Most providers recognize that the underlying healthcare cost pressures the government, employers and consumers face will inevitably lead to changes in how care is reimbursed, progressing in time toward a new form of managed care that preserves consumer choice and access while creating incentives for providers to improve care coordination and lower cost. Reducing the cost of care while improving quality is the right thing to do — the question really is one of timing, pace, and which model(s) (e.g., medical home, bundled payment, clinical integration, ACO) is most appropriate for the organization given local market dynamics and payor and physician relationships. Each of these integrated models incorporates the importance of case management. Despite all of the models to choose from, the same general concepts can lead to success under each. That is, there are really just a few key messages that every healthcare provider executive needs to know.
An organization’s "care management model" is its approach to coordinating inpatient, post-acute, physician office, and home-based care for patients with episodic and chronic disease management needs. How each of the separate components of the Care Management Model functions independently and with each other to identify patients with gaps in care and "high-risk" patients is the integral component to realizing cost savings. For the theorized cost savings of an organization's ACO financial model (typically 3 to 10 percent) to materialize requires a clear plan that deploys resources around high-yield opportunities for clinical quality outcomes and cost improvement. How well defined this care management model is (i.e., the clinical conditions of focus, the staff resources to coordinate care, and the processes and systems to support care management) determines the winners and losers in a value-based payment world.
In the new world of value-based payment, the care management model may provide the greatest opportunity for organizations to differentiate themselves from their competition to manage costs and improve profitability. Providers will increasingly need to take more responsibility for managing the total cost of care as payments migrate from fee-for-service to shared savings/loss, partial-risk and full capitation. This involves broadening the focus from within the walls of the hospital and adopting a broader definition of how care delivery occurs across the continuum (see Diagram 1).
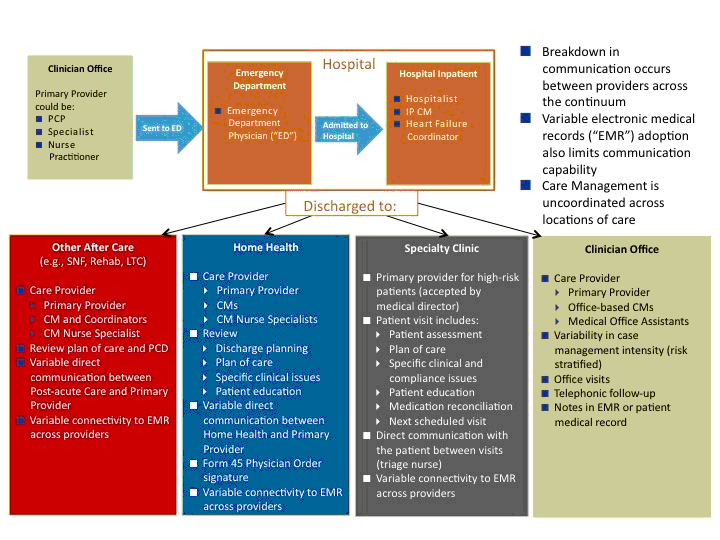
Priority areas to address
Roughly 5 percent of the population accounts for 50 percent of the total healthcare cost in America. [1] Conditions that drive a majority of those costs in a non-Medicare population include coronary artery disease, congestive heart failure, diabetes, chronic obstructive pulmonary disease, asthma, mental disorders (excluding dementia) and osteoarthritis. [2] Medicare high cost conditions include many of the same diseases: hypertension, hyperlidemia, heart disease, diabetes, COPD/asthma and osteoarthritis. [3] As healthcare systems manage the care for the patients with chronic diseases, consideration should be given to the cost opportunity of the anticipated outcomes and the timeline to realize those changes. Opportunities for improving healthcare costs generally fall into a handful of categories with varying ability to influence cost-savings improvement and change (see Table 1).
