The majority of the population get their insurance through their employer1. The employer chooses a health insurance plan which covers all the expenses associated with a patient’s medical care: visits to the hospital, physician office or urgent care center, etc. However, if the patient is prescribed any medication, the health insurance plan segments out the pharmaceutical / medication therapy care to a pharmacy benefits manager, or PBM (see Figure 1). The PBM then identifies where the patient can receive this portion of their therapy – specifically identifying which pharmacy is considered “in network” for the patient.
Figure 1: The Fragmented Care Model
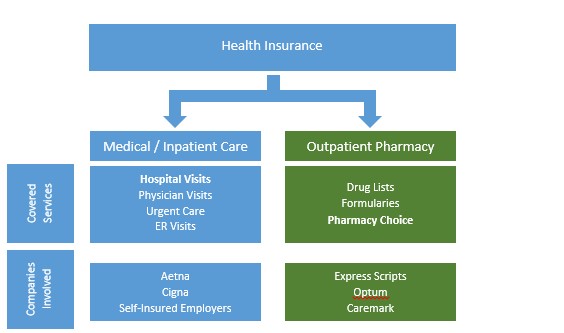
This leads to a significant fragmentation of care – especially for serious, complex diseases requiring advanced therapeutics. For the therapy to be successful in disease treatment or management, adherence and close monitoring of pharmaceutical therapy is paramount2. The pharmacist plays a vital role in managing, monitoring and coordinating with the physician to help drive optimal patient outcomes. For providers located at hospitals, the hospital based pharmacy is the ideal resource to coordinate this care model.
Health system pharmacies are able to monitor medication dispenses, refills and adherence rates for their patients – fully managing the downstream care once when a patient is discharged. The pharmacy’s operating and dispensing systems are directly linked to the hospital’s electronic medical record (EMR), linking the clinical and pharmacy teams. Clinical pharmacists have a breadth of access to that EMR in addition to the providers and specialists prescribing the complex medications.3
Due to their physical proximity and established relationship with physicians, hospital pharmacists are able to efficiently review and dispense therapy to the patient once it is prescribed. This helps cultivate a personal relationship that exists between the three groups: the medical team, the pharmacy team and the patient4. Patients rely on physicians to determine the care plan and on the hospital pharmacist to help execute that treatment regimen. It is imperative that hospital pharmacies have equally unfettered access to service their patients for the long term, once they leave the hospital.
However, that is not the case for all hospitals today. PBMs have set up a number of roadblocks to prevent hospital pharmacists from taking on this role. According to the Specialty Pharmaceutical Care Management Association, PBMs have established accreditation requirements, call center metrics and mandatory access to numerous drugs before getting access to treat their patients5. PBMs have established their own pharmacies – however, these are not integrated into the care team at the hospital or the electronic medical record of the provider. This leads to workflow fragmentation – pharmacists in the hospital will see the patient, educate them on the new therapies, explain specific clinical values but then send them to an out of state pharmacy for fulfilment.6
Health systems are taking note and fighting this unnecessary fragmentation of care. They are realizing the importance of the specialty pharmacy for patient care and are pushing for their network contracts to include coverage of long term retail and specialty pharmacological therapy. This is a grueling but necessary task as hospitals take on the responsibility of post-discharge care – one that requires significant knowledge of the hurdles. Hospital pharmacists are pushing harder to be able to manage the long term care for these patients – and are instrumental in fighting the PBM’s.
The Health System Pharmacist, who is responsible for monitoring the care for the sickest patients, should not be elbowed out of the care paradigm by the PBMs. They should be able to access all patients that are being treated in their clinics, even after they leave the four walls of the facility.
