The following content is sponsored by DataGen.
Healthcare reform initiatives, driven by government, healthcare providers and payers, are shifting the focus of care delivery and payment from individual points of service to the whole patient and entire populations. This transition from “volume” to “value” (or population health) requires a mindset change for hospitals, health systems and other providers. It necessitates an expanded perspective that encompasses the full spectrum of care for patient populations — from primary to post-acute services — to improve health and outcomes while reducing costs.
To be successful in this changing environment, healthcare decision-makers need the right tools and resources to identify, manage and track the progress of initiatives and interventions for the populations they serve. An essential element for success in this arena is access to actionable data and information — and this means the blending of “traditional” metrics (utilization, cost and quality) with newer, patient-centered analytics. These new analytic resources range from defining the characteristics and health status of populations, to identifying at-risk populations and gaps in care, to charting the progress of key interventions.
This Executive Brief offers insight into the new data sources and patient-centered analytics, and demonstrates how they can be applied for population health management, in particular for those with chronic disease.
The evolving analytic journey: New sources of data and their uses for population health management
Traditionally, hospitals and health systems have relied on inpatient metrics to determine their performance in operations, finance and quality. These metrics, largely derived from a hospital’s own data repository (e.g., discharge and billing data, electronic medical records), are fine for assessing performance such as bottom line and operating margins, length of stay, utilization (overall and by product/service line and department), case mix and compliance with core quality measures. However, as the focus started shifting to pay-for-performance, value-based metrics, measures such as readmissions and efficiency have also been introduced at the institutional level.
Understanding and managing the health of populations requires the use of data beyond what is captured in internal discharge data or the electronic medical record. A broader view of care — from primary care delivery to the post-acute care setting — is necessary to identify, manage and coordinate the care needs for population cohorts. This is particularly true for populations of people with chronic conditions, since the majority of the nation’s healthcare and socio-economic costs are associated with chronic diseases and conditions and their related health risk behaviors. According to recent reports, 84 percent of all healthcare spending in 2006 was for the 50 percent of the population with one or more chronic medical conditions.
Hospitals and health systems are now using claims data to better understand the health of populations. Once the purview of insurers/payers only, claims data are becoming more accessible as self-insured plans, insurers, health insurance exchanges, and government are providing access to encourage creative partnerships with healthcare providers. The utility of claims data for population health management is demonstrated through the Medicare Standard Analytics files being made available to hospitals, health systems and others as part of Center for Medicare and Medicaid Innovation initiatives such as the Medicare Shared Savings Program and the Bundled Payments for Care Improvement demonstration.
The full spectrum of claims data provides insight into what services were provided, by whom, at what frequency and at what cost — offering hospitals and health systems an expanded view of what is happening to a population in terms of the health status and the continuum of care.
Identifying the prevalence of chronic disease
DataGen, a national healthcare analytics company, conducted an analysis to identify the prevalence of chronic conditions and show the disparities in care patterns and program costs between beneficiaries with and without certain chronic conditions. Using a 5 percent sample of national Medicare claims data, this analysis focused on Medicare beneficiaries with diabetes and chronic obstructive pulmonary disease. DataGen’s findings show:
- When looking solely at institutional claims (i.e., inpatient, hospital outpatient, rehabilitation facility, skilled nursing facility and home healthcare) the study identified a 20 percent diabetes prevalence rate among Medicare beneficiaries. When physician claims are incorporated into the analysis, a significantly larger prevalence rate (35 percent) is seen. The diabetes prevalence rate varies from a low of 20 percent to 49 percent by state across the country.
- The prevalence of COPD among Medicare patients is 12 percent when relying on institutional data alone; that rate increases to 20 percent when physician data are included. COPD prevalence across the country ranges from 4 percent to 28 percent by state.
One very important takeaway from this data review is how valuable physician data are for deriving a true, clear picture of a population’s health status.
The impact of chronic conditions on the utilization and costs of care
DataGen examined the total Medicare program expenditures for 90-day episodes of care for beneficiaries admitted to acute-care hospitals for complications of diabetes. The average episode cost for the five most expensive regions in the United States was more than 40 percent higher than the average cost for the five least expensive regions ($13,800 vs. $19,600). The variation in program expenditures for these episodes is not driven by the inpatient hospital stay, but by variation in use of skilled nursing facility and long-term care services.
