Birth is by far the leading single reason for admission to U.S. hospitals accounting for 10% of all hospital stays.
(1) Although childbirth usually results in positive outcomes, adverse outcomes do occur and are devastating for families and costly for hospitals and payers. Thus, obstetrical services touch a large portion of the population and hospital budgets. In turn, improvements in labor and delivery processes and outcomes become highly germane for both medical and financial reasons.
This is a success story, describing how a patient safety team in a group of urban hospitals in Maryland changed behavior and improved obstetrical outcomes over a decade using both advanced management strategies and healthcare IT (HIT) tools. The HIT tools operated in real time at the bedside using a variety of techniques including neural networks, expert systems, statistical models and digital signal processing. While the accomplishments are noteworthy and encouraging, the greatest value from this study of more than 78,000 is how the results were obtained; learnings that other leaders in healthcare with similar missions can apply to improve outcomes and save money.
Standardizing care in obstetrics is difficult because many therapeutic decisions during labor and delivery are subjective and confirmatory laboratory tests do not exist. In addition prevalent litigation and high patient expectations fuel ever increasing intervention rates at considerable cost and diminishing returns in terms of clinical benefit.
If the simple definition of management is "the art and science of getting things done by others" then patient safety officers have a double charge of "getting things done by others and doing it more safely." While these goals can be stated rather succinctly, defining exactly how to achieve them cannot, especially when it involves changing well established behaviors. Sustaining change makes the management challenge even greater. Many worthy (and costly) healthcare projects with the best of intentions fail because a critical mass of behavioral change forces are not applied concurrently.
Rising patient complexity: Trends over a decade
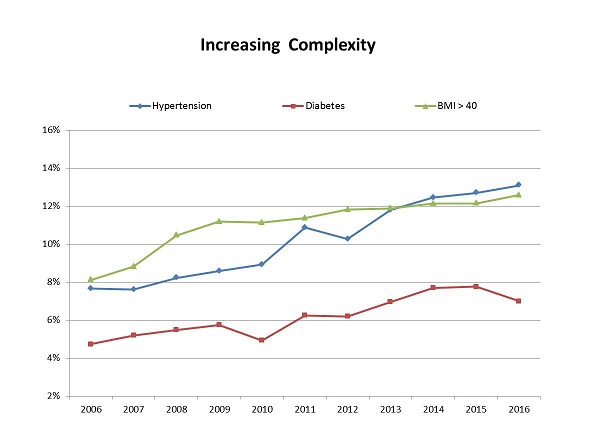
Let's begin by looking at the background, setting and accomplishments of this decade-long research. The study is large, based on 78,459 births from 2006 to 2016. The hospitals involved are four acute care, academic community teaching hospitals and regional referral centers in the Baltimore-Washington corridor. The data includes only births with a singleton baby at term. None of the observations can be attributed to variations in referral practices for preterm babies or complications related to twins or triplets. During this decade poor obstetrical factors steadily increased as is shown in Figure 1. Rates of maternal diabetes, hypertension and severe obesity all increased over time. By the end of the decade one in four mothers had at least one of these complications. Each one of these factors is associated with increased rates of cesarean and/or complications of labor and increased NICU admissions for newborns. (2-4)
Figure 1. The percentages of mothers with hypertension or diabetes or marked obesity increased over the decade.
