Reprinted with permission from Healthcare Strategies & Solutions.
Health care organizations of all types and sizes are evaluating their ability to remain independent given the significant changes underway and on the horizon. According to Irving Levin Associates, 90 hospital merger or acquisition deals targeting 156 hospitals occurred in 2011, the highest level in five years. M&A activity in the physician group sector culminated in 107 deals in 2011, up from 67 in 2010. Deal volume among hospitals and physician groups in the first quarter of 2012 tapered off some, but the consolidation trend is not projected to slow significantly in 2012.
Academic medical centers have been active participants. Examples include Loyola University Medical Center's merger into Trinity Health, University of Colorado Hospital's partnership with Poudre Valley Health System and proposed partnership with Memorial Health System in Colorado Springs, and UC San Diego Health System's acquisition of the Nevada Cancer Institute in Las Vegas.
As more care becomes concentrated within systems, academic expertise and referrals for complex specialty care alone will not protect AMCs' market positions. Sufficient scale and an aligned referral base are now essential for achieving clinical growth and meeting the academic mission. However, AMCs must proceed with caution. Mergers, acquisitions, and affiliations cannot be entered into lightly as an academic medical center's name and brand are valuable assets.
At the organizational level, academic medical centers fall into one of three major categories.
Reactive — evaluating fit and choosing to respond (or not) through a formal process or informal inquiries when other organizations initiate contact.
Opportunistic — identifying preferred partners but waiting to be approached.
Proactive — initiating the conversation with potential partners (hospitals, physician groups, non-acute care providers) who fit the organization's mission, vision and values.
The nature and intensity of the competition in an academic medical center's marketplace will strongly influence the approach chosen. Factors include the following:
When an academic medical center's primary goals for affiliation are related to improving market position and/or achieving economies of scale and capacity-related efficiencies, hospitals, health systems and physician groups are typically the focus. However, as the prevalence of bundled payments, risk-based contracting, and accountable care models increases, strong linkages across the continuum of care will be essential to demonstrate value to payors and patients. Whether the aim is structural (having all the components under one umbrella) or functional integration (effective coordination of services), the list of potential partners is increasingly likely to include home care agencies, long-term care facilities and other non-acute care providers.
1. Determine gaps or weaknesses in strategic and business goals and identify the types of organizations and capabilities that would alleviate shortcomings and strengthen positioning.
2. Identify potential partners, considering the following factors:
Existing affiliations also deserve a closer look to determine if there are opportunities to broaden the scope to include other services or tighten the existing relationship.
3. Conduct a preliminary assessment of each potential partner, including an examination of:
4. Consider other qualitative factors:
5. Summarize the pros/cons for each potential partner and prioritize opportunities.
6. Determine whether an expression of interest, at a minimum, is warranted for the organizations at the top of the list.
As AMCs consider their strategic stance toward affiliations, mergers and acquisitions, the passive approach is unlikely to serve them well and could mean that significant market opportunities are missed. A proactive approach using the six steps noted above prepares AMCs to acquire the scale and capabilities needed to thrive in a consolidating, post-reform market. AMCs that choose to be reactive or opportunistic may find that when they arrive at the dance the most suitable partners are already taken.
Average Department Chair Compensation at Academic Medical Centers
Health care organizations of all types and sizes are evaluating their ability to remain independent given the significant changes underway and on the horizon. According to Irving Levin Associates, 90 hospital merger or acquisition deals targeting 156 hospitals occurred in 2011, the highest level in five years. M&A activity in the physician group sector culminated in 107 deals in 2011, up from 67 in 2010. Deal volume among hospitals and physician groups in the first quarter of 2012 tapered off some, but the consolidation trend is not projected to slow significantly in 2012.
Academic medical centers have been active participants. Examples include Loyola University Medical Center's merger into Trinity Health, University of Colorado Hospital's partnership with Poudre Valley Health System and proposed partnership with Memorial Health System in Colorado Springs, and UC San Diego Health System's acquisition of the Nevada Cancer Institute in Las Vegas.
As more care becomes concentrated within systems, academic expertise and referrals for complex specialty care alone will not protect AMCs' market positions. Sufficient scale and an aligned referral base are now essential for achieving clinical growth and meeting the academic mission. However, AMCs must proceed with caution. Mergers, acquisitions, and affiliations cannot be entered into lightly as an academic medical center's name and brand are valuable assets.
AMCs: Where they are now
Most academic medical centers have multiple affiliations of one kind or another, although the number and type of relationships vary significantly. Partnerships related to the academic mission and medical education, in particular, are common. As technology has advanced, AMCs with service areas that cover extensive geographies have developed telemedicine networks to facilitate access to specialty care in far-flung, communities. Clinical affiliations linked to cancer centers, trauma centers, stroke centers, and neonatal programs are also frequently established.At the organizational level, academic medical centers fall into one of three major categories.
