed in the future
How to overcome obstacles like user adoption, payer alignment and technology infrastructure

In this white paper, you'll learn four key components — which emerged from a roundtable discussion with hospital and health system CEOs and CFOs — to drive sustainable improvements with automation and ensure return on investment.
Download for more insights on:
- Trends in automation investments and complexity
- Opportunities for improvements in clinical quality, productivity + revenue integrity
- Four critical components of an effective automation strategy

In this white paper, top clinical leaders from Salt Lake City, UT-based Intermountain Health and Durham, NC-based Duke University Health System share how their systems are embracing new technologies to support nurses while improving operational efficiencies and the patient experience.
Key learnings:
- Why systems are increasingly investing in technology that aids nurses
- How AI technology can support multiple aspects of nurses' jobs and roles
- Key considerations for thoughtful technology implementations

- One of the most promising potential applications is streamlining important, but time-consuming, administrative responsibilities of health care workers. Health systems can benefit their staff and patients by focusing on AI adoption that enables clinicians and technicians to focus more time and energy on activities with the greatest impact on direct patient care.
- One of the top priorities evaluating the role AI in health care is scalability. With technology tools that effectively handle large volumes of data, health systems can increase efficiency for rapidly expanding areas of responsibility, such as tracking and managing large medical device inventories.
- The rapidly evolving capabilities of AI and growing number of software products emphasize the need for strong process governance, especially in fields such as clinical engineering which already engage with complex, critical technologies.

In this white paper, you'll learn how hospitals and health systems are leveraging a single technology platform to enhance patients' care experiences across all settings, as well as save costs, reduce burden and drive innovation.
See how this approach enables:
- Value across each step of the patient journey, from at home care to the patient room
- Improved daily workflows with apps and integrations
- Innovation with new technologies like artificial intelligence and more

With technologies like artificial intelligence, machine learning and analytics, over 1,000 hospitals and centers have discovered that it's possible to know what's coming and align healthcare assets with staff and patient demand. The result is increased efficiency, improved provider satisfaction, reduced labor costs and fewer delays in patient care. These were the major themes that came to the surface during two recent virtual summits: Transform Hospital Operations and Transform Infusion Center Operations, hosted by Becker's Healthcare and sponsored by LeanTaaS.
This recap examines the key learnings from these five virtual summit sessions:
- Increase ROI Through AI: Unlocking Scarce Capacity and Staffing
- Make AI Work for the Workforce: Empowering Staff and Systems to Thrive
- Optimizing OR Flow: How Data-Driven Insights Help Anesthesia Groups and Hospitals Work Smarter, Together Featuring UCHealth
- Transforming Performance: Uniting AI, Automation and Change Management Featuring Baptist Health Jacksonville
- Resilience in Action: Infusion Centers as Catalysts for Innovation, Featuring Duke Health

Healthcare organizations are now ramping up efforts to consolidate scheduling and communication functions by reducing their vendor footprint. The result? Lower IT burden, lower costs and better clinical outcomes.
See why hospitals are turning to a single platform to make scheduling, communication, and patient care workflows easier. This paper covers:
- The key roadblocks organizations face when it comes to communication and technology
- How 1 standardized platform enhances clinical collaboration, scheduling and patient engagement
- Navigating seamless integration

Preparation efforts paid off for the University of Arkansas for Medical Sciences in Little Rock. The system saw an 187% increase in telemedicine activity after a severe weather event impacted local patients and providers. Through proactive communications, UAMS shifted all in-person patient visits to virtual, resulting in zero missed appointments during the period of severe weather.
Download this case study to learn:
- The role telemedicine plays in safeguarding health systems when disruptions happen
- The importance of proactive planning and communications in disaster management
- What capabilities and features providers should look for in telehealth tools

This white paper covers key insights from a recent advisory call where AI and health system leaders discussed the most important factors that must be considered when applying AI-powered tools to different areas of healthcare.
Learning points:
- Healthcare organizations are adopting AI to improve clinical and operational workstreams
- The set of key criteria organizations should keep in mind when evaluating potential AI partners
- C-suite leaders' thoughts on painting tools that will make real improvements

In this white paper, you'll learn how RPM, when implemented as part of a value-based care (VBC) approach, can effectively address obstacles to care and social determinants of health (SDoH).
Download to learn more about:
- The opportunities RPM and VBC offer federally qualified health centers (FQHCs), rural health centers (RHCs) and critical access hospitals (CAHs)
- The range of benefits (health, social, financial, organizational) that are possible for care providers and patients through the use of RPM and VBC models
- What healthcare policymakers and providers can do to promote wider adoption of telehealth and RPM services to better care for patients beyond in-person care settings

Demands on IT service desks in healthcare have grown immensely over the last five years. They're supporting higher volumes of applications, a constant stream of new technologies and myriad new devices that require IT maintenance. At the same time, the resources, headcount and budget provided to IT are constricting.
To better understand the challenges facing IT leaders, as well as the most promising solutions for addressing them, Becker’s Healthcare took a look at how the role of automation in optimizing IT operations and how, with the right platform, the benefits of IT service management (ITSM) modernization can span the enterprise.
Read this short report to learn:
- The types of solutions CIOs should look for to address IT challenges and alleviate resource strain
- Best practices to determine where AI has the most potential to transform operations and optimize efficiency
- How IT teams can leverage conversational AI to reduce service request burden

Health systems such as CommonSpirit and Novant Health are now tapping into predictive & prescriptive machine learning analytics to address these challenges. Using a new data-driven and strategic approach, these organizations are able to enhance block utilization, streamline scheduling processes, optimize resources like staff and robots, and accommodate varying surgical volumes to improve overall perioperative performance.
Download this case study booklet to learn how 100 health systems from across the country are using this strategy to optimize OR performance and achieve the following results:
- Perform 30-50 more cases per year
- Increase block utilization by up to 20%
- Increase robot utilization by 45%
- Increase case volume by 10% or more without opening additional rooms
- Generate 5-20x ROI based on contribution margin

It also demonstrates how adaptable data systems can support VBC by facilitating the delivery of higher-quality care, while mitigating the burden of soaring healthcare costs.
Key takeaways:
- Recent innovations in health data management are driving the evolution towards emerging models and frameworks for healthcare integration and delivery
- How AI can optimize and future-proof data by enhancing the accuracy and efficiency of healthcare processes
- The importance of choosing a trusted health-specific platform that focuses on data unification

In this white paper, you'll learn how information and technology executives at El Segundo, Calif.-based Pipeline Health — an independent network of community hospitals — revamped the health system's IT department to better support the workforce.
You'll learn more about Pipeline's approach to:
- Getting value out of IT investments without compromising performance, amid rising costs
- Pulling cross-departmental teams together to problem-solve
- Empowering IT teams by bringing in clinical experience, support + a customer service mindset

In this white paper, you'll learn how to overcome common barriers in this area of care with strategies to lead, collaborate and invest in a new, proactive approach that better supports current mental health needs.
Download to gain a deeper understanding of:
- Cost of the mental health crisis in all areas of society
- Importance of aligning financial incentives
- Required investments for a new experience
- How healthcare stakeholders can take new action

It's not viable or realistic for healthcare organizations to tackle today's complex problems alone. This whitepaper report breaks down some of the top concerns from healthcare leaders today and details how the right partner can improve outcomes through greater access to person-centered care and reduce costs by accelerating the digitization and utilization of healthcare data.
You'll learn:
- The top four issues healthcare leaders are focusing on right now
- Strategies and outcomes from leading healthcare organizations
- What to look for in a strategic technology partner

Patients are still frustrated with roadblocks to accessing care, and staff are doing more data entry and other manual repetitive tasks than ever before.
Digital transformation was supposed to bring healthcare into the modern age, but the industry is still burdened by processes like clipboards, faxes, and never-ending manual work queues.
But, there’s a shift happening - thanks to AI and automation. This guide covers:
- Key indicators of an ineffective digital front door.
- Proven strategies from top healthcare organizations for an efficient, AI-powered digital front door that benefits patients and staff.
- How conversational AI is revolutionizing patient navigation in healthcare.

This whitepaper explores 5 key industry trends driving the shift to more personalized care, how companies can respond, and the role technology plays in that response. It covers what it will take for the industry to make good on its promises to deliver better outcomes and more cost-effective care, and the steps individual companies can take today to accelerate progress on personalized care.
Learning points:
- 5 key trends amplifying the importance of patient-centric care
- How healthcare companies can respond to deliver the experience patients expect and improved outcomes
- How integrating technology and data-driven insights is revolutionizing the patient-provider relationship and setting the course for the future of healthcare

- Patient Experience: Generative AI can be used to create personalized and conversational experiences for patients. This includes answering questions, booking appointments, and providing care guidance.
- Care Team Efficiency: With generative AI at their side, health providers can automate tasks such as note-taking and patient outreach, freeing up care teams to focus on more important tasks.
- Care Guidance: Generative AI can be used to provide patients with personalized care guidance, such as medication reminders and disease management tips
This report examines how to overcome barriers to technology integration and realize the promise of generative AI sooner rather than later.

This report explores how healthcare organizations can adopt new technology to improve tumor board workflows, optimize care decisions and prevent treatment delays.
Learning points:
- Best practices for the successful implementation and use of digital tumor board solutions
- Key benefits of the solutions based on real-world implementations

In this paper, you’ll learn how this monitoring technology leads to improved care coordination, more efficient patient workflows and throughput, reduced care costs and better patient outcomes for AF and stroke.
1. Wei M, Do D, Tang P, et al. Optimal disposition for atrial fibrillation patients presenting to the emergency departments. J Am Coll Cardiol. 2018;71(11):A509. doi:10.1016/S0735-1097(18)31050-7

Most facilities management teams at mid-sized or large healthcare organizations rely on various technologies to mitigate risk and boost facility performance. But despite the advantages these technologies deliver, it's impossible for facilities management professionals to fully excel without intensive training.
Wherever your organization is on its technology journey, take steps to achieve a better return on investment from your facilities management technology. Download the guide for key considerations on optimizing your technology to:
- Achieve facilities compliance, maintain accreditation and reduce risk
- Boost performance and reduce costs
- Enhance the employee experience

In this paper, you'll learn four takeaways from an exclusive discussion with hospital and health system leaders, where they candidly shared how they're navigating challenges and lessons learned at various stages of digital transformation. Key points:
- Components of a true digital mindset
- The foundation hospitals + health systems need to meaningfully innovate
- The role of technology in access-to-care disparities
- Opportunities in patient engagement

A persistent challenge that has emerged for leaders, however, is change management — and whether they have the required expertise to allow the capabilities and culture of innovation to take root and spread broadly across clinical, revenue cycle and other operations.
In an executive roundtable at Becker's Health IT + Digital Health + RCM Meeting, Daryle Abrahams, a change effectiveness consultant and leader at DXC Technology, moderated a discussion with three healthcare technology leaders:
- Edward Kim, MD, physician-in-chief and senior vice president, City of Hope Orange County (Irvine, Calif.)
- Marty Sheetz, vice president, business implementation and operations, Delta Dental
- Paul Williams, associate vice president, infrastructure technology, Penn Medicine (Philadelphia)
In this white paper, you'll learn:
- Why behavioral change is often necessary to drive user adoption of new technologies
- Why technology-driven initiatives face multiple challenges, both old and new
- How intrapreneurship can spur innovation

Today, the system has implemented digital scheduling, automated registration and intake, automated care gap outreach, and more, with far-ranging effects across patient and staff experience, as well as financial and care outcomes.
This whitepaper:
- Reveals how performance metrics changed over the course of two years
- Details how frontline workers and clinic managers have responded to the new technology
- Shares the real, human impact of AI and automation on care outcomes

The operating room is a powerful place to begin on this journey, as ORs can generate up to 70% of a hospital's revenue and up to 40% of its expenses. The potential to drive further revenue in the OR through increased case volume, while optimizing resources and staff, is enormous.
This whitepaper offers healthcare leaders a roadmap to identify OR inefficiencies and address them using a "magic equation" of artificial intelligence, automation and change management. The roadmap also includes case studies from Baptist Health Jacksonville (Fla.) and The University of Kansas Health System in Kansas City.
Key learnings:
- 10 ways to identify OR inefficiencies
- Best practices for using AI, automation and change management in the OR
- Real-world results from Baptist Health Jacksonville and The University of Kansas Health System

The challenge requires community hospital leaders to ensure they're adopting technology solutions that are strategic, cost effective and efficient.
This whitepaper offers a roadmap for IT infrastructure investment to help leaders identify and implement solutions that will support their organizations' clinical, business and security needs.
Key learnings:
- How to evaluate evaluate potential IT investments
- The business case for replacing legacy systems and other outdated IT solutions
- 7 steps to a successful IT transformation

Healthcare organizations experienced 1,426 cyberattacks per week in 2022, a 60 percent jump from the year prior, according to data from Check Point Research. As of July, the average cost of a healthcare data breach was $10.9 million — the highest of any industry, a separate report from IBM Security found.
This whitepaper offers a state of the union on healthcare cyberattacks in 2023, examining their rising prevalence and how health systems can work to prevent them.
Key learnings:
- The prevalence of healthcare cyberattacks
- 5 ways to protect against cyberattacks
- The role of cyber insurance

With artificial intelligence, anomalous billings can be flagged or auto-denied, enabling investigators to focus on high-value, complex cases.
What if you could continuously monitor provider behavior and risk levels, manage daily billing fraud risk in real time and access pre‐pay analytics to identify FWA before claims are paid? AI for healthcare fraud detection can do all this and more.
Read this e-book to learn:
- How AI optimizes workflows by triaging good, bad and suspicious claims
- Why higher detection rates and fewer false positives helps teams focus on more complex FWA schemes, resulting in substantial savings
- How models are continuously trained, evolving with schemes as they arise

This white paper explores how hospitals can use automation to reduce stress on nurses, while also improving patient experience and outcomes. See how a blended nursing strategy using bedside nurses, virtual nurses and documentation automation can increase team members' efficiency, reduce procedural errors, and give patients more facetime with caregivers.
Learn how this approach can:
- Shrink length of stay by 90 minutes
- Cut patient sitting hours by 48 percent
- Reduce patient falls by 60 percent

In this e-book, you'll see key takeaways from a survey of more than 190 clinical, administrative and IT leaders on their current approaches to AI and perspectives on what this technology means for the future of healthcare.
Read more to learn:
• How leaders believe AI can help achieve strategic objectives
• The current state of this tech at organizations surveyed
• Privacy, security and ethical concerns + pathways forward

In this white paper, you'll learn key insights from a roundtable discussion with Intermountain Health (Salt Lake City) and Inland Empire Health Plan (Rancho Cucamonga, Calif.), where technology, nursing and medical leaders shared how they're tackling data issues, where they're seeing successes in addressing social determinants of health and what they recommend to other organizations striving to do the same.
Key learning points:
- Challenges in gathering essential SDoH data
- Benefits of real-time data feeds and reports
- Key elements of a successful population health program and building community trust

Despite the high demand for behavioral healthcare services, many face barriers care. To make real change, it's essential to identify and reduce the root causes of mental health inequity and expand access to meet the mental health needs of every individual.
This mental health series for healthcare executives explores how to close the information gaps in mental and behavioral health data, uncover and conquer the root causes of mental health disparities, and evolve to meet an ever-rising mental health demand.
You'll learn:
- 4 steps to assess and improve the quality of your mental health data
- 7 tips for improving health equity and care access
- How to guide your organization through adapting to new strategies and customizing the mental health experience to fit each unique individual

The program is a model for how virtual care can be used to improve stroke care. This approach has the potential to save lives and improve the quality of life for stroke patients.
In this whitepaper, healthcare leaders will learn:
- How the organization implemented a 24/7/365 telestroke program.
- How the program has allowed Hackensack Meridian to improve its stroke response times and treatment rates.
- How the program provides a more coordinated and efficient approach to stroke care, which can lead to better outcomes for patients.

Learning statements:
- Learn about the challenges impacting health system executive decision-making.
- Explore five steps that health systems can take to better inform stronger executive decision-making.
- Review how health systems can achieve better organizational outcomes by formalizing visibility and standardized processes in their clinical asset management strategy.
By harnessing the power of actionable data, health system executives can navigate the challenges of today's healthcare landscape with confidence, drive positive organizational outcomes, and usher in a new era of excellence in patient care and operational performance.

That has major implications for healthcare organizations. Patients with language barriers experience reduced quality outcomes — including 1.5 days longer length of stay and 9.4 percent higher readmission rates than English-speaking patients.
This report explains the value of a robust language access program that goes beyond simple compliance and delivers real financial value for the business and better outcomes for the patients.
This short report will cover:
- Improving reliability
- Reducing costs
- Increasing revenue

In this research-based white paper, you'll learn:
- The current state of instrument sterilization quality + deficiencies at most hospitals and ambulatory surgery centers
- Why the design of reusable surgical instruments makes it challenging to reliably clean them
- Recommended paths forward, including transitioning to single-use, sterile, pre-packaged instruments
Source: Surgical Site Infection (cdc.gov)

This e-book highlights insights from the Becker's Healthcare-Biofourmis leadership survey on the current state of the home-based care paradigm, as well as Augusta (Ga.) University Health's experience implementing a care-at-home strategy.
You'll learn:
- Leaders' target areas for remote care programs
- Top barriers to adopting these initiatives
- How Augusta University Health approached operational barriers + is seeing reduced length of stay and readmissions

But that’s going to change, rapidly.
If you’ve heard the generative AI hype, but aren’t sure where to get started, or if you’re on the fence about the real-world implications of LLMs, this is the resource for you.
Discover:
- How advanced AI technologies are being deployed by health systems to personalize the patient experience at scale
- The right use cases for implementing these technologies in support of the existing healthcare infrastructure and teams
- Practical applications for generative AI and large language models in healthcare

In the 21st century, medical imaging is again experiencing a leap forward. New imaging technologies will allow for more detailed pictures of patients’ tissues and organs — perhaps even at the cellular level.
Technologies powered by artificial intelligence and machine learning also have the potential to detect health issues, such as stroke or heart attack, sooner. Machine learning can also support physicians with real-time feedback as they review images.
Collectively, these solutions could improve speed to diagnosis and treatment which would ultimately improve patient outcomes.
Maintaining, growing and securing on premises data storage presents major challenges for hospitals and health systems in such an environment.
Enter the cloud.

In this white paper, you'll access insights and best practices from mobile technology experts and leadership at Driscoll Children's Hospital (Corpus Christi, Texas) on smart tactics for deploying AI in healthcare to ensure it delivers accurate information and value.
You'll also learn:
- The many pain points in healthcare that AI can address — if deployed thoughtfully
- Two areas leaders should assess before implementing
- New tech, as well as essential regulatory and oversight concerns
- How to ensure your organization's network will support AI traffic + the role of 5G

These issues coupled with workforce gaps demand that hospitals and health systems use technology now to more effectively manage staff and reduce administrative burden. In this research- and case study-backed paper, you'll see how systems like Baptist Health (Jacksonville, Fla.), Health First (Rockledge, Fla.) and Oregon Health and Sciences University in Portland have embraced this method and realized better clinical outcomes.
Download to learn:
- How artificial intelligence and predictive analytics can activate the workforce, support inpatient staffing and help organizations prepare for lingering shortages
- Benefits of technology applied to infusion centers and operating rooms
- Key steps and results from systems like Baptist, which saw 40 percent reduced call volume after using electronic case scheduling at their largest hospital

The model shows how healthcare monitoring is advancing from basic alarms to more sophisticated "smart alerts." These smart alerts utilize high-fidelity, live streaming medical devices data and consider critical patient information like demographics and test results to provide more useful warnings.
The Clinical Surveillance Maturity Model's ultimate goal is to help improve patient safety and outcomes by aligning alerts with evidence based clinical practice guidelines and using advanced technology such as machine learning and artificial intelligence for better and more precise monitoring.
Key learnings:
- How the Clinical Surveillance Maturity Model tracks the progression from basic medical device alarms to more advanced, context-rich smart alerts in health systems.
- What it takes to develop and adopt smart alerts
- Why clinical trust in the smart rules is crucial for successful adoption.

Healthcare leaders are increasingly leveraging remote patient management programs to improve access, affordability, and equity for patients. The evidence demonstrates these programs can achieve these goals while also improving clinical outcomes and lowering the cost of delivering care. Technology is obviously a critical enabler for this care model. But staffing, logistics, supply chain, patient selection, and other “non-tech” considerations remain a challenge and cannot necessarily be solved with wearables or artificial intelligence. This whitepaper outlines six strategies hospitals can take to overcome such obstacles and realize the value of a remote patient management program.
Whitepaper key takeaways:
- Going beyond the tech to focus on the importance of in-home care coordination
- Patient selection as an important part of scaling up care an RPM program
- How to generate clinically actionable insights instead of data
- Considering access and care equity as an objective

Becker's Healthcare and AWS Marketplace collaboratively surveyed 115 healthcare leaders on their organizations' journeys to better technology offerings and capabilities, as well as where key barriers and opportunities lie.
Download to learn:
- The top three areas where leaders are hoping to make the biggest impact via digital innovation
- Planned investments in enterprise applications over the next year and beyond — and what this trend indicates
- Progress, challenges and outlook on artificial intelligence

In this vein, advanced analytics, artificial intelligence and other technologies are showing promise. To successfully transform their organizations, however, healthcare leaders must also identify the right sources of data, get key stakeholders excited about the possibilities and identify projects that will deliver quick wins. This white paper explores how systems such as CommonSpirit Health and Intermountain Health are doing just that.
Key learnings:
- How leading systems are reimagining hospital operations with AI
- Three key elements for a successful capacity management improvement effort
- The future of capacity management

Key Learning Points:
- Explore how technology, automation, and standardization can alleviate clinician burnout and resource constraints in healthcare organizations
- Why patients are an "underutilized resource in healthcare" and how digital processes fit in here
- Best practices for accelerating adoption of new technology, for organizations of any size
- Discover the impact of ambient intelligence in reducing administrative burdens and how generative AI optimizes the clinician experience, transforming healthcare delivery

This white paper features insights from an exclusive discussion with hospital and health system leaders on their respective journeys to achieving health equity via community partnerships, data and technology.
Read more to learn:
- Why organizations should strive to advance health equity and health justice
- How an equity lens should be applied to the use of technology in healthcare delivery
- The data and interventions some hospitals + health systems are using, such as local partnerships and patient advisory councils, to narrow health disparities

Telemedicine allows patients to receive medical advice, diagnosis, disease management and treatment from the comfort of their homes. With 88 percent of surveyed physicians believing telemedicine increases patient access to healthcare, it is clear why it has been pushed to the forefront of care delivery.
This report examines the continued adoption of telemedicine, its applications across various specialties and healthcare services, and its effects on physician well-being, patient access and continuity of care.
- Three of the many questions that will be answered in this report:
- Which specialties are most likely to use telemedicine and why?
- How often do physicians use telemedicine in their practices?
- How has telemedicine affected patients' adherence to treatment plans?

This white paper shares findings from a survey of over 200 IT, security and compliance leaders in the healthcare industry.
Learning points:
- Truths about healthcare providers' cloud cybersecurity hygiene and investments, revealing an industry that is significantly unprepared and overconfident
- Top barriers to cloud adoption for healthcare providers who prioritize cybersecurity
- Proactive steps taken by healthcare providers to increase cybersecurity budgets, protect patient outcomes and remain compliant with evolving regulations

In this e-book, you'll learn key findings from the Becker's-TigerConnect 2023 medical and nursing leadership survey, which captured perspectives from more than 100 clinical leaders on the current state of clinical communications and how communication tools impact day-to-day clinical workflows.
You'll learn:
- How traditional communication tools in the clinical workflow, like email and phone calls, are tolerated by nearly 40 percent of survey respondents — and why this is an issue
- The unrealized need for processes that analyze efficiency of clinical workflows + the recommended measures for tracking improvements
- What hospitals and health systems can do to streamline communications and improve patient outcomes

In this Zoom white paper, you'll learn how collaborative platforms are increasingly supporting clinical and business operations at life sciences organizations, including how one pharmaceutical company is seeing success in staff engagement and physician education.
Read more to discover how this technology:
Enables organizations to fast-track vaccine and drug development
Addresses some of the biggest challenges that life sciences organizations face, like connectivity, data sharing, clinical trials and staffing
Promotes innovation and go-to-market, and advances research

However, HIPAA isn't static, and maintaining compliance requires staying up to date with changes in the law, which creates an additional burden for providers who should be focusing on patient care.
A secure cloud communications platform is key to fostering collaborative communication between providers without fear of violating HIPAA. Download the white paper to learn how to:
- Connect care teams and patients on-site or via telehealth
- Reduce costs through better collaboration with payers
- Keep patient data secure and care team communication HIPAA-compliant

This white paper details a conversation with a group of healthcare leaders about their approach to AI, the benefits they're seeing in leveraging technology and what they think other leaders should consider before implementation.
You'll read about:
- Why investing in technology — despite budget challenges — is important
- The AI frameworks and capabilities that are still missing across the industry
- How some technologies are unburdening staff and enhancing patient care

Healthcare organizations today are reimagining their digital strategy to better support the increased demand for telehealth, and ensure it is accessible to as many patients as possible.
As healthcare technology continues to advance rapidly, it is crucial to stay up to date with the latest telehealth and technology integrations while still maintaining patient privacy and information security.
Key learnings:
- Why future iterations of telehealth technologies must be simplified
- How an increased demand for telehealth caused organizations to reassess their digital strategies
- The importance of a laser-sharp focus on data security and compliance
- Technologies that can propel the patient journey forward

Technology advancements are enabling the healthcare industry to sooner identify and break SDOH-related barriers to care, quickly connect individuals to appropriate resources and optimize engagement to ensure individuals receive the support they need.
This report outlines the many benefits of implementing tech-enabled SDOH interventions to improve health outcomes and reduce hospitalizations, readmissions, emergency department use and costs.
Read more to learn how to:
- Proactively identify SDOH risk factors and connect individuals with appropriate resources sooner.
- Get a more complete picture of an individual's health by leveraging integrated, tech-first tools.
- Track referral status in real-time to close the loop on SDOH referrals and measure the impact of your efforts.

But it doesn’t have to be this way. There’s now a proven playbook for moving beyond the call center to something far better for patients and providers.
This whitepaper:
- Examines findings from a nationwide survey of patient access leaders on scheduling
- Unpacks the differences between what providers provide and what patients want
- Details how two health systems have increased appointments, slashed staff time spent on scheduling, and improved patient satisfaction through intelligent automation

Most technologies in healthcare aim to make things easier for workers and patients, and lower costs. But it's up to organizations to take a thoughtful implementation approach in order to realize these benefits.
Read takeaways from a workshop at the Becker's Hospital Review 13th Annual Meeting where two experts shared how organizations can approach tech investments in a manner that will actually alleviate pressures, not add to them.
Learning points:
- Avoid haphazard tech implementation
- Engage clinicians in the tech investment + implementation processes
- Define and tracking success metrics

This whitepaper explores how leading health systems are leveraging intelligent automation, large language models (LLMs), and generative pre-trained transformer (GPT) technologies to finally realize the potential of patient data.
Discover how:
- One health system reduced no-shows by 8%, leading to $2M in annual cost savings
- Another health system deployed advanced technology to deliver a 50% decrease in eligibility and registration-related denials
- Yet another health system drove $840K in annual cost savings from a 23% reduction in no-shows and cancellations

Securing the internet of medical things requires a new strategy and coordinated approach as more devices hit the market and health systems continue to consolidate.
In this whitepaper, you'll learn:
- What defines IoMT and how it is shaping the future of healthcare
- What cybersecurity risks to expect from internet-connected devices
- Why the IoMT requires a unique approach to security
- The five steps you can take to implement an effective cybersecurity strategy for the IoMT

These drastic improvements allow employees to work the way they prefer: In a sensitive, effective nature caring for patients. In this white paper, EXL thought leaders discuss how applying automated, digital solutions to streamline processes, simplify clinical workflows and eliminate manual administrative tasks, companies can improve patient and employee satisfaction at the same time. More so, you’ll learn how adding digital:
- Engages the members most likely to benefit from specific programs.
- Optimizes clinical resources’ scope of practice.
- Improves member engagement and health outcomes.
- Drives down health care costs across populations.

This white paper recaps an exclusive discussion between nine healthcare executives from systems like Northwell Health (New Hyde Park, N.Y.), Baptist Health South Florida (Coral Gables, Fla.) and Sentara Healthcare (Norfolk, Va.), who shared their thoughts on the promise of digital and automated care tools for closing care gaps and how-to's for successfully implementing them.
Read more to learn:
- How staff shortages are impacting care gaps
- Patient-centric tools that promote preventive care and help manage chronic conditions
- Common missteps in implementing digital interventions and how to avoid them

All along the continuum of care, hidden data silos prevent health systems from achieving the goals of interoperability, namely, the ability to put the right information in the right hands at the right time for better care. Without a clear idea of where data silos exist, achieving true data integration is impossible.
The stakes are high: Lack of data interoperability results in inefficient, disconnected care and undermines value-based care and population health.
Download this white paper to learn how to:
- Overcome top data sharing and access challenges in health systems
- Unlock trapped data in healthcare's 9 billion faxed documents sent each year
- Implement three strategies to eliminate data silos in healthcare

During a recent peer-to-peer discussion hosted by Becker's Hospital Review, healthcare information and technology leaders shared their own experiences and common challenges they've faced in adopting cloud strategies. Download the white paper to see their insights on best practices, goals, criteria and metrics for integrating cloud technology.
Learn how to:
- Make internal cultural shifts to overcome cloud adoption concerns
- Guide your decisions about implementation and integration strategies
- Understand the impact your cloud strategy has on care quality

During a session at Becker's 10th Annual CEO + CFO Roundtable, healthcare leaders from across the country discussed how their organizations are engaging in innovation and lessons they've learned. This report offers a summary of the discussion and features insights from:
Houston Methodist
UC San Diego (Calif.) Health
Fred Hutchinson Cancer Center (Seattle)

However, organizations are often held back in their digital transformation efforts by legacy IT systems and disconnected point solutions.
There's a better way. Healthcare organizations are discovering the transformational benefits of a single application platform that provides a unified, connected view of their data, patients and clinicians.
Download this white paper to learn how innovative healthcare organizations are leveraging this single platform to:
- Accelerate the speed to adapt to changing care requirements
- Improve clinician and patient management
- Dramatically heighten patient satisfaction
- Achieve seamless governance, risk and compliance management

practices.
Download the white paper to learn key takeaways with valuable, first-hand insights on how to
incorporate cloud into healthcare operations in the most effective way.
Key Points:
- Learn how to control security risks by limiting cloud provider and integrations
- Create criteria to evaluate cloud hosting providers for your organization’s specific needs
- Adopt a “why not cloud” approach to assessing cloud investments

Explore further possible uses for telehealth such as:
- Field emergency responses connecting unskilled responders to medical help
- Providing support to smaller hospitals in underserved communities
- “Tele-triage” to help relieve ER overcrowding and screen patients awaiting treatment

The growing complexity of care increases the communication and documentation burden on staff. This is why clinical workflow automation is gaining momentum — and why its adoption is expected to double from 2022 to 2024.
In collaboration with Becker's Healthcare, OmniLife Health conducted its inaugural clinical workflow automation benchmark survey, which elicited responses from 99 C-suite, clinical, transplant leaders and other decision-makers about where their organizations stand on implementing this critical technology.
Key learnings:
- How clinical workflow automation software can help improve efficiency and save staff time
- How the software can improve revenue capture by providing documentation needed for reimbursement.
- How healthcare organizations can use the software in a variety of clinical areas

While ambulatory care is an important strategic move to expand patient access, increase revenue and improve margins, there are critical challenges to navigate.
This eBook – based on an advisory call of health system leaders from across the country with significant ambulatory care expertise – covers keys to successful ambulatory care expansion, such as:
Why understanding the local market is critical
Prioritizing the patient experience when designing sites of care
Different management skills needed for ASCs vs. inpatient care
The need to focus on ambulatory reimbursement models
As the market rapidly shifts to more ambulatory care, it is essential to understand and act on the keys to ambulatory success.

