International productivity expert Blanton Godfrey predicts health reform will produce a lot of “big winners and big losers” among the nation’s 5,000-plus hospitals.
Moody’s predicts that hospitals which can’t generate enough efficiency to stay abreast of all the upcoming changes will be forced to make spending cuts and face mergers after 2014.
It’s clear that hospital executives could use a solution that will address overcrowding and produce revenue immediately. Could the answer be as “simple” as keeping better track of patients, employees and medical devices?
Godfrey, who co-founded the Institute for Healthcare Improvement, recommends hospitals take a page from industry and concentrate on workflow improvement.
With hospitals facing the prospects of tighter payment standards, and with millions of newly insured seeking care, deeper staff cuts and service rollbacks are not a viable means for cost savings.
This year, we will instead see more hospital managers embracing a trend long used by industry and commerce – the “real-time enterprise” – to streamline flow, care for more patients, and drive rapid revenue increases.
The time has come for healthcare systems to embrace real-time capacity management. Optimizing hospital operations is perhaps the most immediate way to improve margin and control increased demand for access. For example, with the help of TeleTracking’s Avanti consulting division and its TransferCenter™ software, Methodist Healthcare System of San Antonio, Texas was able to triple its transfer volume in a year and a half, dramatically improving its bottom line as well as its ability to serve a large rural population. The volume increase was the result of a concerted effort to centralize patient logistics, optimize patient flow and manage all capacity in the eighthospital system from a single location.
Another logistics control technology, Real- Time Locating System (RTLS), has been documented to save hospitals upwards of a million dollars per year in search time and replacement costs for lost, stolen or hoarded mobile medical devices.The convergence of these technologies is creating an automated environment in which all physical operations can be monitored in real-time. This allows managers to react in seconds to changes which can negatively impact their organization.
Real-Time Capacity Management™, as it is called, is a relatively new concept to healthcare. However, it is a concept whose time has come. With this engine of change, hospitals can place themselves ahead of the game. By becoming smarter – by using information in real time -- they can increase patient throughput and revenue while maintaining high quality, preparing them for the standards of this new era of healthcare.
In the decade ahead, the ability to better use existing resources will be critical. These next-generation systems promise to deliver bottom line impact that may be greater and more immediate than the conversion to EMRs. According to venture capitalist Vinod Khosla, the man widely credited with inventing the term “real-time,” every one percent of revenue spent on real time should return 1.5 to two percent in revenue increases. In healthcare, the payoff also includes better infection control, faster transfers, and most importantly, better patient outcomes.
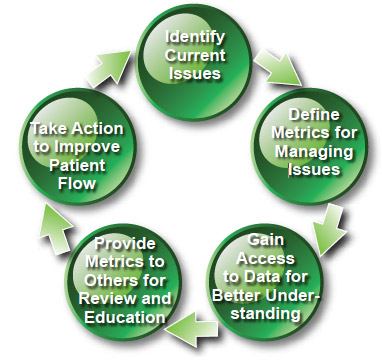
There are 5 key steps involved in the process of implementing Real-Time Capacity Management™ to improve performance:
Real-time systems can power live information to the entire hospital in an easy-to-read summary format on such things as patient tracking, staff locating, asset management and critical workflow process improvement.
Everything can be presented on graphics-rich “digital dashboards” that provide executives, managers, and placement specialists with a live “motion picture” of their institution. For example, patients can be tracked from the minute they enter the patient flow process—when they walk in the emergency department (ED) door, for example. Once bottlenecks are identified, they can be relieved before they become ingrained in the process.
Better care and better bottom line
The federal government set aside $19 billion for hospitals to adopt electronic medical records. While it’s encouraging to see the clinical side of healthcare becoming more digitized to pursue its mission, what will it do for the bottom line? How will EMRs help hospitals with their pledge to trim $155 billion in waste under the current reform law?
Three out of four healthcare executives say it won’t help, according to the 2011 HeathLeaders Media “Better Care and the Bottom Line” survey. Seventy-three percent of those surveyed said technology incentives should go beyond EMRs to include operational and system efficiency needs.
The study noted that “there is available technology that can not only address overcrowding, but also reduce other operational inefficiencies and generate additional revenue at the same time.
“Yet, while most hospitals are quick to adopt new treatment technology, they are slow to accept work flow improvement solutions, perhaps because these are perceived as too ‘industrial’.”