Table 1
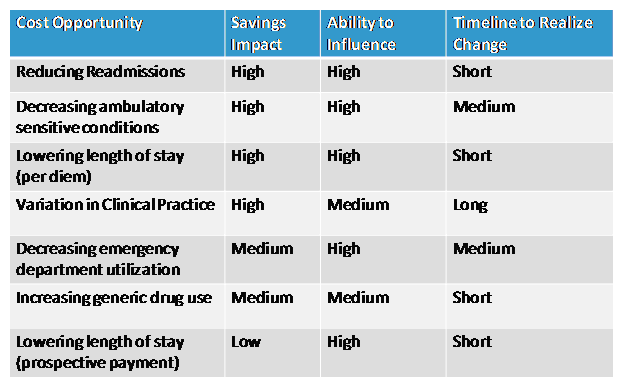
Steps to defining the care model
As an organization undertakes the task of designing a care management model that will coordinate the patient’s care across the continuum, there are several key steps that should be considered. These include:
Transition from today to tomorrow
Organizations have seen successful program development by involving key physician and administrative leaders in an assessment, planning, and implementation process. A model for this approach is to establish a steering committee or planning group with the authority to:
Aligning resources around the patient population
Upon initial assessment and when their clinical status changes, patients may be classified into one of five levels of care management need, depending on their clinical care requirements (see Diagram 2). Within any given year, experience suggests that approximately 10 percent of the patients will be high utilizers of resources based on their chronic disease(s). The care coordination for these complex patients' requires the health system to optimize smooth transitions through various communication strategies. Nurse care managers and physicians work with a team of related disciplines, the patient and their supports to modify the care plan for a patient appropriate to their clinical situation. Then they work to implement a plan of care that addresses their current needs, transitioning the patient higher or lower in the level of care needed.
Diagram 2
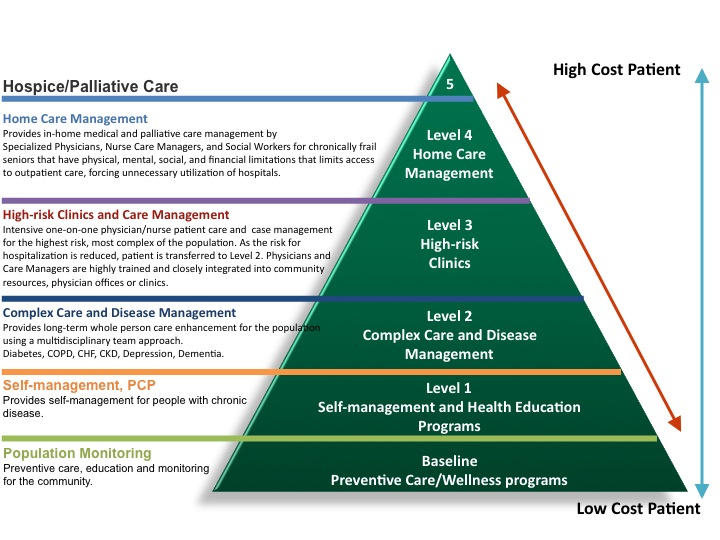
Case study
HealthCare Partners is one of the nation's largest physician groups serving California, Nevada, and Florida. Their approach has been population health aimed at health education and self-management for healthy patients and those with basic chronic diseases. Interdisciplinary teams work intensively to help patients manage complex chronic illnesses.
In recent years, HCP instituted two interventions to support high-need patients at risk of hospitalization. At five Comprehensive Care Centers, multidisciplinary teams care for patients who have just been discharged from a hospital or who have conditions such as COPD or CHF. Homecare Teams of physicians, social workers and case managers visit homebound patients. The goals are to control conditions and return patients to care with their primary care physicians and free up resources for other high-need patients.
Results include Medicare patients use of 800 acute hospital bed days per 1,000 people —roughly one-third the national average. Hospital readmission within 30 days is just 12 percent —half the national average. Patient satisfaction rates are high. Cost savings are $2 million annually for every 1,000 members.
Key lessons for CFOs and CEOs
As organizations engage the healthcare team in designing care management models that are coordinated, seamless and patient-centered, there are few key lessons:
Footnotes:
[1] National Institute for Health Care Management Foundation Data Brief, July 2011.
