The medical staff elects officers to represent its physicians in the hospital enterprise. Payment for medical staff officers varies by facility and position. Although historically positions were funded by medical staff dues, a growing number of hospitals are paying, or splitting the cost of stipends for medical staff officers. Chief of staff positions are most commonly paid but a number of larger hospitals contribute to other officer roles as well — an acknowledgement of the time commitment required to address hospital issues. All such payments are subject to the same Fair Market Value requirements as other physician contracts, yet historically few benchmarks have been available to document market rates without an ad hoc survey. MD Ranger surveys report benchmarks for a growing number of medical staff roles, as well as increasing payment rates.
A hospital’s medical staff typically makes the decision to pay or not to pay its officers. Historically, positions were voluntary or modest stipends were paid from medical staff dues. However, many factors account for the trend toward higher payments and requests for the hospital to help fund the positions.
A major factor contributing to higher payments is increased time demands of the positions. Joint Commission requirements for periodic review of physician credentials and outcomes, technology and quality initiatives, peer review, dispute resolution and board and committee responsibilities have all grown while the pool of physicians interested in committing significant time to such non-billable duties in the hospital has fallen. MD Ranger reports the average chief of staff spends 320 hours each year and a vice chief of staff spends 240.
Another factor in the growing number of hospitals paying for leadership roles is the growing divergence of hospital-based medicine from community/office-based medicine. The traditional role of the medical staff as a source of referrals and cross-consultations, as well as the social importance of the medical staff, is transitioning as medical groups get larger, inpatients are managed by hospital-based specialists and insurers or medical groups dictate referrals.
Lastly, economic factors, including lower reimbursements, larger group practices with productivity incentives, more part-time and employed physicians and competing internal governance demands of a practice all contribute to the trend toward more frequent payments. More physicians are reluctant to volunteer and run for office if it results in lower revenue and fewer patients, or if duties impinge on either clinical or after-hours activities.
When to pay for a leadership position
Similar to any physician contract payment, the first question is always, “Is it reasonable to pay for this position?” There are no hard and fast rules unless the facility’s Medical Staff Bylaws specify payment. However, if finding volunteers to run for office is a challenge, or if the duties of a position involve a significant time commitment that can reasonably be expected to impact a physician’s clinical practice, payment may be justified. Adopting a formal hospital policy that defines which positions are paid and the formula for payment is advisable, with both medical staff and hospital approval. Among MD Ranger partner hospitals, chiefs of staff are more frequently paid than other positions. However, it may not be reasonable or necessary to pay for all medical staff officers.
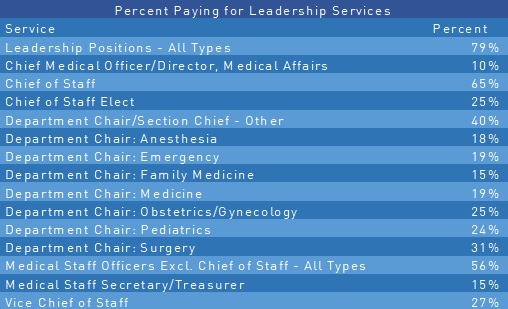
Whether you should pay, and at what benchmark rate, may depend on your institution’s size or initiatives. Sometimes, a specific initiative or issue, such as a medical staff merger, a major quality initiative, or an Electronic Health Record implementation may warrant a higher than normal payment. Larger hospitals with large medical staffs are also more likely to require a higher time commitment. Documentation of the particular circumstances, background, and demands of the position are essential to a strong compliance program.
A large percent of medical staff leadership positions are paid as flat monthly stipends rather than hourly rates. That may result in the equivalent of very low or very high estimated hourly payment rates. For example, the average time commitment of a Chief of Staff in the MD Ranger survey is hours 320, which would result in an estimated hourly payment rate of $156 for a $50,000 stipend. Alternatively, if a medical staff treasurer was paid $20,000 and only had to attend four meetings a year that required only twenty hours of work, the $1,000 per hour would be unlikely to reflect fair market value. Conversely, if a position with a large, complex medical staff required 800 hours per year, and payment was hourly at $200/hour, the resulting $160,000 per year may exceed FMV for comparable positions and could require extra documentation. Fewer leadership position contracts include required hours when compared to other types of medical directors, making hourly rate comparisons difficult. MD Ranger has also found it to be rare for medical staff officer payments to vary by physician specialty.
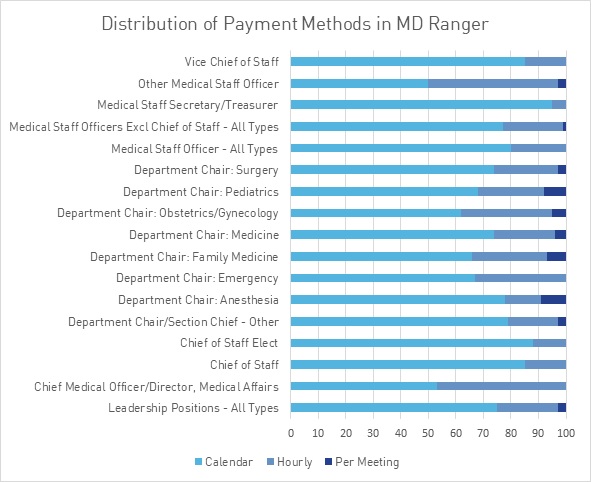
All payments to physicians that are made by health care facilities should comply with Internal Revenue Service, Stark and Anti-Kickback rules. Therefore, documentation of the time commitment, commercial reasonableness and FMV of the payments is essential.