Figure 1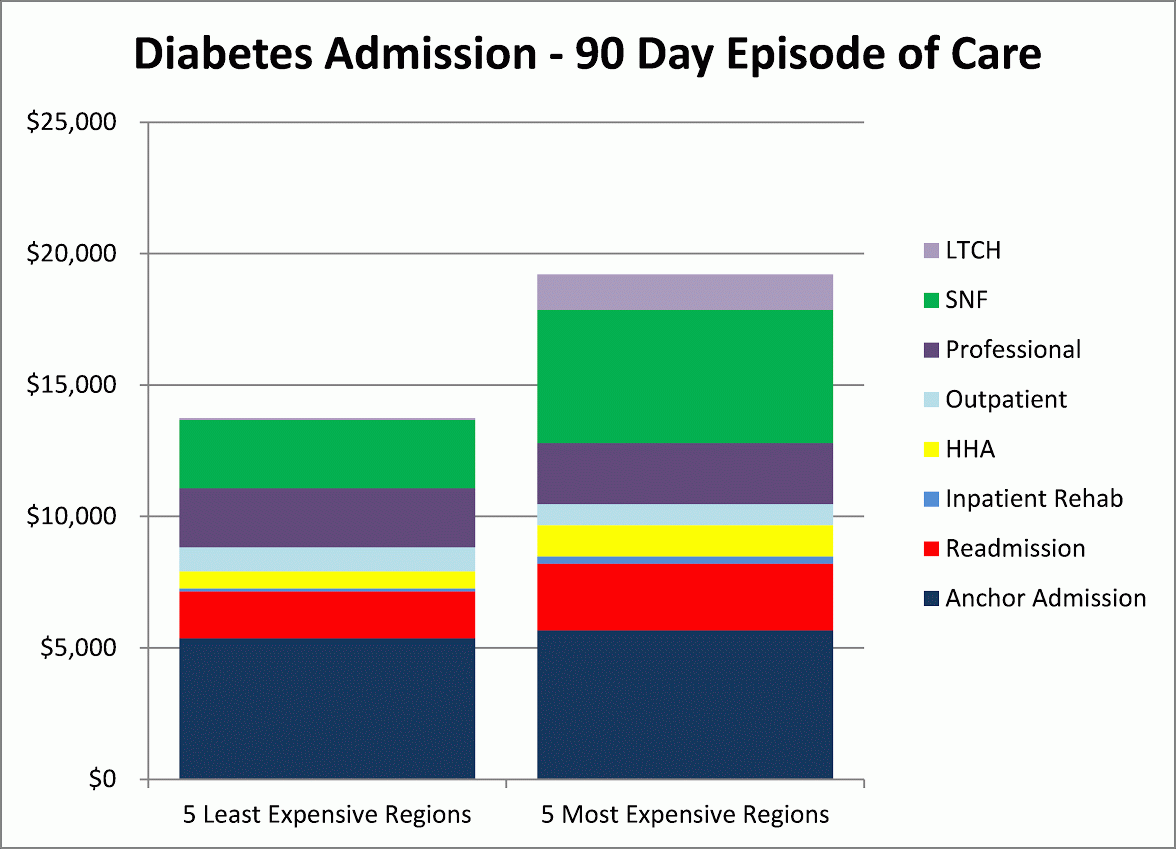
The disparity in and appropriate use of post-acute care services is an issue for hospitals and health systems to examine. DataGen’s analysis shows that within the five least expensive regions, 48 percent of diabetic admissions go home with no institutional care, while in the five most expensive regions, only 35 percent go home without institutional care. The question to be answered is: Does this population require institutional care or are there other post-discharge care arrangements and monitoring that can be just as effective and less costly, particularly since the least expensive regions also reflect lower readmission rates?
Figure 2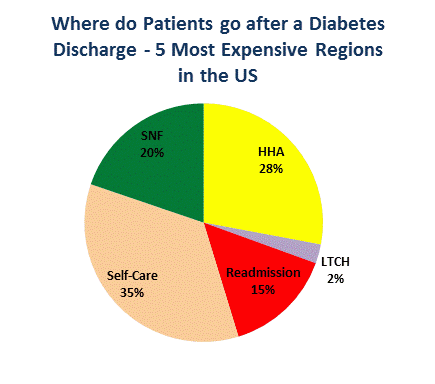
Chronic conditions are also a cost driver as a secondary diagnosis when beneficiaries require other procedures or services. DataGen quantified this impact by looking at the cost of major joint replacements for Medicare patients without chronic conditions and those with either diabetes or COPD. This analysis also looked at 90-day episodes of care and found the following:
- Of the Medicare beneficiaries who had joint replacement surgery in 2012, 11 percent had a secondary diagnosis of diabetes with chronic complications. The average Medicare expenditure for those episodes was 24 percent higher than for episodes involving patients who did not have diabetes. As shown below, the cost differentials are not due to the inpatient acute-care stay, but for higher utilization of post-acute SNF care and for a higher incidence of readmissions.