Falling Complications and Stabilized Cesarean rates
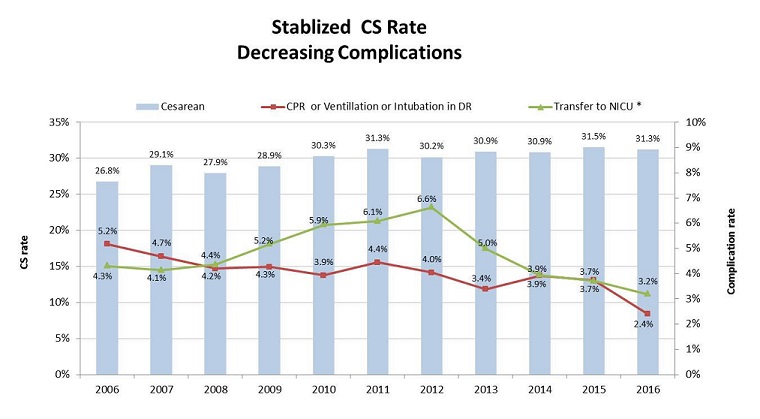
Trends in outcomes over the decade are shown in Figure 2. The rates of babies requiring unusual resuscitation measures in the delivery room (cardiopulmonary resuscitation (CPR) or assisted ventilation or intubation) decreased steadily over the decade from 5.2% to 2.4% (54% reduction P<0.0001.) The rate of babies transferred to the NICU rose during the years 2008-12 to reach a peak of 6.6%. This trend then reversed directions so that the NICU transfer rate reached an all-time low of 3.2% in 2016. (52% reduction from peak P<0.0001). Cesarean rates, which had been rising during the first 5 years (26.8% to 31.3% P<0.0001), stabilized despite the increasing complexity of their patient population. In short, the rate of women with poor obstetrical factors rose by almost one half while the rates of these newborn complications fell by half and cesarean rates stabilized.
Figure 2. Improvement in the rates of cesarean birth, NICU admission and need for resuscitation in the delivery room over the study period.
Motivation and Ability
Motivation and ability are the two foundational determinants of change. The hospital leadership teams had to learn new skills to motivate clinical teams, remove obstacles and resolve conflicts, as well as sustain and reinvigorate the process. In order to facilitate behavioral change and achieve results, clinical teams had to give up many established habits, learn new skills and utilize new tools. The threads linking new behavior patterns included clarity of purpose, collaboration and individual accountability. An impending crisis spurred motivation and the genesis of this progressive patient safety initiative.
At the administrative level
After the precipitating crisis, a highly motivated group coalesced as the change leadership team. They identified the need for new tools that would help their hospitals accomplish what had not been done prior. Some underwent training in the science of organizational behavior. They began by focusing on modifiable factors related to the initial crisis. In time, they expanded this mission and targeted specific problems with serious complications when there was good evidence that best practices improved outcomes. They engaged local clinicians respected by their peers, both for their expertise as well as their positive influence as role models in their clinical units. They listened and responded to the insights of staff on the front lines and the obstacles they and patients faced. Once a consensus was achieved from the team, a new policy was created. Directives were clear and specific to prevent short cuts that would over time jeopardize patient outcomes.
About Oxytocin
Oxytocin is a medication used in the majority of labors at some point to hasten labor and avoid complications of long labor including cesarean birth. Nurses titrate the IV oxytocin dosage at frequent intervals because every mother and fetus respond differently to this drug. Tolerance is evaluated by assessing the rate of contractions and changes in fetal heart rate.
Risk: Oxytocin overuse can cause very frequent contractions, which are occasionally associated with hypoxic injury to the baby or urgent cesarean and need for NICU care.
The problem: Marked human inconsistency in tracing evaluation especially with intermediate abnormality levels and failure to appreciate overly frequent contractions. Oxytocin misuse is common in OB litigation.
There is a maxim, "What is not measured cannot be changed." Any administrative team given the responsibility to modify organizational behavior without an ability to track that behavior and related outcomes is deeply handicapped. Consistent and frequent audits of units and/or its individuals were key factors. In 2004, the hospitals installed an intelligent EMR in the labor and delivery units that continuously evaluated all clinical information it received and produced reminders regarding expected and appropriate clinical care needs. In addition, the software produced summary statistics, not only on outcomes but also on the timing and nature of care administered. The reports were easily accessible, reviewed frequently and adaptable to the changing needs of the team. Such analysis is an essential tool for demonstrating the need for change, measuring progress and holding clinicians accountable in a transparent and equitable manner. Evidence of success is itself a motivating factor. Not only does it enable "peer recognition" but it creates positive "peer pressure," as a stark reminder to naysayers that change is possible. Frequent review with encouragement, recognition and the occasional financial incentive all played an important role in changing behavior.