In times of tight budgets and staffing challenges, technology such as artificial intelligence empower hospitals to run more sustainably.
AI patient monitoring helps hospitals minimize falls, cut costs and reduce the need for full time employees. Now it's time to bring digital nursing into the acute environment for truly flexible nursing teams.
Explore how AI and other digital care tools are making care more efficient in this white paper.
Key learnings:
- How digital care tools can reduce average sitter hours
- How AI patient monitoring can reduce patient falls
- How digital care tools can decrease fall alert response time

Get ready for next-level growth, productivity, and patient engagement with Health Cloud and Tableau CRM. The solution helped MIMIT get a holistic view of patient data with a single source of truth — and a 459% ROI in less than three months.
According to Nucleus Research, MIMIT Health:
Boosted productivity by 30%
Raised patient engagement
Reduced procedure scheduling from two weeks to two to five days
Cut inventory costs by 15%, or $150,000 a year

This white paper explores the steps health systems can take to upgrade manual patient engagement to digital processes for closing referral gaps.
Read more to learn about:
- The inefficiencies in the referral management process + impact on patients and practitioners
- Opportunities for automation in patient engagement for referrals, like SMS or phone-based notifications, and how health systems can get started implementing these
- The success Froedtert & the Medical College of Wisconsin realized in using its EHR-embedded patient engagement platform to create a closed-loop referral management workflow

This report outlines a clear strategy healthcare organizations can implement to improve patients' financial literacy and retain them amid an increasingly competitive marketplace.
You'll learn:
- Ways to lead with open and honest communication to provide compassionate financial care
- Strategies to create better connections with patients
- How to improve patients' knowledge about payments

So why is it so difficult to create a patient's "digital twin?"
In this insight brief, we explore some of the common obstacles to gathering, integrating and leveraging clinical data, such as:
- Siloed information within the EHR and between health IT systems
- Varied data accessibility
- Inadequate capture of detail or specificity
- Inconsistent data structure; and
- Variations in clinical terminology

This e-book highlights findings from Becker's-Teladoc Health's 6th annual telehealth benchmark survey, which elicited responses from healthcare CEOs, CFOs, virtual care leaders, directors, CIOs and other decision-makers about their organizations' stance on virtual care and plans for it going forward.
Key learnings include:
- What the survey findings reveal about the future of virtual care and health systems
- Some of the barriers holding back telehealth expansion and the resources healthcare organizations need to surmount those barriers
- How staffing models need to evolve to continue delivering the benefits of telehealth adoption amid persistent workforce shortages

However, with advances in artificial intelligence, machine learning and insights gleaned from other industries, hospitals and health systems are now better equipped than ever to more efficiently manage scarce resources.
This report outlines how health systems –including Chicago-based CommonSpirit Health and Winston-Salem, N.C.-based Novant Health — are using technology to tackle staffing shortages and optimize capacity and resources management, resulting in:
- Increased access to care for patients
- Higher revenues for provider organizations
- Improved clinician satisfaction

With the help of Tecsys’ Elite™ Healthcare POU technology, Sanford Health has automated and systemized data capture, closed the data loop on preference card picking cycles, eliminated redundant processes and driven down on-hand inventory value.
This success story documents their journey at each step of the way.
Key Takeaways:
- Understand how an ongoing commitment to continuous improvement can increase cost savings, drive operational efficiency and reduce waste.
- Measure inventory performance with accurate analytics and analyze real-time data using the right technology.
- Identify the financial impact of unused materials resulting from out-of-date surgeon preference cards.

In this new white paper, discover how leading plans are leveraging data and artificial intelligence to turbocharge the member experience, transform member interactions and drive engagement across all channels.
Download to learn how health plans can:
-
Use existing data and AI to turbocharge the contact center
-
Create a holistic view of members to transform their experience
-
Drive personalization with existing member data
-
Overcome barriers to technology adoption and build greater trust with members

Maintaining, growing and securing on-premises data storage presents major challenges for hospitals and health systems in such an environment. This white paper examines why cloud storage and computing will become essential supports for hospitals and health systems keen to make the most of medical imaging technology advancements.
In this eBook, you will learn:
- How health systems are reaping the benefits of cloud technology for medical imaging
- The four pillars for optimized medical imaging data use and storage

That’s a key takeaway from Becker’s survey of 102 hospital and health system leaders. This survey revealed lessons from the pandemic about increased resilience for future health crises. Among the key lessons is an increased focus on technology to improve clinical efficiency and staff effectiveness.
Gain insights from this survey on how coping with the last crisis (COVID-19) can help organizations be better prepared for the next one. Learn how health systems leaders are addressing points of failure and building on successful technology-driven strategies from the pandemic.
Key takeaways include:
- Why healthcare leaders feel better prepared for the next crisis
- How technology can augment staffing – before and during a crisis
- Why connecting point solutions to the IT infrastructure for specific use cases can have tremendous value
- The importance of smart technology investments

Becker's Hospital Review recently spoke with five healthcare leaders about the use of artificial intelligence, machine learning and predictive analytics to enhance capacity management. This report offers a summary of the discussion.
Download the report for insights from:
- Brian Dawson, MSN, system vice president of perioperative services at CommonSpirit Health (Chicago)
- Ira Martin, DNP, RN, former assistant chief nursing officer with HCA Healthcare (Nashville, Tenn.)
- Patrick McGill, MD, executive vice president and chief transformation officer of Community Health Network (Indianapolis)
- Cindy Russo, BSN, president of Trumbull Regional Medical Center (Warren, Ohio) and former COO of Steward Health Care's Ohio/Pennsylvania region
- Lori Wightman, vice president of nursing/chief nursing officer of SCL Health (Broomfield, Colo.)

A lack of access, ease, empathy, and partnership have real impacts on individual and
organizational wellbeing. Addressing these issues will require healthcare leaders to
listen, understand, and act. In other words, to adopt a holistic approach to empathy.
The reasons to operationalize empathy at scale are compelling. Not only is it the moral
approach, it makes business sense. Organizations across industries have seen
improved financial performance, increased patient and employee satisfaction, higher net
promoter scores…etc.. With so much at stake, empathy in healthcare is imperative.
In this guide you’ll learn:
- The cost of empathy deficiencies – and how to avoid them
- Three ways to foster human-centred experiences throughout your organization
- How to leverage real-time data, closed-loop processes, and AI to modernize your experience programs

But leading organizations are using data to fundamentally reimagine their offerings and operating models. Data is driving better clinical care, better patient experiences and better performance.
A new ebook from Becker’s Hospital Review shares insights on the "data journeys" and lessons learned from three leading healthcare organizations: Kaiser Permanente, City of Hope and Quorum Health. Each organization has overcome barriers and is now deriving enormous value from data.
Download the ebook to learn:
• How COVID-19 uncovered data challenges and accelerated the need for data-driven decisions
• The change in mindset to treat data as a product
• New data architectures, standards, metrics and technologies
• How organizations envision using AI and natural language processing
The future of healthcare relies on data. Discover how three healthcare leaders are turning their data into business value.

In just nine months, the health system deployed a nationwide virtual care platform with zero latency, resulting in significant cost reductions and improved quality of care.
Download this whitepaper to see how the system:
- Replaced costly 1:1 sitters with 1:12 virtual monitoring solutions
- Saved $23 million in labor costs
- Decreased patient fall rates systemwide

As hospitals and health systems navigate these events, their primary goal of improving patients' health remains unchanged. Organizations must keep downtime to an absolute minimum and ensure continuity of care.
Becker's Healthcare recently spoke with Hector Rodriguez, executive security advisor, WWPS health and life sciences at AWS, about how enterprise resilience and immutable IT infrastructures can reduce risks for patients and organizations.
Download this brief report to learn:
- How enterprise resilience protects patient safety and cuts costly organizational downtime
- What enterprise resilience plans should cover & key considerations for where to focus initial efforts
- The value of immutable IT infrastructures & how employee training fits into enterprise resilience

See how these leaders are improving their teams' workloads and quality of life while making patient care more efficient.
Download the brief to see the strategies and tactics healthcare leaders are using to address:
- Repetitive tasks within EHR workflows
-
Nursing shortage and the rising cost of contract staff
-
Recent resignation and retirement trends

This three-page case study explains how the hospital improved ED processes for patients and clinicians with a combination of new tools and strategy.
Download the report to learn about:
- The hospital's three-step approach to managing high-risk patients
- How to prevent medication errors and readmissions among ED patients
- How to achieve greater staff satisfaction with technology

Health plans are overwhelmed by fraudulent activity. Unfortunately, the pandemic opened the door for even more cybercriminals to find new schemes to submit improper, fraudulent claims.
Given the sheer volume, it’s impossible to pursue every instance of fraud. Health plans have launched special investigation units, with high-dollar cases as their top priority. While many lower-value cases fall by the wayside, these cases can have a broad impact on patients, quality of care and financial results.
A new white paper from Becker’s Hospital Review looks at the fraud landscape, drawbacks of current approaches to fight fraud and the role of AI in preventing fraud. This white paper details:
- The magnitude of fraud in healthcare
- Drawbacks of the rules-based approach used by many organizations
- Why leading healthcare organizations are turning to AI for data protection and fraud prevention
- Specific solutions that can reduce fraud, waste and abuse
Fraud in healthcare is only getting worse. Learn how your organization can use AI to more effectively manage this costly problem.

Learn how top healthcare organizations met these challenges with a new healthcare integration engine and experienced:
- 78 percent faster legacy interface conversion
- Deployment of 2,000 interfaces in less than two years
- Zero hours of unscheduled downtime
- Millions of dollars in savings

Becker’s Hospital Review recently collaborated with Zoom to survey 255 healthcare workers. Respondents were asked about their current level of burnout (teaser: it remains exceedingly high) as well as their use of telehealth technology and applications of video communication technology other than telehealth.
Download this two-page survey summary to discover:
- Current levels of burnout
- Top factors driving burnout (many are controllable)
- Use of and satisfaction with telehealth
- Applications of video communication other than telehealth
- Ways that communication technologies can improve employee satisfaction
This survey identifies actionable ways that video and other communications
technologies can help improve employee satisfaction, reduce burnout and boost productivity.

Key findings examined in the white paper include:
- New porous PEEK technology produced higher osseointegration capability when compared to solid PEEK, solid titanium and porous titanium in cell culture.
- New technology possessed higher fusion and quality of fusion grades at 12- and 26-weeks post-op when compared to solid PEEK.
- New technology Proved to obtain new bone formation throughout porous structure.

Healthcare delivery is experiencing a profound transformation. And as hospital and health system leaders work to balance in-person and remote care while navigating crisis-level staffing shortages and integrating new technology solutions, they must not overlook one facet of healthcare that has long been ripe for improvement — the patient experience.
These 10 articles comprise actionable insights for hospital and health system leaders committed to delivering a better patient experience.
Articles headlines include:
- 5 leaders on their system’s most valuable patient experience strategy this year
- NewYork-Presbyterian CXO Rick Evans: Patient experience is rebounding, but our work is not over
- A powerful way to start a medical appointment? With non-medical questions

Innovative new technology solutions are rapidly turning the vision for connected healthcare into reality.
A new white paper from Becker’s Hospital Review looks at the current state of connected healthcare and details:
- The goals, promise and benefits of connected healthcare
- Opportunities for connected ecosystems to improve patient and provider experiences
- Barriers that must be addressed to achieve truly connected healthcare
- Tips for communicating with and engaging patients in using connected digital tools Learn the benefits to your organization and patients from realizing the vision of connected healthcare and discover what it will take to get there.

Download this short report to see the clinical and patient experience improvements St. Luke's Health Network, MemorialCare Medical Group, OSF HealthCare and the University of Virginia Health System saw after adopting a digital behavioral health program.

New fall prevention technology powered artificial intelligence can help eliminate false alarms and gets nurses back to the bedside. The technology offloads additional tasks for nurses by reducing false alarms by 95 percent. It also provides effective patient safety and nursing support at a fraction of the cost of telesitters.
Key learnings:
How many nursing hours are wasted due to false alarms
How AI technology reduces tasks from nursing workloads, reducing burnout
How AI solutions deliver 1:1 patient fall monitoring

By unifying disparate RCM workflows through intelligent automation, providers can process claims faster with improved accuracy and response time. They can also serve a higher volume of patients without hiring more staff to support them.
Finally, intelligent automation can drive digital patient engagement, reduce workqueue volumes, and boost revenues.
In this whitepaper you will learn:
- Tactics for driving digital patient engagement and boost self-pay collections via intelligent automation
- How to solve revenue growth during an economic downturn by improving the digital front door
- Frameworks for a data-driven improvement cycle that provides structure for revenue growth

With 89 percent of U.S. adults owning a smartphone, telehealth services can help break down barriers as patients are able to get care from anywhere. Advancements in language services and other technologies allow telehealth services to become even more accessible.
Learn how improvements in virtual care and language services can make a difference in this whitepaper.
Key learnings:
- How advances in language services and technology are improving access to care for limited English proficient, deaf or hard of hearing patients
- Why ensuring health equity in telehealth programs is a necessary and vital element of a successful strategy
- Strategies to define telehealth roles and secure talent with the right competencies to fill them

To meet rising demand, health systems are rethinking the delivery of behavior care services. This means increasing use of virtual behavioral healthcare and other digital interventions.
Becker's Hospital Review recently convened a panel of behavioral health leaders from across the country to share best practices on the new normal for behavioral health and the role technology will play.
Organizations represented on the panel were:
- Centra Health (Lynchburg, Va.)
- Cedars-Sinai (Los Angeles)
- Hackensack Meridian Health (Edison, N.J.)
- Penn State Health (Hershey, Pa.)
- Prisma Health (Columbia, S.C.)
- Steward Health Care (headquartered in Dallas)
- How the pandemic drove these health systems to innovate behavioral healthcare delivery
- Why digital interventions may be the next wave of innovation
- Best practices and case studies from behavioral health leaders from across the country

But there are ways to mitigate these limits. With CipherHealth's unified platform, healthcare organizations can successfully engage patients throughout the care process to provide a reliable, digital and retail-like experience.
Download this whitepaper to learn how to:
- Use integration to improve workflows and patient outcomes while consolidating technology solutions
- How a patient engagement platform helps health systems maximize their EHR investment

Increasing demand for care at home programs, at all levels of acuity, is one of the many reasons more health systems are deploying remote care programs.
Care-at-home programs support improved outcomes across staffing, readmissions and patient satisfaction. Download this whitepaper to learn how health systems are utilizing remote care to deliver better care:
- New evidence demonstrating reduced cost of care and improved clinical outcomes
- Considerations for programs that manage acute, post-discharge, and chronic care patients
- Best practices to deliver remote care in the home

Old ways of working simply aren’t up to the challenges of today. They are too expensive, too inflexible and too hard to scale. The network is key to changing how healthcare operates. It enables providers to leverage the latest technologies — including artificial intelligence, machine learning and the internet of medical things — to generate unprecedented insight and make decision making smarter and faster.
In this whitepaper, we walk through the evolving challenges and opportunities for achieving enterprise intelligence across an increasingly decentralized care ecosystem.
What you’ll learn:
What barriers to innovation continue to challenge healthcare’s focus
How infrastructure transformation with network capabilities like private 5G, edge compute and network-as-a-Service will support the evolution of inpatient care
How rearchitecting connectivity, security and collaboration will build the innovation healthcare needs

Today, true care transformation can't be achieved without effective digital health solutions. According to Gartner, the digital health platforms approach guides organizations down "a path to faster value realization when responding to strategic imperatives and external uncertainties." The right digital health platform partnership will help healthcare organizations differentiate themselves and advance care delivery.
Learn more about digital health platforms and access insights from Gartner's "Market Guide for Digital Health Platform for Healthcare Providers."

Having real-time insights into every experience that matters allows healthcare organizations to understand the patient journey from end-to-end, connect feedback from multiple data channels, make data-driven business decisions that improve their bottom line and drive action at every level to deliver on patient and employee expectations.
Toledo, Ohio-based ProMedica is one of 11,000 healthcare organizations globally reaping the benefits of this strategy, known as experience management.
In this guide, readers will learn how to use experience management to:
- Improve patient experience and drive brand loyalty
- Increase revenue and profits while lowering costs
- Lower employee attrition while boosting productivity

Approximately 45 to 60 percent of a hospital’s revenue and expenses are related to perioperative services, and bundled payment models demand standardization and reliability to be successful. Yet at many hospitals, high variability in outcomes and costs produces a misalignment of goals among physicians, staff and administrators.
Besides delayed cases, slow operating room throughput, dissatisfied surgeons and significant deviations between same procedures performed by different surgeons inhibit organizations from offering competitive pricing or assuming the financial risk of managing community health.
At Wilmington, N.C.-based New Hanover Regional Medical Center, North American Partners in Anesthesia's team led by Rob Shakar, MD, chief of anesthesia, worked collaboratively with clinical colleagues to improve standardization in the total joint program by piloting a perioperative surgical home program in orthopedics.
The program generated outstanding clinical and operational outcomes and saved the hospital $4.2 million in the first year, prompting the hospital to scale perioperative surgical home across 16 service lines that produced an annual return on investment of up to $12 million.
Download this case study to learn:
- The benefits of monetizing the perioperative surgical home program
- How perioperative surgical home program can increase operating room utilization, first case on-time starts and patient and surgeon satisfaction
- How a perioperative surgical home program has decisive impacts on patients, surgeons, efficiency and profitability

A surgeon-authored report of patient-specific planning and placement of aprevo® interbody devices is available to spine surgeons, PAs, nurses and C-suite members.
Examples include single and multi-level fusions in patients diagnosed with stenosis, spondylolisthesis and adult deformity.
Planned versus achieved spinal alignment is shown for personalized surgical procedures utilizing aprevo® for:
- Transforaminal approach with a long fusion for scoliosis
- Anterior approach to address anterolisthesis with lateral listhesis
- Lateral approach for disc degeneration and foraminal stenosis

Becker's Hospital Review recently spoke with three experts on technology in the ambulatory setting about how their organizations leverage technology to create a better patient and provider experience. The organizations represented include Kansas City, Mo.-based University Health, University of Missouri (MU) Health Care in Columbia and Charleston Area Medical Center in South Charleston, W.Va.
Key learnings:
• Why outstanding ambulatory care requires consistency across technology systems
• How to balance clinician preference with technology standardization
• Why artificial intelligence and telehealth are poised to transform the EHR

That shifted in July 2017 when they began using Bamboo Health’s Pings solution to help monitor patient events in real time, improve care coordination efforts and succeed under MSSP.
Download this short report to learn:
- How HMCC reduced length of stay for its managed patients from 25 days to 21 days, resulting in $681,000 in savings
- How HMCC was able to earn $1,258,180 in shared savings under MSSP in just one year
- A real-world example on how Pings effectively coordinated care for a patient who fell while visiting a friend out of state

In this whitepaper you'll learn how to make informed prior authorization decisions quickly, reduce time spent dealing with phone calls and faxes, lower your overall expenditures and improve your members' care outcomes.
Key Learnings:
- Seven findings from American Medical Association studies where prior authorization caused time, money and health outcome detriments
- Two trends contributing to prior authorizations challenges
- Four faith-building statistics from an America's Health Insurance Plans study about the use of digital tools for prior authorization

Download this one-page summary to learn why nursing leaders consistently turn to CareRev's technology to post shifts, manage float pools and maintain flexible staffing.
Key learning points:
- An overview of what the CareRev app offers nursing leaders
- How it enables nursing leaders to ensure flexible staffing and organizational resilience
- Why healthcare professionals consistently book shifts through CareRev's technology solution

To attract and retain those patients, providers need to offer the modern, convenient features they’re accustomed to using elsewhere.
Phreesia recently surveyed more than 4,000 patients about their digital expectations for their care, including how they want to check in, manage appointments, make payments and engage with providers. We dive deep into the survey results and explore their implications for providers in our new white paper, How consumerism is reshaping the healthcare landscape—and how provider organizations should respond.
Read the white paper to learn:
- How patients feel about using self-service technology to manage their healthcare experience
- Digital strategies you can implement to increase access, activate patients and make payments easier
- Ways to identify third-party vendors that keep patients’ sensitive health information secure
- A 3-step checklist to successfully introduce new technologies to your patients

Read this white paper by SCP Health Chief Operating Officer Rob Reilly, to learn proven strategies for integrating artificial intelligence for better care and cost, including:
- Applying AI to health care operations
- Identifying AI specific tools that are critical to success
- Revealing a new hospital operations use case that employs AI

Download this two-page report to get a grasp of the why and how behind incorporating human-centered design into health tech solutions.
Key learning points:
- The difference between user-centered design and human-centered design
- Best practices for involving clinicians in the design process
- The benefits human-centered design has for patients and providers

While many leaders have turned to intelligent automation to expand staff capacity and reduce costs, it is increasingly becoming the basis of sustainable topline revenue growth. To drive growth, healthcare organizations need to go beyond acquiring referral channels to securing patient access across the patient journey via a variety of digital doors.
Using intelligent automation, healthcare organizations can deliver hassle-free primary and specialty care access points. They can also hardwire care progression by guiding patients to stay in-network along their care journeys.
In this whitepaper you will learn:
- Why the pursuit of cost-effective growth cannot be solved by continually increasing staffing levels
- How digitized intake can capture accurate patient information on the front-end to improve clinical outcomes and maximize revenue
- Why patient self-scheduling accelerates patient acquisition and retention

In this whitepaper, readers will:
- Learn the definition and value of conversational engagement
- Understand how healthcare providers can use conversational engagement to scale patient interactions
- Integrate conversational engagement with existing digital experiences to build patient loyalty

Learn how to improve patient acquisition, retention, and loyalty. In this guide, we’ll walk you through:
- The comprehensive strategies, technologies, and proven best practices to advance digital transformation
- Where top organizations are investing today to build a solid foundation for PX's future

This white paper outlines various ways hospitals and health systems can mitigate the harms of healthcare's workforce crisis by better supporting nurses. Learnings include.
How generate a renewed focus on caregiver well-being
How to improve both the physical and emotional working environment
How to create a culture of psychological support

Leaders from Mount Sinai Hospital in Chicago, Intermountain Healthcare in Salt Lake City and more recently participated in an advisory call hosted by Becker's Hospital Review to discuss the benefits of telehealth adoption and what healthcare organizations must do to ensure continued advances in the future. This report offers five takeaways from the discussion.
Key learnings:
- Why providers are embracing a digital-first mindset
- How telehealth can help mitigate staff shortages and boost patient access
- Telehealth's role in future care delivery models

The insights in this ebook can empower finance and supply chain managers to reduce spend and improve compliance every day.
Learnings include:
- Why disparate systems for managing supplies will only ever provide some of the data needed for informed decision-making.
- How visibility of the supply chain creates opportunities for reduced spend and better resource allocation.
- Why empowering the right people with the right tools is critically important to being proactive and being able to capitalize on significant opportunities.

This migration can relieve the financial burden of EHR investment, while also making it simpler for providers to adapt to new challenges.
Download this whitepaper to learn:
How much faster upgrade cycles are completed with cloud-based EHR
How quicker response times are when using cloud-based EHR
How to cure EHR update hiccups

How is change managed in your organization, and which processes could be more effective?
Download this checklist to discover ways to:
Improve visibility into projects, processes and resources
Better communicate change plans across teams
Gain buy-in from key stakeholders

Fortunately, advances in artificial intelligence and automation can enable you to break out of the status quo and accelerate growth.
By using six strategies implemented at leading health systems across the country, you can harness these capabilities to improve operating room access, increase strategic case volumes and capture more market share.
In this whitepaper, learn how to:
- Boost operating room and resource utilization
- Automate manual work to reduce staff workload
- Drive immediate bottom-line improvements
- Optimize referrals and prevent leakage
- Improve surgeon satisfaction

Still, too many hospitals' safety efforts are hindered by outdated tech infrastructures that make implementing solutions far more costly than they have to be, resulting in budget considerations canceling safety concerns. It is unacceptable for the physical well-being of nurses and others to become unaffordable.
This guide includes:
The importance of staff safety solutions, featuring a case study from a healthcare facility
An overview of the immediate benefits of staff safety how
5 steps to improve staff safety in your hospital

With synthetic data:
Conduct research 10x faster
Explore data independent of IRB process
Access broad datasets instantly and dynamically
Share research and insights worldwide
The eBook from MDClone will offer an in-depth guide to synthetic data for healthcare and how unlocking data access can drive innovation across the organization.

Specifically, in the face of rising demand and limited resources, healthcare organizations must unlock capacity by improving their utilization of critical, scarce resources like operating rooms, infusion chairs and inpatient beds. The keys to unlocking this capacity include the use of data, predictive and prescriptive analytics, and artificial intelligence to generate hard ROI during these challenging times.

Leaders from Ochsner Health, RWJBarnabas Health, Banner Health and more recently participated in an advisory call hosted by Becker's Hospital Review and RevSpring to discuss why digital must be a top priority in healthcare organizations' strategy to improve the patient experience.
Key learning points:
How providers are getting to know their patients' preferences
Ways to improve cost transparency
Enhancing self-service options for scheduling and payments

By implementing e-signature technology beyond the EHR, organizations can improve the patient intake and consent process saving patients and providers alike time and money–and reduce the burden upon staff.
This report highlights the challenges, opportunities and costs associated with improving the patient intake and consent process, including:
- 63% of providers say their consent process contains risks as a result of poor document storage and retrieval capabilities.
- 88% of healthcare respondents say e-signature is crucial for their organization — and that number is projected to climb to 93% within the next few years.

- Digital health strategy exists in name only – and that must change.
- Health systems need to swap vendor contracts for true partnerships to succeed on consumerism.
- To achieve virtual care integration, health systems must secure operational buy-in from the start.
- Scale is a catch-22. Proceed with caution.

Seven oncology leaders from across the U.S. recently participated in a roundtable sponsored by Elsevier and hosted by Becker's Hospital Review to discuss how COVID-19 reshaped the oncology field and how they are preparing for a pandemic-adjacent future. Download the two-page report to read the main insights from the discussion.
Key learning points:
The changes organizations are making to prioritize cancer care delivery
The unique role of health educators and support staff
What future oncology care models will incorporate
The outlook on the cost of oncology drugs

Healthcare is on the verge of the interconnected, intelligent future patients and clinicians deserve. This report examines the emerging technologies transforming healthcare and outlines the infrastructure necessary to support the coming connectivity revolution.
Key learnings include:
• The future of remote patient monitoring and device interconnectivity
• Why AI + 5G will transform healthcare technology development
• How an in-house innovation lab is transforming home care

In this whitepaper, we have identified seven best practices to optimize care access that support meaningful results without overly standardizing provider utilization.
Learning objectives:
Understand the most common patient access process obstacles and challenges
Learn how to measure each access point and determine how to increase profitability
Learn best practices to optimize patient access, scheduling and physician engagement

However, there are simple steps healthcare organizations can take to make preferred-language communication easier for patients and providers. When organizations use patients’ language of preference, staff can be more efficient and feel more supported while patients receive more personalized care and have better experiences.
Read this white paper to learn:
The impact of communicating with patients in their preferred language
How preferred-language communication improves patients’ access to care
How technology breaks down language barriers to improve care and meet patients where they are

Other asset-intensive industries like airlines or package delivery services face similar challenges. However, through sophisticated modeling and simulations, organizations in these industries can predict and match supply to demand with considerable accuracy. Every day, millions of packages are delivered on time and scores of travelers safely reach their destinations. The healthcare sector needs the same types of capacity-optimization tools.
These were the overarching themes that emerged during a hospital operations summit as part of Becker's Hospital Review's 12th Annual Meeting in Chicago. Dozens of hospital executives participated in the summit. This white paper is based on their conversations and includes specific learnings from:
- Rush University Medical Center in Chicago
- UCHealth in Aurora, Colo.
- Vanderbilt-Ingram Cancer Center in Nashville, Tenn.

This report provides insight on how to stay ahead of attacks, how to get better at restoring data after an attack and tips to secure cyber insurance coverage.
Key learning points:
The wider organizational impact of a ransomware attack on healthcare
Different methods used to recover encrypted data
The amount of ransom paid by health care organizations
Changes healthcare organizations are making to better position themselves for cyber insurance coverage
Leadership, staff and skillset

With 15 years of experience in asynchronous care behind us, we've found it to be the solution to the biggest challenges facing healthcare:
- Staffing shortages
- Provider burnout
- Delayed and avoided care
- Consumerism
- Health equity
- Expanding access
Health systems that are serious about solving these problems must venture outside traditional modes of care to prioritize patients and providers.
This guide also includes COVID-19: The Largest Case Study on Async.
Learning Objectives:
- How asynchronous telemedicine improves patient experience and loyalty by offering convenience and reduced costs, resulting in newly acquired patients and downstream revenue
- How asynchronous intelligent interviews improve clinical efficiency and directly solve for delayed and avoided care by increasing productivity by 56 percent
- How asynchronous virtual care improves access and health equity for rural, disadvantaged and non-English-speaking populations

To better understand how healthcare leaders are thinking about leveraging technology and CX platforms to solve their most critical challenges, Becker’s Hospital Review conducted roundtables and interviews with several healthcare leaders from both provider and payer organizations. Participants included the chief digital officer for Columbia, S.C.-based Prisma Health and Aetna's former chief innovation and digital officer. This report is based on those conversations.
Key learnings include:
4 digital experience trends identified across patients and members
An overview of the technology infrastructure necessary to support greater convenience in the patient experience
A 3-point assessment of a platform approach to healthcare consumer engagement

Recent advancements in technology and telehealth protocols have the potential to transform traditional maternity care. With proper integration, virtual care can start immediately addressing the leading factors in maternal deaths as identified by the CDC.
As we conducted research to bring together the ideas and concepts for this whitepaper, our team pulled information from recent healthcare news as well as interviewed a series of telehealth specialists, maternity care providers, and women who recently experienced high-risk pregnancies. As a telehealth solution provider, we are actively looking for ways to increase access to care, improve patient outcomes, manage healthcare costs and address gaps that have long created barriers in healthcare. Together we have created the potential for solutions that can almost immediately address the challenges facing present and future families in the U.S.
Augmenting Traditional Maternity Care with Virtual Care:
Close gaps in the care cycle from prenatal to postnatal and newborn care
Increase collaboration between healthcare providers to help identify and mitigate high-risk pregnancy conditions
Streamline provider collaboration while reducing cost of care for patients and providers

MU Health Care, an academic medical center in Columbia, Mo., recently completed an enterprisewide rollout of Amwell’s Converge platform to help achieve its vision of a centralized virtual care model. Through this rollout, the health system improved the patient, provider, and staff experience through features like build-in interpreter services, and the ability to launch a visit directly from the EHR.
In this case study, learn how MU Health Care:
Streamlined and centralized virtual care and deployed it across 35 primary and specialty care locations
Prioritized program features critical to patient, provider, and staff success
Simplified the patient experience by eliminating the need for app downloads and logins
Replicated in-person workflows using a virtual rooming workflow

Real-time location services (RTLS) are an important component of smart hospitals. RTLS technology powered by internet-of-things connectivity can accurately determine the location of people and assets throughout a hospital facility. The benefits of this technology extend from the obvious to the inconspicuous. While asset tracking may be the most common use case, RTLS can also address environmental monitoring, staff safety, hand hygiene compliance and wayfinding challenges as well.
By providing hyper-accurate tracking and monitoring solutions, RTLS technology can help mitigate these challenges.
This report covers:
Integrating RTLS into existing systems
The cost of maintaining legacy RTLS systems
How RTLS can improve the patient experience
Choosing the right platform

In the healthcare industry, the problem of employee burnout has been a major challenge for years. Addressing this challenge has only become more urgent amid the COVID-19 pandemic.
The boom of systems and technology has helped the healthcare industry improve efficiency but also has been a major contributor to provider stress and exhaustion. Siloed information systems and limited connectivity mean clinicians have become human data routers, searching for
relevant information to conduct their work and manually moving information from one system to another.
Download this white paper to learn about initiatives at Olive, the automation company:
Olive is creating the Internet of Healthcare to connect disjointed systems, reduce administrative burden and unleash $1 trillion in healthcare costs.
Olive is providing health systems with state-of-the-art automation technology, growing its partner network to further connected solutions and investing in the enhancement of interoperability and intelligence.
The platform provides leaders at health systems and hospitals with critical tools and capabilities to realize their success, including automations, services, APIs, intelligence through an extensive graph database, semantic interoperability and many more.
The platform provides healthcare technology partners with tools to accelerate build times while reducing the cost of customer acquisition and increasing speed to market.

Then everything changed in 2020, and the supply chain was tested even further. Now, the healthcare sector is reexamining how to build greater flexibility into supply chains while preserving efficiency and adjusting to additional shocks to the system.
Recently, Becker’s Hospital Review gathered health system leaders for panel discussions on the current state of the healthcare supply chain as part of a Supply Chain Forum, which was sponsored by Cardinal Health. Learn how Unity Point Health, Mayo Clinic and Cleveland Clinic turned to new technology and a solid new strategy to identify and solve supply chain issues. It all centers on reimagining the supply chain and optimizing competing priorities such as safety, quality, cost and access to products.