Figure 2: The Future Integrated Care Model
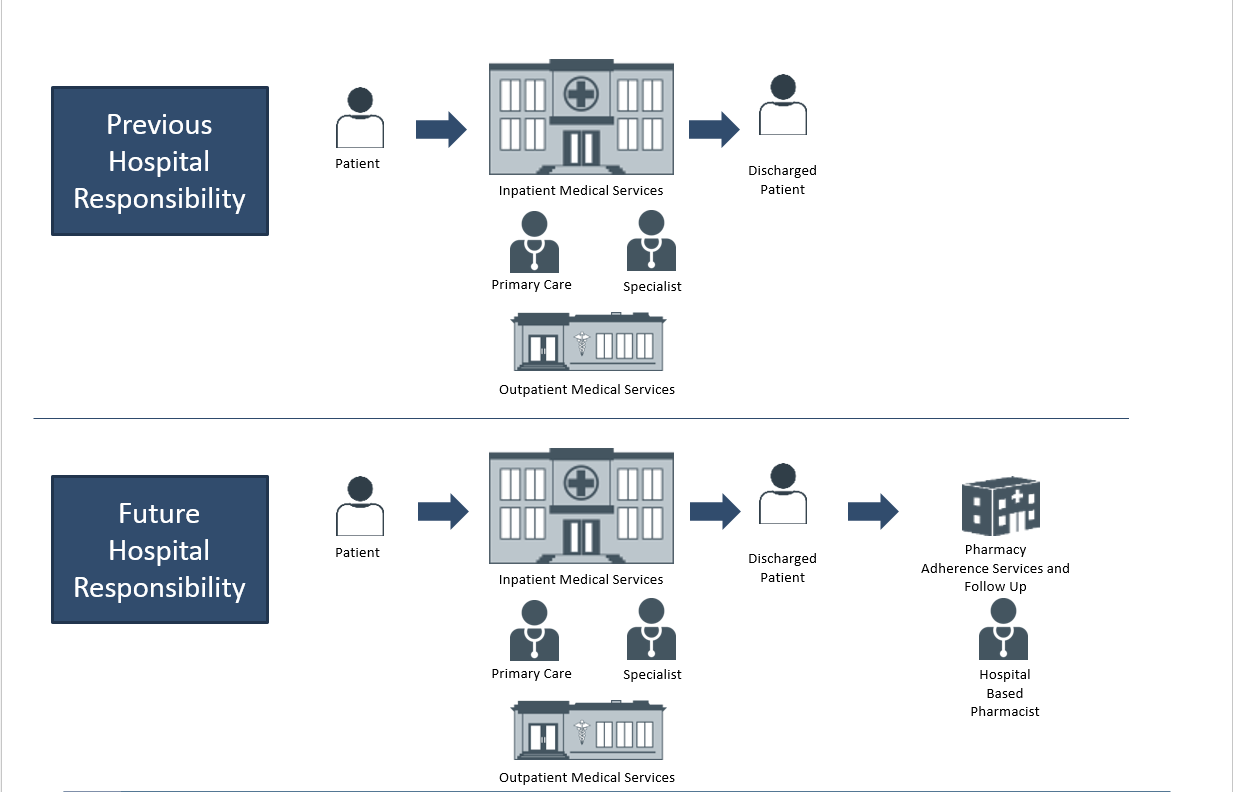
Author: Prashant K. Dilwali, MHA
Director of Business Operations – Shields Health Solutions
Prashant holds a Master of Health Administration from Johns Hopkins Bloomberg School of Public Health and a Bachelor of Science from the Massachusetts Institute of Technology. He has published in the Journal of Healthcare Management about reducing fragmentation of care and is involved with the American College of Healthcare Executives in Boston.
1 https://www.census.gov/newsroom/press-releases/2015/cb15-157.html
2 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3934668/
3 https://www.hhnmag.com/articles/6930-how-hospitals-pharmacists-improve-care-without-breaking-the-bank
4 https://www.todayshospitalist.com/Hospitalists-and-pharmacists-breaking-new-ground-by-teaming-up/
5 https://www.pcmanet.org/wp-content/uploads/2017/04/sPCMA_The_Management_of_Specialty_Drugs.pdf
6 https://www.hhnmag.com/articles/6930-how-hospitals-pharmacists-improve-care-without-breaking-the-bank