[2] Center for Healthcare Research & Transformation, Health Care Cost Drives Issue Brief, August 2010.
[3] Kenneth E. Thorpe, Lydia L. Ogden and Katya Galactionova, Chronic Conditions Account For Rise In Medicare Spending From 1987 To 2006. Health Affairs, 29, no.4 (2010):718-724).
- Changing the way that organizations evolve from volume to value-based will be a multi-year journey that will involve a period of time of living in two worlds: volume-based fee-for-service and fee-for-value. Paying attention to the pace of change in the local environment is key to surviving this schizophrenic period.
- Organizations must embrace changes required in this era as a cultural transformation and a radically different way of thinking about how care is organized and delivered — and the role that various stakeholders play (including the patient!). Incentives and compensation are still predominately based on driving more volume and fees.
- Hospitals need to increase market share and reduce their cost base to remain profitable. Survival will require the ability to live on Medicare reimbursement rates or less.
- Improving payment rates will require organizations to achieve quality thresholds or better.
- Starting first with self-insured employees and beneficiaries or a commercial program can be a mechanism for incrementally increasing exposure to shared savings/loss arrangements and risk-based reimbursement while ramping up care management capabilities.
- The care management model design and implementation will differentiate those who succeed from those who fail.
An organization’s "care management model" is its approach to coordinating inpatient, post-acute, physician office, and home-based care for patients with episodic and chronic disease management needs. How each of the separate components of the Care Management Model functions independently and with each other to identify patients with gaps in care and "high-risk" patients is the integral component to realizing cost savings. For the theorized cost savings of an organization's ACO financial model (typically 3 to 10 percent) to materialize requires a clear plan that deploys resources around high-yield opportunities for clinical quality outcomes and cost improvement. How well defined this care management model is (i.e., the clinical conditions of focus, the staff resources to coordinate care, and the processes and systems to support care management) determines the winners and losers in a value-based payment world.
In the new world of value-based payment, the care management model may provide the greatest opportunity for organizations to differentiate themselves from their competition to manage costs and improve profitability. Providers will increasingly need to take more responsibility for managing the total cost of care as payments migrate from fee-for-service to shared savings/loss, partial-risk and full capitation. This involves broadening the focus from within the walls of the hospital and adopting a broader definition of how care delivery occurs across the continuum (see Diagram 1).
Diagram 1

Priority areas to address
Roughly 5 percent of the population accounts for 50 percent of the total healthcare cost in America. [1] Conditions that drive a majority of those costs in a non-Medicare population include coronary artery disease, congestive heart failure, diabetes, chronic obstructive pulmonary disease, asthma, mental disorders (excluding dementia) and osteoarthritis. [2] Medicare high cost conditions include many of the same diseases: hypertension, hyperlidemia, heart disease, diabetes, COPD/asthma and osteoarthritis. [3] As healthcare systems manage the care for the patients with chronic diseases, consideration should be given to the cost opportunity of the anticipated outcomes and the timeline to realize those changes. Opportunities for improving healthcare costs generally fall into a handful of categories with varying ability to influence cost-savings improvement and change (see Table 1).
Table 1

Steps to defining the care model
As an organization undertakes the task of designing a care management model that will coordinate the patient’s care across the continuum, there are several key steps that should be considered. These include:
- Analyze historical claims, utilization, cost and clinical quality data to identify the clinical care needs for the target patient population.
- Prioritize the four to five key clinical conditions and multiple co-morbidities of focus. These may be different for commercial versus Medicare versus Medicaid.
- Establish clear clinical quality outcomes and cost-improvement goals.
- Design a care management model that coordinates resources — various care managers, transitions in care, post-acute care facilities and ambulatory care
- A general approach is a blend of the top 10 to 20 percent of "high-risk patients" and specific programs for clinical conditions (i.e., disease management).