Healthcare innovation is advancing by leaps and bounds, even as much of that innovation happens faster at the conceptual and technology levels than at the actual implementation level.
During a May advisory call hosted by Becker’s Hospital Review and sponsored by T-Mobile for Business, Baron Kuehlewind, healthcare industry solutions advisor at T-Mobile, and a group of strategy, operations and telehealth leaders discussed how new care delivery models, technology and connectivity are colliding to reimagine the continuum of health services.
Download this whitepaper to learn how:
1. Care delivery outside of the hospital is forging ahead under different modalities.
2. Legacy systems are a major roadblock to advancing integration of remote and in-person care.
3. Connectivity is essential to extending care and supporting staff, with a caveat.
Please fill out the form to download the whitepaper.

Reducing length of stay and moving patients to alternative care settings such as ambulatory care clinics and home-based care is a top priority for many health systems. As care shifts to these settings, medication safety and robust inventory management are critical considerations, especially considering that drug shortages aren't expected to go away anytime soon.
During a May 2 panel at Becker's Virtual Annual Meeting, pharmacy leaders from Avera Health, UC San Diego Health and the University of Rochester Medical Center discussed key challenges surrounding medication inventory management and how they're working to address them. This whitepaper offers a summary of the discussion.
Download this whitepaper to learn:
Tools and techniques to improve inventory visibility and reporting
How inventory analytics can support organizational growth
Becker's Hospital Review conducted an online survey among practitioners to learn more about the current state of kit and tray management.
Here are five key takeaways:
1. Kit Check is overwhelmingly seen as the industry-leading vendor for kit and tray management.
2. Respondents see multiple opportunities for technologies to improve medication management.
3. A minority of health systems represented in the survey are currently using kit and tray management vendors.
4. The primary reasons that a hospital system would consider a new vendor are system standardization and problems with a current vendor.
5. When researching new vendors, traditional methods remain most important.

Technology solutions powered by artificial intelligence can help close the gap between what’s expected and what’s achievable.
But a recent industry survey found that a disconnect between the perceived value of digital revenue cycle management tools powered by AI and robotic process automation (RPA) is a barrier when adopting such emerging tech.
Still, about half of leading health systems report they plan to invest in such revenue cycle management tools within the next three years to improve financial performance.
The survey findings were recently released by Waystar and The Health Management Academy, which works with leading health systems and industry partners to identify barriers and opportunities in the sector, representing 150 of the largest health systems in the industry.
Here's what we know: Hospitals that use the technology, value it.
Currently, 6% to 28% of those surveyed report using AI and RPA for front-end, mid-cycle and back-end rev cycle management. Of these, 82% said they adopted the tools to improve financial performance.
Overall, health systems currently using AI and RPA report higher satisfaction with revenue cycle management processes than those that are not using or only considering the rollout of such tools.
This E-book comprises seven reports on the adoption and benefits of AI and RPA that are instrumental to any healthcare team.
Here's what you'll learn:
The No. 1 obstacle to hospital innovation
12 signs it's time to switch clearinghouses
Doing more with less in your revenue cycle
How to increase revenue with coverage detection

During a roundtable session sponsored by West Monroe at Becker’s Hospital Review’s 12th Annual Meeting in Chicago, Hugh Ma, partner at West Monroe, facilitated a discussion among healthcare executives about how digital health's advancement depends on organizations’ abilities to reinvent their operating models. This report is based on their conversation.

Learning Points:
- Learn about unique third-party remote access risks to the healthcare industry - Better understand industry compliance
- Protect access credentials and permissions
- Evaluate compliance using our HIPAA and HITECH checklist

IDC Research reveals the rollout of Health Cloud in Latin America and Canada saw:
3x faster setup for new care plan templates
10% gain in territorial reach
20% drop in enrollment time
Several new loyalty programs, up from just one

However, a wide range of technical, operational and regulatory challenges make it difficult for many healthcare organizations to properly implement home-care models. In this whitepaper by NTT DATA, you will learn:
Why hospital at home is a fast-rising model for value-based healthcare
The benefits and obstacles of a hospital at home system
The best way to implement a hospital at home solution within your organization

Accurate data matching has been a long-time problem in the healthcare industry. The promotion of interoperability exacerbates that problem by creating duplicate and mismatched records if organizations do not have the ability to see through sparse data.
This report is based on an executive roundtable from Executives for Health Innovation (EHI) and the healthcare business of LexisNexis® Risk Solutions, where experts discussed and shared insights on how their organizations plan on complying with evolving interoperability regulations, while addressing the impacts that it will have on their ability to balance customer experience and data security.

Patient self-scheduling can be a strategic lever for organizations to move from patient leakage to keepage at any point in the patient journey. However, the ROI for previous scheduling investments has been constrained by a myopic focus on the experience of one stakeholder group – be it patients, providers, or staff – and the exclusion of others.
It’s time for leaders to take a closer look at why their status quo scheduling processes have fallen short of expectations – and how they can unlock growth goals with self-scheduling.
Readers will learn:
How to empower providers to open their schedules with confidence, free staff from the administrative burden of managing scheduling requests, and proactively nudge patients to schedule recommended care
How to accurately assess the real benefits and potential pitfalls of self-scheduling solutions
Why a leading health system replaced their patient portal with self-scheduling, garnering a 96% patient satisfaction rating

This whitepaper offers tips from leading Epic organizations such as NYC Health + Hospitals and Optum to help you:
Build an Epic hiring plan
Benchmark Epic salaries
Recruit tough-to-fill Epic roles
Navigate remote work challenges

During Becker’s Hospital Review’s 12th Annual Meeting, in a session sponsored by IBM Watson Health, three company leaders — Steve Vance, provider senior business development executive, Danielle Sebastian, implementation manager, and Anna Moore, product manager — led a roundtable discussion about the impact of those limitations on the parties involved and steps organizations can take to course-correct. This whitepaper reviews the 4 key takeaways from that discussion.

Get this report and discover the top five use cases for digital healthcare staffing.
Applicant tracking systems (ATS)
Offer letters
Credentialing
Contracts
Onboarding
Please fill out the form to download the whitepaper.

As this shift occurs, many physicians are seeking new innovations to reduce costs, perform at a higher level and offer care to larger numbers of patients.
This whitepaper features insights from three leading otolaryngologists about the challenges
facing their practices and how they're adopting a new, single-use approach to microdebridement to create a positive clinician and patient experience.
Key takeaways:
- Challenges and opportunities of shifting ENT procedures to the office
- How single-use microdebriders can expand the scope of ENT care delivered in-office and reduce cost of care

Combining in-person, virtual and automated care to not only strengthen the patient experience but deliver better care with improved outcomes. Take a walk through a patient journey and see how care modalities are combined to create a seamless user experience within acute and outpatient settings, all the way to automated and virtual care in the home.
In this infographic you will walk through one patient’s behavioral health journey as they:
• Receive acute psychiatry care in the emergency department and in-patient unit
• Are entered into a virtual outpatient program
• Enter maintenance mode, including therapy at home, coaching, and self-directed care
• Trigger an escalation from automated to virtual care

However, data integration is more important than ever in healthcare, especially for marketers, who are looking to move away from relying on second- and third-party aggregated data to select target audiences. In the age of personalized, organic customer experiences, healthcare marketers are aiming to make their outreach strategies more individualized.
During a Becker’s webinar held in January and sponsored by Salesforce, data integration experts discussed the importance of having a HIPAA/GDPR-compliant customer data platform for driving more personalized engagement.
Download the whitepaper to learn how customer data platforms help meet evolving marketing and user engagement needs by:
- Delivering on expectations for personalization
- Ensuring privacy
- Providing trusted, compliant communication

As this already massive volume of data is expected to more than double in the next three years, many wonder how they will keep up.
Download this ebook, authored by IDC, for a powerful, visual look at trends, surveyed data, predictions and benefits.
Here's what you'll get:
- The hottest topics among healthcare providers today
- The benefits of connected content— and how to build your business case
- The 9 key next steps to get you there

These 10 articles examine current challenges and opportunities in the healthcare experience. Collectively, they amount to actionable guidance for digital health investment. Articles include:
- The top-rated hospitals for patient experience, state-by-state
- Game-changing EHR improvements at Intermountain, UCLA, and 6 other systems
- How one hospital CIO managed to grow his ranks during the pandemic

Specifically, health plans are currently spending valuable time and resources manually reviewing authorizations, which is a time-consuming process that can delay treatments — or worse, be an obstacle to care. Not only this, but with manual reviews estimated costs between $20 to $50 per prior authorization clinical review.
This white paper outlines how payers can automate the prior authorization process to lower administrative burden and operational costs while enabling the delivery of faster, more efficient care.

In this E-Book, you’ll learn five key trends affecting how providers give care and gain an understanding of how technology is turning passive purchasers into active healthcare consumers.
This E-Book explores the benefits of:
- Online support communities
- Self-monitoring apps and devices
- Performance scorecards
- Interactive online health education

The number of companies providing remote care software and services continues to grow, leaving hospitals with a myriad of options to consider as they navigate delivering acute care in the home. An AI-powered, FDA-cleared analytics engine capable of predicting clinical exacerbation is one platform component that many providers see as critical to effective remote patient management.
This insightful report outlines key success factors in developing a hospital at home program as well as how artificial intelligence and machine learning is accelerating the expansion of these programs.
Key learning points:
- An overview of CMS requirements for its Acute Hospital Care at Home Program
- How an end-to-end AI platform supports earlier interventions, thereby improving outcomes and lowering costs
- Steps and considerations to adopt and scale an acute care at home solution

We put together this whitepaper to guide you through that process. It addresses:
- Why you should consider telepsychiatry
- Considerations for your needs assessment
- The questions you should ask telepsychiatry vendors
- How you can streamline program implementation
Whether you’re revamping your existing program or building one from the ground up, these insights can help you successfully go through this process and alleviate pressure on your EDs.

In this whitepaper, two health systems share how they leveraged Cerner and Amwell's strategic collaboration to bring telehealth and the EHR together. At Fisher-Titus Medical Center in Norwalk, Ohio, embedding telehealth in the EHR helped the health system develop a virtual rooming process that strives to replicate the in-person care experience for its providers. University of Tennessee Medical Center recognized that an app-based program required separate patient logins. To circumvent this issue, in collaboration with Cerner and Amwell, UTMC implemented the embedded solution to streamline the patient experience — part of which included invites coming from text or email without additional app downloads or logins.
Read the whitepaper to learn:
- How health systems are integrating telehealth into the EHR to streamline patient and provider experiences
- How two health systems successfully brought telehealth and the EHR together
- How telehealth should set its sights on integration across the care continuum

There are some unique interoperability considerations for orthopedic practices, so practices must take care to ensure they are choosing the right solutions. Download this article to learn the four interoperability keys for orthopedics.
In this article you'll learn why orthopedic interoperability workflows must consider:
- Referrals and transitions of care
- Imaging integrations
- Unique device identifiers
- Plug and play integrations

Discover how Midwest Health System transformed their care management strategy with Deviceless Remote Patient Monitoring, centralized 24/7 care management teams, and streamlined workflows to reach more patients, faster, and with less resources. Over 35,000 patients participated and claims analyses showed a total medical cost reduction of over $30 million.
Read this case study to learn how to:
- Overcome common cost, logistics, and enrollment challenges when scaling RPM to tens of thousands of patients by going Deviceless
- Build an automated post-discharge workflow enabling outreach and enrollment to every patient, regardless of risk status, within 3 hours of discharge, with no lift from the care team
- Help population health care managers manage 10x the national average patient caseload by transforming care management from a manual outbound call model to an automated inbound

When bolting on additional technologies, it becomes nearly impossible to serve as a single point of data-based truth to the organization. With a properly implemented EHR, hospitals will see clearly defined performance and insights that facilitate better, faster decisions in the organization, compared to the lengthy process of compilation, validation and data debate.
Complete the form to get the whitepaper to learn how to:
- Build long-term strategic partnerships that enhance the success of the EHR implementation.
- Understand how to improve clinical outcomes, optimize operations, and enhance user and patient satisfaction through the EHR.
- Discover best practices that result in timely billing, fewer denials, enhanced patient accessibility and overall improved customer satisfaction.

But there’s a big difference between “cloud-based” and “cloud-native” platforms. For most healthcare organizations, a cloud-native solution provides superior benefits over tactics such as managed services or lift-and-shift to the cloud.
Download this visual white paper authored by Frost & Sullivan to discover cloud migration strategy success factors and learn:
- Short- and long-term benefits that cloud-native can deliver that other cloud-based technologies cannot
- Critical success factors for evaluating potential partners
- Security and efficient data migration considerations
- Business case considerations and ROI expectations

Every competitive organization is on a mission to eliminate grunt work for their people. Onboarding, offboarding, name updates, user management and more: Most healthcare IT service desks spin their wheels when dealing with these procedural, repetitive tasks. Fortunately, it doesn’t need to stay this way.
A recent market study from InformationWeek and TeamDynamix took a pulse on the challenges and priorities IT professionals face right now, finding:
Only 8% of organizations operate with a level of maturity where their IT service management technology is fully optimized
The heavy reliance on IT to administer IT service management systems tops all challenges
A lack of automation was the second most challenge burdening teams, which was named by 41% of organizations
36% of organizations said one of their biggest challenges was in integration and workflow management.
Download this market study to read the full market report, benchmark against your peers, and to gain insight into how you can eliminate grunt work and reduce resource drain.
Please fill out the form to download the whitepaper.

Until now, disparate, and disconnected data created operational blind spots making cost control and efficiency unattainable.
If you want to reduce waste and recover resources, gaining 360-degree visibility is a good place to start. Software can help:
- Identify the cost implications behind hidden data.
- Aggregate data from across the implant lifecycle, including explants, recalls and warranty claims processing.
- Automate processes and present key data in a meaningful way that help hospitals and health systems cut the substantial cost.
- Make visible the information for enterprise-level strategies that lead to impressive bottom-line results.

PINC AITM intelligence engine is a technology and services platform that leverages artificial intelligence, natural language processing (NLP) and machine learning to produce evidence-based insights at the point of care. Premier's value-based care focuses on improving healthcare quality through technology tools, while PINC AITM's margin-improvement solutions find and eliminate unnecessary spending, waste and inefficiencies.
With PINC AITM, organizations face a more stable future through the optimization of data, technology, services and scale. Premier understands healthcare and has the tools, data and innovation to power the significant changes health systems need. PINC AITM solutions enable multiple technologies to work together to optimize performance and accelerate healthcare innovation.
Uncover new value with PINC AITM. Download our e-book now.

With the uptick in the number of patients (55 percent in 2021, compared to 40 percent in 2020) reporting that telemedicine provides the same or better quality compared to in-person doctor visits, it’s clear that telemedicine, with its convenience and favorable cost/reimbursement, continues to deliver a much-needed solution to a host of healthcare challenges.
Download the full report and learn more about:
- The 79 percent of patients who prefer to receive a notification when their provider is ready to see them, rather than wait in a virtual waiting room.
- Mobile devices and why they are still the telehealth platform most preferred by patients.
- Telemedicine platforms that optimize for audio-only patient access allow for more equitable provision of virtual care services.

UiPath gathered insights from analysts, partners, customers and its own marketing, sales, product, partnership and customer success teams to determine 10 key automation trends. These trends present a picture of the years to come, the many possibilities automation presents and what hospitals need to take to take advantage.
Download this whitepaper to learn how:
- Task-based workflows are emerging as alternatives to business-application-based workflows
- Semantic automation revolutionizes robotic process automation
- CIOs are raising automation to the enterprise level

Download the whitepaper to learn more about these insights and the benefits of symptom checkers and triage tools for patients, providers and healthcare organizations.
The analyzed data and expert comments were compiled by Infermedica.
Whitepaper takeaways:
- How to navigate patients to the right point of care using symptom checkers and triage tools
- How patient data generated from symptom checkers can support medical consultations
- Strategies to connect symptom checker users to provider booking systems

This whitepaper will explain how the right safety and security management software can help healthcare organizations meet compliance standards and create a safer workplace.
Download this whitepaper to learn:
- Best practices for establishing and demonstrating your environment of care
- How complete, organized and easy-to-analyze data can help solve compliance challenges, track trends and create a safer environment
- Compliance-supporting features to look for in security management software

To discuss these trends, Becker’s Hospital Review and b.well® Connected Health — a healthcare technology company committed to transforming care — assembled a handful of hospital and health system executives for an advisory call. The conversation took place at the end of 2021 and also included participation from b.well® Connected Health’s founder and CEO Kristen Valdes. The following content is based on this conversation. Article Highlights:
- EHR and digital front door solutions are not a digital transformation strategy
- Cultivate a culture of urgency; New competitors are more consumer-savvy
- Digital transformation defined; It’s about winning and retaining more patients for your system

Learning points:
- Understand the critical role culture and leadership play in establishing and sustaining a high reliability environment
- Learn why it’s essential to integrate clinical, operational, and cultural data to get to the root of systemic problems that could cause harm
- Discover why embracing continuous learning helps teams identify, implement, and sustain improvements that produce meaningful results
- Appreciate the importance of a defined and evidence-based operating model for deploying and sustaining a high reliability strategy.
- See how to foster individual and organizational mindfulness to identify risks early, reduce the chances for error, build community, and improve performance

In December 2021, a diverse group of healthcare leaders from across the country met virtually at the Transform: Hospital Operations Virtual Summit to discuss how they are weathering the current storm by using technology to enhance capacity, streamline operations and provide outstanding care to patients.
This whitepaper offers key insights and best practices for these transformation efforts from leaders at Novant Health, Yale New Haven Health and Banner | Aetna. Learnings include:
- How streamlining operations can support better care and expand health equity
- How better data can build organizational resilience
- Why true transformation requires a technology-first approach

This report outlines five key actions healthcare leaders must take to end the call center in its current form.
Download the report to learn:
- The market forces that will continue to push healthcare towards touchless, self-service processes
- How automation and digitization can address the most common roadblocks to seeking care, from registration to scheduling
- Why intelligent automation must eliminate backend work in addition to optimizing frontend experiences

The size and complexity of healthcare facilities often make it easy to lose organizational control over workflows, but location data can solve that for any facility.
Real Time Location Services and the Internet of Things (IoT) are powerful technologies enabling healthcare organizations to achieve new levels of operational efficiency while also improving the patient experience and clinical outcomes.
Key learning points:
- How hospitals are benefiting from location data and IoT-enabled solutions
- Determining which technologies your organization should prioritize
- Real-world success stories of how U.S. healthcare systems are deploying these technologies

This year's executive brief address high-priority problems in healthcare technology, including cybersecurity, supply chain disruption, medical device safety hazards and telehealth. The brief also discusses building stronger, more resilient processes by leveraging innovations and lessons learned during COVID-19.
Download this whitepaper to learn:
- How persistent technology issues, including cybersecurity, can put patients at risk
- How critical issues with medical devices can lead to medication errors and increase patient risk
- How supply chain issues, artificial intelligence, personal protective equipment and telehealth may affect patients and staff
- Steps to take to manage these risks and encourage safe healthcare technology use throughout your organization

The pandemic sped up the timeline.
Now, the most proactive healthcare organizations are exploring initiatives to mitigate the effects of a growing labor shortage. Learn how central video monitoring enabled "virtual nurses" to support bedside nurses and uphold high standards of patient care amid a COVID-19 surge across Houston-based Memorial Hermann Health System.
Key learning points:
- The basic components of virtual care, including the easy-to-use technology involved to interact with patients and bedside staff
- The policies and workflows that best support virtual nursing staff and make for easy implementation
- How virtual nurses can use specialized care resources to alleviate existing staff

Many physicians have begun using virtual medical documentation specialists (MDS) in both hospitals and health systems as well as group practices. More than a scribe, an MDS is a tech-enabled assistant to the physician or nurse, leveraging automation technologies to capture real-time patient-provider conversations and convert them into precise medical documentation with appropriate context. Imagine how happy physicians could be if the documentation burden reduce time in the EHR and help manage:
- Care Gaps and HCC reminders
- Order tests, medications and labs
- Work down backlogs of charting

The emergence (and resurgence) of technology solutions — such as EHRs, telehealth and digital front doors to — helped deliver necessary support to an industry in crisis.
These 10 must-read Becker's articles offer a look into this unprecedented transformation. Readings include:
- Yale New Haven Health saved 470 hours of nurses' time in 1 year with EHR tool
- NewYork-Presbyterian CXO's: 7 principles to maintain relationships with patients in a world of transactions
- 10 hospital innovation execs on how their role has evolved during the pandemic

Now is a pivotal moment for improving critical access management, which is a vital step in
monitoring and securing third-party access. In this white paper, you’ll not only learn why the risk posed by third parties is particularly high, but also how to protect your organization’s data.
Download this white paper to learn:
- The current state of third-party security among healthcare organizations
- The unique challenges around access rights that the healthcare sector faces
- How critical access management can mitigate the risk of third-party threat

At the center of every hectic hospital emergency department are patients and their families, simply wanting to know what's going on. While caregivers do their best to provide new information as rapidly as possible, this can be a challenge.
Boston-based Brigham and Women's Hospital is working to improve communication and patient experience in the ED via the use of digital patient whiteboards. In a recent study conducted by the hospital, 96 percent of participants preferred a room with a digital whiteboard, saying that it improved communication throughout their stay and left them feeling more knowledgeable about what to do post-discharge.
Download this whitepaper to learn how the Brigham team used digital whiteboards in the ED to:
- Display personalized, real-time education and information to patients and loved ones throughout their stay
- Integrate with the EMR to automate clinical workflow and remove administrative tasks for clinicians
- Customize in-room communication to increase portal enrollment, streamline scheduling, and improve care coordination

In recent years, multiple incidents at healthcare organizations have shown that ransomware attacks can bring down systems, interfere with patient care, damage reputation and interrupt the revenue earning capability of an organization.
Forward-thinking leaders understand that taking cyber risk into account when making investments and setting strategies is the most successful path to using data and technology in their healthcare business.
Cyber Risk is Everywhere, Make Sure it’s Part of Your Healthcare Business Strategy provides valuable context and detailed insights to help your organization:
- Assess specific cyber threats to the healthcare industry
- Understand the underwriting landscape for different cyber risk
- Make cyber risk a key consideration in your business planning and strategy

Stagnant compliance budgets aren’t just a barrier to effective regulatory management, they can also pose regulatory risks. To ensure programs receive full leadership support and adequate resources, healthcare organizations must understand the value of their compliance programs in terms of return on investment.
Read this whitepaper to learn:
- Essential ROI-driving factors for a comprehensive compliance program
- How to better position your program to receive adequate support and resources
- The key roles that configurability and analytics play

Enterprise-wide provider scheduling can help optimize your workforce, improve healthcare operations, drive efficiency and ROI, and increase provider satisfaction. Understand essential use cases for enterprise resource scheduling software and learn the key questions you should ask when considering technology vendors.
Topics covered include:
- The value of an enterprise-wide scheduling solution
- Three questions to ask when auditing your scheduling workflows
- Key considerations when evaluating technology vendors

A growing number of hospitals are evaluating the advantages of IT outsourcing as they look to ease financial pressures and free up internal resources while maintaining quality patient care.
This white paper highlights the benefits of an IT partner that offers speed, agility and flexibility, much like David exhibited when battling Goliath.
In this white paper you’ll learn:
- The benefits of outsourcing your healthcare technology to a trusted partner.
- 5 Insights for Choosing a healthcare IT partner in 2022
- Behaviors that trustworthy partners exhibit.

Gain access to all the insights in the 2021 special report, and see why an overwhelming 98 percent of healthcare leaders say their organization either has or is planning to implement an AI strategy.
Get experts’ perspectives on how AI can deliver practical benefits, including:
- Achieving health equity goals
- Automating workflows
- Gaining tangible cost savings

The COVID-19 pandemic underscored the need for greater interoperability in healthcare. The nation’s pandemic response required health systems, labs, public health entities and payers to share information rapidly. These efforts were effective to a degree, but in many swaths of the country, the public health information technology infrastructure fell short.

While the societal and organizational risks are high, some of the mitigation techniques can be reassuringly simple. This paper provides a wealth of advice and support to help organizations adapt to these threats and improve their cybersecurity posture and resilience.

During a virtual roundtable at Becker's Sixth Annual Health IT + RCM conference, three revenue cycle experts attempted to answer that question. Download this 5-point report to get a breakdown of their insights.
Learnings include:
- How to scale up automation initiatives
- How to drive greater efficiency through technology
- How to translate AI investments into real value

This whitepaper describes how typical approaches to prior authorization fall short and why intelligent automation enables revenue cycle leaders to address this challenge at scale.
Download the whitepaper to learn:
- The five most common pitfalls to avoid in prior authorization automation
- What questions to ask of potential automation partners
- How revenue cycle staff can more successfully obtain prior authorizations the first time and prevent costly back-and-forth


Download this whitepaper to learn why interoperability and cybersecurity are critical health system investments. You’ll learn:
- How health systems can leverage interoperability and cybersecurity to help increase clinical confidence, optimize clinical and operational workflows, and extend care delivery
- Where cybersecurity risks lie
- How health systems are using interoperability to drive better patient care

Download this guide now for:
- Reasons why leading health systems implemented asynchronous telehealth as a key tool for improving care delivery
- Learnings from the origins of asynchronous telehealth
- Common misconceptions of asynchronous technology, debunked
- Ways to measure the value of implementing an asynchronous solution

Through this white paper, we examine the Fidelum Partners research that explores the awareness, perceived value, and use of medical device management services by healthcare executives.

In a 2021 Healthcare Industry Trends Survey of more than 1,300 healthcare organizations, 61 percent of respondents said they still use paper fax to transmit patient data. More surprising is that 56 percent of them believe fax will remain a valuable, or even dominant communication method over the next 5 years.
While paper fax won't disappear overnight, once converted into digital documents, technologies can be applied to provide meaningful, analytics-ready data, which can then be submitted into an EHR and consumed within an efficient workflow, supporting true interoperability.
Read the paper to learn how to:
- Improve healthcare data exchange
- Streamline providers' workflows
- Meet regulatory pressures

These 10 must-read articles examine healthcare in the digital era and include CIO predictions about the future of health IT in the next five years, digital health investment red flags, and a look at the use of technology at leading organizations like Cleveland Clinical and Danville, Pa.-based Geisinger.
Healthcare's digital era has arrived. Here's what you need to know.

In this whitepaper, you’ll learn how artificial intelligence-enabled predictive analytics and workflows can make your organization more strategic and proactive. By delivering up-to-date information and actionable recommendations, these technologies can improve OR block utilization while reducing staff overtime and costs.
Download this whitepaper to learn how predictive analytics can:
- Improve surgeon access to OR time
- Align OR staff to surgical demand
- Grow surgical volume

Download this free ebook to discover:
- Why healthcare organizations are choosing to move their content services to the cloud
- How to prioritize your cloud projects effectively
- Quantifiable and additional benefits of cloud deployment
- ROI assessment results for three healthcare organizations

Cybernetics forms a communication loop between humans and technology to elevate the work of healthcare professionals. Executives from systems around the country told Olive and Becker's Healthcare that tapping these technologies unlocks a path to a human-centric approach that uses cybernetics to enhance jobs, not eliminate them.
Learning points:
- Learn about the foundations of cybernetics and how it uses technology to form efficient workflows.
- Analyze avenues for technological investment and new means to enhance the ROI of human productivity.
- Hear firsthand accounts of how health systems are using cybernetics to improve efficiency, improve efficiency, provide real time intelligence to the workforce and reduce errors.
- Learn how this new technology can reduce the overall burden and burnout of workers without workflow disruption, freeing up their capacity to focus on more important things such as patient care.

By downloading this ebook, you’ll learn how automation can improve the healthcare revenue cycle. The ebook contains six must-reads that explain how automation can cut waste and which AI-driven tools are best for your organization.
In this ebook, you’ll learn:
- How automation can save your organization time and resources spent on repetitive tasks
- How connecting quality, finance and analytics can improve outcomes across your organization
- Which AI tools best improve the revenue cycle

Although healthcare has traditionally been slow to evolve, the past 18 months have shown that rapid change is possible. As health systems prepare for the future, many are evaluating new EHR systems.
To better understand the past, present and future of EHRs, Becker’s Hospital Review recently spoke with leaders from Mercy Iowa City and Allscripts.
In this whitepaper, you’ll learn:
- Which EHR goals to have
- How to negotiate a successful EHR contract
- How to choose an EHR that can accommodate new technologies and care delivery models

It’s time to open the door for care built for consumers.
Learning Points
- Increase patient acquisition and reduce patient leakage
- Using patient reacquisition to address delayed and avoided care
- Accelerate top-line revenue generation
- Route and triage patients efficiently

What does this mean for the future of care? Download this whitepaper to learn:
- How COVID-19 has shifted consumer expectations around access to care
- What key trends should be considered when assessing virtual tools for your organization
- What’s needed to develop a truly sustainable approach to hybrid care in 2021


The clerical burden associated with clinical documentation often falls too heavily on individual physicians tasked with accurately documenting conditions at the point of care. This documentation occurs in the EHR, requires time and attention, and can undermine the human element of care delivery as clinicians’ focus is pulled away from the patient in front them toward a digital screen.
This white paper exams the current medical coding landscape and offers insights into how technology can simplify coding complexity.

Download this white paper to learn how your life science organization can:
- Evaluate different patient services programs
- Understand how to get started in-house
- Scale your program with your business

Artificial intelligence can be a solution to healthcare's capacity conundrum, as it allows leaders to efficiently manage critical resources while using predictive and prescriptive analytics to forecast what's to come.
A recent virtual summit hosted by Becker's Hospital Review and LeanTaaS addressed how technology and perioperative "systemness" can improve hospital operations, now and in the future. Perspectives from leaders at some of the nation's leading health systems, including Chicago-based CommonSpirit Health and New York City-based Mount Sinai, were shared during the summit.
Access the top takeaways to know in this whitepaper.

Ready to learn how no-code tools can help your hospital or medical practice work smarter? In this guide, you will learn:
- How no-code workflows can transform your healthcare organization
- How to add the power of no-code to your health tech stack

Consequently, care facilities are now prioritizing tech-based solutions.
In particular, artificial intelligence can be applied to the video recordings taken in most hospital patient rooms to better categorize alarms related to movement in those rooms. AI-assisted Augmented Video Analysis (AVA) systems can provide additional information and data to hospital decision-makers, resulting in more accurate warnings and alerts, among other benefits.
In this white paper, you’ll learn how:
- AI and machine learning work hand-in-hand with video systems
- Advanced Video Analytics systems function in a hospital room
- Patient privacy can be protected using AVA systems
- Using AVA systems can benefit patient care and your bottom line

Our analysis examines the challenges and available solutions in leveraging data analytics and business intelligence for three main organizational domains: Clinical, Operational/IT, and Administrative/Executive.
- Meeting current and future expectations for care delivery in virtual environments
- Defining success for operational, administrative, and clinical domains
- Leveraging telehealth business intelligence to optimize efficiency and improve the patient experience

This case study covers how the health system:
- Embedded telehealth throughout the enterprise to cover the full spectrum of care across home and hospital settings
- Seamlessly integrated telehealth within its operations and care delivery
- Partnered with Amwell on a series of key integrations involving the patient portal, the EHR, and hospital room TVs

We researched these emerging digital disruptors and analyzed them for the breadth of their offerings and presence in the consumer and/or business marketplace.
As leaders, you want to make the right decisions to secure your place in the competitive landscape regionally and globally. Achieving that level of digital dexterity provides an opportunity to delight customers and achieve provider objectives. In so doing, you’ll achieve your organization’s goals for market leadership, differentiation, clinical revenue and margin.
Download our white paper today to understand where you and your competition fall in the following categories:
- Niche disruptors
- Digital enablers
- Game changers
- Transformation accelerators

The appointment workflow of old can't support the needs of today's patients and health systems. Download this guide to learn how to optimize patient appointments.

Key learnings:
- How the pandemic exposed frailties in legacy systems
- The consequential health IT changes required to address these challenges
- How enterprise imaging can drive improved agility and performance for imaging services

This white paper outlines the opportunity for acute and post-acute care providers to leverage interventional analytics to risk-stratify patients, standardize care and embed best practices across the
network.
Download this whitepaper to learn:
- How live data improves network performance
- How interventional analytics can prevent readmissions and improve length of stay
- The importance of risk stratification and standardization throughout the care continuum
- The qualities of a successful partnership between acute and post-acute players

This landscape leaves plenty of questions to be answered: How should healthcare organizations approach digital transformation? What should they consider when designing a next-generation consumer experience? How will they drive engagement? And how can they do it quickly?

Download this whitepaper for a closer look at why data normalization is needed, the downstream impact of data loss in healthcare, and how adding a robust terminology layer to the process can help solve data quality problems before they even arise.
In this whitepaper, you’ll learn:
- The critical link between data quality and data standardization
- Why standardizing clinical data can be such a challenge
- The foundational role of terminology in healthcare data


It's also elevating the efficiency and effectiveness of the workforce.
No, AI is not replacing humans. But it is easing administrative burdens and allowing staff to tackle higher-value work and collaborate with teams and patients.