At the clinician level
During this transformational period, educational programs, simulation and certification all played a role in standardizing clinical care. Simplifying processes also improved standardization. For example, in 2002 these hospitals instituted a policy that authorized nurses at the bedside to adjust or discontinue the drug oxytocin based on their own assessment of the uterine contractions and fetal heart rate patterns. Giving nurses this drug management authority facilitated timely reaction to contraction frequency.
In late 2011, the hospitals installed a suite of analytical HIT modules (PeriCALM® Solutions, Princeton, NJ) that analyzed labor progression, as well as the fetal heart rate and contraction patterns recorded by electronic monitors at the bedside. These tools addressed a fundamental requirement for a safe medical device by showing users when they were operating within a safe zone and notifying them when safe limits were exceeded. This issue is relevant in obstetrics because the assessment of labor progress and analysis of the fetal heart rates are known to be highly subjective and inconsistent across clinicians. (5-7)
About Cesarean Delivery
Approximately one in three U.S. women deliver by cesarean making it the most common hospital surgical operation. It is generally associated with few short-term complications and it lessens the rate of direct complications of labor and delivery. About 90% of first time cesareans are performed because of slow progress in labor (to avoid traumatic birth) and/or a concerning fetal heart rate pattern (to avoid hypoxic injury). Labor progress is assessed by measuring cervical dilation and fetal descent over time.
Risks: Overuse of cesarean is undesirable because it leads to higher costs and longer convalescence, few benefits and occasional but severe complications in later pregnancies. Underuse of cesarean is highly undesirable because birth related injury can result in lifelong disability for the child and costly litigation.
The problem: Clinicians are inconsistent in their assessment regarding need for cesarean delivery. Clinical guidelines defining when cesarean is indicated do not apply until after 6 cm of dilation but about half cesareans for slow progress in labor are done before even reaching this point in late labor.
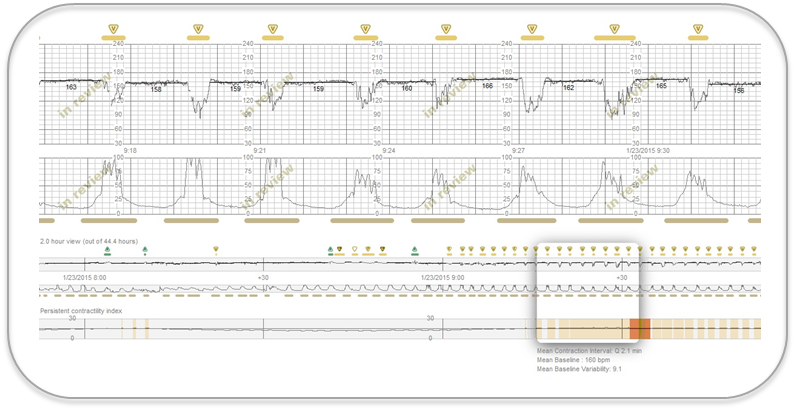
PeriCALM Patterns and CheckList continuously analyzed fetal heart rate and contraction patterns in a consistent and unbiased fashion searching for the criteria that warrant changing the oxytocin dosage. They display several hours and are color-coded to provide quick visual cues when specific criteria are exceeded. At a glance, clinicians can see the degree of abnormality, how it is trending and how long it has lasted.
Figure 3 shows an example. The upper panel shows the current tracing and its analysis. The small panel below with the slider tool summarizes the last two hours. The colors in the horizontal bar beneath show when contraction frequency or worrisome FHR patterns exceeded criteria set by the hospital.
