For some hospital administrators, surgical services are perceived as a fragile “black box” that should not be tampered with for fear of upsetting surgeons and losing case volume to competitors or ambulatory surgery centers. However, hospitals must never put off improvements to surgical services that are necessary for optimal case throughput and cost efficiency. Neglecting this could cripple a hospital’s ability to provide care to communities in need and lead to financial distress.
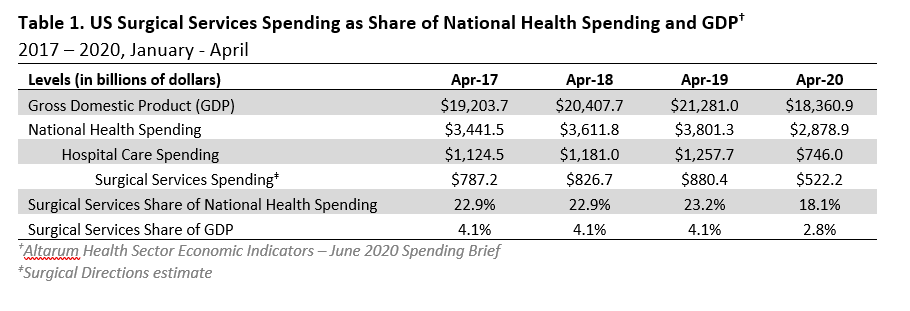
COVID-19 ripped open the “black box” of surgical services. When elective surgeries were postponed in March 2020, surgical services department volume dropped by nearly 80% across the United States. In fact, between March and June, The American Hospital Association estimated losses of over $202 billion resulting from COVID-19.5 The impact was significant: Many hospitals and health systems faced crippling financial difficulties that forced tens of thousands of healthcare employees to be furloughed, and even more took significant salary reductions.4
Savvy leaders and administrators have long been acutely aware of the importance of surgical services and have instituted mechanisms to optimize processes, governance, and staffing while maintaining high-quality patient care. High-performing organizations focused on these key concepts to strengthen their surgical services departments, positioning their hospitals to remain viable through turbulent times:
- Collaborative culture between surgeons, anesthesiology, nursing and administration
- Optimized access through dynamic, efficient block scheduling and surgeon-led governance
- Smooth patient transitions, starting at time of scheduling through 90 days post-surgery
- Leverage technologies and data to maximize outcomes while minimizing costs
Hospital budgets are tighter than ever because of the impact of COVID-19. So, what’s the right balance between reducing short-term costs to “weather the storm” and using this opportunity to make long-term remunerative investments?
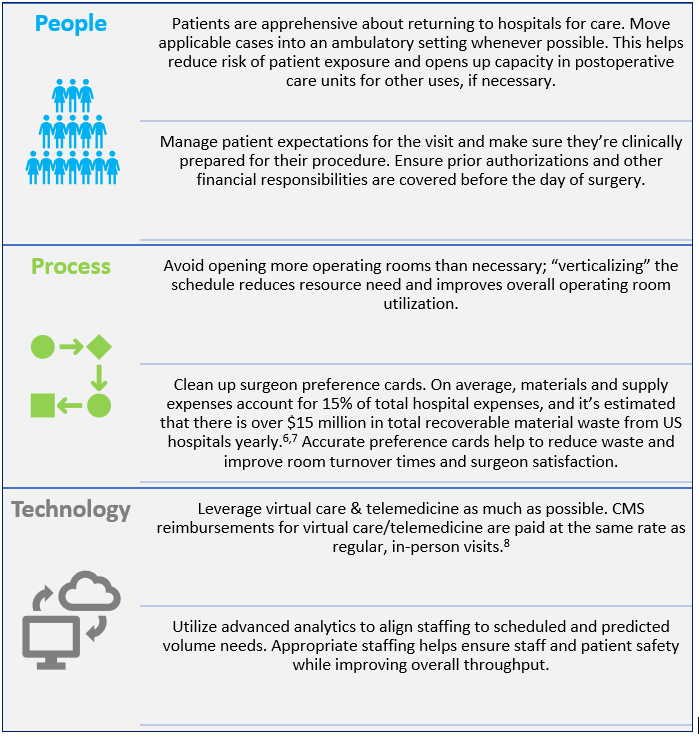
Within the current COVID-19 surgical services environment, there are several strategies you can implement quickly to reduce infrastructure cost while being mindful of budgetary constraints. Balancing People, Process, and Technology (PPT) is a useful way to help hospitals improve, even in these challenging times. New technologies are emerging that can help accelerate financial benefits for hospitals, especially if they can be leveraged at a system-wide level. At that level, the economies of scale of coordinated, system-wide enhancements instead of implementing process and technology changes in a piecemeal, facility-by-facility manner are significant. The time is value is also greatly reduced. The efficacy of a system-wide program should always be explored.
For more information, please contact Surgical Directions at 312-870-5600, or email us at info@surgicaldirections.com. You may also visit our website at www.surgicaldirections.com.
About Surgical Directions
Surgical Directions is the nation’s leading partner for health systems, hospitals, and ambulatory surgery centers committed to improving the operational, financial, and clinical performance of their perioperative and surgical services. Our consulting team is led by nationally recognized, practicing anesthesiologists, nurses, and healthcare business leaders experienced in organizational design, governance, scheduling, block design, strategic planning, material management, physician relations, staffing, and much more. Our team members have helped over 400 facilities nationwide increase surgical volume, enhance anesthesia performance, and improve surgeon satisfaction while reducing perioperative costs and improving patient outcomes.
This article was co-authored by Leslie Basham, President and COO at Surgical Directions, and Michael Besedick, Engagement Manager at Surgical Directions
References:
- Health Sector Economic Indicators – June 2020 Spending Brief. https://altarum.org/sites/default/files/uploaded-publication-files/SHSS-Spending-Brief_June_2020.pdf
- Macario, A. Where Are the Costs in Perioperative Care? 1995. https://anesthesiology.pubs.asahq.org/article.aspx?articleid=2323555
- Ellison, A. et. al. 110 Hospital Benchmarks | 2020. Becker’s Hospital Review. https://www.beckershospitalreview.com/lists/110-hospital-benchmarks-2020.html
- Ellison, A. 29 Hospital Bankruptcies in 2020. Becker’s Hospital Review. https://www.beckershospitalreview.com/finance/29-hospital-bankruptcies-in-2020.html#:~:text=At%20least%2029%20hospitals%20across,many%20hospitals%20across%20the%20nation.
- Hospitals and Health Systems Face Unprecedented Financial Pressures Due to COVID-19. American Hospital Association. https://www.aha.org/system/files/media/file/2020/05/aha-covid19-financial-impact-0520-FINAL.pdf
- Abdulsalam, Y., and E.S. Schneller. 2017. Hospital supply expenses: An important ingredient in health services research. Medical Care Research and Review, http://journals.sagepub.com/doi/10.1177/1077558717719928
- Wan, E. et. al. Global Public Health Impact of Recovered Supplies from Operating Rooms: A Critical Analysis with National Implications. World Journal of Surgery. https://doi.org/10.1007/s00268-014-2834-2
- Medicare Telemedicine Health Care Provider Fact Sheet. Centers for Medicare & Medicaid Services. https://www.cms.gov/newsroom/fact-sheets/medicare-telemedicine-health-care-provider-fact-sheet