What once was an option for convenience soon became a necessity, and the entire spectrum of healthcare has been affected. From adopting the technology platforms to strengthen virtual care best practices, to embracing clinicians’ “webside” manner, telehealth is calling for a new path forward and it is going to be increasingly important for all members of the healthcare industry to remain open and innovative in the face of these new challenges.
In this whitepaper, industry experts illuminate key components of adopting and deploying a telehealth strategy in the face of COVID-19, a strategy that will also reach patients where they are and deliver the care they expect as consumers. Regardless of how we combat the pandemic, telehealth has already proven to be a vital piece of many organizations’ care delivery models, and this whitepaper lays out how to develop the best strategy for achieving success in this new world of healthcare.

To support infection prevention efforts, the industry is now beginning to leverage tech to reduce the room for error. How? By adding in automated pathogen reduction technology as a supplement to existing cleaning protocols.

HIPAA was enacted to create national standards to protect sensitive patient health information, and many hospitals face fines for noncompliance. In this webinar, you’ll learn how a leading healthcare provider upgraded its security response and preparedness to comply with HIPAA and protect valuable patient data.
You’ll also learn:
- Why ransomware, phishing and data breaches are key attack vectors in healthcare
- Why compliance with HIPAA is federally mandated to protect patient records
- How Keysight provides solutions to comply with HIPAA and technologies to respond to cybersecurity threats

This whitepaper shares best practices for using automation and AI to increase telehealth self-pay collections and reimbursements and streamline manual virtual visit workflows, all while providing a delightful experience for patients.
Download the guide to learn:
- A proven 3-step strategic framework for using automation to improve virtual visit efficiency
- 6 workflows across the patient journey that can be automated to increase telehealth program efficiency and revenue capture
- Best practices for avoiding increased staff busywork and reduced provider efficiency from telehealth visits

This whitepaper shares strategies and best practices from automation technology adopters like Intermountain Healthcare on maximizing ROI across patient, clinical, and RCM workflow automation.
Download the guide to learn:
- An overview of robotic process automation (RPA) and artificial intelligence (AI) capabilities in healthcare, and how they can be used to power workflow automation
- How to prioritize which workflows to automate and how to measure the ROI on automation
- How to assess different automation partners and platforms based on your organization’s technical maturity and area of focus for automation
- How to build and scale an agile approach to launching and iterating on automated workflows
- Examples of how leading health systems have automated patient access, population health, and revenue cycle management workflows with Notable

This quick-read report lays it out. It covers:
- The evolution of threat detection and response
- How to separate fact from fictitious vendor assertions in such a crowded market
- The next generation of MDR with a three-pronged approach to prevent, detect, and respond to cyber-attacks

Over that time, they learned that integration between Interlace Health and Meditech is crucial to KDMC as the health system strives to eliminate human error, standardize processes, and accelerate consent completion.
While paper consents get lost or must be carried around in a paper chart until they are scanned into the EHR, Interlace Health’s eConsent forms are instantly archived into Meditech.
With Interlace Health, KDMC has decreased forms by 60 percent and now has more meaningful interactions with patients.

Emerging remote monitoring solutions are taking patient engagement to the next level while increasing provider access to essential clinical information.
These 9 must-reads examine the regulatory environment, emerging monitoring solutions and what hospital innovation chiefs want from health IT.

Read this paper to learn how you too can use ADT notifications to:
- Enhance digital interoperability to improve care coordination, and health outcomes
- Streamline staff workflows and solve other transitions of care challenges
- Roll out ADT notifications without over burdening your in-house IT resources



Read this whitepaper to learn about the challenges uncovered in the recent HIMSS survey and how to address them including:
• What stands in the way of HIT interoperability success
• How to bridge interoperability gaps surfaced by the pandemic
• Solutions for healthcare content and images that improve interoperability

This whitepaper summarizes key findings from several of those studies, such as:
- Institutions using the LEAF System reported reductions of sacrococcygeal HAPIs by up to 85%
- Adherence with institutional turn protocols – critical to prevent HAPIs – rose by up to 95% at institutions using the LEAF System.
- Hospitals using the LEAF System avoided up to $1.4 million in HAPI costs and reported HAPI treatment ROI of up to $3.4 million.

Download the whitepaper to learn:
- The limitations of data and risk scores for actioning SDOH.
- How AI can save millions by helping target beneficial investments for socially vulnerable communities.
- How AI inferences and recommendations can lead to more productive conversations with patients about potential barriers to health.

This whitepaper will explore:
- How mobile apps can improve patient care and provider revenue
- Cost pressures facing providers currently and post-COVID-19
- How patient non-compliance harms revenue
- The prevalence of smartphones and use of technology during the pandemic

In this white paper, you’ll learn how to integrate technology and equipment with the physical environment by:
- Determining the specific needs of your facility and team to gain buy-in
- Reconfiguring your existing space to make technology use easy, safe and efficient
- Implementing ergonomic solutions into the care environment with ongoing evaluation


Key points include:
- How IT is evolving and why organizations need to adapt to a new world of healthcare delivery
- The top five drivers of change in healthcare
- The keys to success for changing times in healthcare


In this whitepaper, we explore:
- Reducing wait times with virtual providers in triage.
- Ensuring continuity of care with virtual follow-up for discharged patients.
- Improving clinician satisfaction and reducing hospital admissions with virtual patient navigation.

Fortunately, there is an innovative platform that integrates the complete implant lifecycle and provides enterprise analytics. The platform’s increased supply chain visibility can help hospitals and health systems enhance patient safety, regulatory compliance and operational efficiency while improving the economics of healthcare.

Download this whitepaper to learn:
- 6 essential strategies for designing and implementing a digital front door that patients love
- Common pitfalls that delay development and reduce adoption of patient engagement solutions
- How Notable uses robotic process automation and AI to power digital intake experiences with over 80% pre-visit completion and 97% patient satisfaction
- How to reduce call volume by automating pre-visit patient registration
- How modernizing patient intake can help optimize revenue cycle management

The good news is that organizations that champion behavioral health integration — or BHI — can accomplish both goals.
In this new report from NeuroFlow, you’ll learn how tech-enabled BHI — or tBHI — can help your organization:
- Achieve cost savings and increase revenue
- Reduce patient leakage and strengthen patient engagement
- Vaccine appointment reminder check-list

Download Part 1 of the Route to Compliance eBook Series for:
- An overview of the CMS E-notifications CoP and all requirements included
- Survey results revealing hospital CIO familiarity with the CMS rule
- An assessment framework for hospitals and CIOs to find compliance solutions
- E-notification solutions available to guarantee full CoP compliance for hospitals

In this report, hospital leaders weigh in on how they're forging a path to profitability under value-based care. It covers how leaders are taking control of the move to full-risk, aligning strategies, payer relationships and more.
Key learning points:
- Overview of current trends driving the shift to value-based care
- The range of VBC approaches health systems are taking
- Key thoughts on alignment with physicians and payers

Healthcare Executives from hospitals and health systems across the country discussed the future of revenue cycle functions and how their organizations are aiming to level the playing field with payers during a roundtable at Becker's 14th Annual Meeting.
Major themes examined during the conversation include:
- Where RCM operations are heading
- AI's role in revenue cycle functions
- How healthcare executives are preparing now for future challenges

This report examined the perspectives of more than 1,200 healthcare employees, patients and guardians on the state of patient access in 2024, including:
- How well patient access functions are managed in U.S. healthcare
- What functions are best meeting patient and staff members' expectations
- Providers' primary cause of denied claims
- The biggest pain point for patients

Through an analysis of the digital payment platforms' role and the hidden costs of their independent use, the paper highlights the complementary nature of patient financing solutions on both financial outcomes for health systems and patient experiences.
Key takeaways in this whitepaper:
- Discover how the integration of digital payment platforms with comprehensive patient financing solutions can address the shortcomings of standalone systems.
- Learn about the benefits of combining digital ease with flexible financing solutions, including the reduction of bad debt, increased patient loyalty and improved financial health for health systems.
- Understand the importance of leveraging data-driven insights from patient financing solutions to make informed decisions that mitigate financial risks while enhancing patient care.
- Gain insights into how the combination of digital platforms and patient financing solutions can lead to more efficient collections at the lowest cost.

Health systems are grappling with increasing levels of uncompensated care as healthcare costs rise and insurance coverage remains inadequate for a significant portion of the population.
This whitepaper outlines key opportunities for organizations to maximize revenue recovery efforts while improving cash flow and operations.
Learn to adapt to rising costs with insights on:
- Understanding the current healthcare environment regarding rising costs, COVID-19 impacts and Medicaid redetermination
- Focusing on more than cost-cutting
- Auditing your current solutions and processes

Choosing the wrong tool could add work for your team and cost you more, or it could become “shelfware”—never being properly implemented at all.
Use this guide to help you make more informed and careful decisions when picking a solution so you don't fall for the hype.
Inside this whitepaper, you'll find:
- 3 foundational ideas that may transform the way you think about AI and modern tech
- A helpful set of questions to run through every time you're looking to introduce a new solution
- A key consideration when assessing if a tech tool will ultimately provide value

All automation is not created equal.
Some solutions are flawed. Some simply require extra expertise. But there is good news: The fixes exist. This eBook will give you tips on how to avoid four common mistakes technologies make while also exploring:
- Estimation rates and accuracy
- Common flaws in prior authorization
- Tips for proactive revenue monitoring
- A 6-step checklist for denials automation

Many health systems are turning to automation to tackle healthcare's thorniest issues, and denials are no exception. With the right solution, organizations can achieve a 72% reduction in their denial rate. This free eBook outlines four steps organizations can take to dramatically reduce denials, boost revenue, and lighten workload for overburdened employees.
You'll learn strategies to:
- Prevent front-end denials using data
- Optimize claim submission with speed and accuracy
- Respond to denials with data-driven intelligence
- Deliver a plan for long-term improvement

In this playbook, you'll gain insights into payer strategies and how providers can develop their own data-driven approaches to improve financial health — ensuring healthcare access and patient well-being remain at the forefront.
Key takeaways:
- Understand the current state of Medicare Advantage plans in payer strategies and implications on healthcare economics.
- Learn key steps that help to ensure fair provider reimbursements.
- Get tips to better manage payer relations and start a journey toward sustainable financial health.

In this white paper, you'll see actionable steps and expert insights on the support needed to effectively navigate these challenges.
You will learn:
- Strategies to mitigate the financial burden of intricate claim types
- The impact of various complex claim categories + practical methods for handling them
- Outsourcing support as an effective strategy

In this expert guide, leaders in clinical documentation integrity, operations and coding share best practices and actionable tips for maximizing revenue in these trying times. Download to learn more about:
- The impact of a unified revenue cycle on enhancing patient experiences and improving outcomes
- Roles of personnel, data, and technology in the revenue optimization process
- Innovative applications of data and analytics for revenue growth strategies

Providers have a unique opportunity to enhance financial performance through billing efficiency — but only if they're willing to take action. Download this white paper to learn about a versatile digital billing platform that eliminates administrative burdens and simplifies the payment process for patients, leading to consistent revenue and a better overall care experience.
Key learnings include:
- Why a patient-centric mobile billing platform is central to making improvements in financial outcomes
- Key features that empower patients and improve engagement
- Opportunities to showcase provider's unique brand identity

In fact, one vice president of revenue cycle operations from a large academic health system recently told Becker's, "Payer behavior is the biggest threat we have to our industry."
This whitepaper outlines an exclusive discussion with health system revenue cycle leaders, who shared how they’re navigating these challenges. They offered strategies for revenue cycle improvements, including automation technology, and their ideas for bettering payer-provider relations, including:
- Exploring service-level agreements and outside industry support
- Building stronger relationships with managed care teams
- Technology and capacity upgrades in RCM

However, a milestone has been reached in modern computing that can finally eliminate this workflow bottleneck: the coupling of existing optical character recognition (OCR) capabilities with modern artificial intelligence technologies such as machine learning and natural language processing. This whitepaper outlines how these technologies, working together, allow an organization to automate its fax triage process, cutting costs and improving efficiency.
You'll learn:
- Three reasons fax remains dominant in healthcare
- How AI can process faxes faster, more accurately and at a significantly lower cost
- Before/after results of installing AI-based fax processing

A strategic partner with end-to-end, automated RCM solutions can help. These solutions can improve operational efficiency, patient experience and financial outcomes with features such as patient engagement tools, financial clearance tools, clean claim submissions and accurate coding.
This whitepaper explores how to select the right RCM partner to better address your revenue cycle pain points and increase your bottom line.
You'll learn how to:
- Improve patient experiences through scheduling and payment options
- Optimize claims processing, reduce denials and increase patient collections
- Integrate clinical workflows to drive appropriate care and streamline outpatient charging

Download this e-book to learn the five-step strategy for optimizing front-end accuracy to prevent denials, reduce administrative costs and increase yield.
You'll get solutions and strategies to:
- Incorporate intelligent automation to improve data accuracy and optimize staff resources
- Automate and streamline prior authorization processes to reduce administrative burden and care delays
- Improve the patient financial experience by generating accurate cost estimates and convenient payments

In this white paper, we'll explore today's RCM workforce landscape and explain how, through the combined use of AI and robotic process automation technology, RCM organizations can not only overcome the current workforce shortages, but also improve the overall productivity and efficiency of their organization.
The combination of these technologies might still be in its early stages, but the potential benefits of the AI/RPA union for RCM organizations are nearly unlimited.
You'll learn:
- How AI and RPA can work together to automate both complex and mundane tasks
- Common problems in RCM and how AI/RPA can help solve them
- Specific tasks and applications for AI/RPA technology

To better understand how hospital and health system leaders are navigating razor-thin margins, Becker's Hospital Review conducted an advisory call with CEOs, CFOs and vice presidents of finance and operations from health systems across the country.
The advisory call participants shared their perspectives on factors contributing to margin pressures, what actions hospitals and health systems are taking to address these challenges and an outlook for the future.
Key learning points:
- Why margins are under such tremendous pressure
- How organizations are responding right now
- Why partnerships should be a key strategic consideration

Within the revenue cycle, clinical and administrative workflows like registration, scheduling, coding and billing traditionally require manual, labor-intensive tasks. But automation presents a valuable opportunity to help reduce workloads and administrative burdens with a digital workforce, allowing providers and staff to focus on improving the overall patient experience.
This whitepaper dives into the benefits of robotic process automation — in which "bots" that mimic human behavior complete repetitive tasks — and outlines how organizations can identify the best places to implement the technology.
You'll learn:
- How automation technology can help address provider organizations' key challenges
- Where automation can be applied specifically throughout the revenue cycle
- The differences between RPA and artificial intelligence

Stay informed with this highlights brief, put together by government reimbursement experts. It summarizes 11 key changes leaders need to know about the new regulations, including:
- A look at the annual increase and market basket percentage
- Updates on new and expired MS-DRGs
- A review of the dramatic reduction in uncompensated care payments

In this white paper, you'll learn how front-end enhancements within your RCM to include pre-care tasks can keep your organization proactive and profitable, while creating a positive patient experience.
Read more to learn about:
- Automating front-end RCM functions to increase efficiency and accuracy
- Delivering accurate patient estimates to support regulatory requirements and improve the patient experience
- Strategies for consolidating disparate, siloed systems to improve consistency across the patient journey
- Three simple steps to start making RCM change happen

Doulas are nonclinical professionals who can provide emotional, physical and informational support during pregnancy, delivery and after childbirth. Research shows working with a doula can reduce cesarean section rates, decrease complications and increase satisfaction with birth experiences. But because doula support is rarely covered by insurance, accessing care can be challenging.
This white paper outlines opportunities for health plans to expand access to doula care and improve outcomes, especially for at-risk populations.
Key learnings:
- How prenatal and birth doula care can improve birth outcomes
- The role postpartum doulas can play in improving postpartum mental health
- Strategies for seamlessly integrating doula support with health plan coverage

You'll learn:
- What your hospital's 2024 CMS Star Rating range is likely to be
- Challenges hospitals face in managing CMS Star Rating and other programs
- How Dexur helps hospitals achieve quality excellence

In the 2023 Revenue IntelligenceTM Data and Insights report, experts from R1 and Cloudmed examine the converging trends reshaping today's healthcare revenue cycle. The report is based on public and private data on hospital RCM performance and patient experience trends.
In this report, you'll learn:
- Expert tips and actionable insights across 13 steps of the revenue cycle
- How to manage complex claims, challenging payer behavior trends and adjudication lags
- The role digital tools and patient experience can have on your bottom line

What’s the best way to stay ahead of denials in healthcare? With the proper insights and action, health organizations can prevent more upfront denials, empower staff with the right tools, and reduce revenue leakage.
In this report, we’ll dive into:
- Research on the current state of denials
- Steps to prevent, prioritize, and outsmart denials
- Real world examples on how healthcare organizations benefit from purpose-built automation
- Strategies to examine where denials most frequently originate and how to stay ahead of them

This brief whitepaper delves into effective strategies for healthcare organizations to overcome the challenges posed by Medicaid enrollments.
Healthcare leaders will learn:
- How to overcome barriers with state agencies
- The importance of Medicaid recipient re-enrollment and retention of coverage
- Opportunities for automation within the revenue cycle process and how to implement it for eligibility and benefits verification
- How patient-centric strategies alleviate payment-related stress and enhance a system’s payment collection success

The question becomes: When teams aren't onsite, how do leaders keep tabs on staff members' day-to-day activities and ensure they're working efficiently and producing results that drive revenue recovery?
In this Finvi white paper, you'll learn about technologies — including voice and data monitoring, dashboards, performance alerts and rankings — that support real-time visibility into your account reps' daily activities and improve overall productivity.
Please fill out the form to download the whitepaper.

In a Becker's advisory call, healthcare leaders from top systems across the country shared their latest strategies and where they're finding success in solving today's most pressing problems. This e-book summarizes their insights on revenue challenges, staffing woes, payer relationships and more.
You'll learn:
- How leaders are mitigating staffing shortages
- Ways to boost financial performance through tech, length-of-stay reductions and less reliance on travel nurses
- One system's unique approach to denials management

So how can organizations do a better job at validating ROI and assessing demand? Becker's Hospital Review hosted a virtual advisory call with healthcare finance leaders to discuss just that.
Download a summary of the session to learn:
- The main challenges systems face when evaluating ROI expectations
- Best practices and frameworks to predict costs and volume growth
- What health systems need to generate buy-in

In this case study, you’ll learn that the technology Montgomery County Memorial Hospital + Clinics uses streamlined accounting and financial processes and led to a 50 percent reduction in month-end close time.
You'll also see:
- Key features of the hospital's enhanced system that are driving efficiency and time gains
- How they gained internal buy-in and saw enthusiastic adoption by team members
- Support that led to successful implementation during the height of the COVID-19 pandemic

After implementing ProviderTrust’s vendor monitoring solution, Meharry was able to onboard, manage, and monitor its entire vendor network with confidence and ease in one central location.
Download this white paper to learn how:
- Partnering with ProviderTrust allowed Meharry to achieve automated compliance monitoring for its vendors
- 90% of Meharry’s vendors are now verified as compliant before an invoice is paid
- Hours of tedious and manual work were eliminated with ProviderTrust’s solution

If this resonates for your organization, use this guide to find out if it's time to finally invest in the efficacy and efficiency that comes from end-to-end RCM.
You'll learn:
- How end-to-end solves five common, complex RCM challenges
- What to look for in a true end-to-end partnership
- How to raise yield by 2 to 5 percent

This e-book features a collection of Becker's top articles and insights on revenue cycle management this year — a comprehensive guide to equip you and your team with the latest, common challenges among healthcare finance executives; best practices from leading hospitals and health systems; and how organizations are adopting technology like automation for improved operations and revenue.
Download the e-book for more on:
- RCM leaders' take on artificial intelligence
- Spending trends for revenue cycle optimization
- How 42 health systems are boosting their revenues

This white paper summarizes 95 survey responses and six interviews with healthcare financial leaders regarding their top revenue cycle challenges and the steps they are taking to address them.
Read this paper to learn:
- What tops the list of RCM headaches
- Where today's RCM solutions fall short
- Why physician productivity remains challenging to measure
- Where AI usage in RCM stands today and expectations for its use tomorrow

This white paper summarizes 95 survey responses and six interviews with healthcare financial leaders regarding their top revenue cycle challenges and the steps they are taking to address them.
Read this paper to learn:
- What tops the list of RCM headaches
- Where today's RCM solutions fall short
- Why physician productivity remains challenging to measure
- Where AI usage in RCM stands today and expectations for its use tomorrow

Read this brief guide to unlock the full potential of ERC and its benefits.
Key takeaways:
- Overview of the ERC, eligibility and compliance requirements
- Real-client outcomes on total credits earned
- Best practices for safe filing and compliance

This white paper outlines concrete strategies for hospitals to excel at quality and safety and avoid surprises when it comes to the results of these CMS programs.
You'll learn:
4 reasons hospitals struggle with quality excellence
7 ways hospitals can avoid surprises and improve on CMS Star Ratings, HRRP penalties and VBP payouts
How to access predictions on CMS Star Ratings and readmissions and mortality

To address these challenges, Novant Health launched a new patient engagement and payment platform that integrates into Epic across hospital and physician billing.
Download the case study to learn:
- The impact of launching a new platform at a health system that already made significant investments in MyChart
- Key opportunities to enable a consumer-centric experience for patients
- How they created a low-friction, easy-to-navigate bill payment experience for both patients and team members

To discuss current challenges and advances in the revenue cycle, Becker's Hospital Review and healthcare technology company AKASA hosted revenue cycle and technology experts at the RCM Innovation Summit held in conjunction with Becker's 13th Annual Meeting. Organizations represented at the summit included:
- Vermont Medical Center (Burlington)
- Mass General Brigham (Boston)
- Waikiki Health Center (Honolulu)
Key learnings:
- Where to start and how to strategically expand automation
- How to Elevate Your Revenue Cycle Staff
- How to get the most out of your automation investment

A patient's first and last interactions are often financial. And market research shows that their satisfaction and your financial sustainability are impacted by these interactions. This whitepaper outlines the latest market research and insights from 35 leading health systems on the current state of the patient financial experience.
What's in the report?
- Research on how automation is connected to financial sustainability and patient loyalty
- Perspectives from 35 leading health systems on what's working (and what's not)
- Strategies to remedy gaps in patient satisfaction

To combat these challenges, member experience transformation has increasingly become a competitive opportunity to drive greater engagement, boost member satisfaction, and meet business and financial objectives.
In this report from Becker's Healthcare, executives from Highmark Health, Cambia, McKinsey and more share insights on how leaders can effectively showcase the value of their CX transformation initiatives and proven strategies to enhance the member experience to deliver on key business objectives.
Key takeaways:
- A best-in-class member experience is now the strategic advantage
- The 4 key value drivers of CX transformation and strategies to execute them
- Proven strategies for measuring the value of CX

In the past, Crawford Memorial's month-end close process took two full weeks. The new ERP cut that time in half.
Multiple departments and about 60 employees at the hospital utilize the ERP for tasks including user setup, workflow facilitation and payroll interface. The financial team, along with other departments, now have easier access to valuable reporting throughout the month, which has streamlined processes and allowed for better tracking and analysis of key metrics.
Download this whitepaper to learn more about Crawford Memorial Hospital's ERP journey.
Key learnings:
- How Crawford Memorial Hospital cut its month-end close process by 50 percent
- How the ERP simplified the hospital's process of tracking key metrics
- How Crawford Memorial Hospital plans to use the ERP to accomplish future goals

It's too much for one department to handle on its own. To tackle these disparate issues, some top hospitals and systems have turned to collaboration between revenue cycle, IT and other departments with great success.
In this white paper, leaders from Houston Methodist, Children's Hospital Los Angeles and more share how their departments banded together to improve the patient financial experience, maximize resources amid staffing shortages, and tighten cybersecurity.
You'll learn:
- Strategies to drive patient-centric collaboration across your organization
- How to meet patient expectations while keeping data safe in the digital age
- Specific types of automation that can alleviate staffing shortages and burnout

CMS audits are revealing incorrect qualified payment amount calculations, providers are continuing to send balance bills to patients, and the independent dispute resolution process is struggling to keep up with the caseload.
This whitepaper helps payers develop a better NSA compliance strategy by outlining:
- Three key strategies for payers to address NSA compliance challenges
- A self-assessment to understand the strength of your NSA strategy

Dartmouth Health, a nonprofit academic health system in Lebanon, N.H., aimed to improve cash collections, patient satisfaction and funding for uninsured patients. Through an eight-year partnership, it achieved 101.6 percent of its cash collection goal and a 97 percent patient satisfaction rate.
This case study showcases how the health system was able to turn its goals into a reality.
Key learnings:
- How a one call customer service model resolved patient billing issues
- How Dartmouth Health saved $15 million in cost-to-collect
- How the health system improved single business office performance

Clearwater, Fla.-based BayCare Health System is staying ahead of these changes by choosing to innovate, acting as a beta customer for RevElate, a new solution from Oracle Health that advances capabilities of its existing EHR and patient accounting platforms.
In this white paper, learn more about how BayCare's RevElate pilot and find out how your health system can:
- Simplify and streamline the revenue cycle with a single master file
- Preserve the integrity and efficiency of the revenue cycle
- Cut down on errors that require time-consuming manual fixes
- Ensure a smooth transition between revenue cycle platforms
In this Finvi-sponsored white paper, you'll read perspectives and successes realized from Dallas-based Methodist Health System and Parallon of HCA Healthcare in using tech-enabled workflows to address RCM staff shortages, improve inventory management and enhance payer engagement.
Read more to learn:
- Primary challenges that healthcare collections teams are facing today, such as increased call hold times and growing adoption of high-deductible health plans
- The importance of measuring team progress + performance to see improvement
- How automation drives quality, compliance and productivity for RCM teams

Overcome the pressure of shrinking margins by increasing workforce efficiency with lessons in this e-book from Proliance Surgeons and Prosthetic & Orthotics Group.
In this e-book, you'll learn:
- Tips to improve workforce efficiency in healthcare
- How one specialty provider slashed staff time spent per denial by up to 30 days
- Strategies that helped an ASC double their processed payments and foster financial growth

Optimizing revenue opportunities and maximizing reimbursements are imperative for financial stability, and contract performance is critical to those efforts. This e-book details concrete steps hospitals and health systems can take to maximize revenue through better insurance contract management, and how having the right data can help them get there.
You'll gain key insights including:
- Three ways to leverage data to maximize revenue
- A step-by-step guide to negotiating profitable contracts
- The types of data you need to make negotiations more productive
- How to evaluate and improve claims compliance
- Tips for managing denials and prior authorizations

Learn best practices from healthcare RCM leaders on how to successfully improve workflows, organizational efficiency, patient experience and more using automation.
In this advisory call, you'll learn:
- How to choose the right kind of automation for your organizational goals
- How to pick the right workflow for automation
- How to expand your perspective of ROI for automation

Craft a plan to exceed patients' financial expectations with this four-step guide.
Learnings include:
- Three of the top financial challenges patients and providers face
- A full exploration of the patient financial care maturity model
- Checklists, metrics, and next steps for each of the four-step process

Gain insights on the state of patient access and learn what you can do to improve it.
Three things you'll learn in this report:
- Access pain points for patients and providers
- Why providers have a more negative view of patient access than patients
- Why providers are optimistic that patient access is about to get better

So how are leading health plans responding to these headwinds? That is exactly what Becker’s asked senior leaders from top health plans in a recent Advisory Call.
This Advisory Call recap summarizes specific actions leading health plans are taking, which include:
- Adapting their strategy and operations
- Revisiting pricing strategies and ways to share cost increases
- Leveraging value-based reimbursement
- Tackling administrative inefficiencies and reducing waste
- Identifying technology solutions to automate mundane tasks
- Steering care to lower cost settings
- And much, much more
Today’s economic headwinds aren’t going away anytime soon. Get ideas for your plan by hearing what top health plans said in this Advisory Call.

These four use cases demonstrate how health plans can positively influence the full picture of member health, leading to better outcomes.
Learn about health plans' role in:
- Post-discharge coaching
- Behavioral health coaching
- Oncology coaching and the future of cancer
- Cardiometabolic coaching with food delivery services

- Learn how you can massively cut your data footprint and compute costs.
- See where you can save time and benefit from AI and automation tools.
- Understand the ways cloud can help you stay on top of regulations.

This new ebook features short, must-read articles on 10 key topics facing C-suite leaders today, with ideas on how to thrive amid today’s challenges. Learn about:
- How one CEO keeps staff turnover under 1 percent
- Growth opportunities despite recessionary trends
- Succeeding despite the lack of access to capital
- Overcoming net operating losses
- How partnerships help health systems thrive

In this white paper, you'll learn how Red Oak, Iowa-based Montgomery County Memorial Hospital leveraged technology to streamline its financial processes, enhance productivity and reduce month-end time to close by 50 percent.
You'll also get more details on how the hospital:
- Streamlined accounting functions within one login application
- Employed its EMR to help with analysis and reporting
- Navigated implementation challenges (during the onset of COVID-19, no less)
- Increased staff satisfaction and buy-in

That’s because RCM today is fraught with challenges. It is labor intensive, exists in silos, burdens employees, lacks data and results in revenue leakage.
A new whitepaper lays out a recipe for better RCM. Key elements of better RCM include making it holistic and more automated, using prescriptive analytics and payer performance management. Results include better communication, improved employee satisfaction, decreased revenue leakage and more data to use when engaging in negotiations with payers.
In this whitepaper, you will learn:
- Why a holistic RCM approach is far better than silos.
- How RCM automation improves efficiency and employee satisfaction.
- How process improvements can maximize revenue and improve team performance.
- The importance of predictive analytics and payer performance management.

Optum commissioned a survey of senior health plan executives on payment processing trends as well as opportunities and barriers to improve payments.
This report lays out the most pressing issues affecting payment processing and details top priorities for streamlining claims payment, including shifting to a paperless system and adopting automation.
Get this report to learn:
- Current state of health plans’ payment strategies
- Top pain points and most important priorities
- Key opportunities to streamline payments and barriers to making it happen
- What to look for when considering a payment solution

Rather than fall further behind, revenue cycle leaders are rethinking workflows and reimagining how work gets done alongside the latest advancements in technology. There are entire organizations that are writing a new playbook, establishing new paradigms for truly doing more with less, and defining a completely new way to tackle these long-standing revenue cycle challenges.
In this whitepaper, you will learn:
- Why now is the time for revenue cycle leaders to move beyond digitizing specific workflows and instead shift their efforts to intelligent automation
- New approaches to evolving patient access, with a focus on eliminating denials
- Best practices and KPIs for analyzing your denial management efforts
- How health systems are deploying advanced technologies to drive end-to-end connectivity throughout the entire revenue cycle and reducing the overall cost to collect

How can health plans simultaneously improve clinical outcomes, boost member satisfaction and lower costs?
The answer: by optimizing interventions for patients with chronic diseases that lead members to the right care at the right time. Effective chronic care interventions improve outcomes, close gaps in care and achieve meaningful cost savings and ROI. In fact, there are interventions with guaranteed year-one cost savings.
Learn about these interventions in the new whitepaper – The ROI of Virtual Health: How Better Outcomes Drive Cost Savings for Health Plans.
This whitepaper explores:
- What drives ROI for health plans
- How to achieve guaranteed costs savings and ROI from interventions in year 1
- How optimized interventions improve outcomes and member retention
- How to provide flexible options for your population and specific cohorts

Among the survey's key insights:
Labor shortages are decimating revenue cycle teams
84 percent of organizations are behind on cash collections
Denials are up, in some case 20 percent higher than previously
But there are solutions to accelerate the revenue cycle and improve cash collections. See the survey results and insights from PwC revenue cycle experts that highlight the importance of:
- Leveraging data to decrease denials
- Using automation and technology to improve efficiency
- Upskilling revenue cycle teams and forming strategic partnership

Trends in healthcare payments will shift as the industry weathers financial instability, scarce resources, and staff burnout.
But even amid changing competitive and regulatory landscapes, many healthcare providers are thriving. They’re finding ways to do more with less, improve patient outcomes, and drive innovation.
Download this report to unlock current trends in healthcare payments for 2023, as well as proven strategies to help revenue cycle teams succeed.
What's Inside:
- Dive deep into top trends in healthcare payments for 2023
- Find new opportunities to foster financial growth
- Discover revenue cycle strategies to achieve your mission

You'll learn:
- How changes in the VA influence Veteran benefits today
- Pitfalls that make it challenging to work with the VA
- Effective ways to capture reimbursement for services rendered to Veterans

To date, kidney care has focused on diagnosis and treatment. But 1 in 4 patients "crash" into dialysis, where dialysis must be initiated urgently with no opportunity for patients and providers to discuss treatment alternatives or make optimal decisions.
What’s needed is "crash prevention" by using predictive intelligence to identify patients likely to need future dialysis, leading to earlier intervention.
Download this white paper on The Kidney Care Paradigm Shift. It focuses on:
- Predicting & preventing advanced CKD
- Identifying at-risk patients earlier through predictive intelligence
- Benefits of avoiding emergent dialysis
Treating CKD is costly and inefficient, but doesn’t have to be. Discover a new paradigm that leverages predictive intelligence for earlier intervention.