Figure 3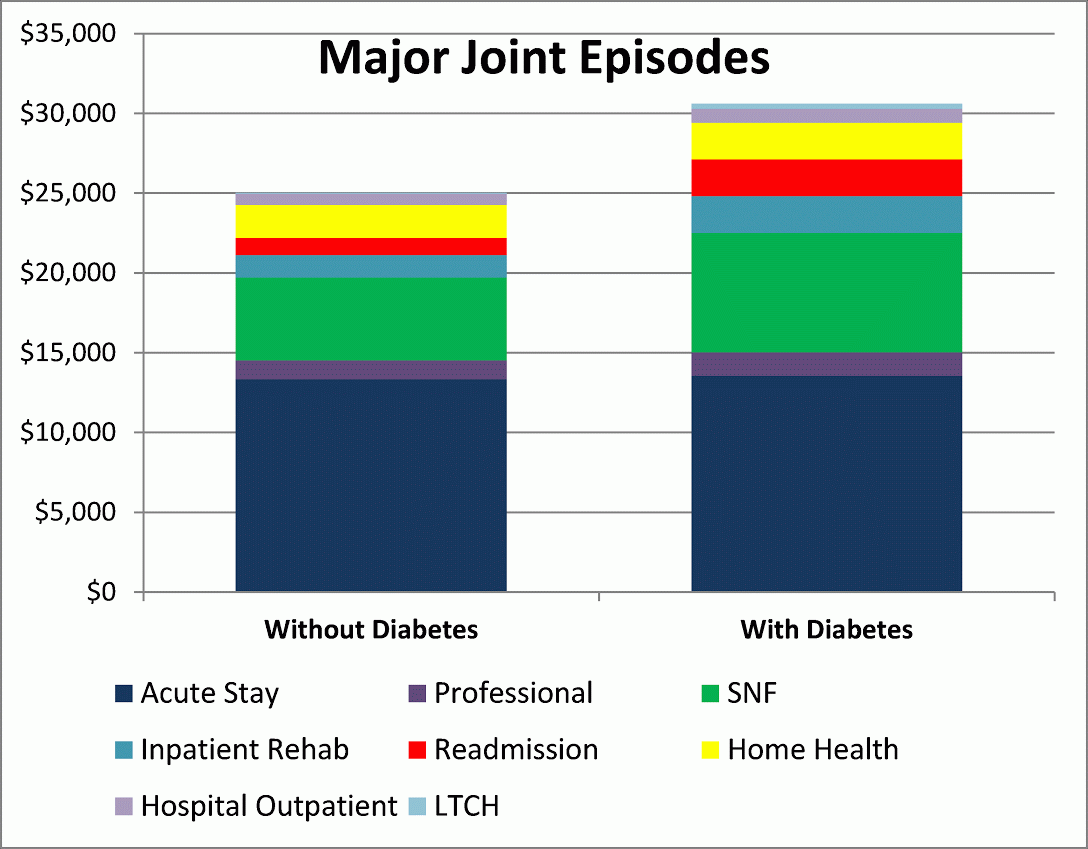
- An almost identical picture emerges for major joint surgeries for beneficiaries with and without a secondary diagnosis of COPD. Twenty-nine percent of Medicare major joint replacement surgeries in 2012 involved a patient with a secondary diagnosis of COPD, at an average episode cost that was 17.6 percent higher than the same procedure for patients without COPD. Again, the inpatient stay was not the driver for the difference in episode expenditure; the differential is due to higher utilization of SNF services and a higher readmission rate.
Figure 4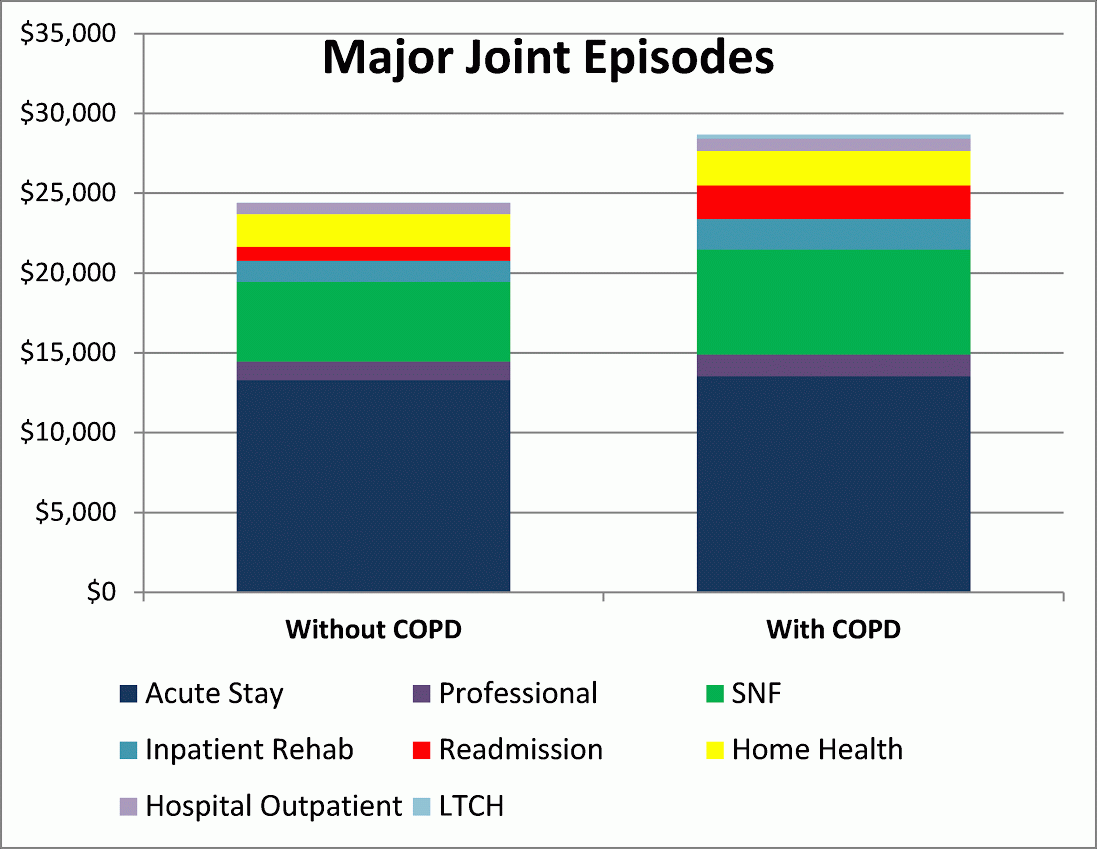
These analyses demonstrate the need for healthcare providers to focus on what occurs after patients are discharged, particularly those who are at risk with chronic conditions. Determination of the extent and magnitude of the differential and the ability to identify and target solutions is only possible with an expanded data set — one that enables the analyst to examine the full spectrum of care and to categorize different population cohorts.
Identifying opportunities for better care management
Utilizing the same 5 percent sample data source, DataGen examined Medicare physician claims in New York State to determine if the three expected tests for the diabetes population (A1C, lipid profile and eye exam) were routinely performed according to best practices for managing patients with diabetes. As shown in Figure 5, more than 55 percent of New York State Medicare diabetes beneficiaries were not receiving all three of the proper screenings. This gap analysis indicates a significant opportunity to manage the care and treatment of individuals with diabetes.
This type of analysis can inform medical homes or accountable care organizations as to “hot spot” for better care management. With these data, hospitals, insurers and/or health systems can drill down to the physician level and provide lists of patients for follow-up care. Over time, with better care management, it would be expected that other significant cost drivers, such as inpatient admissions for complications of diabetes, would decrease.