Within two years of the introduction of this bedside application, an interim analysis showed a 36.1% (4.1%-2.6%) reduction in the time spent with excessive contraction rates. (8)
Figure 3. Fetal heart rate and contraction tracings with analysis by PeriCALM Patterns™ and Checklist™. In the example below on the right, the colors in the bar at the bottoms show when the mother developed excessive contractions with increasing abnormalities in the fetal heart rate.
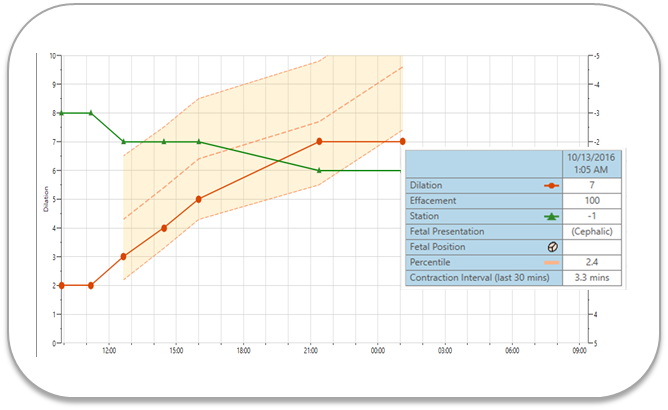
Another tool used by clinicians in this study was PeriCALM® Curve™, a perinatal software that used a quantitative method of assessing labor progress that was applied from a dilation of 3 cm to 10 cm. The mother's exam results are displayed using a dynamic graph that changes based on each exam. Figure 4 shows two examples of labor progress plotted over time. The mother's dilation is shown by the solid red line. The expected dilation, shown by the colored band, is calculated by PeriCALM Curve, based on her information streamed from the medical record and fetal monitor. The example on the left shows a labor that is progressing within the expected range. The labor on the right shows a problem with dilation.
Figure 4. Graphical display of dilation (red line) and station (green line) plotted over time. The superimposed pale red band represents the 5th to 95th percentile range of dilation expected in normal circumstances. The insert shows the values at the last examination.
Complementarity and Synergy
Years ago the "bad apple" approach to remedying medical error was common. To paraphrase the famed psychologist James Reason, blame is natural and universal because it is emotionally satisfying, often legally rewarding and politically convenient. Blaming and removing an individual, namely the "bad apple," was easy compared to changing organizational behavior. Deficiencies at the personal level, such as inadequate knowledge, behavioral issues and interpersonal skills must be addressed and corrected. A mismatch between clinician skill and task creates an error-prone scenario. However, removing a single "bad apple" will rarely make organizations safer over the long term. In fact, instituting any single corrective measure by itself is unlikely to succeed. (9,10)
Today, there is a growing appreciation of just how many forces must be aligned before sustained change occurs. Grenny and Patterson et al. have reviewed decades of original research, social science and numerous successful behavior change initiatives in areas as diverse as criminal recidivism to healthcare. (10) Over and over they have observed that behavior changed only when at least four out of six critical influential forces (affecting motivation and ability) operate concurrently. In our story one particular example stands out. "Huddles" are efficient brief meetings involving the cross-disciplinary team members. In acute care setting they occur several times per day at scheduled intervals with a structured format so that all team members share important information and are clear on the most current management plan and their individual roles. In 2008, the patient safety committee instituted the "Huddle" process and in 2012 they mandated review of the computerized analysis of the tracing and labor progress charts as well as any outstanding alerts from the intelligent EMR be a formal part of the discussion. That is, there was a complementarity between clinical needs and what technology could contribute. Huddles became easier and assessments more efficient and consistent.
Using this framework, Figure 5 shows many important components to improving healthcare outcomes.