To succeed, revenue cycle leaders need to transform the first interaction many patients have in their care experience into a competitive differentiator, manage ever-changing payer rules, and navigate an exacerbated workforce shortage. Leading health systems are automating front-end processes to eliminate back-end administrative burden – removing patient and staff hassles that compromise quality, impact reliability, and escalate cost.
In this whitepaper, you will learn:
- Why common approaches to revenue cycle improvement fall short
- The role of intelligent automation in strengthening the front end of revenue cycles with higher accuracy and faster payment, without additional headcount
- How a leading health system decreased authorization-related write-offs by 55% and saved nearly 3,000 staff hours

Enterprise resource planning software can increase efficiency by providing quick access to a wide range of information, which can also allow the organization to reduce its operational costs.
Explore how enterprise resource planning software can help decrease the need for manual tasks and save on overhead costs while still delivering quality care.
Key takeaways:
- Defining healthcare finance KPIs
- The importance of tracking healthcare finance KPIs
- The challenges of legacy software in healthcare

KeyBank and Cain Brothers are helping healthcare organizations remain flexible and agile. Hear from three industry leaders to learn how your organization can be prepared for upcoming challenges.
- Agapito “Aga” Morgan, commercial healthcare leader, Key Corporate and Commercial Bank
- Dave Morlock, managing director, head of health systems practice, Cain Brothers, a division of KeyBanc Capital Markets
- Kellen Williams, senior manager of business development, Laurel Road, a brand of KeyBank
In this whitepaper you will learn how:
- The healthcare landscape is expected to shift in the coming years
- Value-based care will reshape the industry
- Organizations can be forward-thinking in multiple dimensions

Patient financial obligation reached $491 billion in 2021, and the self-pay portion for patients with insurance now accounts for nearly 60 percent of bad debt. The standard model for patient payments is no longer sufficient.
In this ebook you'll learn:
- How health systems can achieve substantial returns with an integrated technology and services approach
- The components of a bold new patient payment model
- How to create a seamless patient experience that drives higher revenue performance

What can providers do?
Take proactive steps to find hidden insurance coverage among patients who present as self-pay. Results include increased collections from patients and payers, decreased bad debt and improved financials.
A new white paper contains insights on maximizing self-pay revenue through better coverage detection.
Key learnings in the whitepaper focus on:
- Why you’re missing billable insurance coverage
- The impact of missing or hidden coverage – which includes writing off bad debt
- 4 ways to find insurance for self-pay patients
- Selecting the right coverage detection technology to meet your organization’s needs
- How coverage detection works

Based on increasing revenue cycle work and a shortage of skilled workers, it is impossible to hire enough people or ask current employees to work harder.
It’s time to work smarter, not harder. What does working smarter in the revenue cycle mean? It means finding innovative ways to do more with less.
Download for best practices on:
- Developing a smarter revenue cycle and administrative strategy
- Cutting down on outdated manual processes
- Streamlining existing processes with intelligent automation

This whitepaper covers how to best support CFOs today, and how organizations can implement these five steps to improve financial health:

90 percent of respondents to a recent Becker’s/Multiview survey said data analysis is important to achieving their organization’s financial goals, yet only 25 percent have access to robust real-time information to drive better financial performance.
As a result, finance teams are often caught up doing time-consuming “Excel gymnastics.” Many finance teams are more focused on preparing financial statements or getting through audits than making data-driven decisions.
Gain insights from this recent survey among financial leaders which include:
- Why “liquid” data and real-time data are so important
- The unique challenges faced by finance teams at small hospitals
- Effective solutions that enable finance teams to make real-time, data-driven decisions
- Why vendor partnerships are key to data-driven decisions and increased operational efficiencies
Learn what it takes to go from manual, Excel-based processes to real-time, data-driven decisions.

Based on these challenges, a virtual care solution that only caters to the tech-savvy hoping to shed a few pounds isn't going to cut it. This report shares how a SDOH-attuned, virtual solution can offer your members access to:
- Personalized eating plans that fall within their budget and food accessibility
- Accessible, human-led care — even with limited access to technology
- Cognitive behavioral therapy-based coaching to address underlying causes
- Health literacy skills to sustain future success

This e-book comprises three case studies featuring large health systems — Cincinnati-based Mercy Health, Atlanta-based Piedmont Healthcare and Aurora, Colorado-based UCHealth. These organizations reduced costs and increased collections by delivering better patient financial care. Read this eBook to learn how your organization can:
- Increase agency collections by 10 to 15 percent
- Decrease denials related to authorizations by 46 percent
- Boost point-of-service payments by 30 percent

Sample findings:
- Denials are increasing. 30 percent of respondents say denials are increasing between 10 percent to 15 percent.
- LEARN: Discover the top 3 reasons this is happening.
- LEARN: Discover the top 3 reasons this is happening.
- Automation is considered critical. 52 percent of respondents upgraded or replaced previous claims process technology in the last 12 months.
- LEARN: Where are organizations turning for automation technology?
- LEARN: Where are organizations turning for automation technology?
- Everyone is looking for improved performance. 78 percent of respondents say their organizations are at least somewhat likely to replace their existing claims management solution if convinced something else can deliver better ROI.
- LEARN: How do providers define ROI in the claims process?
These themes are further broken down based on survey answers to aide revenue cycle leaders with near- and long-term strategy and planning.

Read this report to learn how to retain patients in a competitive marketplace and keep your organization running smoothly.
You'll learn:
- Ways to lead with open + honest communication to provide compassionate financial care
- Strategies to create better connections with your patients
- How to improve patients’ knowledge about payments

This e-book examines the future of healthcare finance and is informed by the real-world experience of hospital leaders and financial experts.
Key learnings include:
The tenets of agile financial planning
The keys to great financial partnerships
How a lean five-member finance team at a nonprofit provider transformed fiscal operations

How to deliver patients a more transparent, convenient financial experience was the focus of a leadership summit as part of Becker's Hospital Review 12th Annual Meeting in Chicago. Summit participants included technology leaders and top executives from hospitals and health systems around the nation.
Key learnings include:
- How to digitize and personal the patient experience
- How solutions powered by artificial intelligence can enhance front-end patient engagement
- How to build lasting relationships with patients

Building and sustaining trust yields myriad benefits for providers and patients:
Increasing patient retention
Improving appointment adherence
Generating positive referrals
Strengthening healthcare outcomes
Yielding positive patient survey results
Our guide describes how providers can achieve these considerable benefits. Connected communication built on insight—and seamlessly linked throughout the entire patient experience—drives impact. Technology is key, but so is understanding each patient. Equally important: harnessing proven strategies for using digital communication in ways that resonate with individual consumers.
Take a moment to download and read our guide on getting patient communication right. It clearly details the relationship between communication and trust, and how providers can use modern tools and strategies to achieve positive, consistent and connected engagement that builds patient trust and loyalty.

Leaders are now exploring the need for scalable, innovative alternatives to succeed. But they also must contain costs. With data from more than 150 health plan, provider, employer, life science and government leaders, plus insights from industry experts, this research report checks in on:
- Health care's greatest challenges
- Priorities for a sustainable health care system
- What progress has been achieved
- Near-term investment priorities

All of these changes expose healthcare providers to potential front-end errors that can ultimately result in higher denial risk or non-payment from patients. Furthermore, as employees change jobs at a record pace and float in and out of exchanges, it's easy to see why accurate eligibility verification remains elusive for many providers.
In addition to patients changing plans, payers are continually updating member rosters and benefit databases. Payers have shifted much of the member experience and relevant benefit information to online payer portals, which leaves providers to rely on disjointed sources of information and outdated EDI solutions. What’s more, each payer approaches this differently despite established standards-based bodies like CAQH.
Today, it’s not just about whether a patient has coverage. Eligibility is based on specific benefit levels (i.e., copays, coinsurance), in- and out-of-network determination, authorization and deductible/out of pocket information for a specific care episode. It’s not surprising that front-end staff sometimes get it wrong.
What's inside:
Why eligibility is no longer a commodity and what providers must have to ensure eligibility is accurate
A real example of payer analysis
How providers are using purpose-built automation to do less manual work and still get more (and better) benefit rules coverage, and therefore estimation accuracy
Examples of provider use-cases with results

Healthcare technology leaders must take action to modernize fraud protection. If they don't, the industry will continue to fall prey to many more of these schemes.
This two-part guide offers insights into emerging best practices in fraud protection. Key learnings include:
- An overview of the healthcare fraud landscape
- A snapshot of a real-world fraud case
- An examination of the role technology plays in both fraud protection and fraud susceptibility


This report is based on emerging data and examines the state of innovation in healthcare. The report also identifies specific innovation enablers and details the three pillars necessary for crafting a successful digital transformation strategy.
Additional learnings include:
- Five technologies driving innovation in healthcare finance
- Four benefits of system integration

This white paper from R1 RCM will offer best practices to help health systems jump-start their financial recovery efforts. You will learn how implementing standardized processes, automation-driven technology and transparency allows hospitals to thrive financially.

To drive better payment results , healthcare organizations must shift to thinking of patients as travelers. Instead of viewing a fully paid balance as the fastest way to a destination, data analytics enable organizations to identify patients that may need to take a slower route, or payment plans, to pay their bills. Effective use of analytics can also pinpoint patients who would benefit most from financial assistance.
Download this short guide to learn more about the benefits actionable intelligence provides. Key learning points:
- How tailoring billing statements can lead to receiving payments an average of 15 days sooner
- How linking analytics with appropriate OmniChannel strategies for each patient increases self-service payments by an average of 6.5 percent
- How the precise use of dynamic patient portals can generate $250,000 to $2.33 million more in additional revenue

market and greater demand for enhanced technology-enabled experiences.
This e-book will help get you started prioritizing the path toward a sounder financial footing. Seize the opportunity to truly meet the needs of everyone in your community by mastering the five fundamentals for financial performance in a new era of health care.
In this e-book, you'll learn how successful healthcare organizations handle their:
- Cost management
- Revenue integrity
- Workforce optimization
- Digital infrastructure
- Growth strategy

During a February advisory call hosted by Becker's Dental + DSO Review, a group of DSO leaders — including several CEOs — discussed current pain points related to patient financing and potential solutions. This article contains five key takeaways from the conversation.
Learnings include:
- Why patient financing presents a challenge for most DSOs
- Why juggling multiple agreements with finance companies creates administrative burden for staff.
- Why staff training is essential to supporting a better patient financial experience.

The year's report explains how the turmoil of the pandemic is continuing to affect trends in healthcare payments, as well as displaying data that paints a clear picture of what healthcare needs to move forward.
Download the report to learn more about:
- How efforts to improve price transparency fall short
- The role that social determinants of health play in the payment experience
- The changes needed to advance digital channels in healthcare

Proper reimbursement depends on appropriate documentation and reporting.
AMN Healthcare Revenue Cycle Solutions delivers significant benefits. When AMN Healthcare partners with trauma centers, it leverages optimal reimbursement necessary for financial stability. A positive financial impact from a successful billing program can transform a trauma service from a cost center into a revenue generator.

This Allscripts whitepaper explores topics including:
- How logic-based solutions drive better operational outcomes
- Accelerating revenue cycle optimization
- Perioperative supply conservation post COVID-19
- Artificial intelligence and bot technology in revenue cycle processes

Frequently mentioned is the idea that technology can help health systems operate more effectively and efficiently in this climate. One technology receiving a great deal of attention is robotic process automation (RPA).
To learn more about the adoption and use of RPA in the revenue cycle, Becker's Healthcare conducted a survey in November and December 2021 among U.S. health system leaders. This survey looked at adoption of RPA in the revenue cycle, how RPA is being used, expected benefits, expected ROI and considerations when selecting vendors and software solutions.
With about half of survey respondents having adopted RPA within their revenue cycle, RPA has progressed beyond the early adopters to the mainstream.
While finding the organizational resources and bandwidth to implement RPA will be challenging, the benefits and ROI likely provide a compelling business case.

During a Becker’s Hospital Review advisory call in December, VisitPay, an R1 company, hosted a session to explore the changing patient financial engagement landscape and what consumers perceive as a successful billing experience. This ebook details six key takeaways from that call.
Read the ebook to learn:
- Key ways the patient financial engagement landscape is changing
- How to better address patients’ billing needs and preferences
- Why personalized billing helps health systems achieve better outcomes

From this report, you will gain insight into the following key trends (and more):
- The latest financial data reveals the ongoing challenges. What you can expect with a long-tailed recovery.
- How providers and patients are responding to mounting financial pressures.
- Global supply chain breakdowns are impeding recovery for hospitals and health systems. What this means for your organization and what’s next.
Access our study to learn more about what financial executives, like yourself, are challenged with and how they are responding.

The takeaway? There has never been a more important time to modernize your patient payments workflows.
This whitepaper outlines the best practices and strategies to improve payment processes, increase front-end collections and give patients the modern, convenient financial experience they want.
Read this whitepaper to learn:
- Easy-to-implement tips to streamline payment processes and increase efficiency
- How technology can help you automate and standardize time-of-service collections
- Why offering flexible, consumer-friendly payment options helps improve patients’ healthcare experience

Download this whitepaper to learn:
- How to turn the challenges of consumerism into opportunities.
- How to create a flexible, personalized payment experience.
- How to engage patients across multiple channels.

14 must-read articles on emerging challenges and opportunities
The last two years have challenged hospitals and health systems in unprecedented ways. Revenue cycle leaders have overseen shifts to a remote workforce, navigated staffing shortages, managed billing and collections in the face of mounting financial pressures, and adapted to changing patient expectations and rising consumerism. Leaders have achieved varying degrees of success amid this vast disruption and uncertainty. Now, they must look to the future and prepare for what's next.
This collection of articles explores the most consequential revenue cycle trends, challenges, and opportunities for the new year. Topics include process optimization through automation, what finance leaders need to know about recent CMS actions, financial benchmarks necessary to sharpen RCM, and more.
Your journey to revenue cycle success in 2022 starts here.

This measurement will come in the form of having real-time and immediate financial data. And this will create an evolution that will help healthcare finance teams get out of the back seat and steer the strategic direction of a healthcare organization.
Download this eBook to learn a myriad of insights, including:
- The Future of a Data-Driven Healthcare Finance Team
- Healthcare Accounting: Using Agility to Fight the Status Quo
- What is a Healthcare ERP?
**https://go.beckershospitalreview.com/the-future-of-healthcare-finance-0

But growing transparency is a multi-channel journey that is fundamental to patient loyalty and overall satisfaction. In this whitepaper, learn:
- How patient understanding of billing and costs are crucial to their overall experience.
- What holds most healthcare providers from moving toward a transparent revenue model.
- Steps providers can take to deliver on transparency without compromising their current practices.

Download our Market Update to get the latest information on Debt Collection Practices (Regulation F) final rules.
Objectives:
- Learn what it is, why it is important and the implications of failure to comply
- Review the approved communications with debtors that further defines harassment, abuse, and unfair practices (Rule one)
- Understand the requirements for and timing of disclosures of bad debt collection (Rule two)

Becker’s Hospital Review recently spoke with four revenue cycle experts from about the value of evaluating and optimizing. They described what optimization is, how it works and the benefits to both EHR users and patients.

In this whitepaper, experts from Sound Physicians, who has experience managing over 400,000 episodes and $10 billion in at-risk spending, share what this transition means for hospitals, including:
- Annual financial implications relative to hospital size
- Importance of hospital-physician alignment under mandatory bundles
- Three potential models CMS could select

- How to meet price transparency compliance and what stiffer financial penalties are at stake in 2022 under the newly proposed rule
- How automating critical functions in patient access helps maintain the data integrity necessary to generate accurate price quotes, increasing your ability to collect payment prior to service
- Why a consistent patient financial experience is critical to increasing patient satisfaction and trust, and why aligning price estimates and quotes requires one platform
- How combining a machine-readable file, patient-facing estimation tools and payments exceeds compliance measures, enables consumerism and maximizes revenue


Hospitals are all too familiar with the patient affordability crisis. Patient responsibility has more than doubled in the past 20 years and is expected to double again within the next ten.
Still, too many hospitals rely on in-house teams and traditional patient financing solutions that simply don't work. Not only do these programs strain internal resources, but they produce a poor patient experience while bringing in only 15 to 35 cents on the dollar on average for patient responsibility after insurance. With the right solutions and financing options, hospitals can increase collections while at the same time taking debt off their books without recourse.
This whitepaper contains:
- An overview of the patient affordability crisis by the numbers
- Five ways to transform patient affordability
- How Geisinger used fintech to boost collections by 80 percent

Learn more about the partnership here.

In this ebook, you'll learn:
- The current payments context driving urgency for change
- The leading pain points along the patient financial journey
- A three-step playbook for implementing a versatile payment strategy that enhances the patient experience

Download the guide to learn:
- The basics of intelligent automation, including artificial intelligence (AI) and robotic process automation (RPA), and the role they play in a touchless revenue cycle
- How to prioritize use cases for intelligent automation based on business, human, and automation impact
- How to define the ROI for intelligent automation in the revenue cycle
- Why a test and learn approach is necessary to scale quickly and drive impact

Since the launch of the Community Care Network, providers have found themselves dealing with the VA more and more. Just as this new program was getting off the ground, however, COVID-19 led to hospital staffing shortages, the retirement of experienced employees and reduced productivity due to remote work arrangements.
VA claims can be a significant source of hospital revenue, but they require specialized knowledge to bill and collect.
Hospital CFOs and revenue cycle leaders can benefit from this white paper to learn:
- How the various VA community care programs operate
- Why working with the VA is not the same as working with a typical insurer
- How the VA denial and appeal process differs from that of other payers
- Why outsourcing may be the best way to ensure every possible dollar is collected on these claims

However, there is a solution: Proven AI technology increases accuracy in healthcare fraud detection while minimizing false positives.
Read this whitepaper to learn how:
- Proven AI fraud prevention technology is being applied to healthcare fraud, waste and abuse
- Advanced AI detects and prevents fraud before the claim is paid
- Higher detection rates and fewer false positives allow you to focus on more complex FWA schemes

- Common barriers hospitals face in paying doctors and how to overcome them
- The benefits of physician payment automation and how various departments, from finance to compliance to doctors themselves, can take advantage of this type of approach
- Actionable steps hospitals can take to evaluate physician payment technology based on their specific needs

In a June advisory call, finance executives from health systems like Banner Health, Methodist Health System and Spectrum Health discussed how they're prioritizing the patient's financial experience.
Key takeaways from the discussion were featured in a whitepaper. Which include:
- Strategies on patient education, personalization and price transparency
- How training, technology and recognition leads to staff support
- The power of finding a partner for patient financial services

The 2021 Retirement Survey Report provides detailed information and insights on how organizations responded to the impact of COVID-19, including:
- Addressing employee financial stress
- Managing their fiduciary responsibilities and limiting fiduciary liabilities
- Evaluating plan design and more

- Learn how to identify a collaborative value-based approach to construction using data and software to create a more flexible and adaptable healthcare facility
- Discover alternatives to the fee-for-service model of construction
- Learn how verified construction procurement data can help control costs

Onboarding new employees is an incredibly time-consuming and oftentimes money-wasting process. By implementing digital workflows into the onboarding process, hospitals can make it easier and faster for clinicians to begin seeing patients.
Download this infographic to learn how digital workflows improve the way hospitals manage onboarding and other clinician lifecycle events.

This practical guide contains scheduling strategies that will empower staff, reduce turnover, boost productivity and cut costs.

This white paper synthesizes an advisory call that Becker's Hospital Review and Flywire hosted in April with CFOs and revenue cycle executives from organizations like Cleveland Clinic Florida, Ochsner Health and Vanderbilt University Medical Center. During the call, leaders discussed how they use technology to improve patients' financial experiences and how the shift to virtual care is affecting their operations.
Learning points:
- How leaders are prioritizing price transparency and automation
- The benefits of digital tools targeting patient affordability
- The value of digital front doors

Download this white paper to learn:
- How to accelerate technology and process innovation
- The differences between traditional outsourcing and a strategic partnership
- 5 key reasons to adopt a partnership model
- Structuring a partnership to share more risk and gain more benefit
- Things to consider when selecting a strategic partner

Download this e-book to learn why implementing a single, integrated digital patient access, intake and engagement platform is critical to improving patient and staff safety and satisfaction while increasing net revenue.

This whitepaper, developed from a three-part study conducted by HIMSS, and sponsored by Spectrum Enterprise, looks at:
- How telehealth services evolved through the pandemic and the value of virtual care beyond the pandemic
- How HCOs are funding telehealth advancements
- How telehealth helps providers attract and retain patients, trim overhead costs, increase access to care and reduce appointment cancellations
- Building a robust telehealth program that ensures strong patient outcomes, an exceptional patient experience and long-term financial stability

Learn about the 10 criteria used to determine the efficacy and sophistication of your purchased services efforts, and how they compare with others in the market including:
- Spend usage and visibility
- Contract terms and visibility
- Leadership, staff and skillset


This white paper explores how identifying and focusing on the members most likely to experience chronic disease complications in the next 12 months can deliver results.
In this case study, you will learn how one health plan:
- Saved an estimated $7,500 for each identified member
- Recaptured $3 for every dollar spent on case management administrative costs
- Improved member engagement and satisfaction

- The main issues behind physician burnout
- Effective ways to address emotional and financial stress
- How to apply pandemic lessons to the future healthcare operations


Costly write-offs remain a problem for many hospitals and practices. This is especially the case with commercial claims, which are marked by denials and complicated, labor-intensive appeals.
ERISA Recovery's new white paper offers an in-depth look at this topic, with a focus on:
- How focusing on denied, aged commercial claims can improve revenue
- Why ERISA appeals are the ideal solution for such claims
- How ERISA Recovery operates, without impacting existing processes
- How ERISA Recovery collects on aged claims going back up to 10 years
- How all appeals are handled stateside


Highlights include:
- Why early patient engagement saves healthcare providers money in the long run
- How to collect from all payment sources
- Where in the revenue cycle to implement technology-driven solutions to boost revenue

- A background on ERISA and its complexities
- Why ERISA appeals are underutilized in the hospital revenue cycle
- Which plans are covered by ERISA
- Which adverse benefit determinations are appealable under ERISA
- A comparison of an ERISA appeal vs. a traditional denial appeal
- And more…

Three learning points from the eBook:
- The four primary challenges from the COVID-19 pandemic will mark providers' next 12 months
- The immense burden patients and providers face due to rising healthcare costs and what to do about it
- Insights on the technology that is altering the healthcare landscape, including telehealth, workflow automation, information security and digital payments

Additional insights from the advisory call, featured in an e-Book sponsored by Flywire, include:
- Many systems are already providing their patients tools like online price estimators, but hospital and revenue cycle leaders are concerned that disclosing contractual rates won't be helpful for patients
- Price transparency alone can't solve for healthcare's affordability challenge, especially as more patients have high-deductible health plans
- Advocacy, experimentation and new technologies will all be necessary as healthcare providers promote patient engagement and revenue recognition.

Payer executives from hospitals and health systems across the country discussed how they're working to increase access to high-quality, cost-effective specialty testing to rein in costs during a roundtable at Becker's Spring 2024 Payer Issues event.
Major themes examined during the conversation include:
- The evolution of lab services
- How shifting the site of testing can unlock economic savings
- Managing patient and population health through data-driven decision support

In this survey report, you'll learn about current VBC pain points, technologies and plans for transforming care management, per the experiences and insights from 110 payer executives.
Download the report to access key findings, including:
- Lack of interoperability is posing significant barriers to payers' progress in VBC.
- More than one-third of those surveyed are struggling to execute coordinated care.
- Best practices and strategies for payers to align data and tech to advance VBC.

Becker's Healthcare recently hosted a panel-style webinar with three healthcare leaders who shared how organizations can break through these barriers and achieve effective and efficient care management programs. They examined the current state of care management, proposed improvements and discussed how a comprehensive data approach can enable contextual awareness.
Major themes examined during the conversation include:
- Why conventional care management strategies aren't driving positive results
- How healthcare organizations can cultivate patient relationships built on trust
- Why patient data capture must adapt to the patient journey

In this research-based guide, you'll learn the critical challenges and strategies for developing a modern data platform that can effectively integrate, manage and utilize real-time data for better healthcare outcomes.
Key learning points include:
- The significance of embracing platform thinking to overcome fragmented healthcare data systems and the importance of real-time data integration for actionable insights
- Strategies for achieving seamless data integration and overcoming the technical challenges associated with real-time data ingestion, interoperability and integration of both clinical and nonclinical data sources
- The key role of DataOps in monitoring and ensuring the quality, security and compliance of healthcare data

This white paper explores current trends and forecasts future developments in healthcare data analytics and interoperability aims for EHRs. Embracing these trends will be key for healthcare organizations striving to stay at the forefront of innovation, quality care and compliance.
Learning points:
- Achieve a more efficient, accurate and member-focused system
- Improve data quality to positively affect member care and outcomes
- Modernize quality measurement systems

Health plans that take a comprehensive approach to payment integrity can reduce overall costs while minimizing low-value activity and stakeholder abrasion. This whitepaper details how payers can begin to make that shift, along with trends in the industry and considerations going forward.
You'll learn how to:
- Increase claims accuracy, enhance coordination of benefits and refine audits
- Move past traditional data handling processes to get actionable insights
- Use AI and machine learning to reduce billing errors and fraud

Every year, cardiometabolic conditions, including diabetes, cost employers and health plans upwards of $500 billion dollars. Continuing to treat these conditions in silos simply won't cut it: To realize better member outcomes and health plan savings, the full spectrum of these conditions needs to be addressed, and a single platform is supporting organizations to do it.
Read about a virtual care solution that can increase your health plan's ROI by:
- Serving diverse populations with members of all ages, backgrounds and cardiometabolic health acuities in one platform
- Encircling members with personalized, human-led care teams to address and treat co-occurring cardiometabolic conditions at the same time
- Guaranteeing cost savings for health plans in the form of reduced expensive hospital visits and medical interventions

Download this ebook to learn:
- How health equity is key to driving revenue
- The importance of the digital member experience
- Tips to help members navigate burdensome medical bills

Instead, health plans must work to identify an all-inclusive remedy that offers members a realistic and effective approach to diabetes management. This guide discusses the problems with "diabetes reversal," the connection between diabetes and mental health, and more.
Download the guide to discover:
- Why diabetes remission is a better goal than diabetes reversal
- Why treating diabetes and depression together maximizes positive outcomes
- How personalization plays a critical role in effective diabetes management

This collection of 10 articles touch on the significant challenges and opportunities health plans face in this transformative moment. Topics include the state of Medicare Advantage markets, population health and regulatory policy.
Healthcare transformation is here. These articles offer an overview of where the industry is and where it might be headed.

Ongoing exclusion monitoring and license verification doesn’t have to be a manual, costly burden. Centralized provider eligibility and monitoring intelligence ensures data insights exist where stakeholders need it most - and empowers efficient communication across teams. Discover the benefits of one powerful platform with a flexible API that breaks down silos — improving quality of care for your members and reducing both medical and administrative spends for your organization.
Download this white paper to learn about:
- The benefits of centralizing provider data in one platform
- Advantages of continuous provider monitoring
- Alleviating gaps in your compliance program with a population-specific workflow design

Health plan leaders in the areas of quality, clinical, prevention, health engagement and population health will find this case study a helpful resource in determining the types of member benefits they should offer.
It walks through a successful chronic disease prevention program and how it used three member engagement strategies to meet its goals:
- Member buy-in and goal setting
- Assisting and advising
- Accountability and follow-up

During a February roundtable discussion sponsored by IBM Watson Health, a panel of executives from healthcare payers shared how their organizations are using analytics and strategies to reduce disparities, lower costs and improve outcomes. This whitepaper reviews the 6 key takeaways from that discussion.

Download our whitepaper, "Beyond the pandemic: How virtual care leads to better outcomes," to discover how virtual care:
- Improves outcomes through increased access and integrated delivery
- Helps people build resilience while addressing mild and moderate symptoms before they become more severe
- Helps hesitant populations get mental healthcare through what Vida calls the side-door approach

No longer a commodity, identity data management and EMPIs (Enterprise Master Person Index's) have been reinvigorated. EMPIs are not what they used to be — and that’s a good thing.
Learn how next-generation identity management technology has made leaps over legacy software in recent years to support health system and health plans’ goals of a clear, 360-degree view of patients and populations.
Use this guide to:
- Build your identity roadmap with a checklist of requirements
- Determine the total cost of ownership and avoid capital expenditures and resource investments common to enterprise data management
- Raise the bar on implementation & services to keep up momentum
- Compare EMPI costs and time to value with an interactive worksheet

The challenges of the past few years combined with an already arduous schedule have many healthcare workers leaving their organizations, or the industry entirely, because of insufficient family care and education benefits.
To compete for and retain top healthcare talent today, organizations must offer an employee experience that meets their unique needs.
Download this guide to learn:
- The top contributors to healthcare employee burnout and turnover
- How to evaluate the right mix of care benefits to serve the unique needs of a diverse workforce
- How offering family care benefits can have a profound long-term business impact

This white paper includes the insights and tools needed to tackle the complexities of talent acquisition in the healthcare industry and provides talent strategies to address clinical labor shortages in the healthcare recruitment landscape. Learn how to implement scalable and flexible recruitment strategies, create compelling recruitment campaigns, foster candidate engagement, and build a talent pipeline that drives organizational growth.
Key learnings:
- Gain actionable tactics to elevate your healthcare recruitment efforts
- Explore how candidate marketing can be used to attract and retain top-tier talent
- Discover insights on building a talent pipeline that drives organizational growth

In this white paper, you'll learn how a $6 billion health system revolutionized its workforce management through an innovative, on-demand nursing tool. The health system achieved $85 million in savings, streamlined onboarding processes and optimized staffing levels across its 23 hospitals. By successfully onboarding 1,500 healthcare professionals, the health system demonstrated its current growth and commitment to meeting healthcare demands.
Read more to learn:
- How the health system saved $85 million through strategic implementation of an on-demand nursing technology
- The benefits of flexible scheduling options and expedited onboarding processes in optimizing workforce management
- How this technology facilitated seamless transitions to full-time employment for healthcare professionals

Flexibility has become an increasingly important part of a health system's workforce strategy. Clinicians are consistently pointing to scheduling flexibility as a key factor that reduces work-related stress and burnout.
Health systems that have aced their flexibility strategies have tapped into on-demand staffing solutions, like Medely, to address administrative burdens, improve patient care and drive savings. Download this brief eBook to learn more about how systems are delivering the flexibility clinicians expect, while saving on excessive overtime costs and improving nurse satisfaction.
Key learning points:
- Minimize recruiting costs through direct access to pre-screened professionals
- Avoiding excessive overtime
- Strategies to improve retention and morale, and enhance patient care through Medely's flexible scheduling options.

Left unchecked, healthcare's workplace violence crisis will have profound effects on staff engagement, patient satisfaction and quality outcomes. With workers increasingly facing violent and aggressive events on the job, safety has emerged as a central focus for hospital and health system leaders.
Increasingly, nurses and other workers are prioritizing safety in their choice of employment. Now, hospitals are strengthening their approach to foster and elevate a culture of safety and transparency to protect patients and staff, and ensure teams can work without fears about a lack of security.
Becker's and Commure recently caught up with hospital executives to learn more about how their organizations are bolstering security and fostering a culture of safety.
Download a summary of the conversation to learn about:
- Specific security-related interventions hospitals are seeing success with
- Effective, transparent communication with employees about safety measures
- Best practices for creating an integrated safety strategy, and the role technology plays

This guide can help hospital leaders and executives supplement or accelerate their work on professional well-being at the operational level.
What makes this guide special:
- Builds upon existing research and resources from organizations who have made strides to address healthcare worker burnout.
- Includes six evidence-informed actions with useful background information and tools to fully equip leaders to make improvements.
- Real-world tested in six hospitals across the United States.