- Identify staff resource roles (i.e., outpatient care management team, including an RN case manager, clinical pharmacist and the patient's primary care physician), call centers, home care, home-based monitoring, and psychosocial support.
- Evaluate the impact on physician offices and how the care management resources will work with physicians to coordinate care.
- Determine if there is a role for a catastrophic case manager who can act as a coordinator and liaison between all interested parties, enhancing communication and promoting teamwork for the most positive outcome achievable for the top one to two percent of patients who have high utilization needs.
- Measure the effectiveness of outpatient care management support resources by modeling pre- and post-implementation results.
- Reevaluate patient care and resource needs; consider if staffing levels are optimal to maximize results or if resources should be reorganized.
Transition from today to tomorrow
Organizations have seen successful program development by involving key physician and administrative leaders in an assessment, planning, and implementation process. A model for this approach is to establish a steering committee or planning group with the authority to:
- Develop a common vision for coordinating care across the continuum.
- Perform a current state assessment to understand gaps in care and opportunities for improvement and specific program initiatives to be developed in a future state model.
- Define the care model, populations to be served, and how clients transition from one area of service to another depending on their clinical need.
- Establish clinical work groups to prioritize clinical care initiatives and to adapt or adopt evidence-based guidelines to reflect the population characteristics of the communities served.
- Develop a staffing model that supports care delivery in the most appropriate, high quality and cost-effective setting.
- Develop educational resources and a communication strategy to inform physicians, staff and patients on the attributes of the care model, the role of care managers and services that are available to providers and their patients.
Aligning resources around the patient population
Upon initial assessment and when their clinical status changes, patients may be classified into one of five levels of care management need, depending on their clinical care requirements (see Diagram 2). Within any given year, experience suggests that approximately 10 percent of the patients will be high utilizers of resources based on their chronic disease(s). The care coordination for these complex patients' requires the health system to optimize smooth transitions through various communication strategies. Nurse care managers and physicians work with a team of related disciplines, the patient and their supports to modify the care plan for a patient appropriate to their clinical situation. Then they work to implement a plan of care that addresses their current needs, transitioning the patient higher or lower in the level of care needed.
Diagram 2

Case study
HealthCare Partners is one of the nation's largest physician groups serving California, Nevada, and Florida. Their approach has been population health aimed at health education and self-management for healthy patients and those with basic chronic diseases. Interdisciplinary teams work intensively to help patients manage complex chronic illnesses.
In recent years, HCP instituted two interventions to support high-need patients at risk of hospitalization. At five Comprehensive Care Centers, multidisciplinary teams care for patients who have just been discharged from a hospital or who have conditions such as COPD or CHF. Homecare Teams of physicians, social workers and case managers visit homebound patients. The goals are to control conditions and return patients to care with their primary care physicians and free up resources for other high-need patients.
Results include Medicare patients use of 800 acute hospital bed days per 1,000 people —roughly one-third the national average. Hospital readmission within 30 days is just 12 percent —half the national average. Patient satisfaction rates are high. Cost savings are $2 million annually for every 1,000 members.
Key lessons for CFOs and CEOs
As organizations engage the healthcare team in designing care management models that are coordinated, seamless and patient-centered, there are few key lessons:
- Communicate and recommunciate the vision about value-based care.
- Understand that redundancy must be removed from the system.
- Build care management competencies today.
- Organizational change of this magnitude requires a cultural transformation and a clear mandate about the patient.
- Provide opportunities to train existing caregivers to new roles with an emphasis on communication, coordination, collaboration, and accountability.
- In this era of transparency, the winner will be the organization that best manages the continuum of care for the patient.
Footnotes:
[1] National Institute for Health Care Management Foundation Data Brief, July 2011.
[2] Center for Healthcare Research & Transformation, Health Care Cost Drives Issue Brief, August 2010.
[3] Kenneth E. Thorpe, Lydia L. Ogden and Katya Galactionova, Chronic Conditions Account For Rise In Medicare Spending From 1987 To 2006. Health Affairs, 29, no.4 (2010):718-724).