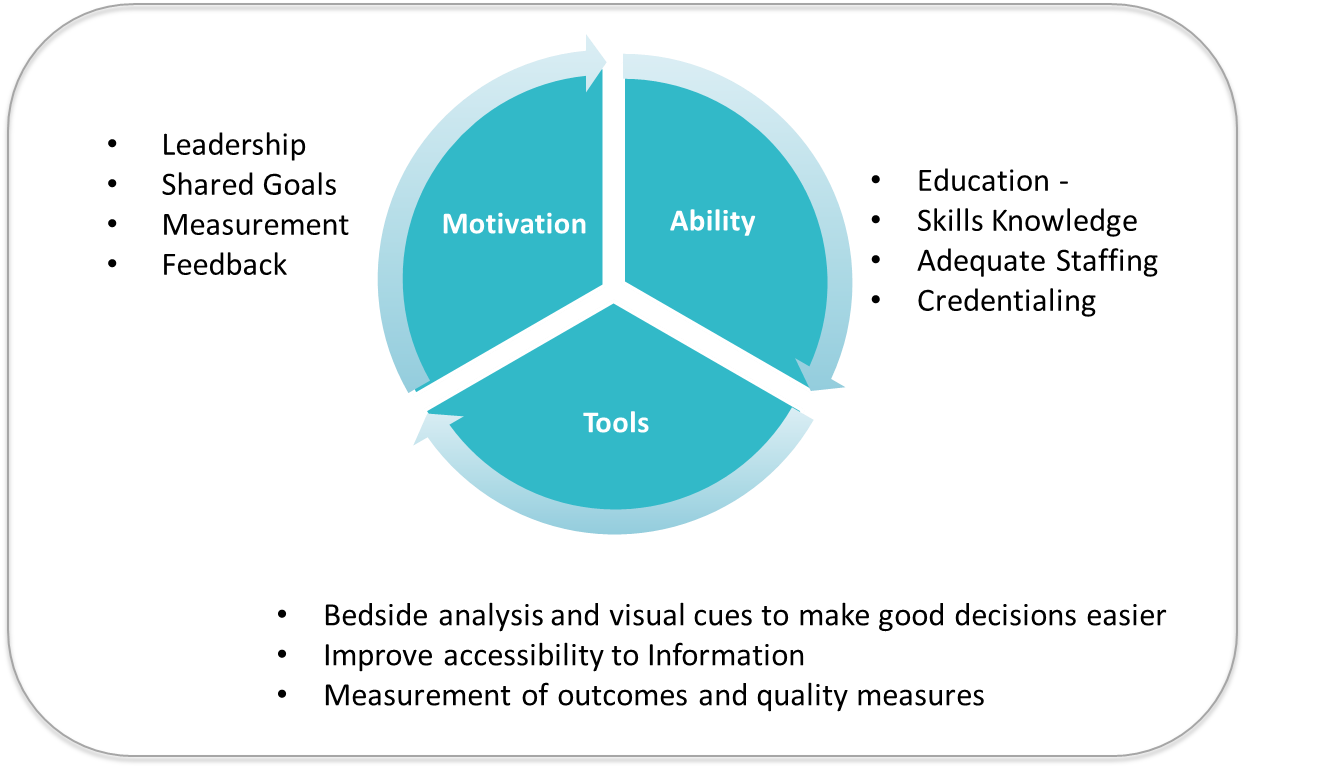
Figure 5. Components to contributing to clinical performance.
Clinical minds excel at deep reasoning, incorporating experience and knowledge to make decisions and care for patients. The human brain is capable of understanding, coming up with creative solutions and utilizing intuition. In contrast, computers have none of these qualities. However, they do excel at other tasks that are taxing for people, such as continuous monitoring, repetitive calculations and recalling and organizing large amounts of data. Medical practices require all of these abilities.