TeamHealth worked around these challenges by implementing a hospital medicine productivity program that raised productivity by 7.7% while increasing early discharges and lowering readmission rates. This case study outlines their strategy.
Download the case study to learn:
- Key takeaways for implementing a productivity program that doesn't overburden physicians
- How to use data to boost productivity and maximize revenue
- A robust set of tactics for leaders to draw from

For the first time since the start of the pandemic, employee engagement is on the upswing, according to Press Ganey's analysis of data from 2.2 million U.S. healthcare workers. However, retention remains a key challenge for healthcare organizations, especially among nursing roles.
This white paper offers a state of the union on the healthcare workforce in 2024, highlighting key trends and strategies organizations can use to boost employee retention and experience.
Key learnings:
- Employee engagement trends, segmented by role
- Key turnover trends and how to mitigate flight risks
- The key drivers of employee retention and engagement

Integrating and scaling much-needed behavioral health services is a challenge, especially when rural communities or high-acuity patients are involved. This white paper details potential roadblocks and offers a path forward for hospitals to create a financially sustainable program.
You will learn:
- How health systems are approaching integrated behavioral health care
- The current challenges facing health systems and potential solutions
- Best practices for delivering true behavioral health integration

To provide the best possible care and optimize health outcomes for patients served, understand how to enable your staff with continuous learning opportunities and strengthen your culture of learning.
In this white paper you will learn:
- What a learning organization looks like
- The 5 disciplines of a learning organization
- How to create and sustain a learning organization

This guide explores the features and advantages of internal agencies and internal float pools and presents case studies demonstrating how clients have executed and achieved favorable outcomes with these solutions.
Health systems that implement internal agencies or internal float pools achieve outcomes including:
- Proactive management of staffing needs
- Increased flexibility to serve areas of highest demand
- Improved fill rates
- Reduced contingent labor spend and overall labor costs
- Improved employee retention

Bon Secours Mercy Health, a 48-hospital system based in Cincinnati, solved the problem of manual data entry through a new integration with their EHR. This whitepaper outlines how the system improved efficiency, regulatory compliance, and patient and provider satisfaction through the new program.
You will learn:
- Potential barriers to language services compliance
- How to eliminate manual data entry and free up time for providers
- How Bon Secours cut report generation time by 50% while dramatically improving data quality

The new 2024 Survey of Hospital Nurse Leaders delves into the workforce management tools and technologies CNOs and other nurse leaders are implementing and where they're seeing the most success in addressing key issues including shortages and scheduling problems.
Key findings:
Three top challenges nurse leaders are facing
How burnout is affecting nurse leaders
The three most useful workforce management and support tools

In this white paper, you'll see results from a front-line nurse career report, which highlights survey findings from 500 active clinicians across 164 health systems and their needs, preferences and views on how leaders can build the future of nursing across generations.
You will learn:
Top preferences for achieving a healthy workforce and higher retention rates
Nurses' desires related to scheduling and travel/rotational programs
Key recommendations for supporting flexibility

In this industry report, you'll learn more about where AI technology can be applied in executive recruiting, its potential benefits to talent management and its limitations.
Download to read more about:
- The facets and current state of AI in the healthcare market
- Use cases for AI in executive recruiting (e.g., drafting core documents, building candidate panels and evaluations, talent insights etc.)
- Concerns about this budding technology

With labor expenses accounting for 50% of hospital costs, tackling these workforce issues is essential to getting labor costs under control. To navigate this complex landscape, healthcare decision-makers must have a future-ready workforce strategy.
In this white paper, you will learn how a flexible workforce model can help healthcare facilities cut down on labor costs and achieve financial sustainability.
Key learning points:
- Introduce a solution that can empower healthcare facilities to effectively address workforce challenges.
- Learn how to leverage a flexible workforce model to enable elastic provisioning effectively.
- Explore the benefits of implementing a flexible workforce platform to ensure your workforce strategy is future-ready.

This white paper details how comprehensive services offered by medical equipment distributors can help health systems contain costs and improve efficiency.
You’ll learn:
- How medical equipment distribution services can help improve staff retention, efficiency, and cost containment.
- What to look for when choosing a medical equipment distributor.
- How systems like NewYork-Presbyterian and PeaceHealth profited from services offered by a medical equipment distributor.

Key learnings:
Building a flexible workforce to fill shifts at a lower cost than contingent labor
The importance of a multigenerational staffing model
Reducing agency staffing from 25% to 8% of total clinical workforce
Real-world clinical and financial results Mercy has achieved
As the demand for nurses is growing steadily, exacerbated by an estimated 640,000 nurse retirements between 2020 and 2030. Nurses are also facing increasingly difficult working environments that are taking a toll on their emotional health, spurring some to leave the profession entirely. Health systems adapting to these headwinds with technology are emerging as leaders in nurse retention, growing access to care, with a focus on the bottom line.

We compiled 10 must-read articles featuring insights from industry leaders that demonstrate the current state of the healthcare supply chain and the types of strategies hospitals and health systems are embracing to strengthen their organizations.
The stories examine:
- Key factors driving challenges across the medical supply chain
- Strategies leading hospitals and health systems are employing to safeguard their supply chains from a range of disruptions
- How technology fits into supply chain strategies

In this white paper, you'll learn five strategies that cut labor expenses without compromising patient care, promote flexibility and improve workforce management.
Download now to create a lean, efficient and effective healthcare workforce with:
- Strategic staffing solutions that help manage workforce flexibility, adjust staffing levels based on patient demand and minimize unnecessary labor expenses
- Innovative cost-reduction techniques that embrace the gig economy via local marketplace platforms
- Data-driven decision-making with technology that uses advanced analytics and forecasting algorithms to accurately predict patient demand

Dive into this whitepaper and learn more about the three purchased services key trends for 2024:
- Addressing Workforce Challenges
- Leveraging “AI” for Contract Management
- Advancing Supplier Diversity

This doesn't just make for a dangerous work environment for healthcare workers — it also instills fear in patients and worsens public perception of the healthcare industry at a time when public trust is already falling. In a 2022 survey, 40% of respondents said they didn't feel safe entering a hospital or medical facility. To combat this and keep employees safe, healthcare leaders need a strong game plan.
Download this whitepaper to learn:
- How workplace violence is affecting staff and patients
- Data on the state of hospital safety today
- 3 proven strategies for better protecting your patients, staff and overall healthcare campus

Combining data analytics, workforce strategy, and recruitment into a technology-forward, total talent solution, AMN Healthcare prescriptively identified Temple Health’s staffing needs and created a foundation of data guidance and utilization to reallocate and balance their workforce.
Download the whitepaper to learn how Temple Health:
- Maintained a steady 92% fill rate
- Reduced employee turnover by 4.1%
- Achieved a total cost savings of $12,250,000 as of 2023

In this e-book, you'll learn how organizations are applying technology that gives providers, nurses and staff more control over their time through self-scheduling, as well as the benefits of putting the schedule at the center of a workforce management strategy.
Download for insights on:
- The importance of scheduling in managing healthcare staff, including ways to enhance operational efficiency and reduce labor costs
- Strategies for balancing workloads, reducing burnout and creating a more positive work environment, leading to improved patient care
- How a unified, schedule-centric approach can streamline healthcare workforce management and provide actionable insights and holistic visibility

In the following eBook, you'll learn about successful initiatives at a variety of leading providers including Pittsburgh-based Allegheny Health Network, Jacksonville, Fla.-based Baptist Health and Nashville, Tenn.-based Ardent Health. Each of these organizations has leveraged an education partnership to achieve positive results that aim to benefit both employees and patients.
Participants will learn:
- How healthcare organizations are leveraging education to address industry change and challenges.
- How to leverage education benefits as a framework for a healthy workplace strategy.
- How leveraging education can help recruit, retain, and upskill not only healthcare employees, but employees across the entire organization.

How are the most successful hospital and health system marketing teams navigating this challenge? This guide, developed by seasoned health system and hospital marketing experts, provides direction on how to overcome some of the most common challenges today's marketing teams are up against.
Learning points:
- How data and tech improve targeting and optimize campaign performance
- Best practices to optimize your marketing team's strategy and shifting priorities
- Questions to ask martech health care marketing vendors and agencies

In this white paper, you'll find takeaways from an executive discussion with CEOs, COOs and nursing and HR leaders on their short- and long-erm strategies for addressing this issue. They share:
- How they're forging connections with local, prospective clinical students via events + social media
- Challenges faced in recruiting support staff for physicians
- The need for customizing retention strategies based on community/staff needs

This white paper details the survey of 650-plus healthcare leaders and dives into the biggest trends and challenges for the coming year. From growth initiatives to recruitment and retention strategies, this report offers a wide range of insights for the year ahead.
You'll learn:
- 7 key trends in healthcare for 2024
- Leaders' top areas of focus to drive organizational growth
- Recruitment and retention strategies for today's workforce

In this white paper, Valerie Bandy, PharmD, MBA, BS, RPh, offers a pharmacist's perspective on the challenges keeping pharmacy leaders up at night, and describes how U.S. health systems and hospitals are mitigating and even solving them through supply chain management optimization.
Key takeaways:
Explore what challenges pharmacy and healthcare leaders are facing today.
Implement strategies to mitigate the impact of several challenges through an end-to-end supply chain management solution.
Assess and identify opportunities to centralize pharmacy services into a consolidated pharmacy service center performing procurement, operational and clinical services.

One university health system partnered with its logistics management provider and leveraged data analytics to spearhead better collaboration with its suppliers, helping to meet its goals and cut costs. This whitepaper details their success story and the methods they used to reduce complexity and drive savings and efficiencies.
Insights include:
- Facilitating the right conversations with stakeholders
- Leveraging data to help lower costs, increase efficiency and streamline operations
- Setting strategic goals that will put you on the path to success

In this short guide, you'll learn how a data-driven system is helping hospitals and health systems optimize permanent, per diem and locum tenens employees, as well as streamline scheduling.
Download to learn more about:
- Key operations, processes & capabilities of a vendor management system
- Why data and reporting empower locums processes
- How to determine if a VMS is the right tool for your organization

With the right technology, it’s possible to retrofit, upgrade and modernize healthcare facilities while minimizing disruptions to patient care and staff workflows.
Download this e-book and get the keys to improving environmental, financial and patient outcomes through operating expenses and not capital expenditures.
You'll learn how to:
- Improve patient care and the patient experience by modernizing older infrastructure.
- Increase safety and security to drive staff retention and manage your reputation.
- Implement technologies to help manage energy use and save operating costs.

Nearly half of U.S. healthcare leaders have had to cancel or reschedule cases at least quarterly in 2022 due to product shortages. Preparing for, responding to, and recovering from disasters, disruptions and traumatic events is essential to overall resiliency for healthcare providers, their supply chains and communities alike.
Download this short report to learn how your organization can future-proof its supply chain and be prepared for the unexpected. It covers:
- Resiliency best practices
- Quick tips for vetting suppliers
- 3 key actions to prepare for any disruptions

Conducting healthcare background checks requires maintaining compliance with different federal and state laws, and helps you meet certain federal funding and industry requirements.
In this whitepaper, you'll learn how background checks can help your organization deliver improved patient outcomes, promote a safer work environment and limit liability.
What you'll learn:
- How to think about risk management and your screening program
- Background check laws you need to know
- Different types of background checks and how they can help you meet regulatory requirements and promote safety.

Some organizations, however, are seeing improvements in decision-making with technology that enables enhanced visibility to locum tenens staffing.
Download this brief white paper to learn more about:
- How business intelligence can support the entire organization
- The key data and reporting capabilities that empower locums processes
- Perspectives on implementing vendor management system technology

In this white paper, you’ll learn how the University of Miami Hospital and Clinics (UHealth) is leveraging a powerful, technology-based approach to workforce engagement: sharing real-time recognition from grateful patients, families and colleagues with staff members.
Download for access to insights on:
- How patient gratitude can help to combat challenges like employee burnout
- The ways technology can streamline feedback & recognition and make it more effective
- Why staff recognition initiatives should be prioritized now

While options for staffing partners abound, many specialize in only a few key areas. This whitepaper outlines how to choose a workforce partner that can provide efficiency and cost savings across your entire enterprise.
You will learn:
- 8 things to look for in a workforce partner
- How to consult and contract with the right partner
- How one state healthcare organization handled various surges in patient volume from 2020 through 2023

For healthcare entities willing to navigate this intricate terrain, the roadmap is clear: leverage data intelligently, engage with physicians actively, be adaptable to changing regulations, invest in continuous learning, and place the patient at the center of all decisions. As challenges arise, so do opportunities, and those prepared to seize them will shape the future of healthcare.
The survey presented in this whitepaper underscores the importance of a technology-backed, collaborative, and patient-centric approach to healthcare value analysis.
Key concepts that you will learn about:
- Optimized Data Management and Product Evaluations: Learn how embracing centralized tools and processes can transform price data management and new product evaluations.
- Advancing Decision Models: Gain insights into transitioning from clinician preference or cost-based models to more informed, standardized decision-making approaches.
- Data-Driven Healthcare Insights: Understand the pivotal role of data and analytics in steering the future of value-based care.
- Clinical Engagement in Decision-Making: Recognize the critical need for physician involvement in value analysis and gain insights on how to close the current gap.
- Criticality of Financial Literacy in Value Analysis: Grasp the importance of understanding key organizational metrics, such as Net Patient Revenue.

Like many systems, Fredericksburg, Va.-based Mary Washington Healthcare was already struggling to handle patient loads before COVID-19. The onset of the pandemic brought operational woes to a tipping point. This short case study examines how the organization has since achieved operational excellence, with $36.2 million in financial benefits annually, safer care and strong staff satisfaction.
The brief report covers:
- How Mary Washington Healthcare's systemwide transformations led to staggering financial improvements, including savings from length of stay improvements, a reduction in healthcare associated infections and more
- How operational excellence drives safer, higher quality care as well as strong staff engagement and satisfaction
- Why having a partner that aligns its resources to your priorities is key to successful continuous operational improvement

Research shows that healthcare workers are looking for companies that provide on-demand pay. A November 2022 Harris Poll survey commissioned by IntelyCare and DailyPay found that 71 percent of healthcare workers would be more likely to remain at a job if their employer offered an on-demand pay benefit than if they didn’t offer one.
This white paper reveals research-based insights that demonstrate:
- The speed of on-demand pay adoption in the healthcare industry
- The impact on-demand pay is having on employees and how it's translating into accelerated recruiting and increased retention for employers
- How on-demand pay works so you can evaluate the potential for your business

This white paper examines three challenges that will dominate the industry throughout 2024: financial constraints, workforce disruption and growing competition. The crosscurrents produced by these challenges will be explored, along with their implications for talent management strategies.
Key learnings:
- Implications of workforce disruptions and solutions being explored
- Organizational strategies that are taking center stage to stimulate top-line growth
- Strategic considerations to help leaders navigate these crosscurrents

Every second wasted tracking down the right provider can have serious repercussions. Lacking centralized visibility into who's on call, clinicians often end up searching multiple sources or accessing outdated schedules.
With patient demand, provider burnout and turnover on the rise, this chaotic approach to on-call scheduling is simply not sustainable. Rethinking on-call scheduling must be a top priority.
Download the e-book to:
- Uncover the high-stakes consequences that on-call inefficiencies can have on patient care.
- Discover how a unified on-call platform improves accuracy and efficiency.
- Identify best practices for choosing an on-call scheduling solution and ensuring a thoughtful and structured implementation.

It's clear hospitals and health systems looking to keep up with innovation and attract top surgeon candidates need to implement or expand robotic surgery programs. In this ebook, experts from New Hyde Park, N.Y.-based Northwell Health and San Diego-based Sharp HealthCare detail how their systems got started and the benefits they've seen from their da Vinci robotic-assisted surgery programs.
You'll learn:
- Meta-analysis data on robotic surgery outcomes
- The right investments for long-term success in the robotic surgery space
- How to expand your robotics program without breaking the bank

Oncology leaders are on top of it: In a recent survey, 90 percent said they saw reducing care variation as a priority. Yet many organizations still rely on multiple manual processes to standardize care, which adds to the total cost of care and burdens clinicians and administrative staff.
This whitepaper dives into insights from 134 oncology leaders on their priorities, strategies and views on the future and details how organizations can more easily achieve care standardization.
You'll learn:
- What clinical pathways leaders are already doing to reduce care variation at their cancer centers
- How to identify and tackle sources of unwanted care variation
- The tech solutions that can help reduce costs, improve patient outcomes and unburden staff

This white paper outlines how hospitals can use W-2 marketplaces as a bridge to hire permanent nurses and ensure uninterrupted patient care. From streamlined staffing to risk management, find out how these platforms redefine workforce excellence, elevate patient outcomes and reduce overall expenses.
Key Points:
- How an on-demand local workforce reduces overall expenses while continuing to engage, support and attract your workforce
- How a nurse marketplace leads to less reliance on agencies, lower labor costs and increased retention rates

This white paper overviews key statistics on violence in healthcare settings today, how legislative measures may change requirements for organizations, and proactive measures that mitigate risks.
Learning points:
- Understand the growing scope of workplace violence in healthcare & the cost to patients, staff, and organizations at large
- Gain insights for conducting a thorough risk assessment of your workforce's safety, wellbeing, and preparedness for workplace violence
- Discover potential sources of workplace violence and determine how to address, deescalate, or prevent each of them as quickly and efficiently as possible

Every part of the consent experience can be improved with a digital process that puts people over paperwork. Digital consent collection enables your staff to collect an eSignature from the patient at the bedside or during an appointment. No paper is ever needed. The form is instantly available to the care team — anywhere, anytime and on any device. On average, eConsent users save more than 10+ minutes per consent completed and two to three days of archiving per consent.
This e-book examines how a simple change in your current consent process can have an outsized impact on your organization and community.
Learning points:
- The true costs of paper and manual errors
- How digital consent collection can improve patient and staff experience, decrease surgical delays and eliminate equipment costs

This white paper outlines how one of the top academic medical centers in the nation used innovative enterprise workforce management approaches to address these challenges, including establishing an internal agency pool. See how the organization optimized its use of external agencies and travelers while achieving an 86 percent registered nurse fill rate consistently over the course of 2022.
Key learnings:
- The strategic, three-layer protocol used to deploy team members
- The technologies necessary to centrally manage all staff
- The unique employment model that helped improve retention and bring back nurses who had left the organization

Many organizations are using managed service providers, vendor management systems and staffing agencies to address these challenges. However, these solutions are outdated, costly and often make managing staff and resources overly complex.
In this whitepaper, industry experts share innovative, technology-driven approaches to mitigate staffing shortages while managing rising labor costs to ensure sustainable, high-quality patient care.
Key learnings:
- The shortcomings of outdated staffing solutions
- How technology can optimize internal resource management, enhance staff scheduling with external resources and improve operational efficiency

In this 2023 Survey of Registered Nurses — the most comprehensive one of its kind — you'll see the viewpoints of more than 18,000 nurses that show the depth of the problems they're facing today. In addition to insights on the pandemic's effect on career and job satisfaction, and mental health and well-being, you'll also learn proven, actionable solutions to help support the healthcare workforce.

Having the flexibility of a reliable, on-demand workforce is critical for retaining staff. This whitepaper dives deeper into actionable solutions for retaining top talent, enhancing patient care, supporting your clinical staff, and reducing labor costs.
Learning points:
- 5 key strategies to retain top talent
- Tapping into a flexible, pre-qualified clinical talent on demand
- Overcoming implementation barriers
- How to keep your facility at the top of the ‘best places to work’ list

- An overview of ten different flexible workforce models
- A process to conduct an organizational assessment to choose and build the right staffing model for your environment
- Defining the nuts and bolts of best practice staffing and scheduling policies, and how to choose the right workforce technology
- A look into the future of nurse staffing with the power of AI and predictive modeling
Authored by Danielle Bowie DNP, RN, NE-BC, The Flexible Workforce Handbook [IBSN: 979-8-9888856-0-3] outlines a plethora of best practice recommendations, based on 16 years of Workforce Transformation experience, alongside leaders across variety of organizations in developing innovative workforce strategies to meet their staffing needs. The Handbook concludes with tools, such as a checklist for implementing an internal staffing agency, that help smooth implementation of the book’s ideas to reality.

With data from 150 health care leaders across health plans, providers, employers, life science organizations and government agencies, this 2023 research report reveals:
- Where progress has been made
- Healthcare's greatest challenges
- Priorities for a sustainable and equitable system
- How leaders are advancing on the path to value
- Governance, investment and partnership priorities

Hospital leaders have attempted various strategies to address care variation, however, none have been fully successful because they aren’t addressing clinical variation in real-time.
In this report, we share effective strategies to reduce care variation, improve margins, and ultimately enhance patient outcomes.
Key points that our readers will learn from the paper:
- The root causes of clinical variation and why it’s important to address.
- Effective ways to reduce care variation, and how to combine them into an effective strategy for your health system.
- How to give real-time feedback on care utilization and cost information that help physicians make more informed care decisions.

To ensure financial stability, immediate action is essential. In this ebook, you'll learn six key strategies to engage and optimize internal nurse resources to help you reduce premium labor spend while making progress in addressing the staffing shortage.
You'll also learn:
- Today’s top workforce management challenges and why current initiatives are not sufficiently addressing the problem.
- Creative approaches to retaining nurses and reducing premium labor spend.
- How your current strategy compares to best practices + where there's room for improvement in nurse retention, resource optimization, and labor cost control.

Instead, they’re asked to make phone calls and endure long hold times to do something as simple as schedule an appointment or pay a bill.
Using lessons learned from three leading health systems, this whitepaper offers best practices for optimizing patient engagement with an automation platform.
Discover how:
- Automation drove $2.8 million in annual cost savings for one health system
- Proactive patient engagement can close thousands of care gaps in a short time
- Leading health systems can 2x the number of new patient appointments without creating more work for staff

The right inventory partner can take the stress out of audits, prevent waste and save time. But choosing a partner is a decision that should not be taken lightly. Find out how to evaluate physical inventory count services in this guide.
Key takeaways:
- How to ensure robust and extensive inventory reporting
- Which tech and platform features to look for
- How to approach due diligence in the evaluation process

Yet there’s another layer to these myriad issues: alignment with important community-based physicians.
The relationship between health systems and physician groups is evolving. Ongoing headwinds necessitate better performance in both fee-for-service and value-based arrangements for health systems and their physician partners. The progression of value-based care will either help address or continue to compound the problem. Health systems that fail to adapt their care model and redefine their relationships with employed and independent physicians will continue to face financial challenges.
However, a growing number of systems, such as Health First, Novant Health, and OhioHealth, recognized this opportunity and reevaluated their broader network strategy through a partnership with Privia Health.
“We recognized Privia as having best-in-class practice management solutions and population health capabilities,” Leelee Thames, MD, Senior Vice President & Chief Value Officer at Novant Health Enterprises, told the American Medical Association. “It’s not a vendor transactional relationship. You're part of something bigger, and, as a physician, there is empowerment in working alongside your colleagues towards something greater to improve patient outcomes.”
Privia’s model aims to unite diverse specialties in a cohesive physician network that enables health systems to stabilize their existing physician footprint, possibly expand geographically with a capital-efficient alignment vehicle, and thoughtfully increase their experience and potential success in risk-based arrangements. This adaptable, complementary, and comprehensive model aligns hospital-employed and community physicians across four key domains:
- Strategic
- Financial
- Structural
- Cultural

Effectively managing vendor risk doesn't have to be a burden on your organization's resources.
This white paper details the vital steps you can take to protect your organization and covers:
- How to mitigate risks and vulnerabilities to an acceptable and suitable degree in accordance with HIPAA
- Best practices for identifying threats and protecting protected health information
- Leveraging technology to reduce operational cost and improve compliance

Because it takes six to nine months to fill these vacancies, the time for healthcare organizations to focus on succession planning is now. This whitepaper outlines how to ensure a strong future for your organization's facilities management even as demand outpaces supply of FM professionals.
You'll learn:
- Why facilities managers are key to attracting and empowering your talent
- How to build a robust FM platform to minimize the impact of personnel changes
- How recruiting and training candidates from other fields can help fill crucial talent gaps

More than 75 percent of respondents in a recent survey said they expect supply chain challenges to worsen or remain the same over the next year. But leaders have learned valuable lessons since 2020, helping the healthcare supply chain evolve and become stronger as it emerges from the pandemic.
This white paper dives into responses from a broad cross-section of healthcare and supply chain leaders who shared what challenges they're still facing — and what they're doing about it.
Download the whitepaper to get:
- Survey insights from hundreds of leaders on their biggest challenges
- Strategies for handling risk prevention and mitigation, among other pressing issues
- Comprehensive recommendations for advancing a stronger supply chain

In this e-book, you'll read insights gleaned from an executive discussion with healthcare and IT leaders — from organizations like Paterson, N.J.-based St. Joseph Health and New Albany, Ind.-based Baptist Health Floyd — on the opportunities they see in robotic process automation to reduce staff burden, raise employee satisfaction, mitigate turnover and build a stronger workforce.
You'll learn:
- How automation can empower clinical staff to work at the top of their licenses
- Why technology can't (and shouldn't) replace the human aspect of care — and why it's critical to effectively communicate this to staff
- Generating buy-in for new technology

It includes perspectives on staff burnout, turnover, artificial intelligence and other topics capturing a holistic view of well-being in the industry.
Download this whitepaper to get the full picture.
Four key findings:
- 79 percent of healthcare leaders and 77 percent of healthcare workers have been struggling with burnout in 2023.
- 62 percent of healthcare workers and 52 percent of healthcare leaders want to leave their job.
- 72 percent of workers are "extremely interested" in technology that would cut down on time spent on administrative tasks (compared to 37 percent of leaders).
- 70 percent of healthcare leaders believe there is potential for ChatGPT and generative AI to improve care delivery.

This article offers suggestions on how to overcome some key challenges and contribute to overall surgery center success by optimizing shipping operations.
Key learnings:
- Offset the impact of rising supply costs
- Drive efficiencies even with limited resources
- Maintain clinician satisfaction and quality patient care

Access this short case study to learn more about creating efficient processes and automation that can result in a savings of 20 percent on your labor spend.
This report spells out how to:
- Reduce complexity
- Provide savings
- Support an internal agency

The current landscape is rocky, but with the right strategy, financial stability is still within reach. Using decades of industry expertise and real-world data, this e-book details the top challenges revenue cycle leaders face today and offers step-by-step instructions on refining processes, implementing change and making the most of your healthcare RCM software.
You'll learn:
- The top 4 challenges for today's revenue cycle leaders
- Insider tips for evaluating your current process and creating an improvement plan
- 7 step-by-step processes that revolutionize your revenue cycle

This white paper debunks four common healthcare logistics management myths for leaders and shares how they can maximize shipping efficiencies and savings.
Key learnings:
- The most common logistics management myths
- The biggest opportunities for cost savings
- How to make more cost-efficient decisions about shipping modes

This whitepaper explores how health systems can use automation technology to help relieve the stress and inefficiencies associated with day-to-day operations. The report also outlines best practices for deploying technology effectively and includes survey insights from 117 healthcare leaders about their priorities for technology implementation, automation efforts and reducing staff burnout.
Key learnings:
- The consequences of excessive administrative workloads and staff burnout
- 3 documentation workflows that are ripe for automation
- Tips for successful implementation of automation technologies

In this e-book, you'll find 10 short articles that will prepare you and your organization to finish the year strong, including:
- A streamlined guide on anticipated Medicare payment shifts for the top 10 ASC procedures
- Orthopedic and spine ASC leaders' main concerns for the year + opportunities they see
- A cheat sheet to run a thriving ASC, with perspective from 55 industry leaders — including CommonSpirit Health (Chicago), Johns Hopkins Medicine (Baltimore) and more

With better capacity management, organizations can handle more OR cases without having to add staff and resources, reduce length of stay by identifying and eliminating barriers to discharge, and schedule staffing levels proactively based on more accurate demand forecasts.
During an April summit hosted by Becker's, healthcare leaders nationwide came together to discuss strategies and best practices surrounding capacity management. This white paper offers a summary of the discussion and includes perspectives from the following organizations:
- Gundersen Health System (La Crosse, Wisc.)
- UCHealth (Aurora, Colo.)
- Rush University Cancer Center (Chicago)
- Nebraska Medicine (Omaha)

The key to bridging the digital disconnect is meeting patients right where they are. To understand patients' wants and needs around communication, proven strategies and feedback directly from patients are vital.
This white paper collects strategic recommendations backed by data science, turning more than 700 million data points from 650-plus leading healthcare organizations into actionable best practices for your organization — no matter your current tech stack.
You'll learn:
- Three concrete steps to bridging the digital disconnect and building better patient relationships
- How to maximize your investment in SMS and reach patients more effectively
- How to get patients to follow through with scheduling appointments online — and showing up

In this changing landscape, old processes like manually scanning and filing credentialing information can overwhelm staff and leave more room for errors and delays. A standardized online process can eliminate many of these issues — yet only 33 percent of healthcare organizations are using digital credentialing, according to a 2023 poll.
This white paper breaks down the digital credentialing process and explains how it increases speed and accuracy to keep your revenue intact.
You'll get:
- Tips to speed up your credentialing process
- Features to look for in digital credentialing solutions
- A cost analysis of existing credentialing processes

In the face of a provider shortage, disrupters are adding even more complexity to the already-challenging provider recruitment environment. This white paper from Provider Solutions & Development explores healthcare delivery disrupters, how they are making their mark and impacting the provider pipeline and what you can do to stay competitive.
Key learnings:
- Who's causing the healthcare delivery disruption — and how
- What disrupters' potential impact will be on the provider pipeline
- How to rethink recruitment to be competitive in today's healthcare landscape

Many hospital and health system leaders are realizing how delivering better data to physicians when they need it most —at the point of care — addresses the care quality, cost and time issues they're facing daily.
In this white paper, you'll learn about the people, processes and technology a physician group leveraged to ensure staff had access to the right data at the right time, and the outcomes that ensued, including higher rates of preventive screenings for mental health and cancer, closer monitoring of patients' A1C levels and boosted CAHPS scores.
Read more to learn:
- The greater need for patient centricity today
- Challenges and solutions to delivering better data insights to care teams
- Current and future innovations + partnerships that support value-based care delivery

In this e-book, you'll learn why streamlined credentialing is crucial to provider engagement, accelerating time to patient care and faster reimbursements.
Download to learn more about:
- The impact the credentialing process has on provider and staff satisfaction, as well as financial results
- Five common challenges facing the market and signs that your credentialing system is holding your organization back
- How addressing shortcomings here helps health systems to complete credentialing faster, more accurately and with ease

This groundbreaking work has placed the health system in a national leadership position for building an end-to-end, automated and digital supply chain across its network.
Read about Parkview Health's success in driving down costs, improving efficiencies and capitalizing on savings opportunities.
Key takeaways:
- Strengthen alignment between the supply chain and pharmacy teams for greater efficiency and significant cost savings.
- Develop a centralized pharmacy supply chain distribution model while ensuring regulatory compliance.
- Gain transparency into drug inventory to make data-driven purchasing decisions to support patient care.

Here’s the reality: People over age 65 enjoy using technology, and they want it to play a bigger role in their healthcare experience. Patients of all ages are flexible and forward-thinking, and they aren’t afraid to try new things. And if healthcare organizations don’t embrace digital tools, they may risk losing patients to their competitors.
Phreesia surveyed more than 500 adults aged 65+ about how they want to manage their care, including how they want to check in, manage appointments, make payments and engage with their providers. We dive deep into the survey results and explore their implications in our white paper, Older adults and technology: Creating an age-inclusive, digital-first patient intake strategy. Read the white paper to learn:
- How older adults feel about using self-service healthcare technology
- Which digital tools older adults would use in the future, if given the option
- Key strategies to increase access, make payments easier and help older adults become more activated in their care

Automated "care orchestration" — well-connected data and actions across multiple systems that enable staff to better coordinate patient care — can help hospitals and health systems sidestep many operational inefficiencies and yield significant return on investment.
This white paper offers a research-backed case for automating care coordination, with compelling insights on:
- The major financial and operational pressures healthcare delivery networks face — and how this trajectory can change
- How care orchestration lowers the cost of care, encourages clinicians to perform at the top of their licenses and promotes better patient experiences
- Case studies that show sizable improvements with automation, like 60 percent reduction in total cost of care, 130 percent increase in care team capacity and an 82 percent decrease in clinician time spent in patient charts

To better control costs and ensure access to flexible staffing options, some health systems have opted to establish internal agencies.
This whitepaper walks through the key components of establishing an internal agency, including the use of analytics, strategies to acquire staff, and deployment methodologies to deliver staff to areas of need.
In this whitepaper, you'll learn:
- Analytic inputs used to identify proper numbers of core and flexible staff
- Effective strategies for acquiring and deploying staff
- How a multilocation East Coast academic medical system saw success with a tech-enabled internal agency

To enact real change, prioritizing staff wellbeing must be a strategic goal. Discover ways to put the power back in the hands of your staff.
In this whitepaper, you'll learn:
- Ways to improve nurse retention rates
- How to reenergize burned out employees
- Practices for enhancing employee flexibility and autonomy

This white paper identifies the root causes of workforce upheaval and offers five key strategies for healthcare organizations to methodically adjust policies, procedures and practices for immediate stability and long-term growth.
Uncover strategies for balancing supply, demand and system transformation through:
- Reconnecting talent to purpose and performance
- Finding the right relationship between people and technology
- Expanding the use of intelligent data
- Building an anywhere, anytime workforce
- Mapping an enterprise-wide workforce strategy

It also details how leading health systems like Intermountain Health have successfully deployed automation-based solutions to the tune of 68% completion of pre-visit registration and intake and a 300% increase in co-payment collections.
Additionally, you will learn:
- How digital access drives patient loyalty and why it matters.
- Why the front end is where revenue capture goes wrong.
- How to deliver a unified approach to patient access.
- Best practices for transforming patient access in today’s environment.