Figure 5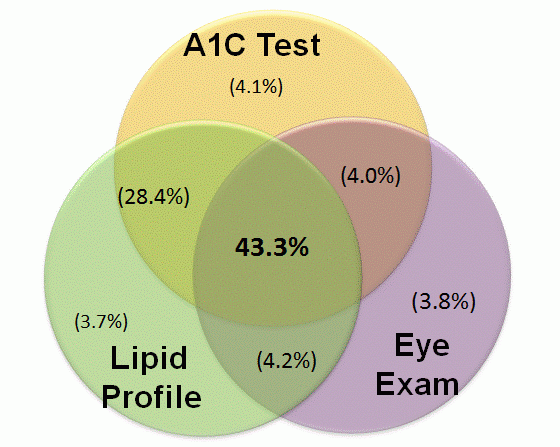
Similar analyses can be performed to measure preventable emergency department visits, preventable inpatient admissions, etc., using other chronic disease cohorts. It has become clear that in order to target and implement effective healthcare management strategies, decision-makers require solid clinical population data — not survey data, not sample data.
Making the shift to population health analytics: Recommendations for providers
The DataGen analysis highlights key areas of focus for healthcare providers, including:
- To succeed in population health management, providers need to broaden their perspective beyond traditional inpatient data sources. This means identifying, accessing and understanding new sources of data, such as claims data, and the types of insight they offer for managing the care of populations across the spectrum of healthcare services. This is particularly important for populations with chronic conditions.
- Data and analytics are a “must use” tool for identifying at-risk populations, assessing the impact of interventions, determining potential gaps in care and tracking the progress of initiatives and interventions.
- Before providers accept a risk-based contract, they need to quantify the prevalence rate of those with chronic conditions since they have higher costs and utilization and require well-coordinated, comprehensive management by primary care physicians.
- As recommended in the June 2014 “Executive Briefing: Bundled Payments,” published by Becker’s Hospital Review and DataGen, it is essential that providers accepting risk through new payment models identify the most clinically appropriate and cost-effective settings for post-acute care. An analysis of post-acute care settings can help to determine those with better outcomes and costs.