- Anchoring multi-hospital/Integrated delivery systems: University of Pittsburgh Medical Center, University of Pennsylvania Medical Center, Massachusetts General Hospital, New York-Presbyterian Hospital, Robert Wood Johnson University Hospital, Johns Hopkins Hospital
- Pursuing partnerships/Affiliations with large, non-academic systems: Loyola University Medical Center/Trinity Health, Georgetown University Hospital/MedStar Health, Creighton University Medical Center/Alegent Health
- Remaining independent (for now), while establishing multiple affiliations to achieve academic and clinical missions: UC Irvine Medical Center, University of Texas Medical Branch Hospitals at Galveston, University of Iowa Hospitals and Clinics, University of Virginia Medical Center, Stony Brook University Hospital
Reactive, opportunistic or proactive: Which approach makes sense for your market?
Academic medical centers typically follow one of three approaches regarding affiliations and other partnerships.Reactive — evaluating fit and choosing to respond (or not) through a formal process or informal inquiries when other organizations initiate contact.
Opportunistic — identifying preferred partners but waiting to be approached.
Proactive — initiating the conversation with potential partners (hospitals, physician groups, non-acute care providers) who fit the organization's mission, vision and values.
The nature and intensity of the competition in an academic medical center's marketplace will strongly influence the approach chosen. Factors include the following:
- Degree of consolidation among independent physician groups
- Size of employed physician groups and/or tightly aligned physician networks
- Number and geographic coverage of multihospital system(s) that may or may not employ and/or tightly align with physicians
- Presence (or absence) of vertically integrated systems with health plans, employed physician groups, and hospitals
- Presence (or absence) of national for-profit or not-for-profit health systems
- Concentration within the commercial payor market
When an academic medical center's primary goals for affiliation are related to improving market position and/or achieving economies of scale and capacity-related efficiencies, hospitals, health systems and physician groups are typically the focus. However, as the prevalence of bundled payments, risk-based contracting, and accountable care models increases, strong linkages across the continuum of care will be essential to demonstrate value to payors and patients. Whether the aim is structural (having all the components under one umbrella) or functional integration (effective coordination of services), the list of potential partners is increasingly likely to include home care agencies, long-term care facilities and other non-acute care providers.
6 proactive steps for AMCs Considering Affiliations, Mergers or Acquisitions
Developing a framework and defining decision-making criteria facilitates objective evaluations of merger and affiliation opportunities, and provides the foundation for AMCs to be proactive about market opportunities.1. Determine gaps or weaknesses in strategic and business goals and identify the types of organizations and capabilities that would alleviate shortcomings and strengthen positioning.
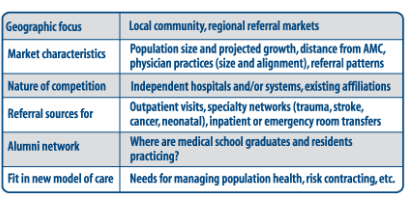
2. Identify potential partners, considering the following factors:

Existing affiliations also deserve a closer look to determine if there are opportunities to broaden the scope to include other services or tighten the existing relationship.
3. Conduct a preliminary assessment of each potential partner, including an examination of:
- Volume statistics and trends from state agency and hospital association reports
- Inpatient market share trends, overall and by specialty
- Clinical service portfolio
- Medical staff mix, quality, and alignment
- Quality metrics, including CMS core measures
- Patient satisfaction scores, including HCAHPS
- Market perception/awareness
- Recent awards, recognitions, and accreditations
- Financial performance, including payor mix
4. Consider other qualitative factors:
- Contribution to/fit with academic mission
- Advancement of priority strategic goals
- Risk/reward ratio
- Ease of implementation
- Political impacts
5. Summarize the pros/cons for each potential partner and prioritize opportunities.
6. Determine whether an expression of interest, at a minimum, is warranted for the organizations at the top of the list.
As AMCs consider their strategic stance toward affiliations, mergers and acquisitions, the passive approach is unlikely to serve them well and could mean that significant market opportunities are missed. A proactive approach using the six steps noted above prepares AMCs to acquire the scale and capabilities needed to thrive in a consolidating, post-reform market. AMCs that choose to be reactive or opportunistic may find that when they arrive at the dance the most suitable partners are already taken.
More Articles on Academic Medical Centers:
12 Revenue Pitfalls for Academic Medical CentersAverage Department Chair Compensation at Academic Medical Centers