Humanity has had a long history of inventing tools to help extend our talents. This success story is no exception and is a great example of the synergy between technological and human aptitudes. Labor and delivery units produce a preponderance of a hospital's malpractice litigation. Fatigue is heightened in scenarios with high patient volumes where adverse outcomes are not uncommon. In addition, working long hours and at night induces clinician fatigue and has deleterious effects on judgement, especially when large amounts of data must be processed by the caregivers over many hours. The technology used by clinicians in this study was designed to address these factors.
The statistical and artificial intelligence techniques applied through the use of PeriCALM reduced the subjectivity of the mental adjustments that clinicians made when assessing labor progression and fetal heart rate patterns. The HIT display techniques consolidated pertinent information concisely and tirelessly providing visual cues at the bedside that helped clinicians make better decisions. Tracking and timely feedback during the 10-year study, which encompassed multiple hospitals, would have been arduous at best, if not impossible, without computerization of medical records. Furthermore, experience and data collected by these systems will fuel the next generation of innovation. In the opinion of noted physicist Stephen Hawking, the rise of artificial intelligence (AI) is an event of global significance on par with that of the industrial revolution.
Emerging technologies in all applications of clinical obstetrics are relevant and important, particularly when results demonstrate improved health outcomes, as well as cost savings to hospitals. We look forward to tomorrow with even greater application of this and other technologies, particularly now that hospitals are collecting vast amounts of electronic data through their EMR and fetal surveillance systems.\
By: Samuel Smith MD, 1,2 Lynette Philip RN1, Adi Zmiri MD3, Emily Hamilton MD3,4 Thomas Garite MD5,6
References
1. Pfuntner A, Wier L, Stocks C. Most Frequent Conditions in U.S. Hospitals 2010. Healthcare Cost and Utilization Project. AHRQ. Statistical Brief #148
2. Joseph KS, Young DC, Dodds L, O'Connell CM, Allen VM, Chandra S, Allen AC. Changes in maternal characteristics and obstetric practice and recent increases in primary cesarean delivery. Obstet Gynecol. 2003 Oct;102(4):791-800.
3. Durst JK, Tuuli MG, Stout MJ, Macones GA, Cahill AG. Degree of obesity at delivery and risk of preeclampsia with severe features. Am J Obstet Gynecol. 2016 May;214(5):651.e1-5.
4. Tabet M, Flick LH, Tuuli MG, Macones GA, Chang JJ. Prepregnancy body mass index in a first uncomplicated pregnancy and outcomes of a second pregnancy. Am J Obstet Gynecol. 2015 Oct;213(4):548.e1-7.
5. Chauhan SP, Klauser CK, Woodring TC, Sanderson M, Magann EF, Morrison JC. Intrapartum nonreassuring fetal heart rate tracing and prediction of adverse outcomes: interobserver variability. Am J Obstet Gynecol. 2008 Dec;199(6):623.e1-5.
6. Kozhimannil KB, Law MR, Virnig BA. Cesarean delivery rates vary tenfold among US hospitals; reducing variation may address quality and cost issues. Health Aff (Millwood). 2013 Mar;32(3):527-35.
7. Henke RM, Wier LM, Marder WD, Friedman BS, Wong HS. Geographic variation in cesarean delivery in the United States by payer. BMC Pregnancy Childbirth. 2014 Nov 19;14:387.
8. Smith S, Bunting C, Hamilton E. Using Intelligent Electronic Fetal Monitoring Software to Reduce Iatrogenic Complications of Childbirth. JHIM 2014;28(4):28-33.
9. Reason J. Human error: models and management. BMJ. 2000 Mar 18;320(7237):768-70.
10. Grenny, Joseph, et al. Influencer: The New Science of Leading Change. New York, McGraw Hill, 2013.
The views, opinions and positions expressed within these guest posts are those of the author alone and do not represent those of Becker's Hospital Review/Becker's Healthcare. The accuracy, completeness and validity of any statements made within this article are not guaranteed. We accept no liability for any errors, omissions or representations. The copyright of this content belongs to the author and any liability with regards to infringement of intellectual property rights remains with them.
