The past several weeks have been overwhelmingly challenging for health care systems and providers across the globe and for our country as a whole. Since the first cases of COVID-19 were reported in China in late 2019, the pandemic continued to grow exponentially and now, for the first time since the start of the pandemic, the number of cases outside China have exceeded those inside the country. Many things are still uncertain, including the shape of the pandemic curve and its total toll. However, what remains certain is that COVID-19 will have lasting impacts on our world and how we practice medicine. Measures such as social distancing, lockdowns, and closures of schools and childcare services have been instituted to help prevent the transmission of the virus. Health care systems have been inundated with COVID-19 related cases, preparing for surges and ensuring the health and safety of those who must continue to receive necessary cancer treatment despite the crisis.
As we have seen and read in recent news headlines, interruptions in chronic care have occurred and those with cancer are faced with the fear of delayed treatments, procedures, surgeries and limited treatment options. Additionally, health care workers are experiencing an increased amount of stress, navigating patient care alongside their personal fears of exposure to the virus, PPE shortages and economic uncertainty around the pandemic. Here we present insights and recommendations to help health systems navigate this challenging learning curve.
Telehealth for oncology patients
These unprecedented times have been met with unprecedented changes in the rules and regulations of telehealth within the US. Recent changes in federal privacy laws in relation to telemedicine and expansion of Centers for Medicare & Medicaid Services (CMS) reimbursements have contributed to a swift acceleration of telehealth services and widespread implementation. Such a rise will ultimately and irreversibly create a shift in the way we practice health care in the future, as well as in patient expectations.
Throughout the aggressive expansion of our oncology telehealth capabilities or program, our providers have ensured that every patient is empowered to continue to undergo the right care at the right time and that continuity of care is upheld. For some patients, oncology telehealth could be a viable bridge to on-site cancer care, and in certain circumstances the services can be utilized by oncology clinicians to provide continued care to their patients.
During this pandemic, we have significantly scaled-up our oncology telehealth program to meet the needs of our patients, providing those who are eligible based on their disease status and upcoming treatment plan with timely appointments with their clinicians, while protecting those from unnecessary exposure to risk of the virus. Prior to COVID-19, Cancer Treatment Centers of America® (CTCA) offered a limited number of telehealth services for those service lines where a physical visit was not always necessary, such as endocrinology or genetic counseling, performing on average 60 visits per month. At the onset of the pandemic, we rapidly deployed telehealth services in every service line at all sites within the CTCA® national oncology network, spanning three different time zones across the country. The result: a remarkable increase in telehealth utilization of over 80-fold in less than four weeks with 7,200 telehealth visits scheduled into June 2020 (Figure 1). Early patient and provider feedback regarding this model has been favorable, and we plan for additional survey tools to assess satisfaction with the care experience.
Oncology telehealth: Insights and recommendations for health systems
To successfully scale oncology telehealth operations, strong clinical leadership and oversight is needed, coupled with a close partnership between operations, technology finance and clinical care teams (Figure 2). Oncology telehealth is rooted within a technology-enabled clinical care delivery model requiring a strategic evaluation of the appropriate telehealth technology. Our team decided upon a technology platform that was scalable, nimble, easy to set up from both provider and patient standpoints and sustainable, as well as being HIPAA compliant and easy to integrate into electronic health records. Close attention was given to the patient-facing technology aspect and a patient concierge service was formed to provide readiness checks and troubleshooting support for every telehealth visit. To date, the patient concierge help desk is performing 130 patient readiness checks per day with an impressive average technical success rate of 97 percent.
For clinicians, we developed a patient eligibility criterion to ensure patient safety and quality. In conjunction, we ensured that those patients who needed on-site services kept their in-person visits and that appropriate PPE was in place. Scheduling was integrated with the telehealth platform and appropriate modifications in the electronic health record, such as telehealth specific notes, were implemented. Legal, compliance, billing and coding departments were incorporated into planning stages, especially given the constant updates to CMS regulations. An oncology telehealth steering committee made up of key organizational stakeholders was formed to ensure programing alignment with the overall health system strategy. Clinicians, nursing and operational leads were quickly trained on telehealth best practices, accounting for the training of nearly 400 participants prior to service launch.