Most ASCs do not.
As a result, ASCs deal with inefficient, server-based technology, spending an increasing amount of time on clinical documentation frustrating clinicians and administrative staff.
Learn how ASCs are increasing efficiency and reducing costs by switching to a clinical documentation solution tailored to ASCs' unique needs.
Find out how your ASC can experience:
- A 10-minute reduction in MD documentation time per procedure
- A 15-minute reduction in administrative billing time per procedure
- An increase in revenue from improved coding and billing accuracy
- An increase in patient volume due to increased referrals from the software’s ability to track and manage referring physicians

However, these requirements are far beyond an electronic health record's core clinical data management capabilities.
Download this white paper to explore how combining integrated patient access, intake and engagement solutions with your EHR can fill gaps, increase ROI, and enhance its value and effectiveness.
Learning points:
- Ensuring data integrity to prevent denials with intelligent automation
- Expediting financial clearance using accurate cost estimates and payment processing
- Enabling end-to-end prior authorization automation
- Increasing staff performance and accountability with systematic reporting

Yet, amid this surging demand, ASCs experience a myriad of challenges: from staffing shortages to streamlining the patient experience and lags in revenue cycle timelines.
To remain successful and ensure uninterrupted growth, ASCs and other healthcare facilities must improve their patients' financial and clinical journeys.
In this whitepaper, you'll learn:
- The tremendous consequences of payment lag to ASCs
- The top three proven patient payment strategies to optimize RCM
- Patient-centric practices to help ASCs maximize growth via transparency, communication and tech-enabled automations

This white paper offers a collection of short articles and tips sheets on recruiting and retaining nurses and healthcare staff, as well as how to make their work more manageable and gratifying.
Read more to learn about:
Five ways to attract new nurses to the field
Steps for boosting retention while recruiting
Technology that improves staffing efficiency and enables on-demand work

During a panel at Becker’s 7th Annual Health IT + Digital Health + RCM Annual Meeting, five health IT experts discussed the benefits of moving to the cloud and best practices for a seamless transition.
This whitepaper offers a summary of the discussion and includes insights from leader at the following health systems:
University of Maryland Medical System (Silver Spring)
Vanderbilt University Medical Center (Nashville)
Michigan Medicine in (Ann Arbor)
CommonSpirit Health (Chicago)

Healthcare organizations are getting creative to tackle the issue by rolling out flexible staffing initiatives, well-being programs and more. One approach, however, is being overlooked: leveraging the right technology that enables patients to do more, reducing staff burden.
Download this whitepaper from Yosi Health to learn more about the role patients play in mitigating burnout among healthcare workers.
Key learning points:
- 3 key areas/trends patients and consumers are looking for
- How empowering your patients improves health outcomes and financial results
- How engaged patients reduce staff burnout and administrative burden

A survey from CHIME-Cerner found that nearly 40 percent of providers lose at least 10 percent of revenue to leakage, as empowered patients leave to seek innovative care options that better meet their needs.
Health systems need to evaluate their key business levers. This may lead to diversification strategies that enhance primary care service offerings, strengthen patient and physician satisfaction, improve the bottom line and create competitive advantage.
This white paper describes key metrics healthcare leaders need to know and strategies to pursue to diversify revenue and create differentiation.
Insights include:
- Calculating patient panel numbers and customer lifetime value
- Effective strategies for provider diversification and differentiation
- Identify drivers of patient acquisition, retention and loyalty to optimize your portfolio and boost revenue

Supply chain leaders have an urgent need to better understand product availability. To address these challenges, create more resilient supply chains and reduce product shortages, leaders don't need another dashboard. They need actionable data and insights.
A new white paper outlines three key strategies to increase supply chain visibility and decrease product shortages.
Key focus areas include:
- Leveraging the data in your ERP system
- Using a supply chain data model with prospective information
- Streamlining pharmacy operations
- How Renown Health is using data to reduce product shortages

This research report gathers perspectives from 150 healthcare leaders from providers, health plans and government agencies.
Key focus areas include:
- Workforce disruptions and their impact on performance
- Obstacles to workforce progress
- Keys to finding and keeping talent
- Top 5 qualities of a sustainable workforce
- Workforce investment priorities in 2023
- The role of partnerships
- How technology empowers a more human workforce
Leaders today are forced to make decisions without a playbook. Find out how C-suite leaders are responding to today’s workforce threats and are investing in a new path forward.

To achieve call center transformation, health systems need to pivot their focus from marginal improvement of agent efficiency to reducing the number of calls that agents need to manage. A digital front door, powered by intelligent automation, can address the reason for most calls upstream – freeing up staff capacity for higher-value and more meaningful work.
In this whitepaper, you will learn:
- Why the call center must be reimagined to meet today’s needs
- New approaches to optimizing patient access, while eliminating downstream work for staff
- Best practices for transforming the call center into a competitive differentiator that complements a world-class patient experience, including the highest ROI workflows to automate
From regulatory-related constraints to inefficient EHR workflows, a day in the life of a provider looks very different than what many envisioned when deciding to pursue a career in medicine. Additionally, the rate of staff departures and early retirements has put even more pressure on overburdened care teams.
No single solution can solve this complex issue.
In this eMagazine, experts share actionable strategies and industry trends that can help healthcare organizations support the providers.
- How to recognize early signs of burnout
- Three ways AI can reduce providers’ administrative burdens
- Using human-centered design to address burnout
- How a 'platform of health' can dismantle burnout and increase collaboration

These 10 must-read articles collectively examine healthcare's workforce crisis and offer insights into the kind of leadership necessary to nurture high-performing teams. Articles examine:
- Why healthcare employees are increasingly less engaged
- How six health systems are battling labor shortages
- The 15 states affected most, least by the "Great Resignation"

But, 28 percent of health system human resources decision-makers say they are "very unfamiliar" with these networks.
It is time to close the gap of awareness and ensure that health system human resources decision-makers fully understand wrap networks, their costs and their benefits.
In this whitepaper, you will learn:
- The most important attributes of a wrap network
- Today's wrap network gaps and the opportunity for better solutions
- Opinions of out-of-network wraps from health system human resources decision makers' and provider-sponsored heath plan executives.

The crisis is pushing leaders to rethink long-term strategies related to training, education, recruitment and contingency planning. In the near-term, health systems must make immediate adjustments to staffing models and learn how to utilize new technology to better support care teams, especially in the operating room.
This e-book offers an inside look at how Northeast Georgia Medical Center in Gainesville, The Ohio State University Wexner Medical Center in Columbus and Methodist Healthcare System in San Antonio are leveraging an ecosystem of technology to alleviate staff burden and optimize OR performance.

Social determinants of health are responsible for 60 percent of health outcomes — and that's before factors like hospital quality and physician experience come into play, according to the CDC. Even as hospitals invest more in diversity, equity and inclusion initiatives, a new survey reveals patients of color still have different healthcare experiences than their white counterparts.
Healthgrades BIPOC Healthcare Attitudes Survey uncovers what's behind this discrepancy to help hospitals better align DEI initiatives with patients' experiences.
Read the findings to learn:
- What patients actually expect from DEI initiatives
- Five ways to make hospital marketing more inclusive
- How hospital marketers can ensure DEI programming connects underserved populations to the right care

To address these inefficiencies, health systems such as Dignity Health and Novant Health are tapping predictive and prescriptive analytics. Using a new data-driven approach, these organizations are optimizing block and open time to maximize OR access.
Download this case study booklet to learn how more than 265 hospitals from across the country are using this strategy to optimize OR performance and achieve the following results:
- Ability to repurpose up to 20 percent of blocks for greater utilization
- Increase case volume by 10 percent or more without opening additional rooms
- Generate five to 20 times ROI based on contribution margin

Download this eBook to uncover the current state of patient scheduling and communication tools, the technology and processes providers are implementing today and how they are prioritizing for the future.
Key learning points:
- The top challenges providers face with patient scheduling and communications
- Common strategies used to address provider staffing challenges
- Understand the use of technology adoption related to patient engagement, scheduling, and access

Providing these workers with the appropriate resources to manage their weight can improve employee retention and lower healthcare costs for both patients and payers.
In this white paper, you'll learn:
- How obesity impacts quality measures, patient outcomes, employee satisfaction and healthcare costs
- How the pandemic exacerbated healthcare worker mental and physical health issues
- Why employee wellness benefits should include weight management programs that take a comprehensive medical approach that incorporate pharmacology when behavior and lifestyle changes alone aren't enough

For this new white paper on leading during tumultuous times, Becker's Hospital Review spoke with industry leadership experts, who shared best practices about:
- Shifting the organization's focus from agility to resilience and purpose
- Leading like a conductor, not a hero
- Leaning in on people development and potential, whether working with a new team or reinvigorating an established one

- See how Baptist Memorial Health Care has been able to achieve sustainable performance improvements
- How to optimize your growth strategy
- See how Vizient helped Baptist improve their quality of care with $50M in opportunities.

This case study examines how Philadelphia-based Temple Health developed a more flexible workforce management strategy by leveraging technology, advanced strategies, and analytics to increase efficiency, reduce costs, and improve patient and provider experiences — while achieving a 93 percent RN fill rate and reducing contingency spend.
You will learn how to:
- Utilize data and analytics to uncover staff supply and demand across a health system
- Implement strategies to decrease premium pay and agency usage while increasing the flexibility of care staff
- Apply flexible staffing solutions can increase fill rates, and improve staff satisfaction and retention
Please fill out the form to download the whitepaper.

This report covers the three pillars required to make a true shift to a patient-centric care paradigm.
Learning points:
- How a hospital-SNF partnership in Fresno, Calif. reduces readmission rate
- How care navigation at Ascension improves outcomes for its Medicaid population
- The value of 'street medicine' being offered through a partnership between a California hospital and clinic

- Make employees feel valued and listened to
- Create a culture of appreciation
- Go beyond compensation to provide meaningful benefits that resonate
- Focus on increasing workplace flexibility
At this time of profound staffing shortages, learn what industry leaders from around the country are doing to engage and retain their top talent.

But where can a hospital get support in the physician payment space? What options are out there? How can they evaluate them in an efficient manner?
Download this whitepaper to learn:
- The benefits of physician payment automation for hospitals
- Why hospitals are choosing automation to streamline payment processes
- How to determine if you should build an in-house solution or partner with an external expert
- Steps to finding the right solution and how to prepare for implementation

Healthcare leaders must examine how other resource-intensive industries like airline, package delivery, and rideshare services have successfully solved the complex operational challenge of matching supply and demand. The answer? Adopting machine learning, AI, and predictive and prescriptive analytics to drive operational decisions.
Sounds too good to be true? It's not. And many healthcare leaders are already reaping the rewards of AI by achieving hard ROI in challenging times. Fortunately, you can “stand on the shoulders” of your industry peers that have adopted AI:
- In operating room operations and generated $40 million in contribution margin for their health system (which translated into a 10x+ ROI)
- In infusion centers and decreased infusion patient wait times by 30%, and delivered an average increase of $20,000/infusion chair per year in cancer centers
- In inpatient bed patient flow management and achieved an 8% decrease in opportunity days, the equivalent to $8 million in ROI – during the pandemic.

Download this report to discover the key values and the biggest challenges for hospital purchasing leaders. Discover how they are addressing those challenges and where they are making critical investments for the future.

The time has come for a new approach when it comes to the ICU to enable a new framework that helps achieve the strategic needs of the hospital.
SCP Health Vice President of Critical Care Medicine, Erika Gabbard, DNP, RN, CCNS, CCRN-K, discusses strategies to transform critical care medicine programs including:
- Expanded roles of physicians, virtual health, and teleintensivist
- Optimized advanced practice provider scope and responsibility
- Clinical staffing integration
- Modernized nurse training

Amid the pandemic and future crises that will certainly come, hospitals and health systems are looking to stay ahead of challenges and craft robust contingency plans.
Download this report to learn:
- How to build contingency plans to ensure your organization can staff for any kind of healthcare event, no matter the level of urgency.
- Why investing in predictive modeling solutions is now the norm rather than an afterthought.
- How to build and maintain a nurturing environment for staff, even during times of crisis.

However, there are resources available to help health systems reduce staff workload and improve operational efficiency while enhancing the patient experience. Read this report to learn how your healthcare organization can bolster the patient experience amid unavoidable staffing limitations.
Key points:
- Solutions to improving patient experience and addressing staffing shortages
- Benefits of automated digital patient engagement
- Results from using the digital patient engagement tactic

Download this brief report, featuring insights from Ryan Garman, Sterling’s Healthcare and Life Sciences Director, and Amiee Hawkins, Senior Vice President of Enterprise Operations at Cross Country Healthcare, to learn how healthcare organizations can quickly modernize the hiring process with technology-enabled background screening services.
Key learning points:
- An overview of the largest inefficiencies in hiring and onboarding workflows
- How tech-enabled workflows specific to healthcare speed hiring and save HR leaders time and frustration
- How a streamlined hiring process helps attract and retain the right candidates

While it might be evident that flexibility is an incentive to retain employees, some industries can’t offer 100% remote options for their frontline employees. Given the competitive hiring environment, how much should healthcare, retail, and manufacturing be concerned with recruitment and retention, and how do they maintain a healthy workforce?
Gartner Peer Insights and Firstup surveyed IT, HR, and internal communications leaders in the healthcare, retail, and manufacturing industry to see how communication and the digital employee experience impact an organization’s ability to recruit and retain its workforce in the current climate.
Read this report to learn:
- Where industry leaders are spending their recruiting budgets this year
- How they rank the value of employee engagement in helping retain a quality workforce
- What they believe really matters to their workers (hint: it’s not just about the money)

North Carolina-based Cone Health was facing that kind of challenge and turned to Stories, Bamboo Health's care transitions assistant, which delivers relevant patient context within clinical workflows at the point of care.
Here's what Cone Health was able to do after using Stories for a 9-month period:
- Saved 20-30 minutes on average per patient assessment.
- Avoided 106 admissions in a 9-month period, amounting to over $1.2M saved.
- Tracked high-utilizers and acute visit histories both in and out of Cone Health hospitals.
- Reduced readmissions and activated home health providers by re-directing patients unnecessarily in the ED back home.
- Gained insight into recent SNF stays within the last 30 days, allowing them to re-direct patients back to the SNF they recently discharged from.
- Easily connected with patients' care teams through surfaced contact information, facilitating communication with community resources like ACO partners, FQHCs, and PCPs.

Healthcare is at a pivotal moment where the nurse-to-patient ratio gap is widening. To alleviate the stresses of this gap, facilities can create their own tech-enabled staffing pool rather than client-vendor relationships.
Transform the current approach to staffing through partnerships backed by technology, and learn more about end-to-end user experience creating efficiency.

Becker’s Hospital Review recently spoke with two KPMG leaders — Anurag Rai, principal of cyber security services, and Kirby Kleeberg, director of enterprise GRC technology — as well as Vishakha Sant, ServiceNow's global head of healthcare provider industry solutions. These three leaders offered perspectives on how healthcare can advance in reinventing itself to meet patients where they are and how to earn them the trust of their stakeholders — patients, physicians, partners, suppliers and communities.
In this whitepaper you will learn:
- Healthcare's multiple strategic and operational risks that require flexibility
- How to adopt solutions that address issues at scale
- How ESG can improves trust and health outcomes

Here's what you will learn:
- How technological agility can help your organization fight the status quo
- What an ERP is and how it can help you streamline operations
- How one organization cut report generating to less than 5 minutes

The Children's Hospital Coalition collaborates with Phlow and children’s hospitals across the nation to prioritize which essential medicines are of most need, and eventually plans to develop novel pediatric essential medicines. Read this 3-page report to learn how children’s hospitals are currently managing pediatric medicine shortages and their efforts to prevent new ones.
Key learning points:
How children's hospitals are handling current essential medicine shortages and mitigating risks for patients
The action items the Children's Hospital Coalition is working on to ensure a reliable and affordable supply of high-quality medicines
Efforts to prevent future medicine shortages

To accomplish purchased services goals, meaningful change is not achieved one contract at a time. Effective initiatives require a strategic, programmatic approach. Start with where your organization lies on the maturity continuum.
With excerpts from the new book Significant Figures: A Practical Guide to Unprecedented Cost Savings in Purchased Services, you'll have access to:
10 metrics of the Purchased Services Program Maturity Continuum assessment
6 strategic opportunities and actions to strengthen purchased services resiliency
5 traits of successful programs

These flexible workforce programs are essential for health systems to stay competitive. However, building and launching these programs can be a challenge.
This guide explains how to build and launch an internal agency as it walks you through step-by-step design principles, workforce segments for the program, and key factors for launch and sustainability.
Key learnings:
- Define what an internal agency is and the benefits of the program for both front-line nurses and health systems.
- Provide an overview on how health systems can build and launch their own internal travel program from start to finish.
- Identify workforce segments that may be interested in joining an internal travel program.
- Explain the necessary workforce technology capabilities needed to efficiently begin the program.

This whitepaper describes the role intelligent automation plays in solving call center staffing and modernizing consumer engagement.
Download the whitepaper to learn:
Why today’s call center-centric model doesn’t work for consumers
How intelligent automation empowers consumers to register and schedule appointments at their convenience– without phone calls
Why provider organizations like Austin Regional Clinic have chosen to modernize patient experiences with touchless registration

Learning points:
- Explore the benefits of automation and the essential capabilities required for care orchestration
- Review business case results and consider example starting points for automated care coordination workflow in your organization
- Learn how to implement orchestration with confidence

Many stories have emerged about hospitals struggling to transfer patients to appropriate sites of care. In some instances, the consequences have been deadly. These tragedies shed light on the need for a new approach to patient transfers that alleviates staff burden, improves rapid access to acute care and closes care gaps.
In a recent advisory call, industry leaders discussed how healthcare organizations optimize transfer services with the right data and technology to retain patients and galvanize growth.
Key takeaways from the discussion are featured in this whitepaper and include:
- The top transfer center challenges for health systems
- The benefits of implementing a centralized patient transfer center model
- How to use data and technology to retain patients and optimize hospital system growth
- How to make it easier for patients to access the care they need when they need it

Executive health programs can give health systems a strategic competitive advantage and generate a predictable, currently unrealized revenue stream. However, operationalizing these programs can be taxing on existing resources, so having an expert partner in this endeavor can save you time and money opening a new entry point into your system.
Download this white paper to:
- Identify the growing market need behind the development of an executive health program
- Understand how executive wellness services address recent workforce and healthcare landscape changes fueled by the pandemic
- Assess the upside potential to health systems, community businesses and C-suite employees by offering a corporate wellness program
- Determine how to evaluate the best partner to help you implement an executive health service line

while long-term shortages are expected to continue
because of an aging workforce and planned retirements.
Despite their challenges, many healthcare leaders remain optimistic about attracting talent in the future. Huron sponsored an advisory call in which a panel of executives shared their organizations’ strategies for winning the war for healthcare talent.
This whitepaper details 6 takeaways from that call. Download to learn:
- How hospitals should be redesigning human resources strategies
- How thinking about retention is changing
- How to funnel new healthcare talent into the pipeline

Using Notable’s intelligent automation platform, Fort HealthCare is digitizing the front end of the patient experience and all areas where staff traditionally engage in manual processes. This includes prior authorizations, registration, and pre-visit planning.
Download the case study to learn how Fort HealthCare:
- Digitized the front- and back-end registration process, automating 91% of prior authorizations
- Deployed an automated prior authorizations workflow in just 4 weeks
- Reduced cancellations by more than 5%

This case study outlines how UCHealth cut training time by 56 percent and saved millions of dollars in the process by harnessing the power of personalized learning.
In this case study, you'll learn how to:
- Significantly reduce EHR training time
- Improve EHR proficiency
- Increase clinician learning satisfaction
- Gain a measurable training ROI

For all these reasons and more, it is critical that healthcare organizations tackle no-shows head-on. This whitepaper outlines how positive, consistent patient engagement can minimize no-shows and offers concrete steps that healthcare organizations can take to ensure patients feel prepared and informed about their upcoming visit.
Read this whitepaper to learn about:
- The 7 most common reasons that patients fail to keep their appointments, and how to address them
- Messaging and outreach strategies for reducing no-shows
- How to engage patients in their care without creating more work for staff

This whitepaper describes how addressing the dual mandate—improving the experience of both healthcare consumers and healthcare workers—through automation can help leaders finally make serious progress toward the Triple Aim.
Download the whitepaper to learn:
- The market forces driving the healthcare industry towards automation
- How automation is the antidote to manual workflows, vastly improving engagement for staff and patients
- The journey of one midwestern hospital that is saving 24 minutes of staff time per patient visit with a 91% patient satisfaction rate through automated patient intake

Beyond recruiting, retention is even more difficult with the increase in turnover and employee burnout. Healthcare workers are grappling with high levels of fear, fatigue and stress amid the pandemic, with widespread burnout fueling turnover as employees seek positions with fewer stressors.
By building a community and embracing a more human-centered approach, your organization can recruit and retain top talent, and put your people first. Download this guide for 10 tips on recruiting and hiring employees, addressing staff burnout and retaining top talent in your healthcare organization, including:
- How to give your staff the opportunity to be part of something bigger than themselves when working for your organization.
- The value of frequent and transparent communication in helping staff feel valued, protecting them from anxiety and burnout.
- Tips for how to equip managers to be there when employees need to talk.
- The importance of having one platform or app where employees can access vital information and connect with other employees.

Take the opportunity to improve your understanding of your patients' experience navigating the entire system—from before they make an appointment, through the care they receive, to the final payment.
This guide provides valuable insight by allowing you to walk in your patients’ shoes. It also identifies places where the patient experience can be improved through better connections, digital interactions and empathy.
Download the guide to learn:
- Why investing in the patient experience often is more powerful than traditional marketing
- Ways to help busy patients feel in control and more engaged with their healthcare
- How a few simple actions in the early phase of a patient’s experience will ensure better engagement from beginning to end

The findings reveal the importance and implications of consumer trust in health.
Download the report to gain an understanding of today's health landscape and:
- How consumer behaviors have changed since 2019
- What can increase trust in the healthcare and life sciences sector
- Variations in consumer trust by generation and sector
- What trusted health organizations do differently

Download this whitepaper to learn:
- Strategies to navigate healthcare staffing challenges in the pandemic
- Methods to craft community and culture in your team
- How to establish a foundation of success for the future nursing workforce

During the Becker's Hospital Review 9th Annual CEO + CFO Roundtable, experts from ServiceNow and senior healthcare leaders discussed how strategies like workforce automation can transform both the patient and clinician experience, and how to make the process simple.
Download this short report for opportunities to streamline and automate workflows, and other key session takeaways.

Physicians have been overburdened by clinical documentation for years. Many have had to rely on the support of medical scribes to accurately document care. However, recent surveys show that 44 percent of medical scribes have no prior experience, and only 22 percent have any form of certification. Scribes also aren't scalable and have high turnover rates, which lead to continuous training for accurate notes.
Emerging technology powered by artificial intelligence can support efficient clinical documentation that supports a better experience for providers and patients.
Download and discover how clinical documentation that writes itself can:
- Improve physician-patient interactions
- Decouple scribes from physicians' and enable scale across the organization with no changes to existing workflows.
- Enhance provider efficiency and satisfaction and improve financial outcomes.

During a workshop at Becker's Hospital Review 9th Annual CEO + CFO roundtable, three experts provided an overview of relevant portions of the regulation and discussed how providers can best prepare to meet coming challenges.
This white paper offers:
- A look at the rule's patient protections
- An overview of how implementation of the rule will challenge physicians
- A breakdown of how physicians and hospitals can partner to mitigate challenges associated with the legislation

During an AMA-led session at Becker's 9th Annual CEO + CFO Roundtable in November, health system leaders from across the country shared their experiences addressing physician well-being and staff turnover amid the pandemic. This whitepaper offers a summary of the discussion, along with a look at emerging research on burnout from AMA.
In this whitepaper, you will learn:
- The current state of burnout and its effect on retention
- The business case for investing in well-being
- How to address the drivers of burnout and improve worker well-being
- Why hospitals should strive for resilient organizations, not just resilient employees

Like many providers, the registration process at ARC was highly manual. Staff had to manage multiple, often duplicative work queues for each patient at each stage of the process.
Using Notable's intelligent automation platform, ARC is powering a touchless patient registration experience, a critical step in patient financial clearance within the revenue cycle. This consists of automating various pre-visit workflows like new patient pre-visit registration, demographic verification, payer/plan matching, and real-time eligibility.
Download the case study to learn how ARC is leveraging Notable to drive:
- 78 percent touchless registrations
- 74 percent digital conversion rates
- 94 percent patient satisfaction rating
- 83 percent reduction in eligibility- and registration-related denials

Healthcare cost reduction is more important than ever, yet legacy accounts payable processes hold providers back, eating up time and inflating costs. Streamlining procure-to-pay in the healthcare industry is key to ensuring that organizations have what they need in order to offer the best, most effective patient care.
However, data from Premier Inc., an industry-leading healthcare improvement company, indicates that most invoices in this sector are still paper-based, with the vast majority of them still paid by paper check. Aside from the expense of doing things this way, manual processes slow down the healthcare P2P workflow and create opportunity for error.
Remitra™, a division of Premier Inc. partnered with the Institute of Finance Management (IOFM) to explore ways in which technology-enabled ordering, invoice processing and payment can help healthcare providers and suppliers do their jobs better. The whitepaper, “Ready, Set, Automate: 5 Ways Healthcare Organizations Can Gain Efficiencies, Reduce Costs with Digitized AP Technology,” explores the benefits of using data to sync up buyers and sellers in order to streamline the supply chain and reduce errors, while minimizing cost and inefficiency.

"The most exciting part of the study is that we know our patients are having better outcomes," Dr. Schmidt said. "We know that our system is going to remain sustainable because we've been able to provide decreased cost of care, while at the same time improving our patient outcomes.”
In this brief report, you can dive into Dr. Schmidt's data and find:
- Steps to understand the influence of order set optimization and mortality, length of stay and variable direct costs across the health system
- Tools used to perform an evidence-based gap analysis on existing EHR order sets
- Benefits Cone Health and its patients experienced because of order set optimization
- What is the distribution and influence of the health plans that provide coverage to members across our network?

Providers rarely have the resources to see these types of broader patterns and opportunities. Oftentimes, claims data external to a provider network can help fill in the gaps to allow for more informed planning and decision support that can provide a much-needed edge in the healthcare marketplace.
In this case study, providers can learn from Lehigh Valley Health Network and how they addressed critical planning challenges including:
- Where are patient referrals coming from?
- What physicians/physician groups should we engage with for network optimization?
- Are there new communities we aren’t serving that provide opportunities for expansion?
- What is the distribution and influence of the health plans that provide coverage to members across our network?

This whitepaper outlines 10 strategies to engage staff and boost retention, while also seizing this opportunity to improve efficiency, automate manual tasks and empower patients to take a more active role in their healthcare experience.
Read this whitepaper to learn:
- Easy-to-implement tips to reduce turnover and engage staff
- Why giving patients the opportunity to take on tasks such as registration and appointment scheduling improves their experience
- How technology can help you weather this staffing crisis and reduce the number of employees you need to add to your organization

Bullet points :
- The top customer operations challenges impacting healthcare organizations
- How improvements in customer operations can drive overall business performance
- What are the key activities and technology enablers being considered?

This e-book is based on the 5th Annual Telehealth Benchmark Survey for Hospitals and Health Systems — conducted by Becker's Hospital Review in partnership with Teladoc Health. More than 150 healthcare leaders responded to the survey. Nearly half of respondents were C-suite executives.
The e-book contains analysis of five crucial telehealth insights identified by the survey:
- Insight 1: Telehealth is a major priority for healthcare executives
- Insight 2: Telehealth goals are consistent across health systems
- Insight 3: Virtual and in-person care are not mutually exclusive
- Insight 4: Engagement and alignment are essential to telehealth success
- Insight 5: Barriers to telehealth advancement remain

In this white paper, you will learn:
- Why not treating obesity carries health and financial risks for individuals, health systems, employers and payers, and society at large.
- Why healthcare providers must treat the disease of obesity using a multidisciplinary approach that includes diet, physical activity, behavioral modifications and pharmacotherapy.
- How tech-enabled services can help overcome vast provider shortages and lack of training to increase access to medical obesity treatment.

This white paper—a culmination of data from over 1,800 patients, physicians and healthcare leaders in 13 countries—focuses on the challenges that arise within the earliest stages of the vascular patient journey.
In this whitepaper, you will learn about:
- Key challenges in symptom recognition and diagnosis that impact patient and physician experience;
- Health equity influence on access to care, emotional impact and physician-patient relationships;
- Expectations your healthcare leader peers have related to adoption of technologies that can alleviate some of these core issues.
It’s a critical time for shaping how healthcare will be delivered and received in future years, and understanding drivers of patient experience is essential. Download the white paper to learn more about these issues and potential solutions related to coronary artery disease (CAD) and peripheral artery disease (PAD) patients around the world.

Find answers to important questions including:
- What are the four factors of digital engagement?
- What is the impact of digital inequity on health outcomes?
- What are the steps for a holistic approach to digital engagement?
- How can executives adopt an innovator's mindset to digital health?

To compete on a level with digital disruptors, healthcare organizations must provide the same connected, frictionless experiences. This requires an overhaul in the standard approach to customer engagement, but it doesn't mean starting from scratch. For HCOs, that means becoming more than just outcome providers. It requires these organizations to become intelligent experience builders too.
Download this short e-book to learn how Pega's customer engagement platform enables HCOs to quickly adopt digital engagement improvements specific to their goals. Key learning points:
- Why many tech transformations fail and how to prevent that
- The key benefits of a customer engagement platform
- Strategies for seamless implementation

The consumerization of healthcare is a paradigm shift—and leading healthcare provider organizations have to shift with it. Having complete and trusted patient data is foundational to your success in this consumer-directed world.

During the worst of the initial economic shutdown between mid-March through mid-June, telehealth visits comprised about 30 percent of total outpatient visits. As the pandemic’s grip loosens, providers must continue to embrace new ways of reaching patients as a large and growing number of consumers expect telehealth to be an option in the future.
The new care paradigm is patient engagement, which encompasses virtual visits, patient education, medication adherence and the ability to monitor and track patients through fitness devices and medical mobile apps that fully involve patients in their care.
Patients who are more engaged in their health enjoy better outcomes and incur lower costs, which benefits both patients and providers. This whitepaper will explore:
- The use of telehealth during the pandemic
- The basics and benefits of patient engagement
- Pros and cons of telehealth when it comes to patient engagement
- How mobile apps propel patient engagement strategies and enhance the patient experience

Download this whitepaper and discover:
- Best practices in loyalty from Mayo Clinic, One Medical, and Baycare that can be adopted by providers
- How loyalty strategy can impact key metrics such as HEDIS, NPS, and star ratings
- A new model of connected membership that works to engage consumers before, during, and after care episodes

Growing call volumes and worsening staffing shortages have led to call centers that are overworked and unable to meet patient expectations. As a result, today’s leading health systems are designing “digital front doors” that can offload call volume by replacing manual calls with automated digital services.
Leading health systems are leveraging AI, robotic process automation, and digital patient engagement to automate many of the workflows that previously ran through the call center. By streamlining cumbersome, manual processes with AI and robotic process automation, teams are increasing their capacity and better serving their patients, while reducing the overall cost of care.
Read this whitepaper to learn best practices from industry leaders on automating common call center workflows with a digital front door, including triage and scheduling, appointment reminders, registration, prior authorization, referral management and payment collection.
Readers will learn:
- Best practices for orchestrating cutting-edge automation, patient engagement, and AI technologies to improve call center efficiency.
- Why digital point solutions for scheduling and appointment reminders require back-end automation to eliminate call center workflows.
- How to diagnose the root causes underpinning call center capacity constraints in your organization.
- How to determine which call center workflows are best suited for automation, and which are best left for staff to manage.
- How Notable partnered with a leading healthcare provider to eliminate over 60% of their call volume through intelligent automation.

