My colleague Carma Bylund and I saw the need for a practical understanding of empathy in the early 2000s. We developed the Empathic Communication Coding System (ECCS) as a research tool to measure if and how physicians respond to empathic
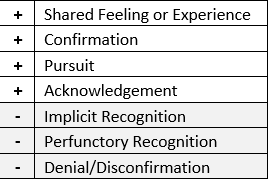
opportunities – statements of emotion, progress, or challenge – generated by patients during clinical encounters. Going beyond the cognitive and affective aspects of empathy to focus on actual behavior, the ECCS outlines 7 distinct responses to empathic opportunities; 4 convey empathy and 3 do not.
As empathy has become more central to discussions of experience and engagement, it seems like the right time for sharing this framework outside of academia. My intention is to offer a lens for better understanding of the extent to which the people involved in innovation efforts – and, by extension, the organizations in which they work – exhibit empathy for end users. A few words about the 7 responses:
- The way most people conceive of empathy is Shared Feeling or Experience (I have a similar emotion, experience, progress, or challenge), but it’s relatively rare outside of interactions that are based on shared feelings or experiences. In our studies, we saw this type of empathic response in about 2% of clinical encounters.
- There is an inherent hierarchy to Confirmation (I hear you and what you’re feeling/experiencing is valid), Pursuit (I hear you and want to know more), and Acknowledgement (I hear you), but all communicate empathy in practice. Taken together, we saw these ways of expressing empathy in about 85% of clinical encounters within our studies.
- Responses that do not convey empathy – Implicit Recognition (focusing on a peripheral aspect of what I heard), Perfunctory Recognition (offering an automatic, scripted response to what I heard), and Denial/Disconfirmation (you don’t feel that way; it’s your fault; ignoring what I heard) – do happen. In our studies, up to 13% of clinical encounters (i.e., way too much).
The percentages associated with each response category in our studies of clinical encounters could differ from those in the innovation world, but this last point deserves attention. People and/or organizations may not convey empathy if they are too busy to really listen or have fixed ways of thinking about their idea, product, or service. The first step is to solicit empathic opportunities, to notice them, be open to hearing them. We all know this doesn’t always happen.
When organizations do listen, the results are remarkable. For example, OSF HealthCare (Illinois) is a very enlightened health system. Starting with the premise that community members have a better sense of what their communities need than do healthcare executives, OSF HealthCare used one of our digital platforms to learn what matters to people living in one of the rural communities they serve. Based on the results, OSF HealthCare directed a significant donation to the local YMCA to better address needs.
An organization’s response to an empathic opportunity likely colors its reputation and portends how users will respond to related products or services in practice. OSF HealthCare could have Denied/Disconfirmed what community members shared or given some Perfunctory or Implicit Recognition, checked the ‘community input’ box, and then gone off and done whatever they were planning to do in the first place. But they didn’t. They incorporated what they heard into decision making. That’s the value of real empathy. That’s leadership. And it is leading to programs that people are more likely to use.
The value of empathy is well understood by OSF HealthCare, Froedtert & the Medical College of Wisconsin, Yale New Haven Health, and the other organizations that partner with us. There are many advantages to using empathy to improve products and services, as well as relationships with and between those who use them. Empathy is the best kind of resource: inexpensive, renewable, and mutually beneficial. The ECCS provides a useful framework for innovators to reflect on their responses to empathic opportunities.
Improving health and care by listening to the people involved is absolutely critical in this era of consumerism, value-based care and – let’s be real – burnout. Innovative digital solutions can help build powerful channels for empathic opportunities, making it easier for hospitals and health systems to understand what matters to patients, providers, and community members. The key is to respond with true empathy. And that’s the bottom line: Empathy is more than a buzzword. To be meaningful, it must be honest and clearly communicated.
***
The way for people to show empathy is to listen for emotions, progress, or challenges and then confirm, pursue, or acknowledge what they hear. The way for organizations to show empathy has another step: DO SOMETHING PRODUCTIVE with what they hear.