For our clinicians, it was important to preserve the personal touch with their patients in each telehealth encounter. This included maintaining eye contact throughout the visit, which often means looking directly into the camera instead of into the patient’s eyes, letting the patient know that the clinician may be looking at an adjacent screen if their head is turned away, ensuring the patient is aware of anyone else in the room and ensuring the clinician introduces themselves to all those in the room with the patient.
Documentation requirements for each encounter were reviewed and telehealth consent was accounted for. Schedulers and clinic support staff were trained as well. Additionally, CTCA-specific care delivery models (including 24/7 care management hotline and e-prescription services) helped to pave the way for rapid adoption of oncology telehealth services. Most patients have smart phones and broadband access but for those experiencing technological issues, CMS has allowed for visits to be conducted through non-HIPAA use of Facetime or Skype during the pandemic.
Beyond COVID-19
Oncology telehealth can provide access to services that offer a significant benefit for both the patient and provider. Telehealth can increase patient engagement and satisfaction, improve patient convenience, provide remote, at-risk, and rural patients with access to care, leverage limited physician resources, reduce cost of care delivery, improve efficiency, provide access to specialty care and ultimately improve patient outcomes.
The pandemic may have been a catalyst for rapid adoption of oncology telehealth services, but its many benefits cannot be denied and will certainly inspire longer lasting and widespread transformation in healthcare. Whole populations of both patients and providers now have experience using telehealth. Though the future of telehealth is in large part dependent on the extent to which government rules and reimbursements continue to be improved, moving forward, expectations among patients and consumers have been set and health care systems will need to incorporate telehealth services into at least some portion of their oncology care delivery model moving forward. Cancer patients everywhere will expect and deserve nothing less.
Figure 1: Telehealth visits scheduled at Cancer Treatment Centers of America (CTCA) facilities since March 25, 2020
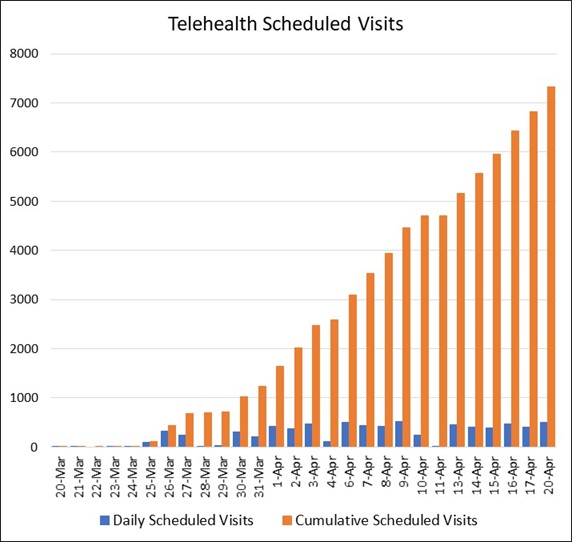
Figure 2: Oncology Telehealth Rapid Scale-Up Checklist
1. Clinical telehealth eligibility criteria
2. Clinical process flow chart
3. Clinician standard work instructions
4. Operational staff standard work instructions
5. Clinician training
6. Staff training
7. Patient eligibility criteria
8. Technology platform
9. Patient and provider help desk
10. Patient technology concierge team
11. Telehealth consent
12. Legal regulations
13. Compliance
14. Coding
15. Note documentation
16. E-prescribing capabilities: controlled substances, noncontrolled substances
17. Establish clinic workflow
18. Schedule integration
19. Patient studies capture: imaging, laboratory
References:
1. Center for Disease Control (CDC) Coronavirus (COVID-19). 14 Apr 2020 https://www.cdc.gov/coronavirus/2019-ncov/index.html
2. CMS coronavirus partner toolkit. 4 Apr 2020 https://www.cms.gov/outreach-education/partner-resources/coronavirus-covid-19-partner-toolkit
3. World Health Organization. Coronavirus disease 2019 (COVID-19): situation report – 48. 8 March 2020. Accessed at https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200308-sitrep-48-covid-19.pdf on 9 March 2020.
4. Jasper (2020) Preparing Hospitals for Coronavirus (COVID-19). Hosp Pract (1995). 2020 Apr 20.doi: 10.1080/21548331.2020.1757337.
5. Klompas (2020). Coronavirus Disease 2019 (COVID-19): Protecting Hospitals From the Invisible. Annals on Int Med