In this eBook, we review hospital discharge processes and discuss the challenges. We also outline how intelligent automation is being used in hospitals and health systems of all sizes to achieve three simple steps for consistently managing patient discharges:
- Identify discharges early
- Develop both system- and unit-level actions
- Assign and manage specific items to take action

This white paper examines how eight healthcare executives are adjusting to meet the challenge and drive down labor costs. Through a combination of monitoring operations, leaning into digital care accessibility and leveraging partnerships to develop a robust digital infrastructure, leaders are not just easing labor strains, but creating more efficient workflows.
Learn how executives are combating rising labor costs by:
- Adjusting to the new norm of outsourcing administrative work.
- Investing in digital transformation and workflow automation.
- Optimizing digital access to care.

To better understand the current state of cardiac care and how health systems can best respond to growing patient consumerism and value-based challenges, Becker’s Hospital Review and Siemens Healthineers conducted a survey of more than 100 cardiologists and health system leaders. Respondents identified key challenges faced by health system cardiology service lines and the means by which they are working to solve them.
This special report shares these industry leaders’ insights and perspectives to identify potential solutions that can help transform cardiac care delivery to benefit patients and health systems.

Recently Becker's Hospital Review asked three healthcare industry experts to share insights from their M&A-related experience:
- Joe Gage, Chief Human Resources Officer, Cincinnati-based Bon Secours Mercy Health
- J. Lankford Wade, CFO, Berkley Heights, N.J.-based Summit Health
- Shana Graff, MHA, Value Manager for Healthcare, Workday
This white paper contains an overview of common M&A challenges and 10 best practices for overcoming these challenges.

To shine a light on how stakeholders across the industry are driving the evolution of virtual care, Amwell teamed up with HIMSS Analytics to ask senior executives at hospitals, health systems, and health plans across the country about their post-pandemic strategy and their planned investments in telehealth. To keep them honest, we also surveyed front-line clinicians caring for patients in a broad range of practice settings.
The findings suggest that telehealth is entering a critical new phase. As healthcare leaders take stock of the telehealth experience of the past year, the focus is shifting from pandemic-fueled expediency to a “smart-growth” mindset that prioritizes consolidation, integration and purposeful central planning. Based on their insights, we’ve identified three key themes that will define this new phase and the future of virtual care.

Growth in patient volume will continue to rise as the nation's population ages and chronic disease rates increase. As a result, hospitals need to be more efficient with their resources than ever before. This means capacity management must become one of the most important areas for hospitals to focus on.
In this whitepaper, you'll learn:- Why current methods of allocating and managing capacity are simply inadequate to meet the challenge's growing complexity
- What mathematical concepts underlie successful capacity management, and what healthcare can learn from the industries that have unlocked them
- How health systems are using tools to solve their mathematical challenges and achieve stunning improvements in their capacity

Learn how they’re achieving:
- More efficient charge capture
- Automated patient attribution
- Streamlined communication among providers and between providers, coders and billers
- Greater productivity while reducing physicians’ burden

Halting HAPIs in American hospitals demands attention. Recent reports from the Agency for Healthcare Research and Quality indicate that the incidence of many hospital-acquired conditions is falling. However, pressure injuries rates continue to rise despite being a top priority for health systems.
A recent survey conducted by Frost and Sullivan was designed to better understand the persistent rise of pressure injuries and examine potential solutions to the problem.
This report is based on those survey findings and in-depth interviews with 20 healthcare professionals.

In this whitepaper, you’ll learn:
- How workflow improvements affect everything from interoperability initiatives to the patient experience
- Why healthcare solutions designed with the future in mind ensure that caregivers remain prepared to address evolving priorities
- Why it's so crucial that healthcare equipment is versatile enough to be used in various applications

- How an ASC’s exceptional experience with standardized regional anesthesia protocols for total joint and breast procedures prompted its affiliated hospital to move many complex procedures across multiple service lines to the outpatient environment, with excellent quality, efficiency, and satisfaction results for patients, physicians, and payers.
- How providing long-acting nerve blocks with minimal or no opiates provides effective pain management with fewer opioid-related perioperative complications, allowing surgical patients to go home the same day without pain, and eliminating costs associated with inpatient length of stay that average $2,500 per patient day.
- How leadership and expertise that enabled one ASC to move to a cutting edge regional anesthesia program has been transformative, by expanding its capabilities, expediting operating room throughput, and achieving patient and surgeon satisfaction scores consistently in the high 90s.

This whitepaper explains how this vantage point yields crucial insights into much-needed changes in health care and issues a call for transformation.
In this whitepaper, you’ll learn:
- What an analysis of more than a million patient encounters reveals about the post-discharge “Care Gap”
- Opportunities to leverage and impact the emergency department’s unique view of the health care system
- Ways to improve patient outcomes and satisfaction while increasing health care value for key populations

Managing the online reputation for a multi-location healthcare organization is a tall task, so instating an effective online reputation program is critical. Doing so will help build brand awareness, grow revenue by driving more customers and increase an organization’s ability to compete online. Read this ebook to learn how to:
- Build an online reputation program that works
- Get started with Google Reviews
- Optimize your review request program

Get insight from experts at The Advisory Board, and learn:
- How providers should be thinking about RPA and AI
- 4 key pivots health care leaders need to make to reach their strategic goals
- Strategies from The Advisory Board's latest research on getting the most out of your organization's investments in intelligent automation

Many turn to data for answers, but overly simplistic data frequently drives organizations in the wrong direction. Instead, methods are needed to help providers understand what's working, what's not and what should happen next. Communication based on an OmniChannel strategy ensures that patient engagement is efficient and effective, whether it's for pre-service preparation, payments or everything in between.
In this whitepaper, you'll learn new strategies for healthcare organizations to:
- Apply intelligence to every type of patient interaction
- Reduce waste, save money and increase engagement
- Seamlessly integrate data science, machine learning and customer engagement to drive better financial results and increased patient loyalty
- Unify the patient experience for happier, more engaged patients every step of the way

To learn about these key trends and projections for recovery and growth over the next decade, as well as how to rework your strategies for success, read this executive summary. The 10-year forecast includes trend analysis and projections for:
- Site-of-care shifts
- Surgical shifts
- Emergency department volumes
- Virtual care

Learning Points:
- The inherent vulnerability of the critical care patient
- The burden of hospital-acquired infections and the benefits of reducing their incidence
- The role of ECG cables and wires

- Strategies to mitigate clinicians' administrative burden in the ED while reducing costs and improving the patient experience.
- Use cases from forward thinking organizations leveraging scribes, hospitalists and telehealth to ease the overload on ED clinicians.
- How to support clinician well-being in times of crisis.

To effectively do this, they need access to trusted information and educational resources to deliver patient-centric care and to engage members in managing their own care.
When all involved are using the same knowledge tools for clinical, drug reference and patient education, you can improve efficiency, increase consumer satisfaction, and achieve the best possible health outcomes. Download this whitepaper to:
- Understand the latest star ratings and their impact on health insurers, PBMs and retail pharmacies
- Learn how accurate, trusted knowledge sources can be an effective strategy in achieving top ratings
- Understand the value of a trusted knowledge partner in this era of misinformation

Equitable care requires innovative solutions.
Download this whitepaper, titled Why Virtual Care is Key to Overcoming Social Determinants, to discover
- How social determinants of health impact chronic conditions
- How virtual care can be an effective and innovative solution
- Why treating both mental and physical care together delivers better outcomes

That's where Emergency Psychiatric Intervention, or EPI, comes in. It's an approach and toolkit designed by Vituity emergency medicine and acute psychiatry physicians that aims to elevate the standard of care for emergency behavioral health patients. EPI brings together front-line physicians and clinical support staff with existing ED teams to optimize workflows and increase staff engagement.
In this whitepaper, you'll learn:
- A deeper look into what EPI is and how it operates
- How EPI helps hospitals improve clinical quality and profitability while strengthening community trust, as well as the other benefits
- Case studies of EPI in caption at two health systems of care.

In this eBook, learn to streamline your OR scheduling process, optimally fill open time and increase surgeon and staff satisfaction. Additionally, explore how to address:
1. Block time left unfilled
2. Missed connections between clinics and/or facilities
3. Reallocating surgeon' block time in a more surgeon-centric manner

Those adopting new patient engagement technologies report a better experience for both patients and staff members.
In this whitepaper you’ll learn more about:
- The hidden costs of manual engagement
- How digital solutions address health system needs
- Improving patient outcomes and resource efficiencies

Sample findings:
- 73 percent of consumers want to schedule their own appointments online
- Improving the patient experience is a top priority for 93 percent of providers
- More than 50 percent of providers find it difficult to keep track of changing pre-authorization requirements
- Just 14 percent of consumers felt their final healthcare cost differed significantly from estimates — down from more than 50 percent in the first survey
These and many other topics were addressed in the survey, making this white paper a useful resource for strategy and planning beyond the pandemic.

In this guide, you’ll learn how to:
- Embrace the power of omnichannel communication
- Cultivate a culture of authenticity
- Personalize the end-to-end journey
- Capture timely feedback and take action

This guide outlines how healthcare organizations can implement equitable and inclusive sourcing practices to support their diversity commitments.
Key insights:
- The definition of a diverse supplier
- The importance of equitable and inclusive sourcing
- Roadblocks to implementing more equitable and inclusive sourcing practices
- Sourcing strategies to increase diverse supplier spend

While this data contains a wealth of patient insights, most healthcare organizations lack the resources, technology and time required to leverage its true value.
In this white paper we share three steps on the road to semantic interoperability that support optimal performance in value-based arrangements.
Download now to learn:
- Why collecting, integrating, normalizing and interpreting data from across care interactions, devices, apps and settings is critical within a value-based care environment
- The role of natural language processing and machine learning in effectively managing population health
- Three strategies for creating a "Rosetta Stone" of health language that will equip you to improve care for entire patient populations

Download this E-book to access 11 must-read articles on the patient affordability crisis and how it’s affecting healthcare. You’ll gain insight on:
- How healthcare’s affordability crisis is negatively influencing patient decisions
- How providers are handling patients’ inability to pay for care
- How technology can make it easier for patients to understand and meet their medical expenses

Amid acquisitions and expansions, health system leaders must work to ensure staff are strategically unified and the right technology systems are in place to support high-quality care. Without this integration, organizations are vulnerable to unnecessary operational complexities and care variation.
This white paper offers insights into the integration journeys at three health systems and is derived from interviews with leaders from Roseville, Calif.-based Adventist Health; Phoenix-based Banner Health; and Springfield, Mo.-based CoxHealth.

Utilizing Vizient's extensive pharmacy analytics, the Vizient Pharmacy Outlook is an industry-leading report providing drug price inflation projections over the next 18 months across multiple classes of trade and therapeutic areas. Health system and hospital financial and pharmacy leaders rely on this report to budget smarter and prepare for future trends that impact their delivery of care.
Key insights include:
- Changes in biosimilars for acute care
- Shifts in non-acute care to outpatient and telemedicine settings
- Impressions of the FDA Accelerated Approval program
- Specialty drugs, changes in disease states, and the pipeline

This whitepaper walks through 7 proven use cases for improving population health program impact by automating manual and repetitive workflows, and outlines best practices for automating population health workflows.
Download our whitepaper to learn:
- How intelligent automation can eliminate repetitive tasks for clinicians, and enable them to practice at top of license
- Why common approaches to population health technology, such as implementing digital nudges for clinicians, often fail to realize expected impact
- How to avoid increasing administrative burden on clinicians through the introduction of new population health technologies
- How to automate the identification and engagement of patients with open care gaps
- Best practices for optimizing HCC coding workflows to ensure appropriate value-based reimbursement

At Medical Center Hospital, disorganized vendor access created three significant problems:
1. Their IT staff had to be heavily involved.
2. There was no common method of tracking the remote access sessions.
3. It was impossible to implement a uniform security policy, making HIPAA compliance difficult to determine.
Download this case study to learn how the hospital was able to implement a uniform security policy and ensure HIPAA compliance by:
- Strictly defining system access for each vendor.
- Taking the load off IT staff in administering support connections.
- Ensuring network security and compliance.

Download the summary report to learn more about these insights and discover organizational well-being resources available through the AMA Health System Program.
Key insights include:
- What insights have we gained from healthcare workers' experience with COVID-19?
- Do care teams feel valued by their organization?
- How has COVID-19 affected the team's sense of meaning and purpose?
- What organizational resources are available to support physician well-being?

From how to effectively use tracking technology to ensuring the supply chain is clinically integrated to how sustainability can reduce costs, there are key trends of which supply chain leaders must be aware.
Download this whitepaper to learn how to:
- Reduce supply chain costs
- Prepare for the next healthcare crisis
- Track the supply chain more effectively

Scattered, often unavailable, information creates frustrating workflows and wastes valuable time that could better be spent on high-level tasks and interactions. This can further lead to care team frustration and poor patient outcomes.
Patient-considerate and patient-facing technology can help fill in missing data at various points in the patient journey, saving care teams time and giving patients a voice in their healthcare journey.
In this report, CoverMyMeds explores:
- The impact of information gaps on quality of care
- The role interoperable technology can play in providing a single source of care team data
- How integration and automation could have a positive influence on reducing care team burnout

These eight articles are must-reads for supply chain leaders who want to stay ahead of the curve and position their ASC for success. They contain insights on topics such as improving surgery center efficiency, addressing burnout and long-term capital planning.

3M and Becker's Hospital Review recently surveyed dozens of hospital and health system executives about the ongoing obstacles in the way of those mission critical goals, and the technology they're relying on to make progress.
In this whitepaper, you'll learn:
- The value of speech recognition technologies in enhancing EHR documentation workflow
- The tech-driven solutions organizations are using to address denials and enhance clinical care documentation
- What solutions hospitals and health systems are using to accelerate the shift to value-based care

Ochsner Health adopted a centralized patient monitoring model, which allowed the New Orleans-based health system to have eight or nine technicians monitoring 90 to 108 patients instead of using individual sitters for each patient. The model delivered a clear return on investment for the system, while also supporting revenue-generating opportunities.
In this whitepaper, you’ll learn how centralized monitoring systems like the one used at Ochsner Health can:
- Improve safety and support for patients and staff
- Result in a 90 percent cost reduction
- Potentially integrate with other centralized healthcare services

To better leverage the new healthcare ecosystem, healthcare leaders must take on four distinct imperatives. To do so, they should consider outside partners who can deliver more: data, access and improved patient experience.
In this whitepaper, you will gain strategies for:
- Embracing new technologies
- Building a customer-centric focus that emphasizes access
- Adopting non-traditional partners
- Improving access, quality and affordability

For many healthcare executives, cost concerns have made them hesitant to invest in surgical robots. However, when built right, a robotic surgery service line can enhance operational efficiencies and reduce the total cost to treat.
This ebook explores the value of robotic surgery in a value-based market, as well as the key considerations needed to shape a viable program.
Key learning points:
- Financial and operational benefits of robotic surgery
- 4 steps health systems can take for robotics to enhance economic value
- Real-world insight on how health systems decreased costs after transitioning to robotics

A supplier payment platform can help providers understand what's working well in their supply management processes and what could use improvement. While healthcare and hospitals systems have historically lagged in adopting automation for invoices and payment processing, those who have are able to strengthen their supply network and use their internal resources smarter.
In this white paper, learn how your organization can:
- Use rebates and bargaining power to work with large medical suppliers
- Customize your supply procurement approach
- Implement an automated accounts payable platform

Health systems are striving to enhance the quality of patient experiences and outcomes, while simultaneously expanding and growing the business aspects of healthcare delivery. This white paper offers an overview of recent industry challenges and insights into new approaches to strategic planning.
Key insights include:
- The role of specialty medications in the modern care continuum.
- The industry pressures affecting all sites of care.
- Four questions all health system leaders should ask when developing a successful growth strategy.

Earlier this spring, Becker’s Hospital Review and Cardinal Health convened a group of health system leaders to discuss how their organizations responded to the COVID-19 pandemic and how they’re adapting their strategies moving forward. This whitepaper summarizes insights from that discussion.

Key learnings:
- How to address patient experience in a COVID-19 world
- The benefits of improved patient experience
- How TeamHealth clinicians are using innovative ways to connect with patients

This whitepaper will cover:
- Impact of broken referral management on patients, such as 33% of patients not following through on a referral
- Current provider data and infrastructure barriers to referral management
- How a patient-first approach to provider data can improve patient care journeys

Health systems’ chief digital officers, chief medical officers, chief quality officers, chief innovation officers and educational deans must reevaluate their digital resources and encourage the use of equitable evidence in medical education and within the exam room. And these actions are needed urgently.
This whitepaper offers a digital solution to the following three problems:
- Most clinical knowledge resources are not equitable.
- Artificial intelligence and machine learning algorithms are not trained on representative data.
- Digital medical education tools and training lectures lack equity in representation of skin of color.

These eight articles are must-reads for healthcare leaders who want to pursue successful innovation programs. They contain insights on topics such as interoperability, artificial intelligence, how to build resilient clinical teams and how to prepare for future health crises.


Download this eBook to learn:
- The three pillars of A/R optimization—and your biggest barriers to progress
- The hallmarks of a high-performing A/R operation
- Real results leading providers have achieved

Seventy percent of hospital executives said they had plans to expand price transparency, but only 25 percent said they strongly agreed that their staff was well-prepared to have financial conversations with patients, according to a survey conducted in early 2021 by CareCredit and Becker’s. This incongruence between priority and ability sheds light on a crucial area hospitals need to improve upon to deliver a consumer-centric, transparent experience to patients.


When their experience in traditional, volume-based medicine falls short, they seek care elsewhere, often outside your hospital system. This is why investigating an innovative primary care model is a valuable strategy to address increasingly savvy patient needs in order to retain current customers and attract new ones.

Learning points:
- 10 best practices to solve last-mile vaccine management
- 5 steps to a safer workplace for everyone
- How 2.5 million high-risk citizens were vaccinated in Scotland


In January, Molnlycke assembled an advisory board of value analysis leaders to discuss how suppliers can achieve more meaningful relationships with healthcare organizations. This e-book provides an overview of the main themes that emerged from the discussion.
Read this whitepaper to learn:
How healthcare organizations can form meaningful relationships with suppliers
The qualities of a strong value-based partnership
The evidence value analysis committees seek to inform their decision-making process

Clinical knowledge is inherently dynamic, but the way healthcare leaders attain this knowledge can sometimes seem static. For hospital leaders, having the ability to track search data within reference tools to understand what clinical information their clinicians need and in what form they need it is crucial both during and after a crisis.
This research guide includes:
- A timeline of COVID-19 research trends
- A breakdown of how research data can inform continuous care improvement strategies


Read this white paper to learn:
- How providers decide when to refer patients and to whom
- Referral senders' goals and the challenges they face when communicating with referral receivers
- Opportunities for technology-based referral solutions that support all providers and eliminate obstacles to high-quality care


In this report you will learn:
- Why a cross-disciplinary team is critical to success
- The importance of establishing and driving a medical equipment standards program
- How the right tools can enhance collaboration and optimize equipment purchasing decisions

This e-book highlights innovations and success factors across the consumer health experience, including:
- Shopping for benefits
- Staying well
- Choosing care
- Receiving care
- Managing conditions
- Saving and paying for care

This whitepaper outlines seven staffing strategies that value, protect and optimize nurses.
- Key learning points:
- How to make staffing and scheduling a collaborative process
- Streamline the open shift management process
- Make it easy to access and act upon critical staffing information


Read this whitepaper to learn:
- How to impact patient reviews to improve your average star rating
- What best practices to implement to increase your number of patient reviews
- Why reviews influence search results and patient growth
- What to expect in future online presence trends for healthcare


Download the ServiceNow whitepaper to learn:
- How the COVID-19 pandemic has accelerated digital strategy development
- Missed opportunities for digital employee engagement in healthcare
- Methods and best practices for implementing new tech solutions


Fill out the form to get the guide, "Cut to the Chase: The Simplified Blueprint for Payer CX Success," and read about:
- The 3 strategies for creating the most impactful consumer experiences
- The trouble with off-the-shelf customer relationship management systems
- The one-stop-shop software solution for accelerating speed-to-market and speed-to-value

Key Takeaways:
- Health systems can support medical device availability through optimized preventative maintenance schedules and standardized workflows.
- Dedicated monitoring and remediation of OEM-reported FDA alerts and recalls can minimize the potential impact on device availability and patient safety.
- Patient safety should be a key consideration throughout a health system's capital planning process

Read this eGuide to find out:
- How lack of capacity optimization affects providers, patients, and revenue.
- How provider scheduling, room scheduling, and workforce analytics solutions help organizations solve the capacity problem.
- Strategies you can implement to address capacity challenges.

Survey finding themes explored in the report:
- Key aspects of the care experience that have always been central to the patient satisfaction
- Patients are more attuned to safety
- Patients are using telehealth services in record numbers
- COVID-19 patients are straining hospital capacity and reporting poorer experiences

Download this white paper to learn:
- What an integrated hybrid care delivery model is and how it differs from just adding telehealth care options
- The risks of not offering a variety of care-delivery options—to both patients and system revenues
- 4 best practices to get you started

In this whitepaper, you’ll learn:
- The kind of personalized experience members expect from payers
- How cloud-based communication technologies give payers better security and efficiency
- How analytics from digital member engagement platforms can optimize payer performance
- How digital engagement tools generate higher employee satisfaction and retention

In this report you will learn:
- What are the different technology approaches to managing imaging across the enterprise?
- How can converging imaging workflow and infrastructure support my business growth initiatives?
- What are the key financial and clinical care metrics that can be used to measure the benefits of enterprise imaging?
- How do I build an effective governance team to oversee my enterprise imaging project?

In this whitepaper, you’ll learn:
- Ways long-term strategic partnerships can improve health systems
- Practical considerations for selecting strategic partners
- Case studies about innovation approaches and successful outcomes

The E-book shares key templates on:
- Frequently asked questions
- Dispelling common myths
- The vaccine’s safety and efficacy
- Vaccine appointment reminder check-list

In this ebook, we'll take a closer look at six significant facets of scheduling for 2021 to paint a clearer picture of what's in store for smart scheduling and healthcare operation. Trends include:
- Personalization
- Instability and agility
- Hybrid care
- And more!

Download this whitepaper to learn:
- 9 critical marketing metrics for healthcare
- How to find each metric (with examples)
- A clear action plan to improve in each area

This white paper highlights findings and an analysis of the 2023 Becker's-NextGen leadership survey, which gathered perspectives on current VBC implementation challenges facing ASCs and specialty providers. You'll find leaders' top obstacles to embracing VBC, as well as expert recommendations for addressing them.
Download to access insights including:
Level of VBC adoption among surveyed organizations + the support they need
ASC and specialty leaders' priorities in shifting away from fee-for-service
Key areas where technology can help to address obstacles to VBC

There are five key characteristics every good ASC billing company has. This white paper examines each of these differentiators, including how they're defined, how they benefit surgery centers, and what ASCs should look for to ensure the billing partner they choose is right for them.
Key insights include:
- The importance of achieving a true partnership with your billing partner
- What it means to provide best-in-class security and next-generation analytics
- How a billing company's team structure and expertise are critical to success

Often a big offer comes unsolicited, but is it a fair offer and will private equity partnership be a good fit? The lure of private equity money can be enticing but what are the risks and challenges? What help do you need to navigate this unfamiliar territory?
A new white paper from Physician Growth Partners answers critical questions for medical practices considering a private equity investment, such as:
- What are the benefits of working with private equity?
- Is it better to sell to a private equity group or a hospital system?
- Can you maintain independence in a private equity partnership?
- How are deals structured and what is “fair” compensation?
- What are the advantages of working with a transaction advisor?
Be prepared when a private equity firm approaches your practice.

This e-book offers candid insights and best practices from dental leaders on their recent technology initiatives.
Download to learn:
- How organizations are streamlining their digital tools and unifying teams
- Opportunities for artificial intelligence at various stages of the patient journey
- Key aspects of change management when deploying new tech

Becker's Dental + DSO Review recently spoke with Sadiye Akturk, global solutions ambassador at Straumann Group DSO Global, to explore how cloud-based dental practice management technology can address the pressing challenges facing these organizations.
Learn how a cloud practice management system can:
- Make it easier to monitor performance across multiple locations and view real-time analytics.
- Increase production at your dental organization.
- Help reduce day sales outstanding.

In this must-read e-book, you'll find a collection of seven articles that paint a picture of today's current DSO and dental landscape, common challenges associated with growth, and how dental leaders are using technology for streamlined patient engagement and stronger finances.
Download to learn more about:
- The role of emerging artificial intelligence technology in dentistry
- Executives' tips for improving the patient experience
- What 60% of the largest DSOs are using to strengthen operations + their bottom line

However, emerging technology can reduce processing fees for practices while seamlessly integrating with most practice management system platforms. This white paper details how dental leaders can use dual payment processing as a substantial cost-saving solution for their practices.
Key learnings:
- Why concealed fees in dental practice payments surpass standard charges
- The nuances between dual pricing and cash discount or surcharge processing
- How software integration can enable seamless payment processing through your PMS while reducing interchange and other fees

This ebook offers a comprehensive guide on navigating the evolving dental landscape, including valuable insights from industry experts on enhancing patient experience, leveraging marketing for growth and adopting cutting-edge technologies. Readers will discover:
- How emerging technologies are transforming the patient experience
- Strategic marketing techniques to align operations and marketing for effective growth
- Effective management techniques to navigate change and foster a culture of continuous improvement

However, even in the face of these challenges, there is cause for optimism. Remarkably, many dental practices are seeing significant growth. This annual survey of dental professionals helps provide clarity and understanding around the state of technology adoption, insurance, patient financing and more. Hundreds of dental practices and DSOs were represented in the survey.
In this report, you'll discover:
- Ways the economy has influenced dental practices' production and treatment acceptance.
- How dental teams are addressing insurance reimbursement challenges.
- Lessons from practices on optimizing workflows and efficiency using technology.
- The unique mindset and strategies that propel high growth practices to remarkable success.

This e-book distills the secrets of the world's best front-line teams into seven habits to help dental practices deliver an exceptional patient experience every time. The insights are based on interviews and analysis on what's worked at thousands of prominent experience brands, such as Starbucks and Uber.
Learning points:
- What daily habits the best and brightest customer experience brands implement
- How to master a seven-step process to increase repeat visits, strengthen staff retention and get more patient referrals
- How to introduce and implement habits across teams

In this guide, you'll find pertinent information and how-to's for navigating regulatory compliance as a DSO.
Download to learn more about:
- What regulatory compliance is and how it can benefit your DSO
- Common compliance mistakes and how to avoid them
- How to simplify compliance management, tracking and reporting

In this must-reads e-book, you'll find a collection of seven articles that paint a picture of today's current DSO and dental landscape, common challenges associated with growth, and how dental leaders are using technology for streamlined patient engagement and stronger finances.
Download to learn more about:
- The role of emerging artificial intelligence technology in dentistry
- Executives' tips for improving the patient experience
- What 60% of the largest DSOs are using to strengthen operations + their bottom line

Same-store growth entails boosting productivity and profitability within your organization compared to the previous year. It's about refining existing systems, adopting innovative technology, and seizing opportunities in an ever-evolving market.
In this eBook authored by Brian Colao, Director of DSO Industry Group at Dykema, you'll learn:
- Ways to leverage data-driven insights to assess your practice's health, identify growth opportunities, and optimize operational efficiency.
- How to boost same-store growth by using technology to enrich the patient journey and provide individualized care.
- Methods to attract, cultivate, train and empower staff using the latest technologies.

In a recent advisory call hosted by Becker's Dental + DSO Review and sponsored by Solutionreach, industry leaders discussed how technology solutions can and are improving operational efficiency, leading to positive effects on the patient and staff experience. They also shared key opportunities and obstacles they are facing
This short summary of the call covers:
- How DSOs are standardizing systems to maximize efficiency
- The type of technology DSOs are using, and for what purposes
- Using technology to improve patient interactions, including around finances

In this white paper discover:
- Emerging trends in subscription-based care, plus the rate of industry adoption
- The ties between patient sacrifice, satisfaction, and profitability
- How to use subscription business strategies to cut patient acquisition costs and extend lifetime value
- Top considerations for implementation in your dental practice(s)

AI detection assistance gives practices a way to improve clinical performance without requiring more team members or tools. AI is also a crucial element in attracting and training new providers.
In this whitepaper, you'll learn six ways to make your DSO attractive to the most talented providers who will help your organization succeed.
Key learnings:
- How to showcase AI during interviews with potential new hires
- Ways AI can improve diagnosis and care
- Using AI as a training tool to improve patient education

However, technology can help dental leaders effectively navigate these challenges.
In this advisory call recap from Becker's Dental + DSO Review, explore how data and analytics can offer operational, clinical and staff support, uncover the best practices in analyzing and reporting data effectively, and learn how data-driven insights can influence not only metrics — but outcomes as well.
Key learnings:
- DSO financial and operational leaders' approaches to navigating crises and how technology can help
- How data analytics can help mitigate staff turnover
- Key metrics to watch

Understaffing not only puts a strain on DSOs, but it also has negative implications for the patient experience and care quality. Since staff shortages aren't going away anytime soon, developing a long-term strategy to overcome burnout and do more with fewer staff is critical to DSO success.
In this guide you'll learn how you can leverage technology to:
- Automate time-consuming administrative tasks
- Shrink practice phone volume
- Give staff flexibility & support
- Improve recruitment efforts
- Keep staff focused on what matters — patients

Read more to learn:
- The DSO's major growth areas, including $150 million in annual revenue
- How they tackled key services like accounting, finance, human resources and technology at each practice in the network
- Analytics used and improvement plans developed, as well as strategies for compliance and risk mitigation

To combat challenges such as maintaining high patient and employee satisfaction levels and managing critical financial KPIs, many DSOs are turning to cloud communications.
In this whitepaper, RingCentral leaders Lance Mehaffey, Senior Director of Healthcare Industry Marketing, and John Poli, Healthcare Industry Principal, spoke with Becker's Dental + DSO Review to discuss how DSOs are getting the most out of communication tools.
Two notable case studies featured in this whitepaper:
- How Pacific Dental Services decreased patient no-shows
- How Heartland Dental turned missed calls into new patient appointments

Juggling these responsibilities on top of providing patients with the care their patients deserve can be a challenge without the right support.
In this white paper, you'll learn about the role of technology in oral surgery management and how it can support clinical excellence and practice efficiency.
Key learnings:
- How cloud-based practice management tools can improve workflows
- Enhancing shared decision-making culture using digital technology
- Using cloud technology to help transform clinical care and administrative processes
Through remote monitoring, orthodontists can detect and manage patient aligner emergencies and decrease the need for an in-person visit.
In this study, you will learn how remote monitoring can be used to benefit both patients and staff by cutting down on in-person appointments and getting patients the care they need in a timely manner.
Key learnings:
- How DentalMonitoring can help improve the remote detection and management of emergencies related to complex aligner treatments
- Understand potential impacts on practice efficiency regarding treatment control and appointment saving

Many leading dental practices have partnered with patient financing solution vendors to improve patients' access to care. Providing best-in-class offerings also improves the patient experience.
In a 2022 survey, 59 percent of respondents from the dental field indicated that fast, safe and secure financing solutions improve the patient experience at their practice.
Take the first step toward providing this much-needed service by getting the facts.
This report describes:
- Trends in patient financing
- Benefits of patient financing solutions for patients and practices
- What to look for in a patient financing solution and in a vendor
- Case studies that highlight the benefits to patients and dental practices of modern, best-in-class financing solutions
Key points of interest:
- Embrace dynamic scheduling to optimize your workflow
- Improve clinical control and safety by using data and analytics
- Improved communication with patients leads to improved treatment outcomes

Patients are craving more convenient ways to communicate with their healthcare providers. In fact, 96 percent of patient complaints are linked to poor communication or service by office staff and physicians, according to a study published in the Journal of Medical Practice
Management.
Increasing demand for real-time communication is leading many dental practices to adopt text messaging instead of relying solely on phone calls, which can be frustrating and inefficient for patients. This whitepaper explores how dental practices can give patients the convenient communication they crave and features insights from Lisa Blair, COO of Inspire Dental Group in western New York.
Key learnings:
What patients want from their dental experience
5 strategies to meet new patient communication expectations

CareCru is the creator of Donna, an AI-driven growth platform for dental practices and dental groups. Donna intelligently automates front office work, thus boosting team productivity, evaluating practice health and providing actionable insights for improvement. This ultimately creates happier employees and an enhanced patient experience.