But the lines are blurring between clinical and operational technology, in large part because they must. Efficiency is now a matter of survival for many hospitals, regardless of reputation or the quality level of care. Increasing a hospital’s bottom line is just as important as increasing its top line. No matter how good the care, it’s irrelevant if your hospital goes out of business. After all, without a margin, there is no mission.
Moody’s predicts that hospitals which can’t generate enough efficiency to stay abreast of all the upcoming changes will be forced to make spending cuts and face mergers after 2014.
It’s clear that hospital executives could use a solution that will address overcrowding and produce revenue immediately. Could the answer be as “simple” as keeping better track of patients, employees and medical devices?
Godfrey, who co-founded the Institute for Healthcare Improvement, recommends hospitals take a page from industry and concentrate on workflow improvement.
With hospitals facing the prospects of tighter payment standards, and with millions of newly insured seeking care, deeper staff cuts and service rollbacks are not a viable means for cost savings.
This year, we will instead see more hospital managers embracing a trend long used by industry and commerce – the “real-time enterprise” – to streamline flow, care for more patients, and drive rapid revenue increases.
The time has come for healthcare systems to embrace real-time capacity management. Optimizing hospital operations is perhaps the most immediate way to improve margin and control increased demand for access. For example, with the help of TeleTracking’s Avanti consulting division and its TransferCenter™ software, Methodist Healthcare System of San Antonio, Texas was able to triple its transfer volume in a year and a half, dramatically improving its bottom line as well as its ability to serve a large rural population. The volume increase was the result of a concerted effort to centralize patient logistics, optimize patient flow and manage all capacity in the eighthospital system from a single location.
Another logistics control technology, Real- Time Locating System (RTLS), has been documented to save hospitals upwards of a million dollars per year in search time and replacement costs for lost, stolen or hoarded mobile medical devices.The convergence of these technologies is creating an automated environment in which all physical operations can be monitored in real-time. This allows managers to react in seconds to changes which can negatively impact their organization.
Real-Time Capacity Management™, as it is called, is a relatively new concept to healthcare. However, it is a concept whose time has come. With this engine of change, hospitals can place themselves ahead of the game. By becoming smarter – by using information in real time -- they can increase patient throughput and revenue while maintaining high quality, preparing them for the standards of this new era of healthcare.
In the decade ahead, the ability to better use existing resources will be critical. These next-generation systems promise to deliver bottom line impact that may be greater and more immediate than the conversion to EMRs. According to venture capitalist Vinod Khosla, the man widely credited with inventing the term “real-time,” every one percent of revenue spent on real time should return 1.5 to two percent in revenue increases. In healthcare, the payoff also includes better infection control, faster transfers, and most importantly, better patient outcomes.
There are 5 key steps involved in the process of implementing Real-Time Capacity Management™ to improve performance:

Real-time systems can power live information to the entire hospital in an easy-to-read summary format on such things as patient tracking, staff locating, asset management and critical workflow process improvement.
Everything can be presented on graphics-rich “digital dashboards” that provide executives, managers, and placement specialists with a live “motion picture” of their institution. For example, patients can be tracked from the minute they enter the patient flow process—when they walk in the emergency department (ED) door, for example. Once bottlenecks are identified, they can be relieved before they become ingrained in the process.
Better care and better bottom line
The federal government set aside $19 billion for hospitals to adopt electronic medical records. While it’s encouraging to see the clinical side of healthcare becoming more digitized to pursue its mission, what will it do for the bottom line? How will EMRs help hospitals with their pledge to trim $155 billion in waste under the current reform law?
Three out of four healthcare executives say it won’t help, according to the 2011 HeathLeaders Media “Better Care and the Bottom Line” survey. Seventy-three percent of those surveyed said technology incentives should go beyond EMRs to include operational and system efficiency needs.
The study noted that “there is available technology that can not only address overcrowding, but also reduce other operational inefficiencies and generate additional revenue at the same time.
“Yet, while most hospitals are quick to adopt new treatment technology, they are slow to accept work flow improvement solutions, perhaps because these are perceived as too ‘industrial’.”
But the lines are blurring between clinical and operational technology, in large part because they must. Efficiency is now a matter of survival for many hospitals, regardless of reputation or the quality level of care. Increasing a hospital’s bottom line is just as important as increasing its top line. No matter how good the care, it’s irrelevant if your hospital goes out of business. After all, without a margin, there is no mission.

